* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download B Cell–Specific MHC Class II Deletion Reveals Multiple
Survey
Document related concepts
Transcript
B Cell−Specific MHC Class II Deletion
Reveals Multiple Nonredundant Roles for B
Cell Antigen Presentation in Murine Lupus
This information is current as
of August 9, 2017.
Josephine R. Giles, Michael Kashgarian, Pandelakis A. Koni
and Mark J. Shlomchik
J Immunol 2015; 195:2571-2579; Prepublished online 12
August 2015;
doi: 10.4049/jimmunol.1500792
http://www.jimmunol.org/content/195/6/2571
References
Subscription
Permissions
Email Alerts
http://www.jimmunol.org/content/suppl/2015/08/12/jimmunol.150079
2.DCSupplemental
This article cites 43 articles, 28 of which you can access for free at:
http://www.jimmunol.org/content/195/6/2571.full#ref-list-1
Information about subscribing to The Journal of Immunology is online at:
http://jimmunol.org/subscription
Submit copyright permission requests at:
http://www.aai.org/About/Publications/JI/copyright.html
Receive free email-alerts when new articles cite this article. Sign up at:
http://jimmunol.org/alerts
The Journal of Immunology is published twice each month by
The American Association of Immunologists, Inc.,
1451 Rockville Pike, Suite 650, Rockville, MD 20852
Copyright © 2015 by The American Association of
Immunologists, Inc. All rights reserved.
Print ISSN: 0022-1767 Online ISSN: 1550-6606.
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
Supplementary
Material
The Journal of Immunology
B Cell–Specific MHC Class II Deletion Reveals Multiple
Nonredundant Roles for B Cell Antigen Presentation in
Murine Lupus
Josephine R. Giles,*,† Michael Kashgarian,‡ Pandelakis A. Koni,x,{
and Mark J. Shlomchik*,†
S
ystemic lupus erythematosus (SLE) is a chronic autoimmune disease with multiple immunologic and clinical manifestations. A hallmark of SLE is the presence of autoantibodies
to ubiquitous self-Ags. Ab deposition in kidneys of lupus patients
underpins the long-held notion that autoantibodies play a major part
in disease pathogenesis. Indeed, B cells have been shown to play
a central role in SLE, with the first direct evidence coming from genetic
ablation in lupus-prone MRL.Faslpr mice (1). In the absence of
B cells, there was a complete amelioration of glomerulonephritis.
Strikingly, in these mice there was no development of interstitial
nephritis, which is largely comprised of a T cell infiltrate. Furthermore, there was a marked reduction in CD4 and CD8 T cell activation as well as lymphadenopathy and splenomegaly, suggesting
direct effects of B cells on T cells and that these effects contributed
to end organ damage. These effects were Ab independent, as demonstrated by MRL.Faslpr mice engineered to have B cells that do not
secrete Ig. Such mice still developed many features of SLE, including extensive T cell activation and renal disease (2). Together,
these experiments indicated that B cells have both Ab-dependent
and -independent functions in murine SLE.
*Department of Immunobiology, Yale University School of Medicine, New Haven,
CT 06519; †Department of Immunology, University of Pittsburgh School of Medicine, Pittsburgh, PA 15261; ‡Department of Pathology, Yale University School
of Medicine, New Haven, CT 06519; xCancer Research Center, Georgia Regents
University, Augusta, GA 30192; and {Department of Medicine, Georgia Regents
University, Augusta, GA 30192
Received for publication April 2, 2015. Accepted for publication July 17, 2015.
This work was supported by National Institutes of Health Grants R01-AR044077 (to
M.J.S.) and T32-AI07019 (to J.R.G.).
Address correspondence and reprint requests to Dr. Mark J. Shlomchik, University of
Pittsburgh School of Medicine, W1052 Biomedical Science Tower, 200 Lothrop
Street, Pittsburgh, PA 15261. E-mail address: [email protected]
The online version of this article contains supplemental material.
Abbreviations used in this article: AFC, Ab-forming cell; DC, dendritic cell; GC,
germinal center; MHCII, MHC class II; RF, rheumatoid factor; SLE, systemic lupus
erythematosus; Sm, Smith Ag; TEFH, T extrafollicular helper cell.
Copyright Ó 2015 by The American Association of Immunologists, Inc. 0022-1767/15/$25.00
www.jimmunol.org/cgi/doi/10.4049/jimmunol.1500792
Although B cells can present Ag to T cells, the importance of this
function in lupus has not been directly demonstrated. In particular,
it remains controversial whether B cells can initiate responses by
presenting to naive T cells. Classically, dendritic cells (DCs) are
considered primary APCs and are arguably essential for initiating
adaptive immune responses. However, DC-deficient MRL.Faslpr mice
(3) had relatively minimal alterations in the activation, expansion,
and differentiation of peripheral T cells. Instead, DCs appeared to be
critical for local T cell expansion and differentiation in target organs,
as these DC-deficient mice had significantly fewer renal infiltrates and
improved kidney function. These findings might suggest that other
APCs are more important in initial activation of autoreactive T cells,
and DCs play a critical role in downstream events leading to disease
pathology. However, results from DC-deficient mice do not exclude
that B cells normally play only a secondary and redundant role, but
that B cells are sufficient when DCs are absent. Given the strong
paradigm that DCs must be the primary APC to initiate an immune
response, this is an important question that remains to be addressed.
The potential importance of B cell APC function in promoting
autoimmunity is highlighted by recent findings that B cells specific
for self-Ags that contain TLR7 or TLR9 ligands can be activated by
coengagement of their BCR and TLRs (4, 5), bypassing, in part, the
need for T cell help (6, 7). This type of autonomous activation also
suggests that, once activated by BCR and TLR signals alone, B cells
may be the initial APCs to break tolerance in the T cell compartment
at the outset of the anti-self response (8–10). Notably, when T cells
are present in vivo, they do amplify this BCR/TLR-driven activation,
which is evidence of productive B–T interactions. Furthermore,
B cells are likely to be particularly relevant APCs in an autoimmune
response due to their ability to concentrate very small amounts of Ag
though selective uptake of the BCR—endowing them with the potential to active low-affinity autoreactive T cells (11–14).
