* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Hormone
Neuroendocrine tumor wikipedia , lookup
Hormone replacement therapy (menopause) wikipedia , lookup
Hypoglycemia wikipedia , lookup
Bioidentical hormone replacement therapy wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
Hypothyroidism wikipedia , lookup
Hyperandrogenism wikipedia , lookup
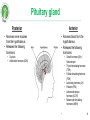
Hyperthyroidism wikipedia , lookup
Pituitary apoplexy wikipedia , lookup
Hypothalamus wikipedia , lookup
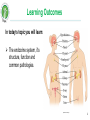
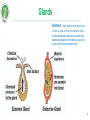
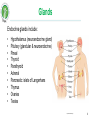
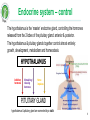
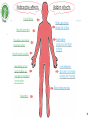
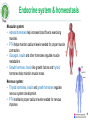
Biomedicine: Human Sciences Lecture 9: Endocrine System 1 Learning Outcomes In today’s topic you will learn: The endocrine system, it’s structure, function and common pathologies. http://www.hormone.org/ 2 Endocrine system & hormones The endocrine system coordinates the activity of organs through hormones – chemical messengers released into the blood from glands which produce them. Hormones have specific target cells / tissues, some far from where the hormone is produced, others effect cells of the organ where they were released (paracrine effect), or the same cell type (autocrine effect). Hormones can be peptides, steroids, or amino acid derivatives. Hormones play an essential role in the bodies homeostasis, including rate of metabolism, blood pressure, blood glucose levels, body acidity etc. AUTONOMIC NERVOUS SYSTEM ENDOCRINE SYSTEM Rapid Change Slower Change Less Precise More Precise Shorter Duration Longer Duration Neurotransmitters Hormones 3 Glands There are 2 types of glands: 1. EXOCRINE - excrete their products into ducts leading to the external environment. Examples include salivary glands (saliva), gastric glands (digestive enzymes), sebaceous glands (sebum), mammary glands (breast milk). 2. ENDOCRINE – are ductless, they secrete their products (hormones) into the blood or nearby target cells / tissues. . 4 Glands Hormone: . from Greek hormōn, from horma n to stir up, urge on, from hormē impulse, move. A chemical substance produced in an endocrine gland and transported in the blood to a certain tis sue on which it exerts a specific effect. 5 Glands Endocrine glands include: • • • • • • • • • • Hypothalamus (neuroendocrine gland) Pituitary (glandular & neuroendocrine) Pineal Thyroid Parathyroid Adrenal Pancreatic: islets of Langerhans Thymus Ovaries Testes http://www.hormone.org/ 6 Endocrine Tissues Some tissues of the body are not considered glands but have endocrine functionality: produce hormones: • • • • • • • Adipose tissue - leptin (suppresses food intake) & resistin (blood glucose, inflammation). Heart - atrial natriuretic peptide (blood pressure). GIT: stomach - ghrelin & gastrin (satiety & gastric emptying). Liver – angiotensinogen, Insulin-like growth factor (IGF), thrombopoietin. Placenta - human chorionic gonadotropin (hCG) & progesterone. Kidneys - erythropoietin (RBC production) & calcitriol (vit. D). Skin – cholecalciferol (vit. D). 7 Hormone activity Hormones have specific target cells – they influence the activity of the target cells by identifying & binding to specific receptors (proteins) within or on the surface of the target cells. The target cells can alter their sensitivity to the hormone: Down-regulation: with an excess quantity of hormone target cells reduce the number of protein receptors to reduce hormone activity on the cell. Up-regulation: a deficiency in hormone causing an increase in the number of receptors on target cells. Hormone secretion regulation: 1. Nervous system signals 2. Chemical changes in the blood 3. Other hormones. They are controlled through feedback loops – positive and negative. 