* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The immune response in atherosclerosis: a double
Monoclonal antibody wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
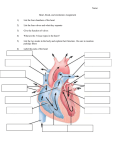
REVIEWS The immune response in atherosclerosis: a double-edged sword Göran K. Hansson*‡ and Peter Libby‡§ Abstract | Immune responses participate in every phase of atherosclerosis. There is increasing evidence that both adaptive and innate immunity tightly regulate atherogenesis. Although improved treatment of hyperlipidaemia reduces the risk for cardiac and cerebral complications of atherosclerosis, these remain among the most prevalent of diseases and will probably become the most common cause of death globally within 15 years. This Review focuses on the role of immune mechanisms in the formation and activation of atherosclerotic plaques, and also includes a discussion of the use of inflammatory markers for predicting cardiovascular events. We also outline possible future targets for prevention, diagnosis and treatment of atherosclerosis. Plaque An atherosclerotic lesion consisting of a fibrotic cap surrounding a lipid-rich core. The lesion is the site of inflammation, lipid accumulation and cell death. Also known as an atheroma. *Center for Molecular Medicine, Department of Medicine, Karolinska University Hospital, Karolinska Institute, Stockholm, SE-17176, Sweden. ‡ Leducq Transatlantic Network of Excellence in Cardiovascular Research, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts, USA. § Donald W. Reynolds Cardiovascular Clinical Research Center, Department of Medicine, Brigham and Women’s Hospital and Harvard Medical School, Boston, Massachusetts 02115, USA. Correspondence to P.L. e-mail: [email protected] doi:10.1038/nri1882 Published online 16 June 2006 Atherosclerosis is an inflammatory disease characterized by intense immunological activity, which increasingly threatens human health worldwide1. Atherosclerosis involves the formation in the arteries of lesions that are characterized by inflammation, lipid accumulation, cell death and fibrosis. Over time, these lesions, which are known as atherosclerotic plaques, mature and gain new characteristics. Although clinical complications of atherosclerosis can arise from plaques causing flow-limiting stenoses, the most severe clinical events follow the rupture of a plaque, which exposes the prothrombotic material in the plaque to the blood and causes sudden thrombotic occlusion of the artery at the site of disruption. In the heart, atherosclerosis can lead to myocardial infarction and heart failure; whereas in the arteries that perfuse the brain, it can cause ischaemic stroke and transient ischaemic attacks. If atherosclerosis affects other arterial branches, it can result in renal impairment, hypertension, abdominal aortic aneurysms and critical limb ischaemia. As our knowledge of this disease increases, we increasingly recognize that there is no simple answer to the question of whether the immune response promotes or retards atherogenesis. Indeed, the two arms of the immune response can either promote or attenuate aspects of atherosclerosis and its complications. This Review summarizes our current understanding of the role of adaptive immunity in atherosclerosis and, in particular, weighs the evidence regarding the yin and yang of the immune response at various places and times in the evolution of this lengthy and complex disease. We do not discuss the arteriosclerosis of allografted transplants, which is a distinct disease with a unique pathogenesis, although it might represent an extreme case of immune-driven arteriopathy. Immunological features of atherosclerosis In humans, atherosclerotic plaques contain blood-borne inflammatory and immune cells (mainly macrophages and T cells), as well as vascular endothelial cells, smooth muscle cells, extracellular matrix, lipids and acellular lipid-rich debris2. These lesions typically present as asymmetrical focal thickenings of the intima, which is the innermost layer of the artery (FIG. 1). Accumulation of immune cells and lipid droplets in the intima occurs during the first stage of plaque formation. Lipid-laden macrophages, known as foam cells, outnumber other cells in early plaques (which are known as fatty streaks), but these nascent plaques also contain T cells. Fatty streaks are prevalent in young individuals, never cause symptoms, and can progress into mature atherosclerotic plaques or disappear with time. Mature plaques (also known as atheromas) have a more complex structure than fatty streaks (FIG. 1). In the centre of a plaque, foam cells and extracellular lipid droplets form a core region that is surrounded by a cap of smooth muscle cells and a collagen-rich matrix2. Other cell types present in plaques include dendritic cells (DCs)3, mast cells4, a few B cells2 and probably natural killer T (NKT) cells. The shoulder region of the plaque, which is where it grows, and the interface between the cap and the core have particularly abundant accumulations of T cells and macrophages2. Many of these immune cells show signs of activation and produce proinflammatory cytokines such as interferon-γ (IFNγ) and 508 | JULY 2006 | VOLUME 6 www.nature.com/reviews/immunol © 2006 Nature Publishing Group REVIEWS Endothelial cell Blood-vessel lumen Shoulder Normal artery Intima Elastic lamina Cellular debris and cholesterol Media Media Cholesterol Dead cell Dendritic cell Foam cell Macrophage Mast cell Monocyte Smooth muscle cell T cell Figure 1 | Cellular composition of atherosclerotic plaques. The atherosclerotic plaque has a core containing lipids (which include esterified cholesterol and cholesterol crystals) and debris from dead cells. Surrounding it, a fibrous cap containing smooth muscle cells and collagen fibres stabilizes the plaque. Immune cells including macrophages, T cells and mast cells populate the plaque, and are frequently in an activated state. They produce cytokines, proteases, prothrombotic molecules and vasoactive substances, all of which can affect plaque inflammation and vascular function. Until complications occur, an intact endothelium covers the plaque. Myocardial infarction An episode of acute cardiac ischaemia that leads to death of heart muscle cells. It is usually caused by a thrombotic atherosclerotic plaque. Ischaemic stroke An episode of acute regional ischaemia in the brain leading to nerve-cell death. It is usually caused by thrombi or emboli from atherosclerotic plaques. Aneurysm The local dilatation of an artery caused by weakening of the artery wall. Some, but not all, aneurysms are caused by atherosclerosis. Intima The innermost layer of an artery, which consists of loose connective tissue and is covered by a monolayer of endothelium. Atherosclerotic plaques form in the intima. Fibrous cap A structure composed of a dense collagen-rich extracellular matrix with occasional smooth muscle cells, macrophages and T cells that typically overlies the characteristic central lipid core of plaques. tumour-necrosis factor (TNF)5. With time, the plaque can progress into an even more complex lesion, the lipid core of which has become a paucicellular pool of cholesterol deposits surrounded by a fibrous cap of varying thickness. The fibrous cap prevents contact between the blood and the pro-thrombotic material in the lesion (FIG. 1). Disruption of the cap can lead to thrombosis and many of the adverse clinical outcomes associated with atherosclerosis. Models of atherogenesis in mutant mice Direct analysis of the early phases of human atherosclerosis presents obvious obstacles. Therefore, systematic investigation of the mechanisms that initiate atherosclerosis relies on animal models of the disease. The available observations indicate that there is substantial overlap between disease development in these animal models and the human disease. Two strains of genetically altered mice have been particularly fruitful in this regard. Apoe–/– mice lack apolipoprotein E (APOE; which is a key component in cholesterol metabolism), and develop spontaneous hypercholesterolaemia and atherosclerotic disease (which is exacerbated by an atherogenic diet) that progresses to myocardial infarction and stroke6,7. Low-density-lipoprotein receptor (LDLR)-deficient mice respond to being fed with fat by developing hypercholesterolaemia and atherosclerotic plaques8. The crossbreeding of these mice with mice that carry deletions in genes encoding crucial components of the immune system has provided important information on the role of the immune system in the pathogenesis of atherosclerosis. In addition, bone-marrow transplantation of, and spleen-cell transfer to, Apoe–/– or Ldlr –/– mice has offered insights into the role of specific populations of bone-marrow-derived cells in disease development. Immune-cell recruitment initiates atheroscleroticplaque formation. In experimental animals, endothelial cells in the arteries express leukocyte adhesion molecules, in particular vascular cell-adhesion molecule 1 (VCAM1), as part of the initial vascular response to cholesterol accumulation in the intima9 (FIG. 2a). The patchy distribution of adhesion-molecule expression corresponds to the subsequent position at which fatty streaks form10. This patchy pattern of expression probably reflects haemodynamic factors, because the shear stresses and disturbed fluid flows vary over the arterial bed in a similar way to the predilection sites for atherosclerosis. Interestingly, exposing cultured endothelial