Nonetheless, despite theories that B cell APC function is critical in
systemic autoimmunity (1, 2, 10, 15), this has never been directly
demonstrated. Nor is it known whether such APC function is nonredundant and whether it is, at least in part, upstream of DCdependent T cell activation. In the current studies, we sought to
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
B cells have both Ab-dependent and Ab-independent functions in systemic autoimmune diseases, including systemic lupus erythematosus (SLE). Ab-independent functions are known to be important, because mice with B cells but no secreted Ig have severe
disease. These functions could include roles in lymphoid development, cytokine secretion, and Ag presentation; however, these
possibilities have not been directly tested in SLE models. In this study, we show by lineage-specific ablation of MHC class II
(MHCII) that B cell Ag presentation plays a nonredundant role in CD4+ T cell activation and effector differentiation in the
MRL.Faslpr mouse model of SLE. MHCII-mediated interactions between B and T cells further promote B cell proliferation
and differentiation, and, in fact, inefficient MHCII deletion on B cells led to strong selection of escaped cells in activated and
plasmablast compartments, further underscoring the central role of B cell Ag presentation. Despite the leakiness in the system,
B cell–specific MHCII deletion resulted in substantially ameliorated clinical disease. Hence, B cell Ag presentation is critical for T
and B cell activation and differentiation, as well as target organ damage. The Journal of Immunology, 2015, 195: 2571–2579.
2572
formally address whether B cell APC function is in fact important in
both disease and T cell activation by specifically deleting MHC class
II (MHCII) on B cells in MRL.Faslpr mice.
Materials and Methods
Mice
CD19-Cre and MHCIIfl/fl mice (16) were backcrossed 10 generations onto the
Fas-deficient, lupus-prone MRL-MpJ-Faslpr/J strain (Jackson; referred to
as MRL.Faslpr). These mice were intercrossed to generate CD19-Cre+/2
MHCIIfl/fl MRL.Faslpr mice. CD19-Cre+/2 MHCIIfl/fl MRL.Faslpr mice
and MHCIIfl/fl MRL.Faslpr mice were bred together to generate experimental
mice. All mice were analyzed at 12 wk of age. For BrdU labeling, mice were
given an i.p. injection of 1 mg BrdU in sterile PBS 1 h before sacrifice. All
animals were maintained under specific pathogen-free conditions and handled according to protocols approved by the Institutional Animal Care and
Use Committee at Yale and the University of Pittsburgh.
Evaluation of renal disease
Kidneys were formalin fixed, paraffin embedded, and stained with H&E. Glomerular and interstitial nephritis were scored blindly by a pathologist (M.K.),
as described (17). Proteinuria was assessed with Bayer Albustix strips.
All surface staining was performed in ice-cold PBS with 3% calf serum and
FcR blocking Ab, 24G.2, except for CXCR4 staining, which was done
at room temperature. Ab clones used for surface staining were as follows:
anti-CD19 (1D3), anti-CD22 (Cy34.1), anti-CD138 (281-2), anti-CD44
(1M7), anti-IE/IA (M5/114), anti–TCR-b (H57-597), anti-CD4 (GK1.5),
anti-CD8 (TIA 105), anti-CD62L (Mel-14), anti–P-selectin glycoprotein
ligand-1 (PSGL-1, 2PH1), anti-CXCR4 (2B11), anti-CD11c (N418), anti-CD11b
(M1/70), anti-F4/80 (BM8), anti-BST2 (927), anti-Siglec H (eBio440c), antiLy6G/Ly6C (RB6-8C5), anti-Ly6C (HK1.4), anti–peanut agglutinin (Vector
Laboratories), and anti-CD38 (90). Bcl6 staining used the eBioscience
FoxP3/Transcription Factor Staining Buffer Set and the K112-91 clone. All
other intracellular staining used the BD Cytofix/Cytoperm and Permwash
buffers. Plasmablasts were detected with intracellular anti-k (187.1) and anti-IgM
(B7-6). For intracellular cytokine staining, 4 3 106 splenocytes were stimulated
with PMA (20 ng/ml) and ionomycin (750 ng/ml) for 4–6 h at 37˚C; brefeldin
A (10 mg/ml) was added after the first 2 h. IFN-g was detected with clone XMG1.2;
IL-21 was detected with a mouse rIL-21R subunit/human IgG1 Fc chimera
(R&D Systems) and goat anti-human Fcg conjugated to PE (Jackson ImmunoResearch). Ethidium monoazidewas used for live-dead discrimination (Invitrogen);
the cells were incubated under foil for 10 min and under a bright fluorescent
light for 10 min. BrdU incorporation was detected, as previously described (18).
Quantitative PCR
To quantitate the deletion efficiency of MHCII, genomic DNA was extracted from FACS-purified cells. For each sample, the D cycle threshold
was calculated by comparing MHCII and the unaffected gene, IL-10 (19).
The DD cycle threshold was calculated by comparing each sorted subset
(naive, activated, and plasmablasts) from CD19-Cre mice to control
mice. IL-10 was amplified with forward primer, (59-39) GCTCTTACTGACTGGCATGAG and reverse primer, CGCAGCTCTAGGAGCATGTG.
MHCII was amplified with forward primer, CCTGGTGACTGCCATTACCT, and reverse primer, AGGGTCCCTCAGAACACGAC.
Cytokine message in FACS-purified DCs was measured, as previously
described (19). Quantitative RT-PCR was performed with the Agilent
Brilliant II SYBR Green QPCR kit on a Stratagene Mx3000P instrument.
pared with MHCIIfl/fl littermate controls. In CD19-Cre mice, an
average of 85% of the B cell population had undetectable surface
MHCII expression (Fig. 1). Negligible loss of MHCII expression
was observed in conventional DCs, plasmacytoid DCs, macrophages, and neutrophils (data not shown). Interestingly, there was an
increase in the total number of conventional DCs in the CD19-Cre
mice, and this population had an increase in surface expression of
MHCII (Supplemental Fig. 1A, 1B). However, there was a decrease
in CD86 expression (Supplemental Fig. 1C) and no detectable differences in cytokine message for IL-1b, IL-6, p35, or p40 by
quantitative PCR (data not shown), indicating the conventional DCs
were not in a more activated state.
