* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 19: The Heart
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Rheumatic fever wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Myocardial infarction wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Artificial heart valve wikipedia , lookup
Jatene procedure wikipedia , lookup
Atrial septal defect wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
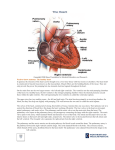
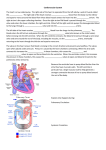
Chapter 18: The Heart Size, location, & orientation • Heart is about 250-350 grams (less than 1 lb) • About the size of a persons fist • Location – – – – – – – found in the mediastinum – medial cavity of thorax 2/3 of mass is left of midsternal Rests on superior surface of the diaphragm Anterior to the vertebral column Posterior to the sternum Flanked by the lungs – – – – Posterior surface (top) Broad & flat 9 cm wide Directed towards right shoulder • Base – • Apex – – Pointed end – Base of both ventricles – Point towards the left hip Coverings • Heart is enclosed in the pericardium: – Protects the heart – Anchors it to surrounding structures (diaphragm) – Prevents over filling • Serous pericardium: – Thin serous membrane – Two layers: • Parietal – – Lines the inside of the pericardium – internal surface – Tough fibrous connective tissue layer – Anchors to diaphragm & sternum • Visceral – – Covers the external surface of the heart – Serous layer turns downward to cover the heart – Part of heart wall – laced with fat • Pericardial cavity – – Potential space – space between visceral & serous layer of parietal pericardium – Contains pericardial fluid – allows serous membranes to glide past one another Layers of the heart wall • 3 layers: – Superficial epicardium (viseral pericardium): • Visceral layer of the serious pericardium • Infiltrated with fat – Middle myocardium: • Mostly cardiac muscle – bulk of the heart • Layer that actually contracts • Branching cardiac cells held together by crisscrossing connective tissue fibers & arranged in bundles – Connective tissue fibers form network – fibrous skeleton – reinforcement of heart muscle especially around valve areas & where vessels attach to the heart – Deep endocardium: • White sheet of endothelium resting on connective tissue layer • Located – inner myocardial surface, lining of chambers, & covers connective tissue skeleton of valves • Continuous w/ the endothelial linings of blood vessels leaving & entering the heart Chambers • 4 chambers – 2 atria & 2 ventricles • Internal septum – – divides the atria internally longitudinally • Interventricular septum – – divides the ventricle internally longitudinally • Right ventricle = – most of the anterior surface • Left ventricle = – inferoposterior aspect & forms most of the apex Chambers • Atria – – Superior – Receiving chambers for blood returning to the heart from circulation – Small chambers – Push blood to ventricles – Auricles – ear-like flap – from outside of each atria – increase atrial volume – Internal walls have ridges of muscles – pectinate – Fossa ovalis – shallow depression in interatrial septum – residual from fetal heart – Blood enters the right atrium from – • Superior vena cava – returns blood from above the diaphragm (upper body) • Inferior vena cava – blood returning from below the diaphragm (below the heart) • Coronary sinus – collects blood draining from myocardium – Blood enters the left atrium from – • 4 pulmonary veins • Seen from posterior view of the heart • Transport blood from the lungs Chambers • Ventricles – – – – – – Inferior Most of the mass of the heart Right ventricle = anterior surface Left ventricle = apex Trabecuae carneae – • irregular ridges of muscles – Papillary muscles – • project into the ventricular cavity – play a role in valve function • (muscle folds = trabeculae carnae – some are stalklike and attach to valves = papillary muscles) – – – – Discharging chambers – pumps of the heart Blood propels out of the heart into circulation Walls much thicker than atrial walls Right ventricle – pulmonary trunk – routs blood to lungs (gass exchange occurs) – Left ventricle - aorta – body Blood pathway through heart • Pulmonary circuit – – Right side of the heart – Low pressure – Blood to and from the lungs – Blood flow path• Blood in right atrium from body (oxygen poor, CO2 rich) via superior and inferior venae cavae • right ventricle • pumps into lungs (for oxygen pickup) via pulmonary trunk • from lungs to heart through pulmonary veins • left atrium • left ventricle Blood pathway cont • Systemic circuit – – Left side of the heart – High pressure – Supplies body w/ oxygenated blood – Pathway – • From lungs • Pulmonary veins • Left atrium • Left ventricle – contracts • Aorta • Body Valves • Atrioventricular valves (AV) – – Atrial-ventricular junction – Prevent backflow into the atria when ventricles are contracting – Attached to AV valves – collagen cords – chordae tendineane – anchor papillary muscles