cells to oscillatory shear stress that mimics arterial blood flow increases the expression of several leukocyte adhesion molecules11. Shortly after VCAM1 induction, monocytes and T cells enter the arterial intima (FIG. 2a). Under the influence of macrophage colony-stimulating factor (M-CSF) produced by endothelial cells and smooth muscle cells12, the monocytes differentiate into macrophages13 (FIG. 2b) and T cells can undergo antigen-dependent activation (FIG. 2c; see later). Interestingly, VCAM1 expression by the endothelium ceases after a few weeks, but smooth muscle cells begin to express this adhesion molecule14. Expression of VCAM1 and other adhesion molecules by smooth muscle cells might promote the recruitment and retention of mononuclear cells in the arterial intima. NATURE REVIEWS | IMMUNOLOGY VOLUME 6 | JULY 2006 | 509 © 2006 Nature Publishing Group REVIEWS a T cell d Monocyte Increased adhesion molecules Increased permeability Increased propensity for thrombus formation Blood-vessel lumen LDL VLA4 VCAM1 Endothelial cell T cell Endothelial cell oxLDL Chemokine receptor Chemokine IFNγ TNF CD40L b TLR T cell Proteases Pro-inflammatory mediators TH1 cell Endothelial cell TCR Scavenger receptor LPS, HSP60 or oxLDL Macrophage CD40 MHC class II oxLDL Smooth muscle cell M-CSF Monocyte Macrophage Pro-inflammatory cytokines Proteases Procoagulants Pro-apoptotic factors Decreased collagen production Decreased proliferation Foam cell e c T cell T cell Endothelial cell Endothelial cell CD4+ T cell TH1 cell Macrophage TGFβ TH2 cell or regulatory T cell IL-10 IL-12 IL-15 IL-18 TCR TH1 cell MHC class II TGFβ APC Smooth muscle cell Decreased inflammation Figure 2 | Recruitment and activation of immune cells in atherosclerotic plaques. a | Low-density lipoprotein (LDL) diffuses from the blood into the innermost layer of the artery, where LDL particles can associate with proteoglycans of the extracellular matrix. The LDL of this extracellular pool is modified by enzymes and oxygen radicals to form molecules such as oxidized LDL (oxLDL). Biologically active lipids are released and induce endothelial cells to express leukocyte adhesion molecules, such as vascular cell-adhesion molecule 1 (VCAM1). Monocytes and T cells bind to VCAM1-expressing endothelial cells through very late antigen 4 (VLA4) and respond to locally produced chemokines by migrating into the arterial tissue. b | Monocytes differentiate into macrophages in response to local macrophage colony-stimulating factor (M-CSF) and other stimuli. Expression of many pattern-recognition receptors increases, including scavenger receptors and Toll-like receptors (TLRs). Scavenger receptors mediate macrophage uptake of oxLDL particles, which leads to intracellular cholesterol accumulation and the formation of foam cells. TLRs bind lipopolysaccharide (LPS), heat-shock protein 60 (HSP60), oxLDL and other ligands, which instigates the production of many pro-inflammatory molecules by macrophages. c | T cells undergo activation after interacting with antigen-presenting cells (APCs), such as macrophages or dendritic cells, both of which process and present local antigens including oxLDL, HSP60 and possibly components of local microorganisms. A T helper 1 (TH1)-cell-dominated response ensues, possibly owing to the local production of interleukin-12 (IL-12), IL-18 and other cytokines. Antigen presentation and TH1-cell differentiation might also occur in regional lymph nodes. d | TH1 cells produce inflammatory cytokines including interferon-γ (IFNγ ) and tumour-necrosis factor (TNF) and express CD40 ligand (CD40L). These messengers prompt macrophage activation, production of proteases and other pro-inflammatory mediators, activate endothelial cells, increase adhesion-molecule expression and the propensity for thrombus formation, and inhibit smooth-muscle-cell proliferation and collagen production. e | Plaque inflammation might be attenuated in response to the anti-inflammatory cytokines IL-10 and transforming growth factor-β (TGFβ), which are produced by several cell types including regulatory T cells, macrophages, and for TGFβ, also vascular cells and platelets. TCR, T-cell receptor. 510 | JULY 2006 | VOLUME 6 www.nature.com/reviews/immunol © 2006 Nature Publishing Group REVIEWS Experiments using genetically altered mice show that leukocyte adhesion molecules participate in the initiation of atherosclerosis. Apoe–/– mice that are also deficient for both endothelial-cell selectin (E-selectin) and platelet selectin (P-selectin) have reduced severity of atherosclerosis15. Similarly, Ldlr –/– mice that express a truncated form of VCAM1 with impaired function develop less severe disease than those expressing wild-type VCAM1 (REF. 16). Such studies use truncated VCAM1 because complete VCAM1 deficiency is lethal at the embryonic stage. In addition to the expression of adhesion molecules, several chemokines produced by vascular cells guide the recruitment of immune cells (FIG. 2a). Data obtained using knockout mice show a key role for CC-chemokine ligand 2 (CCL2; also known as MCP1) and its receptor, CC-chemokine receptor 2 (CCR2), in the initiation of atherosclerosis17,18. Indeed, absence of CCL2 or CCR2 limits the entry of monocytes and T cells into the arterial intima and inhibits atherogenesis. Macrophages and vascular cells of the forming plaque also produce the T-cell attractants CCL5 (also known as RANTES), CXC-chemokine ligand 10 (CXCL10; also known as IP10) and CXCL11 (also known as ITAC)19, the mastcell attractant CCL11 (also known as eotaxin)20 and also the Janus molecule CXCL16, which can function as both a scavenger receptor and a chemokine21. Administration of a blocking form of CCL5 attenuates atherogenesis in mice22. Atherosclerotic plaques in humans and mice also express another chemokine, the cell-surface anchored CX 3 -chemokine ligand 1 (CX 3 CL1; also known as fractalkine), which is a transmembrane protein preferentially expressed by smooth muscle cells. CX3CL1 that is shed by proteolysis can engage CX3-chemokine receptor 1 (CX3CR1), which is expressed by monocytes and macrophages. Ligation of CX3CR1 on blood-borne monocytes stimulates their migration to the artery wall and contributes to atherogenesis, as indicated by studies using mice deficient for both APOE and CX3CR1 (REFS 23,24). Scavenger receptors Cell-membrane proteins that take up oxidatively or otherwise modified low-density lipoproteins. Innate immunity and lipid accumulation Monocyte-derived macrophages abound in plaques and are outnumbered only by vascular smooth muscle cells in some plaques. Several phenotypes of macrophage are found in plaques, including inflammatory macrophages and also foam cells, which develop when cholesteryl esters accumulate in the cytosol of intimal macrophages (FIG. 2b). Cholesterol derives from lipoproteins that have undergone oxidation or enzymatic modification in the tissue. This renders the lipoprotein particle amenable to uptake by macrophages that express scavenger receptors25, a family of proteins that includes CD36, CD68, CXCL16, lectin-type oxidized low-density lipoprotein receptor 1 (LOX1), scavenger receptor A (SR-A) and SR-B1 . Scavenger receptors are pattern-recognition receptors (PRRs) that mediate internalization and lysosomal degradation of modified lipoprotein particles, lipopolysaccharide, fragments of malaria parasites and apoptotic bodies26. Uptake by scavenger receptors does not lead directly to inflammation but can lead to MHC-class-II-restricted antigen presentation of internalized material, thereby linking innate and adaptive immunity 27. Considering their role in the formation of foam cells, one would expect scavenger receptors to have an important, if not crucial, role in atherogenesis. However, recent results showing increased, rather than decreased, atherosclerosis in mice lacking CD36, CXCL16 or SR-A have cast doubt on this conclusion28. This might be because receptor-mediated internalization of modified lipoproteins by macrophages can facilitate the eventual elimination of these particles from plaques through high-density-lipoprotein-dependent mechanisms29. If, as a result of the absence of foam cells, this clearance of modified lipoprotein did not occur, removal of such lipids from plaques would be less efficient and the accumulation of extracellular cholesterol in the lipid pool might be more detrimental than the presence of foam cells. Whereas scavenger receptors mediate internalization, degradation and antigen presentation of ligands, Toll-like receptors (TLRs) can elicit inflammatory responses directly 30. The many TLR-family members that can be detected in plaques are expressed mainly by macrophages and endothelial cells31. By contrast, in the normal artery wall, only TLR2 and TLR4 are expressed by endothelial cells and the underlying smooth muscle cells do not express TLRs. Therefore, plaque formation causes a considerable increase in the repertoire of PRRs expressed by the artery wall. A broad range of pathogen-associated molecular patterns can ligate the different TLRs30. Among them, microbial components, heat-shock proteins (HSPs) and unmethylated CpG DNA might be directly relevant to atherogenesis because several microorganisms are associated with atherosclerosis. In addition, some data indicate that endogenous HSP60 and oxidized LDL (oxLDL) bind TLR4–CD14 complexes and elicit inflammatory responses32–34. Following ligation, TLRs activate nuclear factor-κB (NF-κB) and mitogen-activated protein kinase– activator