To directly assess the effect of MHCII expression on B cell activation and differentiation, we sorted naive B cells, activated B
cells, and plasmablasts from the same CD19-Cre animals (Fig. 2A).
Because MHCII is downregulated as B cells differentiate into AFCs,
we used quantitative PCR to determine the amount of deletion within
each population. Deletion efficiency among naive B cells was
95%. In stark contrast, only 29% of alleles were deleted in sorted
plasmablasts (Fig. 2B). Activated B cells exhibited an intermediate
genotype with 75% deletion. Because germinal center (GC)
B cells normally express MHCII, we could assess deletion efficiency in this population by flow cytometry (Fig. 2C). In CD19-Cre
mice, ∼75% of GC B cells expressed MHCII (Fig. 2D). Thus,
although 95% of naive B cells and the majority of activated
B cells lacked MHCII expression, the B cells that were able
to form Ag-specific interactions with T cells had a significant
advantage in further differentiation into both plasmablasts and
GC B cells. The presence of these activated MHCII+ B cells in the
CD19-Cre mice, however, does limit the impact of genetic deletion
of MHCII in the CD19-Cre mice. Because there is only a partial
loss of MHCII expression and such loss is further attenuated
upon differentiation, any observed phenotypes would be minimal
approximations of what would be achieved by complete deletion of
MHCII on all B cells.
MHCII-positive B cells have a significant proliferation
advantage
To assess the dependence of B cell proliferation on MHCII expression, we performed a 1-h BrdU pulse, which labels cells in S
phase. There were ∼50% fewer splenic BrdU+ B cells in the CD19Cre mice compared with littermate controls (Fig. 3A). Strikingly,
within the BrdU+ population in CD19-Cre mice, 65% of the cells
were MHCII positive. In contrast, only 10% of the BrdU2 cells
expressed MHCII (Fig. 3B). In contrast, there was no difference
in the percentage of BrdU+ cells within the plasmablast compart-
ELISPOT, ELISA, and Luminex
Ab-forming cells (AFCs) were analyzed by ELISPOT, as previously described (19). Antinucleosome (20), anti-RNA (17), and anti-Smith Ag (Sm)
(21) serum titers were determined by specific ELISAs, as previously described. The total serum Ig of IgM, IgG2a, IgG1, and IgAwas analyzed using
Luminex assay (Millipore), according to the manufacturer’s instructions.
Results
Effects of selective deletion of MHCII in B cells
To study the role of Ag presentation by B cells in lupus, we generated
mice carrying both CD19-Cre and homozygous loxP-flanked MHCII
(MHCIIfl/fl) alleles, hereafter called CD19-Cre mice, on the
MRL.Faslpr background. The mice were aged to 12 wk and com-
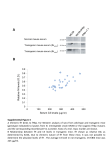
FIGURE 1. Deletion of MHCII in B cells. (A) Representative histograms
of MHCII staining of splenic B cells from control, MHCIIfl/fl, and CD19-Cre
MHCIIfl/fl mice. Cells were first gated as ethidium monoazide2 TCR-b2,
then CD19highCD1382. (B) Frequency of MHCII+ splenic B cells, identified
as in (A), in the experimental cohorts. Data are pooled from six independent
cohorts of 12-wk-old mice; control n = 30 and CD19-Cre n = 32. Data are
represented as mean 6 SEM. Statistics were calculated by two-tailed Mann–
Whitney U test. ****p , 0.0001.
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
Flow cytometry
B CELL–SPECIFIC MHCII DELETION IN LUPUS
The Journal of Immunology
ment between CD19-Cre and control animals (Fig. 3C), most likely
reflective of the fact that essentially all plasmablasts must harbor at
least one intact MHCII allele (given the ∼25% deletion frequency;
Fig. 2B) and were thus able to engage T cell help at some point
during their evolution.
Expression of MHCII is critical for B cell differentiation
Although there was clearly strong selection for cells that escaped
deletion of MHCII during the progression of B cell activation, in
the CD19-Cre mice there were nevertheless fewer total CD19high
CD1382 B cells, a population that most likely included a combination
of activated, naive, and memory B cells (Fig. 4A, 4B). This was
probably, at least in part, due to the observed difference in proliferation (Fig. 3A). There were also decreases in the transitional
and marginal zone B cell compartments, but no alterations were
found in the bone marrow (data not shown). The total number
of plasmablasts (CD19 IntCD138+ CD44highintracellular-khigh)
per spleen was also reduced in CD19-Cre mice compared with littermate controls (Fig. 4A, 4C), probably due to decreased differentiation, as proliferation within the plasmablast compartment was
similar between genotypes (Fig. 3C). Furthermore, the ratio of
isotype-switched to nonswitched plasmablasts was significantly
reduced in CD19-Cre mice (Fig. 4A, 4D). Similarly, GC B cells were
also drastically reduced in CD19-Cre mice (Fig. 4E, 4F).
CD19-Cre mice did not have significantly reduced IgM AFC
numbers as measured by ELISPOT, but, commensurate with flow
FIGURE 3. MHCII+ B cells have a significant proliferation advantage. One
hour before sacrifice, mice were injected with 1 mg BrdU i.p. (A) Splenic B cells
(ethidium monoazide2 TCR-b2CD22+) were evaluated for BrdU incorporation
by flow cytometry. Data are represented as mean 6 SEM. (B) Representative
staining plot of MHCII expression and BrdU incorporation of B cells from
a CD19-Cre mouse. The bar graph represents the percentage of MHCII+ B cells
within the BrdU2 and BrdU+ B cell populations as the mean 6 SEM. (C) Plasmablasts (ethidium monoazide2 TCR-b2CD22IntCD138+) were evaluated for
BrdU incorporation by flow cytometry. Data are represented as mean 6SEM. Data
are pooled from two independent experiments; control n = 21, CD19-Cre n = 20.
Statistics were calculated by two-tailed Mann–Whitney U test. ****p , 0.0001.
cytometry data on plasmablasts, IgG2a and IgG1 AFCs were
decreased (Fig. 5A). These differences were reflected in the total
serum Ig titers (Fig. 5B). Total serum IgG2a and IgG1 correlated
with the percentage of residual MHCII+ B cells (Supplemental
Fig. 2A, 2B). These findings agree with previous data that rheumatoid factor (RF) B cell AFC differentiation in T cell–deficient
hosts showed a strong effect on isotype-switched AFCs, but no
effect on IgM AFCs (7). The results support a critical role for
cognate interactions with MHCII-restricted T cells in B cell differentiation and isotype switch.