8 Endocrine system – control The hypothalamus is the ‘master’ endocrine gland, controlling the hormones released from the 2 lobes of the pituitary gland: anterior & posterior. The hypothalamus & pituitary glands together control almost entirely: growth, development, metabolism and homeostasis. HYPOTHALAMUS Inhibitory hormones Stimulating/ releasing hormones Nerve impulses PITUITARY GLAND hypothalamus & pituitary gland are connected by a stalk 9 Pituitary gland Posterior • Receives nerve impulses from the hypothalamus. • Releases the following hormones: • • Anterior • Receives blood from the hypothalamus. • Releases the following hormones: • Oxytocin Antidiuretic hormone (ADH) • • • • • • • Growth hormone (GH) / Somatotropin Thyroid stimulating hormone (TSH) Follicle stimulating hormone (FSH) Luteinizing hormone (LH) Prolactin (PRL) Adrenocorticotropic hormone (ACTH) Melanocyte stimulating hormones (MSH) 10 HORMONES of the HYPOTHALAMUS, ANTERIOR PITUITARY & THEIR TARGET ORGANS / TISSUES Growth Hormone Releasing Hormone Growth Hormone Growth Hormone Releasing Inhibiting Hormone Thyroid Releasing Hormone Corticotropin Releasing Hormone Prolactin Releasing Hormone Thyroid Stimulating Hormone Adrenocorticotropic Hormone Prolactin Prolactin Inhibiting Hormone Follicle Stimulating Hormone Gonadotropin Releasing Hormone Luteinizing Hormone 11 Growth hormone (GH) Also known as somatotropin. Growth hormone releasing inhibiting hormone (GHRIH) / somatostatin. ACTIVITY: 1. Regulates metabolism in many organs. 2. Promotes growth & division of (most) body cells (especially bone & muscle). 3. Stimulates release of insulin-like growth factors (IGF’s) in cells. INCREASED PRODUCTION: • Night (sleep) • Hypoglycaemia • Exercise • Anxiety • Childhood & adolescence Growth hormone releasing hormone (GHRH). Growth hormone / somatotropin ALL TISSUES 12 Thyroid Stimulating Hormone (TSH) ACTIVITY: 1. Growth & activity of the thyroid gland: increasing thyroid hormone production thyroxine (T4) & tri-iodothyronine (T3). PRODUCTION: • Lowest levels in the early evening & highest during the night. Thyroid releasing hormone (TRH) TSH 13 Adrenocorticotropic hormone (ACTH) High ACTH levels ACTIVITY: 1. Circadian rhythm (sleep / wake cycle) 2. Output of steroid hormones: glucocorticoids, especially cortisol. INCREASED PRODUCTION: • Hypoglycaemia • Exercise • Stressors such as emotions, fever • Interleukin-1 Corticotropin releasing hormone (CRH) Adrenocorticotropic hormone (ACTH) / corticotrophin ADRENAL COTREX PRODUCTION: • Highest in the morning and lowest at midnight. 14 Prolactin (PRL) ACTIVITY: 1. Stimulates lactation (together with other hormones) 2. Prevents pregnancy during lactation. 3. Breast maturation after childbirth. PRODUCTION: • After birth • Suckling • Emotional stress • Sleep (at any time of day) Prolactin releasing hormone (PRH) Prolactin MAMMARY GLANDS 15 Follicle stimulating hormone (FSH) & luteinizing hormone (LH) ACTIVITY: • FSH: • • • • • High levels of: • Oestrogen, • Progesterone • Testosterone Production of gametes (male & female) Increase oestrogen production (F) Maturation of ovarian follicles (F) Stimulate testosterone production (M) Sperm production (M) • LH • • • Triggers ovulation & formation of corpus luteum Increase secretion of progesterone (F) Stimulates secretion of testosterone (M) Gonadotropin releasing hormone (GnRH) Follicle stimulating hormone (FSH) Luteinizing hormone (LH) OVARIES & TESTES 16 Melanocyte Stimulating Hormone (MSH) • Produced by the anterior pituitary • Fx • Increases skin pigmentation in amphibians. Exact role in humans is unknown but MSH can be erroneous produced as part of some pathologies • Stimulated by: Corticotrophin releasing hormone • Inhibited by: Prolaction inhibiting hormone (dopamine) 17 Oxytocin ACTIVITY: 1. Contracts uterus in childbirth (parturition) 2. Contracts lactating breast 3. Bonding hormone (mother with baby) Nerve Impulses (no stimulation) PRODUCTION: • Suckling • Childbirth • POSITIVE FEEDBACK Posterior pituitary OXYTOCIN Mammary glands & muscles Uterine Muscles 18 Antidiuretic hormone (ADH) Also known as vasopressin. ACTIVITY: 1. Reduces urine output by stimulating reabsorption sodium & water in the kidneys. 