protein 1 signalling pathways 30,32. Direct immunohistochemical analysis has shown that a large proportion of the TLR4-expressing cells in human plaques have nuclear translocation of NF-κB, which is consistent with a role for TLR4 ligation in inflammatory activation in the plaques31. The response downstream of TLR ligation in the plaque probably involves the secretion of pro-inflammatory cytokines and matrix metalloproteinases (MMPs), as well as the production of low-molecular-weight inflammatory mediators such as nitric oxide and endothelin-1 (REF. 30). Genetic deficiency of TLR4 or its signal-transducing adaptor molecule myeloid differentiation primary-response gene 88 (MyD88) reduces plaques in mice35,36. T cells promote atherogenesis Human atherosclerotic plaques contain numerous T cells. In a plaque, ~40% of the cells express macrophage markers, ~10% are CD3+ T cells and most of the remainder have the characteristics of smooth muscle NATURE REVIEWS | IMMUNOLOGY VOLUME 6 | JULY 2006 | 511 © 2006 Nature Publishing Group REVIEWS cells2. Small populations of mast cells, B cells and DCs occur in plaques and, together with T cells, monocytes and macrophages, might traffic between the blood in the arterial lumina, the lesioned artery wall, the vasa vasorum — microvessels that penetrate the artery — and the regional lymph nodes. The ratio of CD4 + to CD8 + T cells in advanced plaques resembles that found in peripheral blood2. Most T cells are αβ T cells, but there is also a small proportion of γδ T cells. Lesions of early stages of experimental atherosclerosis contain oligoclonal expansions of CD4+ cells expressing an αβ T-cell receptor (TCR)37, indicating activation in response to a limited set of local antigens (FIG. 2c). The CD4+ T cells that are isolated from human plaques are mostly CD45RO-expressing memory and/or effector T cells38. An initial round of T-cell activation in response to ‘athero-antigens’ might occur in the regional lymph nodes, possibly after antigen presentation by DCs trafficking from the plaque to the lymph node39. After entering the blood, previously activated memory and/or effector T cells bind cell-surface adhesion molecules that are expressed by endothelial cells at the plaque surface and/or in the vasa vasorum, and then enter the plaque. Macrophages in the plaque expressing MHC class II molecules might then present antigen to these T cells, leading to further rounds of activation. Very recently, Ath1, which is an atherosclerosis susceptibility locus on mouse chromosome 1, was mapped to the gene encoding OX40 ligand (OX40L; also known as TNFSF4), which is a co-stimulatory factor for T-cell activation40. Reduced expression of this protein was associated with reduced atherosclerosis in inbred strains that differ in their Tnfsf4 alleles and also in mice carrying a targeted deletion of this gene40. Polymorphisms in human TNFSF4 were found to be associated with coronary atherosclerosis and with an increased risk for myocardial infarction in a human genetic epidemiology study 40. These data re-emphasize the importance of immune activation in atherosclerosis and its complications41. Vasa vasorum Small nutrient vessels in the normal adventitia and outer media of the artery wall, which can also give rise to microvessels in the plaque. Plaque antigens activate local cellular adaptive immunity. Cloning T cells from surgically removed human plaques has identified several cell-mediated, local adaptive immune reactions. CD4+ T-cell clones derived from plaques recognize oxLDL, with other clones recognizing HSP60 or other antigens derived from certain pathogenic microorganisms, such as Chlamydia pneumoniae 42,43 (FIG. 2c). In all of these cases, antigen recognition was restricted by HLA-DR and involved αβ TCR+ CD4+ T cells42,44,45. Antigen-presenting cells selectively internalize oxLDL particles through the scavenger-receptor pathway. After proteolytic processing, fragments of the protein component of LDL, APOB, bind nascent MHC class II molecules and traffic to the cell surface. Indeed, APOB fragments are among the peptides displayed most frequently by HLA-DR molecules in cultured human lymphoblastoid cells46. Therefore, receptor-mediated endocytosis and the antigen-presentation pathway facilitate MHC class II presentation of LDL-derived peptides to CD4+ T cells. As expected, no T cells react with native LDL components. However, oxidative modification of LDL breaks tolerance and oxLDL-reactive T cells localize in plaques, lymph nodes, and in the blood of patients with atherosclerosis and experimental animals42,47. OxLDL-reactive CD4 + T cells probably recognize APOB-derived oligopeptides carrying adducts formed during oxidation48; whereas oxLDL-specific antibodies react with oxidized phospholipids such as phosphorylcholine49,50, as well as aldehyde-peptide epitopes including malondialdehyde-lysine42,44,45. Most oxLDL-reactive CD4+ T cells have a T helper 1 (TH1)-cell phenotype42,47. Because TH1 cytokines (such as IFNγ) generally stimulate pro-atherosclerotic processes (see later), these T cells probably promote atherogenesis, a conclusion supported by adoptive-transfer studies in severe combined immunodeficient (SCID) mice lacking APOE51. As expected, these mice show substantially reduced atherosclerotic plaques compared with immunocompetent Apoe–/– mice. Transfer of CD4+ T cells from immunocompetent Apoe–/– mice to SCID mice lacking ApoE increases the atherogenesis found in immunodeficient mice, to almost the same level as that found in fully immunocompetent Apoe–/– mice. Therefore, the net effect of CD4+ T cells is to increase atherogenesis in mice susceptible to atherosclerotic disease. Obviously, this finding does not preclude the existence of T-cell subsets that might mitigate disease. Recent studies have identified transcripts encoding Vα14Jα281-containing TCR α-chains in plaques of hypercholesterolaemic mice, indicating the presence of NKT cells52. The abundance of CD1 molecules in plaques53 indicates that CD1-mediated NKT-cell activation takes place, but the absence of specific markers for NKT cells has hampered direct immunohistological demonstration of NKT cells in plaques. However, administration of ligands that specifically activate NKT cells to Apoe–/– mice shows that NKT-cell activation increases early atherosclerotic plaque development concomitantly with increased local expression of pro-inflammatory cytokines, whereas abrogation of CD1-mediated antigen presentation reduces disease52,54. Therefore, NKT cells contribute to atherosclerosis, probably by antigenspecific activation in response to lipid antigens present in plaques. A role for T H1/T H2-cytokine balance? Analyses of cell-surface-marker expression and cytokine secretion indicate activation of a remarkably large proportion of T cells in plaques38. TH1-type cytokines dominate in mouse models of atherosclerosis and in human plaques. For example, human plaques contain cells producing IFNγ, interleukin-12 (IL-12), IL-15, IL-18 and TNF, but few cells producing the TH2-type cytokine IL-4 (REFS 42,55,56). Together with the histopathological features of accumulation of macrophages and T cells, the predominance of TH1-type cytokines indicates that atherosclerosis is a TH1-cell-driven disease (FIG. 2d) . This hypothesis is supported by studies in genetically altered mice that show that there is reduced atherosclerosis in hypercholesterolaemic mice lacking 512 | JULY 2006 | VOLUME 6 www.nature.com/reviews/immunol © 2006 Nature Publishing Group REVIEWS IFNγ or its receptor57,58, IL-12 (REF. 59), IL-18 (REF. 60), TNF61 or the TH1-cell-inducing transcription factor T-bet 62. Administration of recombinant IFNγ 63 or the TH1-cell-inhibiting drug pentoxifyllin64 to hypercholesterolaemic mice led to increased and decreased atherosclerosis, respectively, lending further support to this hypothesis64. If TH1 cytokines stimulate plaque formation and TH2 cytokines inhibit TH1-cell responses, can TH2-cell responses protect against atherosclerosis? In support of this proposition, C57BL/6 mice (which are prone to TH1-type immune responses) develop fatty streaks if fed a high-cholesterol diet, whereas BALB/c mice (which are prone to T H 2-type immune responses) are resistant to atherogenesis 65,66. Targeted deletion of the gene encoding signal transducer and activator of transcription 6 (STAT6), a transcription factor that is essential for the differentiation of TH2 cells, renders BALB/c mice susceptible to atherogenesis and this occurs in parallel with a switch from TH2-cell to TH1-cell responses66. Although these studies of the development of fatty streaks indicate opposing roles for TH1 and TH2 cells in disease development, mice that develop more advanced plaques show a more complicated picture. Pharmacological inhibition of TH1 cells using pentoxifyllin or IL-18-binding protein inhibits atherosclerosis in Apoe–/– mice64,67, and administration of recombinant TH1 cytokines (recombinant IL-18 and IFNγ) exacerbates disease 63,68. However, data for IL-4, which is the prototypic TH2 cytokine, are inconclusive. Some studies have shown that IL-4 has a protective effect, whereas others found reduced disease in the absence of IL-4 (REFS 59,69). These divergent findings, under different experimental conditions, might reflect the complex range of biological activities found for IL-4, including stimulation of scavenger-receptor expression and the induction of elastin degrading MMP12, which can lead to aneurysm formation70. Defining the role