protruding from ventricular walls – Right AV valve = tricuspid valve • 3 flaps (tri) – endocardium & connective tissue – Left AV valve = bicuspid valve • 2 flaps (bi) – How it works – • • • • When heart is relaxed – AV valves hang into ventricle Blood into atria & into ventricle (through open AV valve) Ventricle contracts Ventricular pressure rises – forces blood (superiorly) against AV valve • Valve edges meet – closing the valve • Chordae tendineae & papillary muscles – anchor valves while they are closed Valves • Semilunar (half moon) valves – – Major arteries leaving the heart – Prevent backflow into the ventricles – Aortic semilunar – • Valve at the base of the aorta – Pulmonary semilunar – • Valve at the base of the pulmonary trunk – No chordae tendinae – valve movement caused by force of blood • Heart is relaxed – valves are closed • Heart contracts – valves are forced open Microscopic anatomy • Cardiac muscle – – Striated, short fat, branched, & interconnected muscle – One or two nuclei – Intracellular space filled w/ loose connective tissue matrix & capillaries – connected to fibrous skeleton – allows cardiac cells to exert force • Contraction occurs via sliding filaments – Adjacent muscles interconnect @ intercalated discs • Disc contains desmosomes (hold cardiac cells together) & gap junctions (allow ions to pass from cell to cell) • Allow cardiac cells to electrically behave as a unit – High concentration of mitochondria • Metabolize fatty acids for ATP • Can switch nutrient pathways to use whatever nutrient supply that is available – Depends on a continual supply of oxygen • Aerobic respiration – can’t have oxygen deprivation & still operate Heart contraction • Sodium & calcium needs: – Sodium ions enter cardiac muscle cells from extracellular fluid (sodium ion channels) – Causes a depolarization that causes the sarcoplasmic reticulum (specialized ER) to release calcium – Calcium enters the sarcoplasm (cytoplasm of cardiac cells) – Calcium signals myofilaments (individual muscle fibers) to contract – Cardiac muscles contract as a unit or not at all Electrical events • Intrinsic cardiac conduction system – made up of specialized cardiac cells – nodal system • Initiate & distribute impulses • Ensures that the heart depolarizes in sequential order • Contracts because of gap junction (allows signals to pass between cells) Electrical events • Sequence of excitation – – 1. SA node – • • • • • • Sinoatrial Pacemaker - sets pace for the heart In right atrial wall Minute cell mass Depolarizes 70-80 times per min Called sinus rhythm – determines heart rate – 2. AV node – • • • • • Atrioventricular In interatrial septum – above the tricuspid valve Depolarization spreads via gap junctions From SA node to AV node Impulse delayed 1 sec to allow atria to completely contract – 3. AV bundle – • • • • Atrioventricular “Bundle of His” Superior part of interventricular septum Connects atria & ventricles electronically Sequence of excitation cont. – 4. right & left bundles – • Along interventricular septum toward apex of the heart • Conduct signal through ventricles – 5. ventricular walls – • • • • Penetrate the heart apex Turn superiorly into ventricular walls Bundle branches excite septal cells Contraction depends on cell-to-cell transmission via gap junctions • Total elapsed time from SA node to ventricular node = .22 sec • Ventricles contract w/ wringing motion beginning at apex, moving toward atria Nodes Excitation http://www.youtube.com/watch?v=MGxxR yJTmwU&feature=related Heart sounds & CO • Lub – – 1st heart sound – AV valves close – Beginning of systole (ventricular pressure rises above atrial pressure) • Dup – – 2nd heart sound – Closure of semilunar valves – During ventricular diastole • Cardiac output (CO) – – Amount of blood pumped out each ventricle in one minute (one cycle) – CO = HR x SV • Stroke volume (SV) – – Volume of blood pumped by a ventricle with each beat (during one contraction) – Correlated w/ force of ventricular contraction Defects • Murmurs – – Abnormal heart sounds – Indicate valve problems • Tachycardia – – Abnormally fast heart rate – Over 100 beats per min • Arrhythmias – – Uncoordinated contractions – Irregular heart rhythms • Fibrillation – – Rapid, irregular, out of phase contractions – Heart is useless – Must be defibrillated immediately before brain death (electric shock) • Abnormal pacemaker – – Ectopic pacemaker – AV node may take over – but at a slower pace – Caffeine can cause irregular rhythms separate from the SA node Cardiac cycle • Ventricular filling – – Flows passively through atria into ventricles (70% of blood) – Atria contract propelling left over blood into ventricles • Ventricular systole – – – – – – Atria relax Ventricles contract Pressure rises closing the AV valves Semilunar valves forced open Blood passes into the aorta & pulmonary trunk • Isovolumetric relaxation – – Ventricular pressure drops – Closes the semilunar valves – Blood rebounds off the valves & continues its path