2. Vasoconstriction in skin & abdominal organs to increase blood pressure, preventing hypovolaemic shock. PRODUCTION: • ADH production: increased osmotic pressure, reduced fluid intake. • ADH production inhibited by: reduced osmotic pressure, increased fluid intake, alcohol. Hypothalamic Osmoreceptors Nerve Impulses Posterior lobe of pituitary gland ADH Kidneys 19 Antidiuretic hormone (ADH) Decreased reabsorption of urine (increased elimination) Osmoreceptors In Hypothalamus Indicate High Osmotic Pressure (Not enough fluid) ADH Secretion Suppressed/ Inhibited ADH Secretion Stimulated Osmoreceptors In Hypothalamus Indicate Low Osmotic Pressure (Too much fluid) Increased reabsorption of urine & Vasoconstriction (decreased urination) 20 Pituitary gland pathologies Usually caused by autoimmune disease or tumours causing either: • Hyper-secretion • Hypo-secretion Signs & symptoms depend on the hormones affected. 21 Acromegaly & gigantism Acromegaly: excess growth hormone (GH) after ossification (bone formation) leading to the excess growth of body tissues over time. Gigantism: excess growth hormone (GH) while the bones are still growing. CAUSES: Usually a pituitary tumour causing hyper-secretion & damage to the optic nerve. SIGNS & SYMPTOMS (Sx): Large, prominent facial features, increased size of hands & feet - spade like hands & feet, headaches, excessive sweating, large tongue, oedema, tiredness, deep voice, impotence, joint pain, little bony deformities, soft-tissue swellings. Gigantism: giant-like features because the WHOLE body is able to grow. TREATMENT (Rx): Surgery to remove cancer, reduce GH levels to normal. ALTERNATIVE SUPPORT (Rx): Treat / support cause. Herbs & nutritional supplements – antioxidants, diet is essential for all forms of cancer (primarily plant based diet rich in nutrients & antioxidants), alkalising the body. 22 Acromegaly & gigantism COMPLICATIONS: If left untreated can be serious, even fatal: type 2 diabetes, hypertension, cardiovascular disease, arthritis, bowel polyps (may become cancerous). 23 Hyperprolactinaemia Excess prolactin production. CAUSES: Tumour on the pituitary, acromegaly, PCOS, hypothyroidism. SIGNS & SYMPTOMS (Sx): Galactorrhoea, amenorrhoea / oligomenorrhoea, decreased libido (both male & female), subfertility. ALTERNATIVE SUPPORT (Rx): Treat / support the cause. Herbs can help balance hormone levels in cases of hypothyroid & PCOS. Nutrition to support thyroid function. In cases of cancer – antioxidants, diet (primarily plant based diet rich in nutrients & antioxidants), alkalising, acupuncture, homeopathy. http://www.rayur.com 24 Diabetes insipidus ADH deficiency causing the kidneys to allow over excretion of water from the body. CAUSES: Usually brain trauma, tumour, encephalitis (inflammation of the brain). SIGNS & SYMPTOMS (Sx): Extreme thirst & urination - large quantities often, 4-5 L of liquid may be consumed daily. TREATMENT (Rx): Treat cause. Rehydration: water & electrolytes, homeopathy, acupuncture. . 25 Pineal gland - Melatonin A small pine-cone shaped gland in the midline of the brain under control by the hypothalamus. It produces the hormone melatonin. ACTIVITY: Contribute to the setting of the circadian rhythm. A potent antioxidant. Atrophy of gonads & may play a role in the onset of puberty & inhibiting reproduction with increasing age. PRODUCTION: Made from serotonin. Levels are highest in children & decline with age. Stimulated by: night, darkness. Reduced by: daylight, irregular sleep patterns (jetlag, night-work), some medications. 26 Thymus gland - Thymosin A bi-lobed gland behind the sternum which plays an important role with immune cells. It atrophies with age. ACTIVITY: Site of maturation of T-cells of the immune system. 27 Thyroid gland A butterfly shaped gland inferior to the larynx. It has 2 lobes located on either side of the trachea. Follicular cells produce thyroid hormones: thyroxine (T4) & triiodothyronine (T3) Parafollicular cells produce calcitonin (CT). Production begins in the 3rd month of development in the foetus. T4 & T3 are synthesized from tyrosine & iodine within a specialized thyroid protein called thyroglobulin (Tg). T4 has 4 iodine atoms, T3 contains 3 iodine atoms. Follicular cells trap & store most of the bodies iodide (approx. 100 day supply). 28 Thyroid gland - Thyroxine The major form of thyroid hormone in the blood is thyroxine (ratio of T4 to T3 is approx. 