* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Hepatology: Anatomy, Physiology and Dev
Survey
Document related concepts
Peptide synthesis wikipedia , lookup
Genetic code wikipedia , lookup
Proteolysis wikipedia , lookup
Citric acid cycle wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Biosynthesis wikipedia , lookup
Butyric acid wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Biochemistry wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Transcript
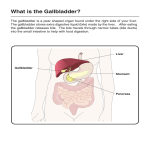
-The liver has diaphragmatic and visceral surfaces which contact the diaphragm and abdominal viscera, respectively. Note the right triangular, left triangular, and coronary ligaments that attach to the diaphragm. Note also the bare area not covered by peritoneum. Anteriorly, there is a fold of peritoneum connecting the liver to the umbilicus called the falciform ligament, which contains the round ligament or ligamentum teres. It is the remnant of the umbilical vein that brought oxygenated blood from the placenta to the fetus heart. The ligamentum venosum is the remnant of the fetal ductus venosus that shunted blood from the umbilical vein to the inferior vena cava to bypass the liver. In the adult liver, the porta hepatis includes the hepatic arteries from the hepatic artery proper, the hepatic portal vein, and the hepatic and cystic ducts joining to form the common bile duct. - The portal vein brings nutrients and other compounds absorbed by the GI tract to be stored and/or processed. - Anatomical lobes: Note how the inferior vena cava, gallbladder, ligamentum teres, ligamentum venosum, and porta hepatis form an “H” shape on the visceral surface. It divides the liver into 4 anatomical lobes based on outer appearance – the right, left, caudate, and quadrate lobes. - Functional lobes: These are based on the distribution of the hepatic arteries, portal vein, and hepatic bile duct. -The liver and gallbladder play important roles in digestion via the production and storage of bile. The liver is also the major organ for metabolism and detoxification. The pancreas also produces digestive enzymes to break down proteins, sugars, and fats. - The processes described above are the exocrine functions of the liver and gallbladder. But they also have endocrine roles, secreting compounds into the bloodstream. The hepatocytes produce albumin, fibrinogen, and thrombin, for example. The pancreatic islets produce insulin, glucagon, and somatostatin. - The liver, gallbladder, and pancreas receive blood supply from the celiac trunk. One main branch is the common hepatic artery, leading to the hepatic artery proper that branches into left and right hepatic arteries to supply the liver. The right hepatic artery gives off the cystic artery to supply the gallbladder. - The pancreas is supplied by multiple vessels. The body and tail are supplied by the dorsal, inferior, and great pancreatic arteries, which all branch off the splenic artery (another main branch of the celiac trunk). The head, neck, and uncinate process are supplied by anastomoses of arteries branching off the celiac trunk and superior mesenteric artery. The gastroduodenal artery, from the common hepatic artery, divides into the anterior and posterior superior pancreaticoduodenal arteries. They anastomose with inferior branches of the inferior pancreatico-duodenal artery from the superior mesenteric artery. The same arteries supply the duodenum. Sole blood supply to the bile duct is through the hepatic artery via the cystic artery Reduced blood flow through the hepatic artery causes ischemic injury to the extrahepatic bile ducts Ischemia or damage to the bile duct often leads to injury, fibrosis, stricture - The liver is divided into many hepatic lobules. Inflow to the liver involves hepatic arteries, which bring oxygenated blood to hepatic tissue, and portal veins, which bring nutrients and other compounds absorbed by the GI tract to be processed and/or stored in the liver. Outflow also involves two routes – hepatic veins which drain into the inferior vena cava and the common hepatic duct which joins the cystic duct and empties bile into the duodenum. - Major characteristics of the liver are portal triads (labeled “portal” in bottom left and shown in the middle) and central veins (labeled in