Specific autoantibodies differ in their dependence on B cell
MHCII expression
Although serum IgG is generally thought to be generated by GCderived long-lived plasma cells, at least some autoantibodies are
largely produced by short-lived plasmablasts, which may be less
dependent on MHCII expression and T cell help (22, 23). To
assess the effects of B cell MHCII expression on the titers of serum
autoantibodies, we performed specific ELISAs for antinucleosome,
anti-RNA, and anti-Sm. Antinucleosome IgM titers were significantly
reduced in CD19-Cre mice; however, there was not a statistically
significant difference between CD19-Cre and control mice in isotypeswitched antinucleosome titers (Fig. 6A). Anti-RNA autoantibodies
exhibited the opposite pattern: no difference in the IgM titer,
but lower titers of anti-RNA IgG (Fig. 6B) in CD19-Cre mice,
which correlated with the percentage of residual MHCII+
B cells (Supplemental Fig. 2C). Anti-Sm exhibited the greatest
dependence on B cell MHCII expression; both IgM and IgG
anti-Sm titers were lower in the CD19-Cre mice (Fig. 6C); IgG
correlated with the percentage of residual MHCII+ B cells
(Supplemental Fig. 2D). These results are likely a reflection of
the differential abilities of the particular self-Ags to induce autonomous B cell activation without the initial need for T cells. In particular, B cells specific for Ags with strong BCR and TLR ligand
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
FIGURE 2. Selective differentiation of residual MHCII+ B cells in CD19-Cre
mice. (A) FACS strategy to identify naive B cells, activated B cells, and plasmablasts. The cells were first gated as ethidium monoazide2 TCR-b2 CD11c2
CD11b2. (B) Deletion efficiency of MHCII in the three sorted cell populations
was determined by quantitative RT-PCR. Deletion efficiency was calculated
with the equation (1 2 residual MHCII) 3 100. Residual MHCII was calculated
as 22DDCt. Data represent a total of nine CD19-Cre mice from two independent
experiments; each dot is an individual mouse. Horizontal bars mark the mean.
(C) Representative staining plots of MHCII staining on total B cells (ethidium
monoazide2 TCR-b2CD22+) and GC B cells (ethidium monoazide2 TCR-b2
CD22+ CD38Int peanut agglutinin+) from one CD19-Cre mouse. (D) Summary
data are represented as mean 6 SEM. Data are pooled from two independent
cohorts of 12-wk-old mice; control n = 16 and CD19-Cre n = 16. Statistics were
calculated by two-tailed Mann–Whitney U test. **p , 0.01, ****p , 0.0001.
2573
2574
B CELL–SPECIFIC MHCII DELETION IN LUPUS
activities may not depend as greatly on T cell help for activation
and differentiation.
B cell Ag presentation plays a nonredundant role in T cell
activation and differentiation
Thegreater reduction innumbers ofactivated and memoryphenotype
T cells previously reported in B cell–deficient versus DC-deficient
MRL.Faslpr mice suggests that B cells may be more important in
initial Ag presentation and activation (1, 3, 24). We assessed the
FIGURE 5. Isotype switch in AFCs is dependent on
MHCII. (A) Total numbers of AFCs per spleen were
determined by ELISPOT for IgM, IgG2a, and IgG1.
Each dot is an individual mouse. Bars show geometric
means. Data are pooled from six independent cohorts of
12-wk-old mice; control n = 29 and CD19-Cre n = 32. (B)
Serum Ig concentrations determined by multiplex
ELISAs. Data are represented as mean 6 SEM. Data are
pooled from seven independent cohorts of 12-wk-old
mice; control n = 35 and CD19-Cre n = 32. Statistics
were calculated by two-tailed Mann–Whitney U test.
*p , 0.05, ****p , 0.0001.
T cell compartment in CD19-Cre mice to directly test whether B cell
APC function is needed for optimal T cell activation and expansion.
CD19-Cre mice had no reduction in the total number of splenic
T cells (Fig. 7A). However, the percentage of activated T cells in
CD19-Cre mice was significantly lower in both the CD4 and CD8
populations (Fig. 7B, 7C). There was a concurrent increase in naive
phenotype cells that correlated with the percentage of residual
MHCII+ B cells (Fig. 7B, 7C, Supplemental Fig. 2E, 2F). There was
a consistent decrease in frequencies of IFN-g+ CD4 T cells, but not
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
FIGURE 4. Expression of MHCII is critical for plasmablast and GC B cell differentiation. (A) Representative staining plots of plasmablast and B cell gating.
Cells were first gated as ethidium monoazide2 TCR-b2. (B) Total number of B cells and (C) plasmablasts per spleen determined by flow cytometry. Data are
represented as mean 6 SEM. (D) Isotype-switched plasmablasts (IgM2) were normalized to the nonswitched (IgM+). Data are represented as mean 6 SEM.
Data are pooled from six independent cohorts of 12-wk-old mice; control n = 30 and CD19-Cre n = 32. (E) Representative staining plots of GC B cell gating
from one control mouse and one CD19-Cre mouse. Cells were first gated on ethidium monoazide2 TCR-b2CD22+. (F) Total number of GC B cells per
spleen identified as in (E). Data are represented as mean 6 SEM. Data are pooled from two independent cohorts of 12-wk-old mice; control n = 26 and CD19-Cre
n = 16. Statistics were calculated by two-tailed Mann–Whitney U test. ***p , 0.001, ****p , 0.0001.
The Journal of Immunology
2575
in IFN-g+ CD8 T cells, upon PMA/ionomycin restimulation in vitro,
which also correlated with the percentage of residual MHCII+
B cells (Fig. 7D, 7E, Supplemental Fig. 2G). Hence, there is a nonredundant role for B cell–MHCII expression in the activation and
subsequent differentiation of T cells in lupus. As discussed above,
the incomplete deletion and preferential activation of escaped
MHCII+ B cells could have led to the large number of activated
effectors observed in the CD19-Cre mice. A more complete deletion
almost certainly would have resulted in a more profound effect in the
T cell compartment, possibly approaching that seen in the total
B cell knockout. It is also possible that other professional APCs
could have compensated in the absence of B cell–expressed MHCII.