20:1). Selenium-containing enzymes are used in the conversion of T 4 to T3. T3 is a more biologically active form, being 3 to 4 times more potent than T4. T4 & T3 are hydrophobic and require carrier proteins in the blood: thyroxinebinding globulin (TBG). This prevents these hormones from entering parts of the body that don't require thyroid hormones & allows the body to maintain a stable pool of thyroid hormones from which the active, free hormones can be released when & where required. Thyroid hormone levels must therefore be measured in terms of free T4 & T3. 29 Thyroid gland - Thyroxine ACTIVITY: Increase metabolic rate & heat production. Essential for normal growth / development. Central nervous system (CNS) function. Work in conjunction, & enhance, the activities of adrenalin (epinephrine) & noradrenaline (norepinephrine), insulin & hGH. PRODUCTION: Stimulated by: TSH, exercise, stress, malnutrition, low blood glucose, low T3 to T4. Reduced by: low TSH, high T3 to T4. Highest levels at night. Higher levels during adolescence, pregnancy & female reproductive years. 30 T3, T4 & TSH Levels Low Plasma Glucose, Stress, Exercise, Sleep, Malnutrition Stimulates Hypothalamus • If TSH levels are RAISED this indicates that the Thyroid is FAILING • TSH is usually LOW in a Thyroid Releasing Hormone (TRH) Decreases TRH secretion Stimulates Anterior Pituitary Thyroid Stimulating Hormone (TSH) Decreases Pituitary sensitivity to TRH Stimulates Thyroid ↑ Thyroxine (T4) ↑ Tri-iodothyronine (T3) REGULARLY functioning Thyroid 31 Thyroid gland - Thyroxine LAB TESTS: 1. TSH Levels. 2. Free T3 & T4 - unbound form of thyroid hormones are the more bioavailable by the target cells & tissues. 3. Thyroglobulin (Tg) - levels in the blood can be used as a tumour marker for certain kinds of thyroid cancer. 4. Anti-thyroglobulin antibodies (ATA), frequently referred to as TgAb, are often found in patients with Hashimoto's thyroiditis or Graves' disease, although may be present in healthy individuals (can be destructive or stimulating & may co-exist). 32 Hypothyroidism Is a condition of thyroid hormone deficiency, common in the elderly. CAUSES: Autoimmune - hashimoto’s thyroiditis, iodine deficiency, thyroid destruction (radioactive iodine, surgery, side-effects of medication e.g. lithium, congenital, tumour (thyroid / hypothalamic, pituitary). SIGNS & SYMPTOMS (Sx): Tiredness, malaise, weight gain, goitre, anorexia, cold intolerance, poor memory, mental slowness, goitre, puffy around the eyes (myxoedema), depression, mood swings, low libido, dry brittle hair / skin, muscle cramps, arthralgia, constipation, psychosis, menorrhagia or oligomenorrhoea, loss of eyebrows, slow reflexes, deep voice, bradycardia and hypertension. 33 Hypothyroidism ALLOPATHIC TREATMENT: Levothyroxine – thyroid hormone replacement ALTERNATIVE SUPPORT (Rx): Cause. Thyroid support: iodine, selenium, tyrosine, thyroid replacement therapy. Herbs to support thyroid. Herbs to support tumour or autoimmune condition. 34 Hyperthyroidism (Grave's disease) Hyperthyroidism (also known as thyrotoxicosis) is characterised by hypermetabolism and elevated serum levels of free thyroid hormones. CAUSES: Graves disease (most common cause): autoimmune condition - IgG antibodies bind to TSH receptor and stimulate production of thyroid hormones, excessive intake of iodine or thyroid hormone, tumour (hypothalamic, pituitary), thyroiditis, nodule. SIGNS & SYMPTOMS (Sx): Nervousness, palpitations, hyperactivity, increased sweating, heat hypersensitivity, fatigue, increased appetite, weight loss, insomnia, weakness, frequent bowel movements, warm, moist skin, tremor, tachycardia, atrial fibrillation, and palpitations. ALLOPATHIC TREATMENT (Rx): Drugs: antithyroid, radioactive iodine, β-Blockers, surgery. 35 Hyperthyroidism (Grave's disease) ALTERNATIVE SUPPORT (Rx): Treat cause. In the case of Grave’s disease herbs & nutritional supplements to restore immune system balance, homeopathy. COMPLICATIONS: Thyrotoxic crisis: hyperthermia (> 40°C / 104°Fahrenheit), tachycardia, heart failure. 36 Barnes Temperature Test 1. Prepare the thermometer before going to bed. 2. On waking, before getting out of bed, with as little movement as possible, place the thermometer under your arm. 3. Leave it in position for 10 minutes. 