of TH2 cells in atherosclerosis, therefore, requires further study. Tissue factor A procoagulant that stimulates thrombus formation, when in contact with blood, by accelerating the action of factors VIIa and Xa. Pro-atherosclerotic action of TH1 cells. How can TH1 cells promote disease development? IL-12 and IL-18, which are produced by macrophages and smooth muscle cells in plaques, can indirectly affect the development of plaques by promoting TH1-cell differentiation. By contrast, IFNγ and TNF directly accelerate disease through their actions on macrophages and vascular cells (FIG. 2c,d). IFNγ activates macrophages, thereby increasing their production of nitric oxide, pro-inflammatory cytokines, and pro-thrombotic and vasoactive mediators. Additionally, IFNγ inhibits endothelial-cell proliferation71, the proliferation and differentiation of vascular smooth muscle cells72, and also decreases collagen production by these smooth muscle cells73. Decreasing the cell and collagen content of the fibrous cap might reduce the stability of the plaque. Therefore, the combined effects of IFNγ on cells of the forming plaque promote inflammation and extracellular-matrix destabilization. The pro-inflammatory cytokine TNF triggers vascular inflammation through the NF-κB pathway, inducing the production of reactive oxygen and nitrogen species, proteolytic enzymes and pro-thrombotic tissue factor by endothelial cells, and modulates the fibrinolytic capacity of the cells74–76. TNF also has profound metabolic effects that include the suppression of lipoprotein lipase, which leads to the accumulation of triglyceride-rich lipoproteins in the blood. Such lipoproteins, and the TNF levels, have been associated with heart disease in clinical studies77–79. Genetic loss-of-function studies also support the idea that TNF has a pro-atherogenic role61. CD40 and CD40L: a co-stimulatory dyad with proatherogenic action. The cell-surface proteins CD40 and CD40 ligand (CD40L; also known as CD154) have several similarities to soluble pro-inflammatory cytokines. CD40 ligation on cells found in plaques triggers an inflammatory response similar to that elicited by TNF, that is, secretion of other cytokines and MMPs, and expression of adhesion molecules80. Importantly, CD40 ligation causes expression of the procoagulant tissue factor by human macrophages, something that soluble pro-inflammatory cytokines do not do. Macrophages and T cells express CD40 and CD40L, as do vascular endothelial cells, smooth muscle cells and platelets81,82. Therefore, CD40 ligation propagates inflammatory activation in all the main cell types involved in atherogenesis. Inhibition of CD40 ligation and inactivation of the gene encoding CD40L reduces atherosclerotic plaques in hypercholesterolaemic mice83,84. Unfortunately, CD40 blockade in humans can promote platelet aggregation and thrombosis, which is an obstacle to its clinical application. Anti-atherogenic immunity Anti-inflammatory cytokines. Although local cellular immunity predominantly promotes atherosclerosis through the action of cell-surface molecules (such as CD40–CD40L) and cytokines (such as IFNγ and TNF), counterbalancing factors can function to dampen disease activity (FIG. 2e). Two anti-inflammatory cytokines, IL-10 and transforming growth factor-β (TGFβ), provide particularly important atheroprotective signals. Two groups have reported previously that IL-10deficient C57BL/6 mice that consume a fatty diet develop an increased quantity of fatty streaks compared with wild-type mice85,86. By contrast, Il10 transgenic C57BL/6 mice do not develop fatty streaks, thereby providing evidence of a protective role for IL-10 in atherosclerosis85,86. The mouse model used in these early studies mimicked the initial stage of atherogenesis, but the mice did not develop lesions similar to human clinical disease. However, subsequent experiments using Apoe–/– mice, which develop atherosclerotic lesions that are more similar to those found in humans, also show an atheroprotective role for IL-10 (REF. 87). Interestingly, IL-10 promotes arteriopathy in transplanted hearts, indicating a more complex picture. The pluripotent cytokine TGFβ has many effects on a diverse range of cell types and can inhibit atherosclerosis at least as well as IL-10. For example, TGFβ promotes NATURE REVIEWS | IMMUNOLOGY VOLUME 6 | JULY 2006 | 513 © 2006 Nature Publishing Group REVIEWS collagen production, which could increase plaque stability. Treatment with tamoxifen, which is a TGFβstimulating oestrogen-receptor agonist, reduces the formation of fatty streaks in C57BL/6 mice fed with fat88, whereas administration of TGFβ-specific blocking antibodies or decoy receptors for TGFβ reduces atherosclerotic plaque formation in Ldlr –/– mice89,90. However, these studies did not identify the mechanism of action of TGFβ. Two more-recent studies show that TGFβ exerts its atheroprotective effects by modulating T-cell activation. In the first study, crossbreeding mice carrying dominantnegative TGFβ receptors (that were expressed under the control of the Cd4 promoter) with Apoe–/– mice led to a fivefold increase in plaque size and advanced plaques were found in the proximal aorta of 12-weekold crossbred mice91. Notably, the plaques showed signs of increased inflammation and had fewer interstitial collagen fibres, a characteristic of human plaques that cause thrombosis (see later). In the second study, bone marrow from mice that expressed a dominant-negative form of the type II TGFβ receptor (that was expressed under the control of the Cd2 promoter) was transplanted to irradiated Ldlr –/– mice92. Again, plaques showed signs of substantial inflammation and a poorly developed collagenous matrix. These studies show the important atheroprotective effects of TGFβ that occur through the dampening of T-cell activity. Several cell types can produce TGFβ and IL-10, including platelets, macrophages, endothelial cells, smooth muscle cells and regulatory T cells. Activation of regulatory T cells could therefore offer a means of antigen-specific atheroprotection (FIG. 2e). A recent study supports this idea by showing that the transfer of natural CD4+CD25+ regulatory T (TReg) cells reduces atherosclerosis, whereas depletion of CD25+ cells increases disease in Apoe–/– mice93. Depletion of CD25+ cells in mice lacking functional TGFβ receptors on T cells did not alter plaque size, indicating that this cytokine mediates the atheroprotective effect of regulatory T cells93. Humoral immunity. In addition to innate immunity and T cells, antibodies with different specificities can participate in atherosclerosis. Humans and experimental animals with disease have antibodies specific for oxLDL particles44. B-cell epitopes in oxLDL include amino-acid residues of APOB that are modified by lipid peroxidation products, such as malondialdehyde and 4-hydroxynonenal. Although some clinical and epidemiological studies have found positive correlations between the presence of antibodies specific for oxLDL and the progression of atherosclerosis94,95, other studies have not detected any correlation. Interestingly, antibodies specific for oxLDL, mainly of the IgM isotype, also circulate in asymptomatic humans96 and crossreact with apoptotic bodies 49. These antibodies bind the oxidized phospholipids in oxLDL and also recognize phosphorylcholine in the cell wall of Streptococcus pneumoniae49. Phosphorylcholine-specific IgM consists of germline-encoded antibodies of the T15 type that are produced by B1 cells49. Therefore, expansion of B-cell clones that produce T15-type antibodies, for example during a pneumococcal infection, might affect the development of plaques. Indeed, immunization of Ldlr –/– mice with a pneumococcal vaccine reduced the extent of atherosclerosis50. Molecular mimicry could explain the crossreactivity between the humoral immune responses to oxLDL, apoptotic bodies and pneumococci. This mechanism might also apply to HSP60, another antigen associated with atherosclerosis97. HSP60 is a chaperone molecule that is involved in protein folding and can be detected in plaques. Antibodies specific for HSP60 are found in experimental animals that have atherosclerosis and have been correlated with disease progression in a human cohort study98. Present in prokaryotes and eukaryotes, HSP60 has shown remarkable sequence conservation during evolution. As antibodies specific for HSP60 crossreact between microbial and eukaryotic HSP60, antibodies that react to human HSP60 can be generated in response to infection with microbes that express HSP60, such as C. pneumoniae99. Several further experimental, and some human, studies show that humoral immunity can protect against atherosclerosis. Splenectomy increases atherosclerosis in both Apoe–/– mice and humans100. In Apoe–/– mice, transfer of splenic B cells from atherosclerotic animals into splenectomized recipients protects against disease, possibly because of the production of protective antibodies by B cells100. Immunization experiments identify oxLDL and HSP60 as important antigens that can induce protective, as well as detrimental, immune responses (TABLE 1; see also later). A tentative conclusion from these studies is that TH1-type immune responses promote disease; whereas humoral immunity has protective effects, possibly by eliminating antigens before they reach plaques. Adaptive immunity disrupts plaques In general, the gravest clinical complications of atherosclerosis result from the sudden thrombotic occlusion of an