bottom left and shown in the right). Red arrows indicate direction of blood flow within blood sinusoids flanking cords of liver cells. - Note the portal triad contains 1) the portal vein, 2) the hepatic artery, and 3) the bile duct. Each has its typical appearance. The central vein is lined with endothelial cells, with perforations into which the sinusoids empty. - Once again, inflow to the liver involves oxygenated blood via hepatic arteries and absorbed nutrients and compounds from the GI tract via the hepatic portal veins. - All venous drainage from the GI tract and abdominal visceral organs enters the portal system back to the liver. The overall order is as following: arteries → capillaries → veins → portal vein → hepatic sinusoids → veins → vena cava → heart. - In contrast, the caval system is as following: arteries → capillaries → veins → vena cava → heart. Obviously, this is the circulatory system within the rest of the body. - The portal and caval system are not exclusive from each other. There are 4 sites of portocaval anastomoses: - 1) esophageal veins - 2) paraumbilical veins - 3) rectal veins - 4) retroperitoneal veins - If there is liver damage or cirrhosis – accumulation of fibrous tissue that constricts the sinusoids – there may be portal hypertension. This may lead to varicose veins at the 4 sites of anastomoses. Anatomy of Liver Acinus bile duct hepatic artery portal vein blood flow bile portal triad sinusoids Michigan Histology Collection central vein HV PV American Gastroenterological Association Space of Disse Other serum proteins Albumin Kupffer Cell Tissue macrophage Filtration device bacteria, endotoxin Releases inflammatory mediators that influence hepatocytes positively or negatively Looking Down a Sinusoid at a Kupffer Cell Poised to Grab Passing Bacteria Ito Cell/Fat-storing Cell Rare cell, located in sinusoids under endothelium Stores lipophilic materials such as Vitamin A Stimulated by chronic inflammation/alcohol converts to myofibroblast produces collagen and extracellular matrix Responsible for much of the excess fibrotic material in cirrhosis Ito Cell (Fat-storing Cell) on a Sinusoid (S) Defects in Glucose Metabolism in Liver Disease Acute liver failure: Hypoglycemia (rapid neuronal death) Chronic liver disease: Insulin resistance and diabetes (unknown mechanism) UREA Fatty acid metabolism within hepatocytes albumin FABP hepatocyte free fatty acid pool to mitochondria for energy cholin e esterification to TAG excess glucose, amino acids Apo B100 VLDL cholesterol esters Regents of the University of Michigan Greater Role of the Liver in Production and Metabolism of Lipoproteins and Lipids HDL Chol. LDL Cholesterol Gut Liver Chylomycrons TG CM remnants TG VLDL-TG BILE Cholesterol Bile acids Phospholipids Fatty Liver with Inflammation Liver as Protein Synthetic Machine Vena cava systemic outflow Liver synthesizes and secretes: Lipoproteins Albumin Clotting factors Anti-proteases (α1-anti-trypsin) Fibrinogen Complement factors Ceruloplasmin Transferrin and other binding proteins Hepatic artery carries arterial blood with blood proteins Portal vein carries venous blood from intestine, spleen and pancreas Protein Secretion Defects in Liver Disease Example Clinical Consequence Albumin Decreased plasma oncotic pressure/ edema Decreased binding of hydrophobic compounds Clotting factors : Decreased factors II, VII, IX and X Increased bleeding Fibrinogen Decreased fibrin formation in clotting Defects in Protein Synthesis/release also cause liver disease: Alpha1-Anti-trypsin Deficiency Image of pathophysiology of alpha-1anti-trypsin deficiency removed PAS Stain Showing Retained Globs of Mutant Alpha1 Anti-trypsin Protein in Hepatocyte ER Lipoprotein release: another liver synthetic function VLDL: a combination of fat and protein Bile Formation Transports material to the intestine for excretion Drugs, toxins, xenobiotics Cholesterol Bilirubin Copper Transports bile acids to the intestine to aid in fat absorption Organic acid synthesized in liver from cholesterol Conjugated to amino acids Secreted in bile - essential for fat digestion/absorption Reabsorbed in distal ileum and returned to liver via portal vein Cholesterol: Flat (planar) hydrophobic compound OH Metamorphosis to a bile acid you now have a tri-hydroxy bile acid: cholic acid OH COOH OH OH One more change conjugation of an amino acid to the side chain yields Taurocholate (taurine conjugated cholic acid) OH CO NH OH COOH OH Bile acids cycle between the liver and the small intestine. Bile acid synthesis Total bile acid pool is about 3 grams. Liver About 90% of bile acids are reabsorbed in the terminal ileum. However about 5-10% of bile acids are lost daily into the colon. Effect? Small bowel Colon Liver synthesizes about 5-10% of the total bile acid pool each day. Resection of 40 cm of the terminal ileum will result in what problem? Bile acid synthesis Bile acid loss into the cecum will increase. What will this cause? Liver Liver upregulates bile acid synthesis and bile acid pool remains normal. Fat absorption remains the same. Colon 40 cm resection of terminal ileum Bile acid synthesis Resection of >100 cm of the terminal ileum will result in what problem? Liver Initially, bile acid loss into the colon will be massive. What will be the initial effect of this loss of bile acids into the colon? Colon >100 cm resection of terminal ileum Resection of > 100 cm of the terminal ileum will result in what problem over time? Bile acid synthesis Liver upregulates bile acid synthesis but cannot keep up with loss rate. Bile acid pool is reduced Fat is malabsorbed. Liver Colon > 100 cm resection of terminal ileum As the bile acid pool falls, loss into the colon is less per day and secretory diarrhea due to bile acids converts to steatorrhea (+ secretory diarrhea from fatty acids). Cholestyramine: bile acid binding resin that removes bile acids from the enterohepatic circulation Bile acid synthesis Liver Liver upregulates bile acid synthesis (using up what compound in the process?) If liver cannot keep up, what happens? Small bowel Colon Less free bile acid in the colon causes what? Liver takes up and excretes many other organic compounds: bilirubin is the classic and historic example Hepatic Bilirubin Transport SER RBC breakdown in RES UDP-glucuronide + Unconj BR Conj BR Unconj Bilirubin Unconj BR Bile Canaliculus Conj BR MRP-2: Multispecific organic anion transporter Conj BR AT P Blood Hepatocyte Conjugated bilirubin Glutathione S-conjugates other organic anions Hepatic Bilirubin Transport and Mechanisms of Hyperbilirubinemia Gilbert's syndrome (mild) Crigler-Najjar syndrome (severe) SER Hemolysis Unconj Bilirubin Bile Canaliculus Unconj BR Conj BR Multispecific organic anion transporter Conj BR AT P Conjugated bilirubin Glutathione S-conjugates other organic anions Blood Hepatocyte Dubin-Johnson syndrome Rotor's syndrome ?estrogen/cyclosporin Bilirubin conjugation is an example Many other organic compounds undergo two-step biotransformation Example: cholesterol to bile acids After biotransformation, metabolites excreted Larger, lipophilic molecules excreted in bile Smaller (<400 Da) transported to blood and excreted by kidneys Prometheus Bound P.P.Reubens An early case of of hepatic regeneration P. P. Rubens Hypoglycemia Poor blood clotting Cholestasis and jaundice Increased blood ammonia - affects cognitive function Decreased drug disposition Abnormal lipid metabolism Liver exhibits a wide range of functions Liver diseases may cause malfunction of one or more normal function Functions regulated separately so any one liver disease can affect each to a different extent Liver diseases cause: Altered liver functions Altered tests of liver injury At the end of this presentation students should be able to: 1. Describe the basic organization of the liver cell plate and its functional consequences: a. Blood supply b. Configuration of hepatocytes c. Configuration of other liver cells d. Concentration gradients in sinusoidal blood. 2. Describe the basic physiological processes the liver utilizes to accomplish function: a. transport b. metabolism c. biotransformation d. synthesis e. secretion 3. Be able to give examples of the consequences of liver damage on above processes. 