4. Test for 5 consecutive days and make a note of the 3 lowest readings. If menstruating do the test starting the second day of menses. 5. 36.6 - 36.8OC (97.8 - 98.2OF) is normal. Below 36.6OC (97.8OF) is below normal, and may indicate hypothyroid. Seeing a GP is recommended. 37 Thyroid gland – Calcitonin Produced by the parafollicular cells of the thyroid gland. ACTIVITY: Reduces blood calcium (Ca) by: inhibiting Ca reabsorption from the bone & kidneys, inhibiting osteoclast activity, opposing parathyroid activity. Important during childhood for bone growth. PRODUCTION: Stimulated by: increased blood Ca levels. Inhibited by: reduced blood Ca levels. 38 Parathyroid Glands Four small glands located posteriorly to the thyroid. Produces parathyroid hormone. http://www.parathyroidglands.com 39 Parathyroid hormone (PTH) ACTIVITY: Increase blood Ca when low by: Increase Ca absorption from intestines. Increase Ca reabsorption in bone & kidney. Increase osteoclast activity. Increase production of active vit. D, which increases Ca & P absorption of the GIT. Regulates magnesium & phosphate blood levels. PRODUCTION: Stimulated by: reduced blood Ca levels. Inhibited by: increased blood Ca levels. Blood calcium allows is essential for muscle contraction, nerve transmission, blood clotting. 40 Hyperparathyroidism Hyperparathyroidism is characterised by hyper-metabolism and elevated serum levels of parathyroid hormone (PTH). CAUSES: Usually tumours. SIGNS & SYMPTOMS (Sx): Often no / few symptoms, hypercalcaemia, increased risk of kidney stone formation, osteoporosis / osteopenia, low energy, depression, in some cases: nausea, vomiting, constipation, anorexia, muscle paralysis. TREATMENT (Rx): Surgery to remove some or all of the parathyroid glands. Surgery may include implanting parathyroid tissue into the forearm muscle to provide residual parathyroid function. ALTERNATIVE SUPPORT (Rx): Herbs & nutritional supplements – antioxidants, primarily plant based diet rich in nutrients & antioxidants), alkalising the body. http://www.aafp.org/ 41 Hypoparathyroidism Hypoparathyroidism is characterised by hypo-metabolism and reduced serum levels of parathyroid hormone (PTH). CAUSES: Usually surgery or radiation (while treating thyroid). SIGNS & SYMPTOMS (Sx): Hypocalcaemia, muscle cramps & spasms (called tetany), tingling lips, fingers, and toes, pain in the face, legs, and feet, abdominal pain, dry hair, brittle nails, dry scaly skin, cataracts, weakened tooth enamel (in children). TREATMENT (Rx): Calcium and vitamin D. Hormone replacement is being developed. 42 Adrenal Glands Pair of glands superior to the kidneys. Two parts: • Inner medulla: part of the autonomic NS, producing: • • Adrenaline (epinephrine) Noradrenaline (norepinephrine) • Outer cortex – produces 3 groups of steroid hormones: • • • Glucocorticoids (primarily cortisol) Mineral corticoids (primarily aldosterone) Sex hormones (primarily androgens) 43 Glucocorticoids Steroid hormones produced in the adrenal cortex which regulate metabolism & resistance to stress. They include: 1. Cortisol / hydrocortisone (most abundant: about 95%). 2. Cortisone 3. Corticosterone ACTIVITY: 1. Stimulating gluconeogenesis 2. Proteolysis (amino acids from protein) 3. Lipolysis 4. Production of glucose by the liver 5. Reduce immune response 6. Weak reabsorption of sodium & water from kidney tubules. 7. Anti-inflammatory – hence therapeutic use of steroids 44 Mineral corticoids Primarily aldosterone. ACTIVITY: maintenance of water / electrolyte balance:1. Reabsorption of Na in renal tubules 2. Excretion of K in urine 3. All cause retention of water to regulate blood volume and blood pressure 4. Removal of acid from the body. PRODUCTION: Stimulated by: angiotensin, high blood K. Inhibited by: low blood K. 45 Sex hormones Primarily androgens in the form of DHEA. ACTIVITY: 1. Production of pubic & axillary hair 2. Growth (pre-pubertal) 3. Production / converted to oestrogen (in females) PRODUCTION: Not fully understood. Cortical androgens are insignificant compared to amount produced in the ovaries & testes during puberty and adulthood. Important only at pre-pubescent and post-menopausal stages of life. 46 Adrenaline & Noradrenaline Adrenaline (80%) & noradrenaline (20%) are produced in uneven quantities by the adrenal medulla. ACTIVITY: The function of these hormones is to intensify the sympathetic response: 1. Increase heart rate & contraction causing an increase in blood pressure. 