artery101. The sudden onset of myocardial infarction, as well as many strokes and episodes of acute limb ischaemia, is caused by thrombi that arise from atherosclerotic plaques that do not necessarily tightly narrow the artery. Therefore, many episodes of damage to the heart muscle, brain or lower extremities can occur without warning, all too often with devastating consequences. Physical disruption of a plaque is the most frequent cause of thrombotic occlusions. Indeed, the most frequent patho-anatomical substrate for sudden coronary thrombosis is rupture of the fibrous cap that overlies the lipid core of the plaque101 (FIG. 3). Fibres of interstitial collagens (types I and III) normally confer biomechanical stability on the fibrous cap of the plaque. As discussed earlier, the TH1-cytokine IFNγ strongly inhibits the production of interstitial collagens by vascular smooth muscle cells, which are the main source in the arterial wall of this extracellular-matrix macromolecule73. IFNγ can also inhibit the proliferation of smooth muscle cells, thereby reducing the stabilizing and collagensynthesizing cellular component of the plaque72. Also, 514 | JULY 2006 | VOLUME 6 www.nature.com/reviews/immunol © 2006 Nature Publishing Group REVIEWS Table 1 | Immunization against atherosclerosis in experimental models Antigen Route Animal model Effect on atherosclerosis MDA-LDL Subcutaneous WHHL rabbits Reduced 124 oxLDL Subcutaneous Fat-fed NZW rabbits Reduced 125 –/– References MDA-LDL Subcutaneous Apoe mice Reduced 47,126 MDA-LDL Subcutaneous Ldlr–/– mice Reduced 127 –/– APOB-peptides Subcutaneous Apoe mice Reduced 95,128 MDA-LDL Subcutaneous Cd4–/–Apoe–/– mice Reduced 129 –/– HSP65 Subcutaneous Ldlr mice Increased 130 HSP65 Peroral/nasal Ldlr–/– mice Reduced 131,132 β2-GPI Subcutaneous Ldlr–/– mice Increased 133 APO, apolipoprotein; GPI, glycoprotein I; HSP65, heat-shock protein 65; LDL, low-density lipoprotein; LDLR, LDL receptor; MDA-LDL, malondialdehyde-modified LDL; NZW, New Zealand white; oxLDL, oxidized LDL; WHHL, Watanabe hereditably hyperlipidaemic. Angina pectoris A reversible attack of chest discomfort, usually caused by an imbalance between the oxygen demand of the working heart muscle and the insufficient supply through narrow, atherosclerotic coronary arteries. Angioplasty A percutaneous catheter procedure that inflates a balloon in areas of narrowing (stenosis) in arteries. Statins A class of drugs that inhibit the rate-limiting enzyme (3hydroxy-3-methylglutaryl coenzyme A reductase) in the pathway of cholesterol biosynthesis. proteases elaborated mainly from activated macrophages in plaques can degrade collagen102,103. In addition, ligation of CD40 expressed by macrophages increases the production of matrix-degrading proteases that include the interstitial collagenases of the MMP family, MMP1, MMP8 and MMP13 (REF. 104). Therefore, TH1 cells probably have an essential role in regulating the functions of smooth muscle cells (collagen-fibre formation) and macrophages (collagen degradation) that crucially regulate the integrity of the fibrous cap of the plaque and therefore its susceptibility to rupture and provoke thrombosis. Once coagulation factors in the blood gain access to the lipid core of the plaque following rupture of the fibrous cap, thrombosis commonly ensues. Tissue factor, the potent procoagulant expressed by a subpopulation of macrophages in the lipid core of the plaque, triggers these thromboses101. As noted earlier, ligation of CD40 expressed by macrophages strongly induces expression of tissue factor80. Indeed, T cells expressing CD40L localize in the vicinity of macrophages that are expressing tissue factor in the lipid core of human plaques105. Because platelets can also express CD40L82 when activated, positive feedback can amplify the local inflammatory response, once a thrombus begins to form, because of generation of the protease thrombin induced by tissue factor and platelet activation induced by thrombin. Therefore, although T cells could orchestrate the pathophysiology of plaque disruption, dysregulated antigen-nonspecific pathways probably amplify and sustain the formation of thrombi. Modulation of immunity in atherosclerosis Immunopharmacological intervention against symptomatic atherosclerosis. Although thrombi cause most of the acute complications of atherosclerosis, the gradual formation of stenoses that impede blood flow causes many of the chronic symptoms of atherosclerotic disease, such as angina pectoris (chest discomfort precipitated typically by physical or emotional stress). Recent decades have witnessed important advances in the ability of interventions, particularly percutaneous procedures, to relieve stenoses and reduce ischaemia. Until recently, however, the long-term success of mechanical procedures, such as the deployment of arterial stents (metal scaffolds to hold arteries open) and balloon angioplasty (inflation of miniature balloons in blocked segments of arteries to expand the arterial lumen), has been limited by re-growth of intimal tissue — which is known as in-stent stenosis and restenosis, respectively. This fibro-proliferative response of the injured artery can re-occlude the lumen within months in a substantial minority of patients. Recently, the coating of stents with immunosuppressive agents, for example sirolimus (Rapamycin), has shown striking effectiveness at reducing in-stent stenosis106. This advance has markedly improved clinical outcomes in patients undergoing percutaneous intervention. Early preclinical studies provided the experimental basis for this important therapeutic advance by showing that another immunosuppressant, cyclosporin, reduces intimal-cell proliferation in response to arterial injury 107. The use of statins has shown striking clinical benefit in preventing atherosclerotic complications during the past decade. Numerous clinical trials have established that 3-hydroxy-3-methylglutaryl coenzyme A (HMGCoA) reductase inhibitors (drugs of the statin family) can reduce various atherosclerotic complications108. The lowering of LDL cholesterol concentrations in the blood doubtless accounts for much of this remarkable clinical benefit. However, recent data indicate that part of the clinical benefit of statins occurs because of an anti-inflammatory effect that is apparently not related to LDL reduction109. (See REF. 110 for a detailed discussion of non-LDL-lowering effects of statins). By blocking HMG-CoA reductase, statins prevent the formation of lipids that control the function of several intracellular proteins111. By acting on the MHC class II transactivator (CIITA), statins can interfere with the transcriptional induction of MHC class II molecules, which would decrease immune activation in the plaque112. Statins can also limit the accelerated arteriosclerosis (sclerosis of the arterial walls) that complicates solid-organ transplantation, a disease that often occurs in the absence of increased concentrations of LDL113. They also seem to reduce disease activity in patients with rheumatoid arthritis114 and in mice with experimental autoimmune encephalomyelitis115. All these results lend NATURE REVIEWS | IMMUNOLOGY VOLUME 6 | JULY 2006 | 515 © 2006 Nature Publishing Group REVIEWS support to the idea that the immunomodulatory actions of statins also contribute to their effects in patients with atherosclerosis. Recent studies have established that another category of anti-atherosclerotic drugs, the ligands for a group of nuclear transcription factors known as peroxisomeproliferator-activated receptors (PPARs), can inhibit T-cell activation in vitro. Activators of both PPARα (members of the fibrate class of drugs) and PPARγ (members of the thiazolidinedione family of drugs) can reduce T-cell activation, as was shown by decreased production of IFNγ, TNF and IL-2 (REF. 116). PPARα agonists also inhibit inflammatory activation of vascular smooth muscle cells117. Therefore, activation of PPARα or PPARγ might also affect atherosclerosis in a beneficial manner by blunting the adaptive and innate immune responses. Nonspecific anti-inflammatory therapies, such as non-steroidal anti-inflammatory drugs (NSAIDs), have not improved the cardiovascular outcome. Indeed, treatment with NSAIDs selective for cyclooxygenase-2 seems to increase the risk of thrombotic complications118,119. Despite their marked anti-inflammatory properties, gluco corticosteroids themselves probably increase, rather than decrease, atherogenesis, as chronic administration of these agents adversely affects plasma lipoproteins, promotes insulin resistance and sodium retention, Thrombus Platelet Erythrocyte Fibrin Rupture Blood-vessel lumen Endothelial cell Elastic lamina Cellular debris and cholesterol Peroxisome-proliferatoractivated receptors Nuclear receptors that participate in the regulation of cellular metabolism and differentiation. Thiazolidinedione A class of medication, used to treat diabetes, that binds peroxisome-proliferatoractivated receptor-γ. Cholesterol Dead cell Dendritic cell Foam cell Macrophage Mast cell Monocyte Smooth muscle cell T cell Figure 3 | Plaque activation, rupture and thrombosis. When activated, immune cells including macrophages, T cells and mast cells can release pro-inflammatory cytokines, which reduce collagen formation and induce the expression of tissue factor. Proteases that attack the collagenous cap are also released by activated immune cells. The weakened plaque might fissure when subjected to the forces of arterial blood pressure. Exposure of subendothelial structures and procoagulants such as tissue factor promotes platelet aggregation and thrombosis. A thrombus forms and might occlude the lumen of the artery, leading to acute ischaemia. 