Decrease in Th cells in CD19-Cre mice
T extrafollicular helper cells (TEFH) comprise in both lupus-prone
and normal mice a Bcl6-expressing B-helper CD4 T cell subset that
is present extrafollicularly, presumably as a result of CXCR4, rather
than CXCR5, expression (25–29). Work from our laboratory has
found a near-complete loss of these cells in B cell–deficient
MRL.Faslpr mice (30). There was a significant decrease in the
number of splenic TEFH cells in the CD19-Cre mice (Fig. 8A, 8B).
However, the frequency of IL-21–producing cells within the CD4
T cell compartment, which include TEFH as well as other more numerous effector populations, was similar between CD19-Cre and
control mice (Fig. 8C).
MHCII on B cells significantly affects clinical disease
Perhaps the most important aspect of our studies was the opportunity to directly test whether the development of clinical disease
would depend on the ability of B cells to present Ag to CD4
T cells. Critically, and despite inefficient B cell MHCII deletion,
CD19-Cre mice had significantly less interstitial and glomerular
FIGURE 7. B cell Ag presentation plays a nonredundant role in T cell activation and differentiation. (A) Total numbers of CD4, CD8, DN, and T cells
enumerated by flow cytometry. Frequency of naive (CD442CD62L+) and activated (CD44+CD62L2) (B) CD4 and (C) CD8 T cells determined by flow
cytometry. Representative intracellular IFN-g staining histograms and numbers of (D) CD4 and (E) CD8 T cells stimulated with PMA and ionomycin. Control
mice are shown in bold. Data are represented as mean 6 SEM. Data are pooled from six independent cohorts of 12-wk-old mice; control n = 30 and CD19-Cre
n = 32. Statistics were calculated by two-tailed Mann–Whitney U test. **p , 0.01, ***p , 0.001, ****p , 0.0001.
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
FIGURE 6. Specific autoantibodies differ in their dependence on B cell MHCII expression. (A) Serum concentration of antinucleosome IgM and IgG, (B)
anti-RNA IgM and IgG, and (C) anti-Sm IgM and IgG was determined by ELISA. Bars show geometric means. Data are pooled from seven independent cohorts
of 12-wk-old mice; control n = 35 and CD19-Cre n = 39. Statistics were calculated by two-tailed Mann–Whitney U test. *p , 0.05, **p , 0.01, ***p , 0.001,
****p , 0.0001.
2576
B CELL–SPECIFIC MHCII DELETION IN LUPUS
nephritis than littermate controls (Fig. 9A). These histological
differences were reflected in the improved kidney function as
measured by proteinuria (Fig. 9B). CD19-Cre mice had substantially reduced lymph node weight and a small but significant
decrease in spleen weight compared with controls (Fig. 9C, 9D).
These findings demonstrate a nonredundant role for Ag presentation by B cells in end-organ damage and overall pathogenesis
(Fig. 10).
Discussion
B cells play central and multiple roles in systemic autoimmune
diseases (31). Although autoantibody production was originally
thought to be the main contribution of B cells, accumulating data
support that B cells have important Ab-independent functions. It
is critical to distinguish putative functions that were suggested or
inferred in discussions of data derived from complete B cell deletion
or receptor restriction from those that have been directly tested
and proven (32–35). Subsequent work has addressed these various
functions in turn. Ab-independent roles in autoimmunity have
been demonstrated by the observation of persistent disease in mice
with B cells that cannot secrete Abs (2). Potential roles in lymphoid
tissue development were addressed by depletion of B cells in adult
mice, which did partially ameliorate disease, demonstrating that
at least some aspects by which B cells promote disease are independent of developmental issues (36, 37). However, although a role
for Ag presentation may have been inferred, in our view it could
not have been addressed without directly impairing Ag presentation
on B cells, which in turn would be most convincingly achieved by
cell-specific deletion of MHCII. An important role for B cells as
APCs has been implicated in other autoimmune diseases. A role
for B cell–specific Ag presentation was recently shown in myelin
oligodendrocyte glycoprotein–induced experimental autoimmune
encephalomyelitis, in which heterologous Ag given in CFA induces
a transient T cell autoimmune syndrome (38). In the NOD mice,
MHCII expression on B cells was necessary for the development
of spontaneous destructive diabetes (39). To our knowledge, the
importance of B cell presentation has yet to be directly tested in
any model of SLE. In this study, we report the outcome in mice
carrying CD19-Cre and MHCIIfl/fl genotypes that were fully backcrossed onto the lupus-prone MRL.Faslpr background. These results
provide direct evidence that Ag presentation by B cells does have
a nonredundant role in T cell activation, Th1 differentiation, and Th
cell differentiation in a murine model of lupus. We also found that
the cognate, MHCII-mediated interactions between B and T cells are
important for B cell activation, proliferation, and differentiation.
Given the robust response of the escapee B cells in our system, it is
notable that there was a clear biologically and statistically significant
effect on clinical disease—including kidney disease, lymphadenopathy, and splenomegaly—indicating a requisite role for B cell
APC function in these processes. Complete deletion of MHCII
in the B cell compartment almost certainly would have led to an
even more profound effect. These results, in combination with
previous studies, formally demonstrate that B cells are key APCs
in systemic autoimmune disease and highlight the importance
FIGURE 9. Deletion of MHCII on B cells ameliorates clinical disease.
(A) Glomerular and interstitial nephritis (GN and IN) were scored from
0 to 6. (B) Proteinuria was scored from 0 to 5. Each dot represents an individual mouse. Horizontal lines represent the medians. (C) Weights of combined axillary lymph nodes and (D) spleen were measured. Data are
represented as median 6 SEM. Data are pooled from six independent cohorts
of 12-wk-old mice; control n = 30 and CD19-Cre n = 32. Statistics were
calculated by two-tailed Mann–Whitney U test. *p , 0.05, ***p , 0.001.
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
FIGURE 8. TEFH cells are decreased in CD19-Cre mice. (A) Representative staining plots of TEFH gating. Cells are first gated on ethidium
monoazide2 CD192 . Percentage is the mean of TEFH of CD4 T cells in CD19-Cre mice. (B) The number of TEFH cells per spleen, as identified in (A).