2. Increase blood flow to the heart, brain, skeletal muscles & adipose tissue. 3. Increase metabolism. 4. Increase blood glucose & triglycerides (for metabolism) 5. Decrease blood to digestion & skin. 6. Dilate pupils & airways. Adrenaline has greater influence on the heart. Noradrenaline effects blood vessel PRODUCTION: Stimulated by: exercise, fasting, shock, elevated temperature, infection, disease, emotional stress. Inhibited by: eating, sleeping, calmness. 47 Adrenal glands – medulla: adrenaline & noradrenaline . 48 Cushing syndrome / disease Chronic high blood levels of cortisol or related corticosteroids. Cushing syndrome is a cortisol excess from any cause, Cushing disease is hyperfunction of the adrenal cortex from pituitary ACTH excess. CAUSES: Hyperfunction of the adrenal cortex can be ACTH dependent or ACTH independent: hypersecretion of ACTH by the pituitary gland, carcinoma of pituitary or adrenals, administration of exogenous ACTH. SIGNS & SYMPTOMS (Sx): Central weight gain, depression, insomnia, psychosis, amenorrhoea, poor libido, thin skin, easy bruising, reduced immunity, muscular weakness, growth arrest in children, back pain, moon face, buffalo hump, bone fractures, osteoporosis, insulin resistance, hirsutism, hypertension. 49 Cushing syndrome / disease TREATMENT (Rx): Drugs inhibiting cortisol production, surgery (for cancer). ALTERNATIVE SUPPORT (Rx): Treat cause with herbs, homeopathy & nutritional supplements if indicated (cancer support). COMPLICATIONS: Lowered immunity, paper skin, bone fractures. 50 Addison’s disease An insidious, usually progressive hypo-functioning of the adrenal cortex causing mineralocorticoids (Na reabsorption and K excretion) and glucocorticoids (blood glucose & metabolism) to be deficient. CAUSES: Atrophy of the adrenal gland often due to auto-immune destruction but may be from other causes such as disease, abrupt cessation of steroid medications. SIGNS & SYMPTOMS (Sx): Weakness, fatigue, and hypotension are early signs. Hyperpigmentation, black freckles, weight loss, anorexia, malaise, weakness, fever, depression, impotence / amenorrhoea, muscle fatigue, low blood pressure, syncope, nausea / vomiting, confusion, diarrhoea, cravings for salty foods, abdominal pain, myalgia, joint pain, loss of body hair, dehydration. TREATMENT (Rx): Hormone replacement. 51 Addison’s Disease Adrenal failure leads to lack of adrenal hormone production and a failure of the normal negative feedback mechanism. This leads to the hypothalamus production an excess of corticotrophin releasing hormone which causes the pituitary to erroneously produce melanocyte stimulating hormone. This causes the skin colour to darken, hence hyperpigmentation Hypothalamus CRH Pituitary MSH Skin Pigmentation ACTH Adrenals 52 Adrenal glands – pathologies: Addison’s disease ALTERNATIVE SUPPORT (Rx): Treat the cause. Herbs to support autoimmunity, homeopathy. COMPLICATIONS: May experience adrenal crisis when under stress (e.g. surgery, infection, illness): asthenia; severe pain, peripheral vascular collapse, renal shutdown, severe fever. 53 http://www.medicalassessment.com/ Pancreas The pancreas has both endocrine & exocrine function: endocrine function is via the cells called the islets of Langerhans. Three types of endocrine cells: 1. Alpha cells: produce glucagon. 2. Beta cells: produce insulin. 3. Delta cells: produce somatostatin / GHRIH. Main endocrine function of the pancreas is to regulate blood glucose levels & maintain within normal range (4-7mmol/L). 54 Pancreas - Insulin The first protein to have it’s amino acid sequence identified. ACTIVITY: Lowers blood glucose levels, amino acids & fatty acids. Stimulates cells to up-take glucose from the blood. Promotes synthesis of proteins, glycogen (glycogenesis) & fats (lipogenesis). PRODUCTION: Stimulated by: high blood glucose, elevated blood amino acids, eating, sweet taste (artificial sweeteners). Reduced by: low blood glucose, starvation, glucagon. 