516 | JULY 2006 | VOLUME 6 www.nature.com/reviews/immunol © 2006 Nature Publishing Group REVIEWS C-reactive protein An acute-phase reactant protein, the plasma concentration of which increases in inflammatory states. 1. 2. 3. 4. 5. 6. 7. 8. 9. and inhibits collagen and elastin formation. It therefore does not offer a reasonable therapeutic alternative in the chronic phases of atherosclerosis. Vaccination against atherosclerosis? Parenteral immunization with malondialdehyde-modified LDL (that is, LDL with a defined oxidative modification) or malondialdehyde-modified peptides derived from the LDL protein apolipoprotein inhibits atherosclerosis and this occurs in parallel with increased titres of antibody specific for the immunogen (TABLE 1). Interestingly, protection through this route does not require CD4+ T-cell help120. Therefore, protection seems to depend mostly on humoral immunity, at least in this model. By contrast, the outcomes after immunization with HSP60 or its mycobacterial homologue HSP65 are complex (TABLE 1). Parenteral immunization in C57BL/6 mice fed with fat, as well as Ldlr –/– mice, aggravates disease, whereas oral or nasal immunization elicits protective immunity. Induction of mucosal immunity involves activation of regulatory T cells that produce anti-inflammatory cytokines and also high titres of specific antibodies. Therefore, the precise mechanism by which mucosal immunization leads to reduced atherosclerosis remains to be clarified. Although several questions remain, the immunization experiments with malondialdehyde-modified LDL and HSP60 indicate that it is possible that a vaccination strategy might protect against atherosclerosis and its complications. Obviously, many obstacles remain, rendering the success of this approach unpredictable, particularly in humans. Murray, C. J. & Lopez, A. D. Global mortality, disability, and the contribution of risk factors: global burden of disease study. Lancet 349, 1436–1442 (1997). Jonasson, L., Holm, J., Skalli, O., Bondjers, G. & Hansson, G. K. Regional accumulations of T cells, macrophages, and smooth muscle cells in the human atherosclerotic plaque. Arteriosclerosis 6, 131–138 (1986). Bobryshev, Y. V. & Lord, R. S. A. S-100 positive cells in human arterial intima and in atherosclerotic lesions. Cardiovas. Res. 29, 689–696 (1995). Kovanen, P. T., Kaartinen, M. & Paavonen, T. Infiltrates of activated mast cells at the site of coronary atheromatous erosion or rupture in myocardial infarction. Circulation 92, 1084–1088 (1995). Jonasson, L., Holm, J., Skalli, O., Gabbiani, G. & Hansson, G. K. Expression of class II transplantation antigen on vascular smooth muscle cells in human atherosclerosis. J. Clin. Invest. 76, 125–131 (1985). Plump, A. S. et al. Severe hypercholesterolemia and atherosclerosis in apolipoprotein E-deficient mice created by homologous recombination in ES cells. Cell 71, 343–353 (1992). Piedrahita, J. A., Zhang, S. H., Hagaman, J. R., Oliver, P. M. & Maeda, N. Generation of mice carrying a mutant apolipoprotein E gene inactivated by gene targeting in embryonic stem cells. Proc. Natl Acad. Sci. USA 89, 4471–4475 (1992). Ishibashi, S., Goldstein, J. L., Brown, M. S., Herz, J. & Burns, D. K. Massive xanthomatosis and atherosclerosis in cholesterol-fed low density lipoprotein receptor-negative mice. J. Clin. Invest. 93, 1885–1893 (1994). Cybulsky, M. I. & Gimbrone, M. A. Endothelial expression of a mononuclear leukocyte adhesion molecule during atherosclerosis. Science 251, 788–791 (1991). Conclusion The evidence reviewed in this article supports the involvement of the immune response in atherosclerosis from its initiation through to its thrombotic complications. The concept that adaptive immunity pivotally regulates atherogenesis has already been clinically useful. Markers of the acute-phase response, notably C-reactive protein (CRP), predict the prognosis of patients who have already sustained a cardiovascular event121. Lesser elevations of CRP concentration, measured with a highly sensitive assay and previously considered in the ‘normal range,’ can be used to predict cardiovascular events in apparently well populations109,122,123. Markers of heightened innate immune responses, such as CRP, correlate with worse outcomes in individuals with acute coronary syndromes121. Systemic administration of non-selective immunosuppressive drugs will probably not be useful for the treatment of atherosclerosis, at least during its long asymptomatic phase, because of the need for prolonged therapy and the potential toxicities of such treatments. However, the immune system in its full complexity offers much more subtle targets for therapeutic manipulation. As more details emerge of the specific pathways involved in the immune response and the inflammation that occur in atherosclerosis, more selective interventions might prove appropriate for long-term anti-atherosclerotic therapy. Also, as our ability to gauge the risk of acute complications improves, we might be able to target in a much more selective manner those therapies that would otherwise impair host defences if administered on a long-term basis. 10. Nakashima, Y., Raines, E. W., Plump, A. S., Breslow, J. L. & Ross, R. Upregulation of VCAM-1 and ICAM-1 at atherosclerosis-prone sites on the endothelium in the apoE-deficient mouse. Arterioscler. Thromb. Vasc. Biol. 18, 842–851 (1998). 11. Dai, G. et al. Distinct endothelial phenotypes evoked by arterial waveforms derived from atherosclerosis-susceptible and-resistant regions of human vasculature. Proc. Natl Acad. Sci. USA 101, 14871–14876 (2004). 12. Rajavashisth, T. B. et al. Induction of endothelial cell expression of granulocyte and macrophage colony-stimulating factors by modified low-density lipoproteins. Nature 344, 254–257 (1990). 13. Smith, J. D. et al. Decreased atherosclerosis in mice deficient in both macrophage colony-stimulating factor (op) and apolipoprotein E. Proc. Natl Acad. Sci. USA 92, 8264–8268 (1995). 14. Li, H., Cybulsky, M. I., Gimbrone, M. A. & Libby, P. Inducible expression of vascular cell adhesion molecule-1 by vascular smooth muscle cells in vitro and within rabbit atheroma. Am. J. Pathol. 143, 1551–1559 (1993). 15. Dong, Z. M. et al. The combined role of P- and E-selectins in atherosclerosis. J. Clin. Invest. 102, 145–152 (1998). 16. Cybulsky, M. I. et al. A major role for VCAM-1, but not ICAM-1, in early atherosclerosis. J. Clin. Invest. 107, 1255–1262 (2001). 17. Boring, L., Gosling, J., Cleary, M. & Charo, I. F. Decreased lesion formation in CCR2–/– mice reveals a role for chemokines in the initiation of atherosclerosis. Nature 394, 894–897 (1998). 18. Gu, L. et al. Absence of monocyte chemoattractant protein-1 reduces atherosclerosis in low density lipoprotein receptor-deficient mice. Mol. Cell 2, 275–281 (1998). NATURE REVIEWS | IMMUNOLOGY 19. Mach, F. et al. Differential expression of three T lymphocyte-activating CXC chemokines by human atheroma-associated cells. J. Clin. Invest. 104, 1041–1050 (1999). 20. Haley, K. J. et al. Overexpression of eotaxin and the CCR3 receptor in human atherosclerosis: using genomic technology to identify a potential novel pathway of vascular inflammation. Circulation 102, 2185–2189 (2000). 21. Minami, M. et al. Expression of SR-PSOX, a novel cell-surface scavenger receptor for phosphatidylserine and oxidized LDL in human atherosclerotic lesions. Arterioscler. Thromb. Vasc. Biol. 21, 1796–1800 (2001). 22. Veillard, N. R. et al. Antagonism of RANTES receptors reduces atherosclerotic plaque formation in mice. Circ. Res. 94, 253–261 (2004). 23. Combadiere, C. et al. Decreased atherosclerotic lesion formation in CX3CR1/apolipoprotein E double knockout mice. Circulation 107, 1009–1016 (2003). 24. Lesnik, P., Haskell, C. A. & Charo, I. F. Decreased atherosclerosis in CX3CR1–/– mice reveals a role for fractalkine in atherogenesis. J. Clin. Invest. 111, 333–340 (2003). 25. Steinberg, D. Low density lipoprotein oxidation and its pathobiological significance. J. Biol. Chem. 272, 20963–20966 (1997). 26. Peiser, L., Mukhopadhyay, S. & Gordon, S. Scavenger receptors in innate immunity. Curr. Opin. Immunol. 14, 123–128 (2002). 27. Nicoletti, A. et al. The macrophage scavenger receptor type A directs modified proteins to antigen presentation. Eur. J. Immunol. 29, 512–521 (1999). 28. Moore, K. J. et al. Loss of receptor-mediated lipid uptake via scavenger receptor A or CD36 pathways does not ameliorate atherosclerosis in hyperlipidemic mice. J. Clin. Invest. 115, 2192–2201 (2005). VOLUME 6 | JULY 2006 | 517 © 2006 Nature Publishing Group REVIEWS 29. Bodzioch, M. et al. The gene encoding ATP-binding cassette transporter 1 is mutated in Tangier disease. Nature Genet. 22, 347–351 (1999). 30. Janeway, C. A. Jr & Medzhitov, R. Innate immune recognition. Annu. Rev. Immunol. 20, 197–216 (2002). 31. Edfeldt, K., Swedenborg, J., Hansson, G. K. & Yan, Z. Q. Expression of toll-like receptors in human atherosclerotic lesions: a possible pathway for plaque activation. Circulation 105, 1158–1161 (2002). 32. Kol, A., Lichtman, A. H., Finberg, R. W., Libby, P. & Kurt-Jones, E. A. Cutting edge: heat shock protein (HSP) 60 activates the innate immune response: CD14 is an essential receptor for HSP60 activation of mononuclear cells. J. Immunol. 164, 13–17 (2000). 