Data are pooled from two independent cohorts; control n = 9, CD19-Cre n = 12. (C) Representative intracellular IL-21 staining plots of CD4 T cells
unstimulated (left) and stimulated with PMA and ionomycin (right). Data are represented as mean 6 SEM. Data are pooled from two independent
cohorts of 12-wk-old mice; control n = 15 and CD19-Cre n = 10. Statistics were calculated by two-tailed Mann–Whitney U test. *p , 0.05.
The Journal of Immunology
2577
of Ag-specific B cell–T cell interactions even in a TLR-driven
response that can occur outside of GCs.
The incomplete deletion of MHCII on B cells in the CD19-Cre
MHCIIfl/fl mice, although not ideal, did enable us to compare the
fate of MHCII+ and MHCII2 B cells within the same animal.
MHCII+ B cells had a substantial advantage in almost every parameter we examined: proliferation, differentiation into plasmablasts or GC B cells, and isotype switching. The dramatic expansion
of B cells that retained a MHCII allele during progression through
expansion and differentiation underscores the importance of B–T
cognate interactions in all of these processes. A similar escape
phenomenon was observed in a study using the same Cre-LoxP
system and a traditional T-dependent model Ag. When CD19-Cre
MHCIIfl/fl C57BL/6 mice were immunized with nitrophenyl–
chicken gamma globulin, as few as 2% of residual MHCII+ B cells
were able to expand, with the response eventually reaching similar
numbers of GC B cells to the MHCII-intact animals (40).
Despite the importance of T–B cognate interactions, our experiments do show that expression of MHCII is not strictly required
for any aspect of the B cell response. Indeed, the majority of acti-
vated B cells still had fully deleted MHCII. This indicates that
initial activation is mostly T independent, as we have previously
found for the TLR-dependent RF B cell response in the AM14 model
system (6, 7). However, further differentiation into plasmablasts
or GC B cells is substantially affected by the loss of cognate T cell
help. Although the differentiation into plasmablasts was significantly decreased in the CD19-Cre MHCIIfl/fl mice, only isotypeswitched AFC and resulting serum IgG were affected. This greater
dependence on T cell help for isotype-switched AFCs is also consistent with our previous studies with the AM14 B cells and also
studies of T cell–deficient MRL.Faslpr mice (6, 7, 41, 42). It is
interesting that the large number of activated and cytokineproducing CD4 T cells that were present in CD19-Cre mice
could not compensate for the lack of Ag-specific interactions.
The necessity for cognate interactions to promote full-blown
B cell–mediated autoimmunity was also suggested by a previous
study showing reduced disease in TCR transgenic MRL.Faslpr mice
with a restricted repertoire (43).
The partial T cell–independence of B cell activation, as shown in
this work and also as demonstrated for in vivo activation of RF
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
FIGURE 10. Activation and pathogenesis in systemic autoimmunity (1). Autoreactive B cells, such as those specific for DNA, become activated through
engagement of their BCR and TLRs in a MyD88-dependent manner (2). Activated autoreactive B cells present Ag on MHCII and upregulate costimulatory
molecules, resulting in the activation of cognate autoreactive CD4 T cells (3). B cells and DCs promote subsequent differentiation into Th1 and TEFH cells (4).
Cognate-activated T cells provide help such as CD40 ligation and cytokines, resulting in significant expansion and isotype switch of the plasmablasts (5).
Activated autoreactive B cells promote epitope spreading and expansion of the anti-self response. B cells have the potential to present anything that is endocytosed through their BCR, not only the protein sequences recognized by the CDR3 region (6). Activated T cells migrate and infiltrate target tissues, such as
the kidneys, in a DC-dependent manner. These T cells may activate resident or migratory DCs through CD40-CD40L ligation that induces ICOSL expression on
the DCs. DC-expressed ICOSL promotes kidney damage.
2578
Acknowledgments
We thank Jaime Cullen for excellent technical assistance. We thank
the technicians of the Yale Animal Resources Center and Division of
Laboratory Animal Resources at the University of Pittsburgh for excellent work in animal husbandry.
Disclosures
The authors have no financial conflicts of interest.
References
1. Chan, O., and M. J. Shlomchik. 1998. A new role for B cells in systemic autoimmunity: B cells promote spontaneous T cell activation in MRL-lpr/lpr mice.
J. Immunol. 160: 51–59.
2. Chan, O. T. M., L. G. Hannum, A. M. Haberman, M. P. Madaio, and
M. J. Shlomchik. 1999. A novel mouse with B cells but lacking serum antibody
reveals an antibody-independent role for B cells in murine lupus. J. Exp. Med.
189: 1639–1648.
3. Teichmann, L. L., M. L. Ols, M. Kashgarian, B. Reizis, D. H. Kaplan, and
M. J. Shlomchik. 2010. Dendritic cells in lupus are not required for activation of
T and B cells but promote their expansion, resulting in tissue damage. Immunity
33: 967–978.
4. Leadbetter, E. A., I. R. Rifkin, A. M. Hohlbaum, B. C. Beaudette, M. J. Shlomchik,
and A. Marshak-Rothstein. 2002. Chromatin-IgG complexes activate B cells by
dual engagement of IgM and Toll-like receptors. Nature 416: 603–607.
5. Lau, C. M., C. Broughton, A. S. Tabor, S. Akira, R. A. Flavell, M. J. Mamula,
S. R. Christensen, M. J. Shlomchik, G. A. Viglianti, I. R. Rifkin, and
A. Marshak-Rothstein. 2005. RNA-associated autoantigens activate B cells by
combined B cell antigen receptor/Toll-like receptor 7 engagement. J. Exp. Med.
202: 1171–1177.
6. Herlands, R. A., S. R. Christensen, R. A. Sweet, U. Hershberg, and
M. J. Shlomchik. 2008. T cell-independent and Toll-like receptor-dependent
antigen-driven activation of autoreactive B cells. Immunity 29: 249–260.
7. Sweet, R. A., M. L. Ols, J. L. Cullen, A. V. Milam, H. Yagita, and
M. J. Shlomchik. 2011. Facultative role for T cells in extrafollicular Toll-like
receptor-dependent autoreactive B-cell responses in vivo. Proc. Natl. Acad. Sci.
