* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lecture 20 Final Exam Preparation Part 1
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Jatene procedure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Artificial heart valve wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Aortic stenosis wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
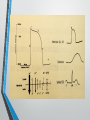
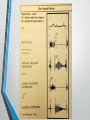
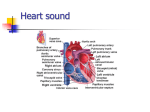
Lecture 20 Adult Echocardiography Final Exam Preparation Part 1 Harry H. Holdorf PhD, MPA, RDMS, RVT Action Potential: Myocardial cellular level • Phase 0 • Phase 1 • Phase 2 • Phase 3 • Phase 4 depolarization, rapid influx of sodium Brief repolarization , potassium exits cell Excitation-contraction coupling-influx of calcium early repolarization- sodium/potassium pump. Sodium and calcium are pumped out and potassium in. Resting membrane potential-sodium and calcium remain inside and potassium ions remain inside During what phase does contraction occur? • Phase 2 Cellular influx of which of the following ions results in contraction? • calcium How does the vagus nerve stimulation affect heart rate? • Vagus nerve stimulation decreases HR Normal timing of the aortic and mitral valves White arrow: Mitral diastolic flow Black arrow: Aortic Systolic flow Valve clicks: Isovolumic contraction and relaxation time Mitral stenosis or Aortic Regurgitation: which occurs first? • Aortic regurgitation is first Mitral Regurgitation or Aortic stenosis: Which occurs first? • Mitral regurgitation is first Any regurgitant lesion is first, as it will include the isovolumic periods Normal timing of left sided pressures • The first heat sound involves? • Atrioventricular (mitral and tricuspid valves) closing Heart sounds • First: • Second • Third • Fourth closure of mitral and tricuspid valves Closure of aortic A2 and pulmonic P2 valves Early diastolic ventricular inflow Atrial contraction Which is louder the first or second heart sound? • First heart sound (mitral and tricuspid closure) What caused the third heart sound? • Rapid, early diastolic flow into a stiff (non-compliant) ventricle In patients with A-fib, which heart sound would be missing? • Fourth (occurs during atrial contraction) Thrill • A palpable murmur; one that can be felt. • Murmurs of grade V or VI have associated thrills. A pansystolic (holosystolic) apical murmur which radiates to the axilla is: • Mitral regurgitation Phonocardiography • • • • • • • Murmurs are created by abnormal blood flow A diamond shaped flow pattern (crescendo-decrescendo) is a flow murmur and is created by a stenotic valve Systolic crescendo-decrescendo murmurs arise from stenotic valves that have flow across them during systole. This means that the murmur is due to aortic stenosis or pulmonic stenosis. Aortic stenosis murmurs radiate to the left side of the sternum. Pulmonic stenosis murmurs radiate to the left side Diastolic crescendo-decrescendo murmurs arise from stenotic valves that have flow across them in diastole. This means that the murmur is due to mitral or tricuspid stenosis Mitral stenosis murmurs are located at the apex or the left side. Tricuspid stenosis murmurs are located in the mid-sternum. • • • • • • • Any term other than crescendo-decrescendo such as pansystolic, holosystolic, or decrescendo is created by a regurgitant flow. Remember: crescendo-decrescendo means stenotic. Systolic murmurs other than crescendo-decrescendo (such as holosystolic murmurs) arise from regurgitant valves that have flow across them in systole. This means that the murmur is doe to mitral regurgitation or tricuspid regurgitation. Mitral regurgitation murmurs are located on the left side. Tricuspid regurgitation murmurs are located closer to the suprasternal notch. Diastolic murmurs other than crescendo-decrescendo (such as diastolic decrescendo murmurs) arise from regurgitant valves that have flow across them in diastole. This means that the murmur is due to aortic or pulmonic regurgitation. Aortic regurgitation murmurs are located at the apex. Pulmonic regurgitation murmurs are located closer at the mid sternum. RIGHT SIDED MURMURS ARE MORE LIKELY TO BE AFFECTED BY RESPIRATION. A patient with a systolic ejection murmur and diminished A2 has? • Aortic stenosis Abnormal pressures and volumes • Congestive heart failure: Pump failure. Fatigue, shortness of breath, peripheral edema, and abdominal distention • Hypovolemic shock: Volume loss. Unable to maintain Blood pressure. • Left to right vs. right to left shunts • • Most cardiac shunts (VSDs & ASDs) shunt left to right due to higher left sided pressure. Right sided enlargement and increased pressure. • Eisenmenger’s Syndrome: PHTN from long-standing left to right shunt and the reversal of the shunt to right to left. • Cor Pulmonale: Heart disease secondary to disease of the lung. PHTN, RV hypertrophy, dilatation. • Tamponade: increased intra-pericardial pressure causes impaired ventricular filling and decreased cardiac output. • Constrictive pericarditis: Fibrosis, thickening of the pericardium restricting diastolic filling. Doppler • Maximum flow is then the Doppler beam is parallel to flow. Pulsed wave vs. Continuous wave • Pulsed wave • Continuous wave Range resolution Aliasing No range resolution No aliasing What is the typical gradient range for aortic stenosis? • 3.0 – 5.0 m/sec Which valve lesion has the highest Doppler peak? • Mitral regurgitation Characteristics of Flow • Laminar • Blood cells move in the same direction with similar velocities: bullet shaped. Also called parabolic • Turbulent • Disturbed flow. Blood cells move in different directions with varying velocities creating vortices Laminar flow is… • smooth In Laminar flow, where is the area of highest velocity? • The center What is smooth flow in the same direction called? • Laminar or parabolic Factors affecting flow • Pressure gradient: Driving pressure • Length of blood vessel: Longer the vessel the greater the resistance • Diameter of blood vessel: smaller the vessel the greater the resistance • Blood viscosity: Higher hematocrit equals higher resistance (decreased velocity, and lower hematocrit equals lower resistance (increased velocity) Factors affecting jet size • • • • • • • Flow volume Color Doppler Gain Frame rate Size and configuration of orifice Size and configuration of receiving chamber Other inflow into the receiving chamber Pressure drop across the orifice Which has the most impact on color Doppler Jet size? • Gain Color Flow Doppler • Separate imaging and color flow processors • Pulsed Doppler technique • Multi-gate systems • Mean velocity estimator • Angle dependent In the apical 5 chamber view, what color is normal left ventricular outflow tract flow? • blue What would you do to prevent ghosting? • Increase wall filter (because the flashes are low velocity What is ghosting in color Doppler? • Flashes of color caused by moving anatomic structures other than blood flow. Medicines • Basic Pharmacology Routes of Drug Administration • Topical: local effect- applied where action is desired • Eye drops, ear drops, skin applications for allergy testing… • Enteral: desired effect is systemic – via digestive tract • By mouth via tables, capsules, or drops- Gastric feeding tube-rectally • Parenteral: Systemic-other routes than the digestive tract • Injection- into vein, artery, muscle, inhalation, subcutaneous • Antihypertensives: beta blockers • Anticoagulants: Heparin (promotes the action of antithrombin III, Coumadin (interferes with the production of vitamin K dependent clotting factors) • Aspirin • Calcium channel blockers • Chronotropic agents: increases the heart rate • Inotropic agents: increase the stroke volume by increasing cardiac contraction • Nitrates: for occasional angian • Oxygen • Sedatives – valium, demeral • Vasopressors: act by causing constriction of blood vessels, thus increasing blood pressure • Diuretics: nephron in the kidney • ACE inhibitors: inhibits angio-tensin converting enzyme which results in vasodilation • Contrast agents: Normal saline is often injected via venous access to r/o atrial shunts, persistent left SVC. Allergic Reactions • Anaphylactic Shock • The severest form of allergy, which is a medical emergency. • Antihistamines Benadryl- for treatment of allergic reactions to blood or plasma. • Epinephrine: plays a central role in the short-term stress reaction “fight-orflight” . It is secreted by the adrenal medulla. • Adverse reactions to epinephrine • • • • Palpitations Tachycardia Hypertension Acute pulmonary edema Antiarrhythmics • Antiarrhythmics are used to treat heart rhythm disorders. • • • • • • • Heart palpitations Irregular heartbeats Fast heartbeats Lightheadedness Fainting Chest pain Shortness of breath • Lidocaine: used to restore a regular heartbeat in patients with arrhythmia. • Digitalis: used to treat congestive heart failure and heart rhythm problems (atrial arrhythmias) • Atropine: used to treat bradycardia, asystole and pulseless electoral activity in cardiac arrest. Analgesics • Analgesics: any of a diverse group of drugs used to relieve pain. • • Aspirin: reduce fever and inflammation as well as pain Morphine: acts upon receptors in the brain and spinal cord to decrease the feeling of pain. Treatment of Angina • Nitroglycerin: treats angina pectoris (suffocating chest pain). Occurs when the coronary arteries become constricted and are not able carry sufficient oxygen to the heart muscle. • Beta-adrenergic blocking agents • • Reduces the heart rate and strength of cardiac muscle contractions, thus reducing the heart’s demand for oxygen. Calcium channel blockers • • Reduces the rate at which calcium ions differs into cardiac muscles. Controls the force of heart contractions and reduce arrhythmia, tachycardia, and hypertension. Dilate coronary blood vessels and increase blood flow to cardiac muscle. Others • Antihypertensive agents • • Treats hypertension. Reduce blood pressure and reduce the work required by the heart to reduce blood and myocardial consumption. • Anticoagulants • • Prevent clot formation. Asprin