33. Xu, X. H. et al. Toll-like receptor-4 is expressed by macrophages in murine and human lipid-rich atherosclerotic plaques and upregulated by oxidized LDL. Circulation 104, 3103–3108 (2001). 34. Miller, Y. I. et al. Minimally modified LDL binds to CD14, induces macrophage spreading via TLR4/ MD-2, and inhibits phagocytosis of apoptotic cells. J. Biol. Chem. 278, 1561–1568 (2003). 35. Michelsen, K. S. et al. Lack of Toll-like receptor 4 or myeloid differentiation factor 88 reduces atherosclerosis and alters plaque phenotype in mice deficient in apolipoprotein E. Proc. Natl Acad. Sci. USA 101, 10679–10684 (2004). 36. Bjorkbacka, H. et al. Reduced atherosclerosis in MyD88-null mice links elevated serum cholesterol levels to activation of innate immunity signaling pathways. Nature Med. 10, 416–421 (2004). 37. Paulsson, G., Zhou, X., Törnquist, E. & Hansson, G. K. Oligoclonal T cell expansions in atherosclerotic lesions of apoE-deficient mice. Arterioscler. Thromb. Vasc. Biol. 20, 10–17 (2000). 38. Stemme, S., Holm, J. & Hansson, G. K. T lymphocytes in human atherosclerotic plaques are memory cells expressing CD45RO and the integrin VLA-1. Arterioscler. Thromb. 12, 206–211 (1992). 39. Angeli, V. et al. Dyslipidemia associated with atherosclerotic disease systemically alters dendritic cell mobilization. Immunity 21, 561–574 (2004). 40. Wang, X. et al. Positional identification of TNFSF4, encoding OX40 ligand, as a gene that influences atherosclerosis susceptibility. Nature Genet. 37, 365–372 (2005). 41. Swanberg, M. et al. MHC2TA is associated with differential MHC molecule expression and susceptibility to rheumatoid arthritis, multiple sclerosis and myocardial infarction. Nature Genet. 37, 486–494 (2005). 42. Stemme, S. et al. T lymphocytes from human atherosclerotic plaques recognize oxidized low density lipoprotein. Proc. Natl Acad. Sci. USA 92, 3893–3897 (1995). 43. de Boer, O. J. et al. Unstable atherosclerotic plaques contain T-cells that respond to Chlamydia pneumoniae. Cardiovasc. Res. 48, 402–408 (2000). 44. Palinski, W. et al. Low density lipoprotein undergoes oxidative modification in vivo. Proc. Natl Acad. Sci. USA 86, 1372–1376 (1989). 45. Palinski, W. et al. Cloning of monoclonal autoantibodies to epitopes of oxidized lipoproteins from apolipoprotein E-deficient mice. Demonstration of epitopes of oxidized low density lipoprotein in human plasma. J. Clin. Invest. 98, 800–814 (1996). 46. Chicz, R. M. et al. Specificity and promiscuity among naturally processed peptides bound to HLA-DR alleles. J. Exp. Med. 178, 27–47 (1993). 47. Zhou, X., Caligiuri, G., Hamsten, A., Lefvert, A. K. & Hansson, G. K. LDL immunization induces T-celldependent antibody formation and protection against atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 21, 108–114 (2001). 48. Stemme, S. et al. T lymphocytes from human atherosclerotic plaques recognize oxidized LDL. Proc. Natl Acad. Sci. USA 92, 3893–3897 (1995). 49. Shaw, P. X. et al. Natural antibodies with the T15 idiotype may act in atherosclerosis, apoptotic clearance, and protective immunity. J. Clin. Invest. 105, 1731–17340 (2000). 50. Binder, C. J. et al. Pneumococcal vaccination decreases atherosclerotic lesion formation: molecular mimicry between Streptococcus pneumoniae and oxidized LDL. Nature Med. 9, 736–743 (2003). 51. Zhou, X., Nicoletti, A., Elhage, R. & Hansson, G. K. Transfer of CD4+ T cells aggravates atherosclerosis in immunodeficient apolipoprotein E knockout mice. Circulation 102, 2919–2922 (2000). 52. Tupin, E. et al. CD1d-dependent activation of NKT cells aggravates atherosclerosis. J. Exp. Med. 199, 417–422 (2004). 53. Melian, A., Geng, Y. J., Sukhova, G. K., Libby, P. & Porcelli, S. A. CD1 expression in human atherosclerosis. A potential mechanism for T cell activation by foam cells. Am. J. Pathol. 155, 775–786 (1999). 54. Nakai, Y. et al. Natural killer T cells accelerate atherogenesis in mice. Blood 104, 2051–2059 (2004). 55. Uyemura, K. et al. Cross-regulatory roles of interleukin (IL)-12 and IL-10 in atherosclerosis. J. Clin. Invest. 97, 2130–2138 (1996). 56. Frostegard, J. et al. Cytokine expression in advanced human atherosclerotic plaques: dominance of pro-inflammatory (Th1) and macrophage-stimulating cytokines. Atherosclerosis 145, 33–43. (1999). 57. Gupta, S. et al. IFN-γ potentiates atherosclerosis in ApoE knock-out mice. J. Clin. Invest. 99, 2752–2761 (1997). 58. Buono, C. et al. Influence of interferon-γ on the extent and phenotype of diet-induced atherosclerosis in the LDLR-deficient mouse. Arterioscler. Thromb. Vasc. Biol.23, 454–460 (2003). 59. Davenport, P. & Tipping, P. G. The role of interleukin-4 and interleukin-12 in the progression of atherosclerosis in apolipoprotein E-deficient mice. Am. J. Pathol. 163, 1117–1125 (2003). 60. Elhage, R. et al. Reduced atherosclerosis in interleukin-18 deficient apolipoprotein E-knockout mice. Cardiovasc. Res. 59, 234–240 (2003). 61. Branen, L. et al. Inhibition of tumor necrosis factor-α reduces atherosclerosis in apolipoprotein E knockout mice. Arterioscler. Thromb. Vasc. Biol. 24, 2137–2142 (2004). 62. Buono, C. et al. T-bet deficiency reduces atherosclerosis and alters plaque antigen-specific immune responses. Proc. Natl Acad. Sci. USA 102, 1596–1601 (2005). 63. Whitman, S. C., Ravisankar, P., Elam, H. & Daugherty, A. Exogenous interferon-γ enhances atherosclerosis in apolipoprotein E–/– mice. Am. J. Pathol. 157, 1819–1824 (2000). 64. Laurat, E. et al. In vivo downregulation of T helper cell 1 immune responses reduces atherogenesis in apolipoprotein E-knockout mice. Circulation 104, 197–202 (2001). 65. Paigen, B., Morrow, A., Brandon, C., Mitchell, D. & Holmes, P. Variation in susceptibility to atherosclerosis among inbred strains of mice. Atherosclerosis 57, 65–73 (1985). 66. Huber, S. A., Sakkinen, P., David, C., Newell, M. K. & Tracy, R. P. T helper-cell phenotype regulates atherosclerosis in mice under conditions of mild hypercholesterolemia. Circulation 103, 2610–2616 (2001). 67. Mallat, Z. et al. Interleukin-18/interleukin-18 binding protein signaling modulates atherosclerotic lesion development and stability. Circ. Res. 89, E41–E45 (2001). 68. Whitman, S. C., Ravisankar, P. & Daugherty, A. Interleukin-18 enhances atherosclerosis in apolipoprotein E–/– mice through release of interferon-γ. Circ. Res. 90, e34–e38 (2002). 69. King, V. L., Szilvassy, S. J. & Daugherty, A. Interleukin-4 deficiency decreases atherosclerotic lesion formation in a site-specific manner in female LDL receptor–/– mice. Arterioscler. Thromb. Vasc. Biol. 22, 456–461 (2002). 70. Shimizu, K., Shichiri, M., Libby, P., Lee, R. T. & Mitchell, R. N. Th2-predominant inflammation and blockade of IFN-γ signaling induce aneurysms in allografted aortas. J. Clin. Invest. 114, 300–308 (2004). 71. Friesel, R., Komoriya, A. & Maciag, T. Inhibition of endothelial cell proliferation by γ-interferon. J. Cell Biol. 104, 689–696 (1987). 72. Hansson, G. K., Hellstrand, M., Rymo, L., Rubbia, L. & Gabbiani, G. Interferon γ inhibits both proliferation and expression of differentiation-specific α-smooth muscle actin in arterial smooth muscle cells. J. Exp. Med. 170, 1595–1608 (1989). 73. Amento, E. P., Ehsani, N., Palmer, H. & Libby, P. Cytokines and growth factors positively and negatively regulate interstitial collagen gene expression in human vascular smooth muscle cells. Arterioscler. Thromb. 11, 1223–1230 (1991). 74. van Hinsbergh, V. W. M., van den Berg, E. A., Fiers, W. & Dooijewaard, G. Tumor necrosis factor induces the production of urokinase-type plasminogen activator by human endothelial cells. Blood 75, 1991–1998 (1990). 518 | JULY 2006 | VOLUME 6 75. Lee, E. et al. Regulation of matrix metalloproteinases and plasminogen activator inhibitor-1 synthesis by plasminogen in cultured human vascular smooth muscle cells. Circ. Res. 78, 44–49 (1996). 76. Saren, P., Welgus, H. G. & Kovanen, P. T. TNF-α and IL-1β selectively induce expression of 92-kDa gelatinase by human macrophages. J. Immunol. 157, 4159–4165 (1996). 77. Jovinge, S. et al. Evidence for a role of tumor necrosis factor α in disturbances of triglyceride and glucose metabolism predisposing to coronary heart disease. Metabolism 47, 113–118 (1998). 78. Boquist, S. et al. Alimentary lipemia, postprandial triglyceride-rich lipoproteins, and common carotid intima-media thickness in healthy, middle-aged men. Circulation 100, 723–728 (1999). 79. Beutler, B. & Cerami, A. Cachectin and tumour necrosis factor as two sided of the same biological coin. Nature 320, 584–588 (1986). 80. Mach, F., Schoenbeck, U., Bonnefoy, J.-Y., Pober, J. & Libby, P. Activation of monocyte/macrophage functions related to acute atheroma complication by ligation of CD40. Induction of collagenase, stromelysin, and tissue factor. Circulation 96, 396–399 (1997). 81. Mach, F. et al. Functional CD40 ligand is expressed on human vascular endothelial cells, smooth muscle cells, and macrophages- implications for CD40–CD40 ligand signaling in atherosclerosis. Proc. Natl Acad. Sci. USA 94, 1931–1936 (1997). 82. Henn, V. et al. CD40 ligand on activated platelets triggers an inflammatory reaction of endothelial cells. Nature 391, 591–594 (1998). 83. Mach, F., Schönbeck, U., Sukhova, G. K., Atkinson, E. & Libby, P. Reduction of atherosclerosis in mice by inhibition of CD40 signalling. Nature 394, 200–203 (1998). 84. Lutgens, E. et al. Requirement for CD154 in the progression of atherosclerosis. Nature Med. 5, 1313–1316 (1999). 85. Mallat, Z. et al. Protective role of interleukin-10 in atherosclerosis. Circ. Res. 85, e17–e24 (1999). 