4. Be able to give examples of possible consequences of liver disease/injury on liver barrier function and hepatic regeneration. Cystic artery sole supply to bile duct Dual Blood Supply of Liver liver Hepatic artery: 20% Portal vein: 80% spleen pancreas Regents of the University of Michigan Liver has dual blood supply: 80% portal vein 20% hepatic artery Increased vena caval pressure/hepatic vein obstruction? Decreased hepatic artery blood flow? and/or Decreased portal vein blood flow? Effects on the bile duct? Normal Budd-Chiari Hemorrhage in pericentral area; hepatic vein obscured Dilated upstream sinusoids; atrophic/ischemic hepatocytes Decreased inflow: ischemic infarction Liver Cell Anatomy: Consider functional consequences Image showing relationship between sinusoid, sinusoid lining cells, and hepatocyte removed. Scanning Electron micrograph of Liver The Liver: The Body’s Refinery Defects in Glucose Metabolism in Liver Disease Acute liver failure: Hypoglycemia (rapid neuronal death) Chronic liver disease: Insulin resistance and diabetes (unknown mechanism) UREA Fatty acid metabolism within hepatocytes albumin FABP hepatocyte free fatty acid pool to mitochondria for energy cholin e esterification to TAG excess glucose, amino acids Apo B100 VLDL cholesterol esters Regents of the University of Michigan Greater Role of the Liver in Production and Metabolism of Lipoproteins and Lipids HDL Chol. LDL Cholesterol Gut Liver Chylomycrons TG CM remnants TG VLDL-TG BILE Cholesterol Bile acids Phospholipids Fatty Liver with Inflammation Liver as Protein Synthetic Machine Vena cava systemic outflow Liver synthesizes and secretes: Lipoproteins Albumin Clotting factors Anti-proteases (α1-anti-trypsin) Fibrinogen Complement factors Ceruloplasmin Transferrin and other binding proteins Hepatic artery carries arterial blood with blood proteins Portal vein carries venous blood from intestine, spleen and pancreas Protein Secretion Defects in Liver Disease Example Clinical Consequence Albumin Decreased plasma oncotic pressure/ edema Decreased binding of hydrophobic compounds Clotting factors : Decreased factors II, VII, IX and X Increased bleeding Fibrinogen Decreased fibrin formation in clotting Defects in Protein Synthesis/release also cause liver disease: Alpha1-Anti-trypsin Deficiency Image of pathophysiology of alpha-1anti-trypsin deficiency removed PAS Stain Showing Retained Globs of Mutant Alpha1 Anti-trypsin Protein in Hepatocyte ER Lipoprotein release: another liver synthetic function VLDL: a combination of fat and protein The unique position and blood supply of the liver also affect liver physiology Anatomy of Liver Acinus bile duct hepatic artery portal vein blood flow bile portal triad sinusoids Michigan Histology Collection central vein Peri-central vein (hepatic vein) clotted off with ischemic damage to hepatocytes Peri-central ischemia HV clot Peri-portal normal tissue Not all liver cells are alike. Substances found in higher concentrations in the portal vein •Albumin •CPS •FABP •HMG CoA Substances found in higher concentrations in the hepatic vein •P450s •ADH •C7αH •Cysteine •GR •Gluatamate α2µG •GS •GLUT-1 α-KG Normal cells PV HV Necrosis Bile Formation Transports material to the intestine for excretion Drugs, toxins, xenobiotics Cholesterol Bilirubin Copper Transports bile acids to the intestine to aid in fat absorption Organic acid synthesized in liver from cholesterol Conjugated to amino acids Secreted in bile - essential for fat digestion/absorption Reabsorbed in distal ileum and returned to liver via portal vein Bile Acid Cholesterol Cholesterol: Flat (planar) hydrophobic compound OH Metamorphosis to a bile acid OH Lose the double bond Metamorphosis to a bile acid OH Shorten the side chain Metamorphosis to a bile acid COOH OH Add a carboxylic acid group and bend this below the plane of the rings Metamorphosis to a bile acid COOH OH Add a hydroxyl group that is bent down OH Metamorphosis to a bile acid Add another hydroxyl group OH COOH OH OH Metamorphosis to a bile acid you now have a tri-hydroxy bile acid: cholic acid OH COOH OH OH One more change conjugation of an amino acid to the side chain yields Taurocholate (taurine conjugated cholic acid) OH CO NH OH COOH OH Conjugated tri-OH Bile Acid Hydrophobic side OH- OH- OH- COOHydrophilic side Bile acids from intestine To intestine for fat digestion Bile acids cycle between the liver and the small intestine. Bile acid synthesis Total bile acid pool is about 3 grams. Liver About 90% of bile acids are reabsorbed in the terminal ileum. However about 5-10% of bile acids are lost daily into the colon. Effect? Small bowel Colon Liver synthesizes