USA 108: 7932–7937.
8. Rodrı́guez-Pinto, D. 2005. B cells as antigen presenting cells. Cell. Immunol.
238: 67–75.
9. Rodrı́guez-Pinto, D., and J. Moreno. 2005. B cells can prime naive CD4+ T cells
in vivo in the absence of other professional antigen-presenting cells in a CD154CD40-dependent manner. Eur. J. Immunol. 35: 1097–1105.
10. Yan, J., B. P. Harvey, R. J. Gee, M. J. Shlomchik, and M. J. Mamula. 2006.
B cells drive early T cell autoimmunity in vivo prior to dendritic cell-mediated
autoantigen presentation. J. Immunol. 177: 4481–4487.
11. Kurt-Jones, E. A., D. Liano, K. A. HayGlass, B. Benacerraf, M. S. Sy, and
A. K. Abbas. 1988. The role of antigen-presenting B cells in T cell priming
in vivo: studies of B cell-deficient mice. J. Immunol. 140: 3773–3778.
12. Lanzavecchia, A. 1985. Antigen-specific interaction between T and B cells.
Nature 314: 537–539.
13. Lanzavecchia, A. 1990. Receptor-mediated antigen uptake and its effect on
antigen presentation to class II-restricted T lymphocytes. Annu. Rev. Immunol. 8:
773–793.
14. Tony, H. P., N. E. Phillips, and D. C. Parker. 1985. Role of membrane immunoglobulin (Ig) crosslinking in membrane Ig-mediated, major histocompatibilityrestricted T cell-B cell cooperation. J. Exp. Med. 162: 1695–1708.
15. Mamula, M. J., S. Fatenejad, and J. Craft. 1994. B cells process and present
lupus autoantigens that initiate autoimmune T cell responses. J. Immunol. 152:
1453–1461.
16. Hashimoto, K., S. K. Joshi, and P. A. Koni. 2002. A conditional null allele of the
major histocompatibility IA-beta chain gene. Genesis 32: 152–153.
17. Campbell, A. M., M. Kashgarian, and M. J. Shlomchik. 2012. NADPH oxidase
inhibits the pathogenesis of systemic lupus erythematosus. Sci. Transl. Med. 4:
157ra141.
18. Nickerson, K. M., J. L. Cullen, M. Kashgarian, and M. J. Shlomchik. 2013.
Exacerbated autoimmunity in the absence of TLR9 in MRL.Fas(lpr) mice
depends on Ifnar1. J. Immunol. 190: 3889–3894.
19. Teichmann, L. L., D. Schenten, R. Medzhitov, M. Kashgarian, and
M. J. Shlomchik. 2013. Signals via the adaptor MyD88 in B cells and DCs make
distinct and synergistic contributions to immune activation and tissue damage in
lupus. Immunity 38: 528–540.
20. Nickerson, K. M., S. R. Christensen, J. Shupe, M. Kashgarian, D. Kim, K. Elkon,
and M. J. Shlomchik. 2010. TLR9 regulates TLR7- and MyD88-dependent autoantibody production and disease in a murine model of lupus. J. Immunol. 184:
1840–1848.
21. Christensen, S. R., M. Kashgarian, L. Alexopoulou, R. A. Flavell, S. Akira, and
M. J. Shlomchik. 2005. Toll-like receptor 9 controls anti-DNA autoantibody
production in murine lupus. J. Exp. Med. 202: 321–331.
22. William, J., C. Euler, and M. J. Shlomchik. 2005. Short-lived plasmablasts
dominate the early spontaneous rheumatoid factor response: differentiation
pathways, hypermutating cell types, and affinity maturation outside the germinal
center. J. Immunol. 174: 6879–6887.
23. Hoyer, B. F., K. Moser, A. E. Hauser, A. Peddinghaus, C. Voigt, D. Eilat,
A. Radbruch, F. Hiepe, and R. A. Manz. 2004. Short-lived plasmablasts and
long-lived plasma cells contribute to chronic humoral autoimmunity in NZB/W
mice. J. Exp. Med. 199: 1577–1584.
24. Chan, O. T. M., M. P. Madaio, and M. J. Shlomchik. 1999. B cells are required
for lupus nephritis in the polygenic, Fas-intact MRL model of systemic autoimmunity. J. Immunol. 163: 3592–3596.
25. Odegard, J. M., B. R. Marks, L. D. DiPlacido, A. C. Poholek, D. H. Kono,
C. Dong, R. A. Flavell, and J. Craft. 2008. ICOS-dependent extrafollicular helper
T cells elicit IgG production via IL-21 in systemic autoimmunity. J. Exp. Med.
205: 2873–2886.
26. Weinstein, J. S., S. G. Hernandez, and J. Craft. 2012. T cells that promote B-cell
maturation in systemic autoimmunity. Immunol. Rev. 247: 160–171.
27. Yu, D., A. H. Tan, X. Hu, V. Athanasopoulos, N. Simpson, D. G. Silva,
A. Hutloff, K. M. Giles, P. J. Leedman, K. P. Lam, et al. 2007. Roquin represses
autoimmunity by limiting inducible T-cell co-stimulator messenger RNA. Nature
450: 299–303.
28. Linterman, M. A., R. J. Rigby, R. K. Wong, D. Yu, R. Brink, J. L. Cannons,
P. L. Schwartzberg, M. C. Cook, G. D. Walters, and C. G. Vinuesa. 2009. Follicular helper T cells are required for systemic autoimmunity. J. Exp. Med. 206:
561–576.
29. Lee, S. K., R. J. Rigby, D. Zotos, L. M. Tsai, S. Kawamoto, J. L. Marshall,
R. R. Ramiscal, T. D. Chan, D. Gatto, R. Brink, et al. 2011. B cell priming for
extrafollicular antibody responses requires Bcl-6 expression by T cells. J. Exp.
Med. 208: 1377–1388.
30. Teichmann, L. L., J. L. Cullen, M. Kashgarian, C. Dong, J. Craft, and
M. J. Shlomchik. 2015. Local triggering of the ICOS coreceptor by CD11c(+)
myeloid cells drives organ inflammation in lupus. Immunity 42: 552–565.