86. Pinderski Oslund, L. J. et al. Interleukin-10 blocks atherosclerotic events in vitro and in vivo. Arterioscler. Thromb. Vasc. Biol.19, 2847–53 (1999). 87. Caligiuri, G. et al. Interleukin-10 deficiency increases atherosclerosis, thrombosis, and low-density lipoproteins in apolipoprotein E knockout mice. Mol. Med. 9, 10–17 (2003). 88. Grainger, D. J. et al. The serum concentration of active transforming growth factor-β is severely depressed in advanced atherosclerosis. Nature Med. 1, 74–79 (1995). 89. Mallat, Z. et al. Inhibition of transforming growth factor-β signaling accelerates atherosclerosis and induces an unstable plaque phenotype in mice. Circ. Res. 89, 930–934 (2001). 90. Lutgens, E. et al. Transforming growth factor-β mediates balance between inflammation and fibrosis during plaque progression. Arterioscler. Thromb. Vasc. Biol. 22, 975–982 (2002). 91. Robertson, A. K. et al. Disruption of TGF-β signaling in T cells accelerates atherosclerosis. J. Clin. Invest. 112, 1342–1350 (2003). 92. Gojova, A. et al. Specific abrogation of transforming growth factor-β signaling in T cells alters atherosclerotic lesion size and composition in mice. Blood 102, 4052–4058 (2003). 93. Ait-Oufella, H. et al., Natural regulatory T cells control the development of atherosclerosis in mice. Nature Med. 12, 178–180 (2006). 94. Salonen, J. T. et al. Autoantibody against oxidised LDL and progression of carotid atherosclerosis. Lancet 339, 883–887 (1992). 95. Fredrikson, G. N. et al. Identification of immune responses against aldehyde-modified peptide sequences in apoB associated with cardiovascular disease. Arterioscler. Thromb. Vasc. Biol. 23, 872–878 (2003). 96. Shaw, P. X. et al. Human-derived anti-oxidized LDL autoantibody blocks uptake of oxidized LDL by macrophages and localizes to atherosclerotic lesions in vivo. Arterioscler. Thromb. Vasc. Biol. 21, 1333–1339 (2001). 97. Kol, A., Sukhova, G. K., Lichtman, A. H. & Libby, P. Chlamydial heat shock protein 60 localizes in human atheroma and regulates macrophage tumor necrosis factor-α and matrix metalloproteinase expression. Circulation 98, 300–307 (1998). 98. Xu, Q. et al. Association of serum antibodies to heat-shock protein 65 with carotid atherosclerosis. Lancet 341, 255–259 (1993). www.nature.com/reviews/immunol © 2006 Nature Publishing Group REVIEWS 99. Perschinka, H. et al. Cross-reactive B-cell epitopes of microbial and human heat shock protein 60/65 in atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 23, 1060–1065 (2003). 100. Caligiuri, G., Nicoletti, A., Poirier, B. & Hansson, G. K. Protective immunity against atherosclerosis carried by B cells of hypercholesterolemic mice. J. Clin. Invest. 109, 745–753 (2002). 101. Libby, P. & Aikawa, M. Stabilization of atherosclerotic plaques: new mechanisms and clinical targets. Nature Med. 8, 1257–1262 (2002). 102. Henney, A. M. et al. Localization of stromelysin gene expression in atherosclerotic plaques by in situ hybridization. Proc. Natl Acad. Sci. USA 88, 8154–8158 (1991). 103. Galis, Z. S., Sukhova, G. K., Lark, M. W. & Libby, P. Increased expression of matrix metalloproteinases and matrix degrading activity in vulnarable regions of human atherosclerotic plaques. J. Clin. Invest. 94, 2493–2503 (1994). 104. Dollery, C. & Libby, P. Atherosclerosis and proteinase activation. Cardiovasc. Res. 69, 625–635 (2006). 105. Buchner, K. et al. CD40 ligand is selectively expressed on CD4+ T cells and platelets: implications for CD40–CD40L signalling in atherosclerosis. J. Pathol. 201, 288–295 (2003). 106. Poon, M., Badimon, J. J. & Fuster, V. Overcoming restenosis with sirolimus: from alphabet soup to clinical reality. Lancet 359, 619–622 (2002). 107. Jonasson, L., Holm, J. & Hansson, G. K. Cyclosporin A inhibits smooth muscle proliferation in the vascular response to injury. Proc. Natl Acad. Sci. USA 85, 2303–2306 (1988). 108. Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S). Lancet 344, 1383–1389 (1994). 109. Ridker, P. M. et al. C-reactive protein levels and outcomes after statin therapy. N. Engl. J. Med. 352, 20–28 (2005). 110. Greenwood, J., Steinman, L. & Zamvil, S.S. Statin therapy and autoimmune disease: from protein prenylation to immunomodulation. Nature Rev. Immunol. 6, 358–370 111. Takemoto, M. & Liao, J. K. Pleiotropic effects of 3-hydroxy-3-methylglutaryl coenzyme a reductase inhibitors. Arterioscler. Thromb. Vasc. Biol. 21, 1712–1719 (2001). 112. Kwak, B., Mulhaupt, F., Myit, S. & Mach, F. Statins as a newly recognized type of immunomodulator. Nature Med. 6, 1399–1402 (2000). 113. Mehra, M. R. & Raval, N. Y. Metaanalysis of statins and survival in de novo cardiac transplantation. Transplant. Proc. 36, 1539–1541 (2004). 114. McCarey, D. W. et al. Trial of atorvastatin in rheumatoid arthritis (TARA): double-blind, randomised placebocontrolled trial. Lancet 363, 2015–2021 (2004). 115. Youssef, S. et al. The HMG-CoA reductase inhibitor, atorvastatin, promotes a Th2 bias and reverses paralysis in central nervous system autoimmune disease. Nature 420, 78–84 (2002). 116. Marx, N. et al. PPAR activators as antiinflammatory mediators in human T lymphocytes: implications for atherosclerosis and transplantation-associated arteriosclerosis. Circ. Res. 90, 703–710 (2002). 117. Staels, B. et al. Activation of human aortic smoothmuscle cells is inhibited by PPARα but not by PPARγ activators. Nature 393, 790–793 (1998). 118. Fitzgerald, G. A. Coxibs and cardiovascular disease. N. Engl. J. Med. 351, 1709–1711 (2004). 119. Solomon, S. D. et al. Cardiovascular risk associated with celecoxib in a clinical trial for colorectal adenoma prevention. N. Engl. J. Med. 352, 1071–1080 (2005). 120. Mattner, J. et al. Exogenous and endogenous glycolipid antigens activate NKT cells during microbial infections. Nature 434, 525–529 (2005). 121. Liuzzo, G. et al. The prognostic value of C-reactive protein and serum amyloid A protein in severe unstable angina. N. Engl. J. Med. 331, 417–424 (1994). 122. Ridker, P. M., Hennekens, C. H., Buring, J. E. & Rifai, N. C-reactive protein and other markers of inflammation in the prediction of cardiovascular disease in women. N. Engl. J. Med. 342, 836–843 (2000). 123. Danesh, J. et al. C-reactive protein and other circulating markers of inflammation in the prediction of coronary heart disease. N. Engl. J. Med. 350, 1387–1397 (2004). 124. Palinski, W., Miller, E. & Witztum, J. L. Immunization of low density lipoprotein (LDL) receptor-deficient rabbits with homologous malondialdehyde-modified LDL reduces atherogenesis. Proc. Natl Acad. Sci. USA 92, 821–825 (1995). 125. Ameli, S. et al. Effect of immunization with homologous LDL and oxidized LDL on early atherosclerosis in hypercholesterolemic rabbits. Arterioscler. Thromb. Vasc. Biol. 16, 1074–1079 (1996). 126. George, J. et al. Hyperimmunization of apo-E-deficient mice with homologous malondialdehyde low-density lipoprotein suppresses early atherogenesis. Atherosclerosis 138, 147–152 (1998). 127. Freigang, S., Hörkkö, S., Miller, E., Witztum, J. L. & Palinski, W. Immunization of LDL receptor-deficient mice with homologous malondialdehyde-modified and native LDL reduces progression of atherosclerosis by mechanisms other than induction of high titers of antibodies to oxidative neoepitopes. Arterioscler. Thromb. Vasc. Biol.18, 1972–1982 (1998). NATURE REVIEWS | IMMUNOLOGY 128. Fredrikson, G. N. et al. Inhibition of atherosclerosis in apoE-null mice by immunization with apoB-100 peptide sequences. Arterioscler. Thromb. Vasc. Biol.23, 879–884 (2003). 129. Zhou, X., Robertson, A. K., Hjerpe, C. & Hansson, G. K. Adoptive transfer of CD4+ T cells reactive to modified low-density lipoprotein aggravates atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 26, 864–870 (2006). 130. Afek, A. et al. Immunization of low-density lipoprotein receptor deficient (LDL-RD) mice with heat shock protein 65 (HSP-65) promotes early atherosclerosis. J. Autoimmun. 14, 115–121 (2000). 131. Harats, D., Yacov, N., Gilburd, B., Shoenfeld, Y. & George, J. Oral tolerance with heat shock protein 65 attenuates Mycobacterium tuberculosis-induced and high-fat-diet-driven atherosclerotic lesions. J. Am. Coll. Cardiol. 40, 1333–1338 (2002). 132. Maron, R. et al. Mucosal administration of heat shock protein-65 decreases atherosclerosis and inflammation in aortic arch of low-density lipoprotein receptor-deficient mice. Circulation 106, 1708–1715 (2002). 133. George, J. et al. Induction of early atherosclerosis in LDL-receptor-deficient mice immunized with β2-glycoprotein I. Circulation 98, 1108–1115 (1998). Acknowledgements We regret that we have not been able to cite many important papers owing to space limitations. Our research is supported by grants from the Swedish Research Council, Heart-Lung Foundation, European Community, US National Institutes of Health and Leducq Foundation. Competing interests statement The authors declare no competing financial interests. DATABASES The following terms in this article are linked online to: Entrez Gene: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?db=gene APOE | CCL2 | CD14 | CD40 | CD40L | CD68 | CX3CR1 | HSP60 | IFNγ | IL-4 | LDLR | MMP1 | PPARα | PPARγ | TLR4 | TNF | VCAM1 FURTHER INFORMATION Peter Libby’s homepage: http://reynolds.brighamandwomens.org/faculty/libby.asp Göran K. Hansson’s homepage: http://www.ki.se/medicin/medicine_ks/experimental_ cardiovascular_research_unit/index_en.html Access to this links box is available online. VOLUME 6 | JULY 2006 | 519 © 2006 Nature Publishing Group