55 Pancreas - Glucagon ACTIVITY: Raises blood glucose levels. Converts glycogen to glucose in liver and skeletal muscle: glycogenolysis & gluconeogenesis. Lipolysis for use in metabolism. PRODUCTION: Stimulated by: low blood sugar, exercise. Reduced by: insulin, high blood sugar. 56 Pancreas - Somatostatin (GHRIH) Growth hormone releasing inhibiting hormone Also produced by the hypothalamus & digestive system e.g. stomach & intestines. ACTIVITY: Inhibits insulin & glucagon. PRODUCTION: Stimulated by: low blood sugar, exercise. Reduced by: insulin, high blood sugar. 57 Diabetes A metabolic disorder characterized by a deficiency / absence of insulin due to impaired production or resistance causing a disruption of carbohydrate & fat metabolism & elevated blood glucose levels: HYPERGLYCAEMIA. TYPES: • Type I: autoimmune • Type II: insulin resistance • Secondary: due to certain medications (cortisone, some diuretics), pancreatitis, hormone disorders (high GH, thyroid hormone, cortisol, adrenaline. • Gestational: during pregnancy as a result of placental hormones blocking Insulin action in the mother. Usually disappears after delivery, and returns as Type 2 years later. 58 Type I diabetes Previously called juvenile-onset or insulin-dependent (IDDM). CAUSES: An auto-immune condition causing destruction of pancreatic ß-cells possibly due to an environmental exposure in genetically susceptible people: viruses (coxsackie, rubella, cytomegalovirus, Epstein-Barr, and retroviruses) have been linked, diet exposure of infants to dairy products (especially cow's milk and the milk protein β casein), nitrates, low vit. D consumption, early exposure to gluten and cereals increases islet cell autoantibody production. SIGNS & SYMPTOMS (Sx): Glycosuria, polyuria, polydipsia, dehydration causing weakness, fatigue, and mental status changes, weight loss, nausea and vomiting, blurred vision, predisposition to infections, ketoacidosis: lethargy, hypotensive, tachycardia, breathe rapidly and deeply, fruity breath due to exhaled acetone, coma. 59 Type I diabetes TREATMENT (Rx): Insulin. ALTERNATIVE SUPPORT (Rx): Herbs (support pancreas, insulin sensitivity), nutrition (low GI & GL, antioxidants, fibre, chromium, vit. D, magnesium rich foods, zinc), alkalising the body, homeopathy and acupuncture. COMPLICATIONS: Increased risk of heart disease, vascular disease, neuropathy, retinopathy, high cholesterol, hypertension. 60 Type II diabetes A milder form of diabetes, previously called adult-onset or non–insulin-dependent, whereby insulin secretion is inadequate because patients have developed resistance to insulin. hyperglycaemia develops when insulin secretion can no longer compensate for insulin resistance. Up to one third of adults over 65 have impaired glucose tolerance. It is becoming increasingly common among children. CAUSES: Clear genetic link: strong hereditary link and a high prevalence in American Indians, Hispanics, and Asians, β-cell dysfunction and impaired insulin secretion, obesity & weight gain, diet, exercise, and lifestyle, low birth weight, pregnancy causes some insulin resistance. SIGNS & SYMPTOMS (Sx): Often asymptomatic because of mild hyperglycaemia (unlike in type I diabetes), initial symptoms are often complications, indicating the disease has been present for some time, ketoacidosis in severe cases. 61 Type II diabetes CONVENTIONAL TREATMENT (Rx): Diet (low GI & GL), exercise, oral antihyperglycaemics, insulin, or both. To prevent complications: ACE inhibitors, statins, and aspirin. ALTERNATIVE SUPPORT: Diet, exercise, weight loss, chromium, Herb - Gymnema, Cinnamon, vit. D COMPLICATIONS: Increased risk of heart disease, vascular disease, neuropathy, retinopathy, high cholesterol, hypertension. DIAGNOSIS: Fasting / random blood glucose test Oral glucose tolerance test Urine test . 62 Ketoacidosis Ketones are acidic, toxic, by-products of metabolising fats & proteins for energy when carbohydrates (glucose & glycogen) levels are depleted OR when cells are unable to utilise available glucose, as in diabetes. Tests: Ketones in urine (urine stick test) Increased thirst (kidneys flush out ketones) Breath smells fruity (acetone) Ketoacidosis may cause coma and death. 