about 5-10% of the total bile acid pool each day. Resection of 40 cm of the terminal ileum will result in what problem? Bile acid synthesis Bile acid loss into the cecum will increase. What will this cause? Liver Liver upregulates bile acid synthesis and bile acid pool remains normal. Fat absorption remains the same. Colon 40 cm resection of terminal ileum Bile acid synthesis Resection of >100 cm of the terminal ileum will result in what problem? Liver Initially, bile acid loss into the colon will be massive. What will be the initial effect of this loss of bile acids into the colon? Colon >100 cm resection of terminal ileum Resection of > 100 cm of the terminal ileum will result in what problem over time? Bile acid synthesis Liver upregulates bile acid synthesis but cannot keep up with loss rate. Bile acid pool is reduced Fat is malabsorbed. Liver Colon > 100 cm resection of terminal ileum As the bile acid pool falls, loss into the colon is less per day and secretory diarrhea due to bile acids converts to steatorrhea (+ secretory diarrhea from fatty acids). Cholestyramine: bile acid binding resin that removes bile acids from the enterohepatic circulation Bile acid synthesis Liver Liver upregulates bile acid synthesis (using up what compound in the process?) If liver cannot keep up, what happens? Small bowel Colon Less free bile acid in the colon causes what? Liver takes up and excretes many other organic compounds: bilirubin is the classic and historic example Hepatic Bilirubin Transport SER RBC breakdown in RES UDP-glucuronide + Unconj BR Conj BR Unconj Bilirubin Unconj BR Bile Canaliculus Conj BR MRP-2: Multispecific organic anion transporter Conj BR AT P Blood Hepatocyte Conjugated bilirubin Glutathione S-conjugates other organic anions Newborn infants have poorly developed bilirubin conjugation enzymes and jaundice is common. Premature infants are even more affected Unconjugated bilirubin in the brain causes permanent damage (kernicterus) How to prevent brain damage in neonates? Regents of the University of Michigan Martybugs, Wikimedia Commons. Hepatic Bilirubin Transport and Mechanisms of Hyperbilirubinemia Gilbert's syndrome (mild) Crigler-Najjar syndrome (severe) SER Hemolysis Unconj Bilirubin Bile Canaliculus Unconj BR Conj BR Multispecific organic anion transporter Conj BR AT P Conjugated bilirubin Glutathione S-conjugates other organic anions Blood Hepatocyte Dubin-Johnson syndrome Rotor's syndrome ?estrogen/cyclosporin Bilirubin: Jaundice The first liver disease test CDC Bilirubin conjugation is an example Many other organic compounds undergo two-step biotransformation Example: cholesterol to bile acids After biotransformation, metabolites excreted Larger, lipophilic molecules excreted in bile Smaller (<400 Da) transported to blood and excreted by kidneys Step-wise Synthesis of Bile Acids from Cholesterol Steps are analogous to Phase I and Phase II steps of drug/xenobiotic metabolism Cholesterol P450- mediated hydroxylations OH group amino acid Conjugation of side chain to glycine or taurine Liver and Gut Barrier Functions Liver RES/filter Metabolism Biliary excretion Liver helps to remove/eliminate: Insoluble, nonabsorbable compounds Xenobiotics: metabolism, excretion Xenobiotics Drugs Drugs Bacteria (acid,:physical metabolism, excretion barrier, gut immune Bacteria : Kupfer cells system, liver RES) Intestine mucosal barrier Pancreas Liver’s Magic Trick: Regeneration Image of liver regeneration process removed Prometheus Bound P.P.Reubens An early case of of hepatic regeneration P. P. Rubens Hypoglycemia Poor blood clotting Cholestasis and jaundice Increased blood ammonia - affects cognitive function Decreased drug disposition Abnormal lipid metabolism Liver exhibits a wide range of functions Liver diseases may cause malfunction of one or more normal function Functions regulated separately so any one liver disease can affect each to a different extent Liver diseases cause: Altered liver functions Altered tests of liver injury Additional Source Information for more information see: http://open.umich.edu/wiki/AttributionPolicy Slide 73, Image 1 (top): Martybugs, "Jaundice phototherapy," Wikimedia Commons, http://commons.wikimedia.org/wiki/File:Jaundice_phototherapy.jpg, CC; BY-SA 3.0, http://creativecommons.org/licenses/by-sa/3.0/.