31. Chan, O. T., M. P. Madaio, and M. J. Schlomchik. 1999. The central and multiple
roles of B cells in lupus pathogenesis. Immunol. Rev. 169: 107–121.
32. Noorchashm, H., N. Noorchashm, J. Kern, S. Y. Rostami, C. F. Barker, and
A. Naji. 1997. B-cells are required for the initiation of insulitis and sialitis in
nonobese diabetic mice. Diabetes 46: 941–946.
33. Akashi, T., S. Nagafuchi, K. Anzai, S. Kondo, D. Kitamura, S. Wakana, J. Ono,
M. Kikuchi, Y. Niho, and T. Watanabe. 1997. Direct evidence for the contribution of B cells to the progression of insulitis and the development of diabetes
in non-obese diabetic mice. Int. Immunol. 9: 1159–1164.
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017
B cells, raises the question of how important T–B interactions are in
an immune response that is driven by B cell–intrinsic TLR signaling
(6). B cell–specific deletion of MyD88 in otherwise intact
MRL.Faslpr mice demonstrated that this molecule is not only critical
for intrinsic activation, but also promotes disease, including kidney
infiltration by T cells (19). This in turn indicates that certain types of
autoreactive B cells that can initially be activated via BCR and TLR
dual signals are subsequently important for broader T cell activation
and disease pathology. Autoreactive T cells are believed to escape
central deletion because they have very low affinity for self Ags.
Cognate autoreactive B cells could concentrate and present self Ag
at levels high enough to induce activation even in very low-affinity
T cells. Conversely, DCs are not needed for the vast majority of
peripheral T cell activation in this lupus model, suggesting that at
best they play a redundant role in this process (3). Although these
findings are consistent with the notion that B cells have nonredundant roles in Ag presentation, the lack of requirement for DCs in
peripheral T cell activation by no means proved that B cells are required. This key fact is something that only B cell–intrinsic deletion
of MHCII could demonstrate.
By incorporating present and prior studies, we present a model
(Fig. 10) in which B cells are the initial APCs for the activation of
autoreactive T cells, something that occurs after T cell–independent/
TLR-dependent activation of the B cell. Subsequent B cell and
T cell expansion and differentiation—both of which result in
target organ damage—depend on B cell–expressed MHCII. Once
there has been substantial T cell activation and epitope spreading,
T cells that infiltrate organs will be sustained by CD11c+ cells in
an ICOSL-dependent, MyD88-independent fashion (19, 30). In
target organs, we propose that previously activated infiltrating
T cells can provide CD40L signals to DCs to induce optimal costimulatory signals from DCs. This is consistent with the fact that
MyD88-dependent signals are dispensable in DCs with respect to
kidney disease. The next step in defining this schema is to better
understand the nature and regulation of the autoreactive T cells that
help B cells and promote tissue damage.
B CELL–SPECIFIC MHCII DELETION IN LUPUS
The Journal of Immunology
34. Serreze, D. V., H. D. Chapman, D. S. Varnum, M. S. Hanson, P. C. Reifsnyder,
S. D. Richard, S. A. Fleming, E. H. Leiter, and L. D. Shultz. 1996.
B lymphocytes are essential for the initiation of T cell-mediated autoimmune
diabetes: analysis of a new “speed congenic” stock of NOD.Ig m null mice. J.
Exp. Med. 184: 2049–2053.
35. Serreze, D. V., S. A. Fleming, H. D. Chapman, S. D. Richard, E. H. Leiter, and
R. M. Tisch. 1998. B lymphocytes are critical antigen-presenting cells for the
initiation of T cell-mediated autoimmune diabetes in nonobese diabetic mice. J.
Immunol. 161: 3912–3918.
36. Ahuja, A., J. Shupe, R. Dunn, M. Kashgarian, M. R. Kehry, and M. J. Shlomchik.
2007. Depletion of B cells in murine lupus: efficacy and resistance. J. Immunol.
179: 3351–3361.
37. Bekar, K. W., T. Owen, R. Dunn, T. Ichikawa, W. Wang, R. Wang, J. Barnard,
S. Brady, S. Nevarez, B. I. Goldman, et al. 2010. Prolonged effects of short-term
anti-CD20 B cell depletion therapy in murine systemic lupus erythematosus.
Arthritis Rheum. 62: 2443–2457.
38. Molnarfi, N., U. Schulze-Topphoff, M. S. Weber, J. C. Patarroyo,
T. Prod’homme, M. Varrin-Doyer, A. Shetty, C. Linington, A. J. Slavin,
J. Hidalgo, et al. 2013. MHC class II-dependent B cell APC function is required
2579
39.
40.
41.
42.
43.
for induction of CNS autoimmunity independent of myelin-specific antibodies.
J. Exp. Med. 210: 2921–2937.
Noorchashm, H., Y. K. Lieu, N. Noorchashm, S. Y. Rostami, S. A. S. Greeley,
A. Schlachterman, H. K. Song, L. E. Noto, A. M. Jevnikar, C. F. Barker, and
A. Naji. 1999. I-Ag7-mediated antigen presentation by B lymphocytes is critical
in overcoming a checkpoint in T cell tolerance to islet b cells of nonobese diabetic mice. J. Immunol. 163: 743–750.
Shimoda, M., T. Li, J. P. S. Pihkala, and P. A. Koni. 2006. Role of MHC class II
on memory B cells in post-germinal center B cell homeostasis and memory
response. J. Immunol. 176: 2122–2133.
Jevnikar, A. M., M. J. Grusby, and L. H. Glimcher. 1994. Prevention of nephritis
in major histocompatibility complex class II-deficient MRL-lpr mice. J. Exp.
Med. 179: 1137–1143.
Wofsy, D., J. A. Ledbetter, P. L. Hendler, and W. E. Seaman. 1985. Treatment of
murine lupus with monoclonal anti-T cell antibody. J. Immunol. 134: 852–857.
Peng, S. L., S. Fatenejad, and J. Craft. 1996. Induction of nonpathologic, humoral autoimmunity in lupus-prone mice by a class II-restricted, transgenic a b
T cell: separation of autoantigen-specific and -nonspecific help. J. Immunol. 157:
5225–5230.
Downloaded from http://www.jimmunol.org/ by guest on August 9, 2017