63 Diabetics Symptoms HYPERGLYCAEMIA HYPOGLYCAEMIA Need for frequent urination Shaking & sweating Extreme hunger and / or thirst Extreme hunger & irritability Blurred vision Tachycardia Drowsiness Dizziness, headache Nausea Anxiety / confusion, weak & tired Ketoacidosis, coma Ketoacidosis, seizures, coma, death 64 Diabetic Coma Aetiology/ pathophysiology Differential diagnosis Rx / First Aid: HYPERGLYCAEMIC HYPOGLYCAEMIC COMA COMA • Lack of insulin • Dehydration • Acidosis due to build up of ketones • Elevated blood glucose If coma, smell breath. Hyperglycaemic coma will often smell like nail varnish remover • If conscious- water • If in coma - 999 • Too much Insulin • Too much exercise • Delayed meal May or may not have ketone smell • Sugar • If in coma - 999 65 Local hormones Hormone Secreted by Action Histamine Basophils, mast cells Part of inflammation – vasodilatation and increased blood vessel permeability Prostaglandins, leukotrienes & thromboxane's Most tissues Chemical messengers involved in many different body processes Serotonin Platelets, brain, intestinal wall Blood clotting, temperature regulation, appetite, sleep Dopamine Primarily brain Muscle tone and some movements Erythropoietin Kidneys Red blood cell production Gastrin GI tract Promotes gastric juice secretion and stomach motility Secretin GI tract Stimulates bile and pancreatic juice secretion CCK GI tract Stimulates bile & pancreatic juice secretion. Promotes a sense of fullness after meals 66 Endocrine system & homeostasis Whole body: The endocrine system regulates growth and activities of cells throughout the body e.g. glucose uptake and metabolism. Integumentary system: • Androgens stimulate pubic hair growth and sebaceous gland activation. • Melanocyte-stimulating hormone (MSH) causes skin darkening. Skeletal system: • Growth hormone and insulin like growth factors stimulate bone growth. • Oestrogen helps maintain bone mass. • Parathyroid hormone (PTH) and calcitonin regulate calcium levels in the bone and blood. • Thyroid hormones are needed for development and growth of the skeleton. 67 Endocrine system & homeostasis Muscular system: • Adrenal hormones help increase blood flow to exercising muscles. • PTH helps maintain calcium levels needed for proper muscle contraction. • Glucagon, insulin and other hormones regulate muscle metabolism. • Growth hormone, Insulin like growth factors and thyroid hormones help maintain muscle mass. Nervous system: • Thyroid hormones, insulin and growth hormones regulate nervous system development. • PTH maintains proper calcium levels needed for nervous impulses. 68 Endocrine system & homeostasis Lymphatic system: • Glucocorticoids depress immune response and inflammation. • Thymus hormones promote T-cell maturation. Cardiovascular system: • Erythropoietin promotes formation of RBCs. • Aldosterone and antidiuretic hormone (ADH) increase blood volume. • Adrenaline and noradrenalin increase heart rate and contraction force. Respiratory system: • Adrenaline and noradrenalin dilate airways during exercise and stress. • Erythropoietin regulates amount of oxygen carried in the blood by adjusting the number of RBCs. 69 Endocrine system & homeostasis Digestive system: • Adrenaline and noradrenalin depress digestion. • Gastrin, CCK and secretin help regulate digestion. Urinary system: • ADH and aldosterone adjust rate of water and electrolyte loss to regulate blood volume. Reproductive system: • FSH and LH regulate development growth and secretions of the ovaries and testes. • Oestrogen and testosterone stimulate sex cell development and changes during puberty. • Prolactin promotes milk secretion from the mammary glands. • Oxytocin causes contraction of the uterus and ejection of milk from the mammary glands. 70 Activity • Complete the Endocrine System Practice Quiz and Exercises. 71 ACTIVITY Have a look at the glossary for this topic (on the student website). Please also look at the prefixes & suffixes to help you understand the medical terminology used in this lecture. 72