* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download anesthesia for a patient of mitral stenosis
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Aortic stenosis wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Atrial septal defect wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
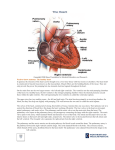
DR.SANDEEP SAINI LLRM COLLEGE MEERUT U.P. INDIA INDEX INTRODUCTION ETIOLOGY & PATHOLOGY PATHOPHYSIOLOGY SYMPTOMS AND SIGNS DIAGNOSIS ANESTHETIC MANAGEMENT INTRODUCTION- Mitral stenosis is the narrowing of mitral orifice as a result of diffuse thickening of valve leaflets by fibrous tissue and calcific deposits. ETIOLOGY AND PATHOLOGY-Most common cause of mitral stenosis is rheumatic heart disease. Females are affected more than males. Less common – carcinoid syndrome, left atrial myxoma, cor triatriatum, rheumatoid arthritis, systemic lupus erythematosus congenital. Thickening of valve leaflets and cusps become rigid. Fusion of mitral commissures. Shortening and fusion of chordae tendinae. All the changes leads to funnel shaped (fish mouth) valve. Calcification immobilize the leaflets and narrows the orifice further. PATHOPHYSIOLOGY Cardiac changes- Normal valve area: 4-6 cm2 Mild mitral stenosis: MVA 1.5-2.5 cm2 Minimal symptoms Mod mitral stenosis MVA 1.0-1.5 cm2 usually does not produce symptoms at rest Severe mitral stenosis MVA < 1.0 cm2 Symptoms at rest Mean gradient: >10 mmHg Severe 5-10 mmHg Moderate <5 mmHg Mild Pathophysiology Right Heart Failure: Hepatic Congestion ↑JVP Tricuspid Regurgitation RA Enlargement RV Pressure Overload RVH RV Failure Pulmonary HTN Pulmonary Congestion Atrial Fib LA Thrombi LA Enlargement LA Pressure Obstruction of diastolic inflow Prolonged early diastolic mitral inflow &delayed filling Pressure volume loops shifted to left so LVEDP and LVEDV are↓ Pulmonary changes Pulmonary arterial hypertension results as1)Increased left atrial pressure. 2)Pulmonary arterial constriction. 3)Interstitial edema in the wall of the small pulmonary vessels. 4)Organic obliterative changes in the pulmonary vascular bed. At last if there is severe pulmonary arterial hypertension→Tricuspid regurgitation Pulmonary in competence Rt sided heart failure HEMODYNAMIC CHANGES THAT OCCURS AT VARIOUS STAGES OF SEVERITY OF MITRAL STENOSIS SEVERITY→ AT R E S T MILD (1.5-2.5 cm2) MODERATE (1.1-1.5 cm2) SEVERE ( < 1cm2 ) Left atrial pressure N ↑ Pulmonary arterial pressure N ↑ ↑↑ or ↑↑↑↑ N N ↓ or ↓↓↓ Left atrial pressure ↑ ↑↑ Pulmonary arterial pressure ↑ ↑↑ ↑ ↑ ↑↑ Cardiac output E X E R C I S E Cardiac output Symptoms Breathlessness Fatigue Oedema, ascites Palpitation Haemoptysis Cough Chest pain Hoarseness Mitral facies or malar flush Symptoms of thromboembolic complications (e.g. stroke, ischaemic limb) o Are worsened by conditions that demand increase in cardiac output. ◦ Exertion,fever, anemia, pregnancy, thyrotoxicosis NYHA FUNCTIONAL CLASSIFICATION OF PATIENT WITH HEART DISEASE CLASS Ι -Asymptomatic CLASS ΙΙ –Symptoms with ordinary activity but comfortable at rest. CLASS ΙΙΙ –Symptoms with minimal activity but comfortable at rest. CLASS ΙV – Symptoms at rest Signs Palpation: Small volume pulse Tapping apex-palpable S1 Palpable S2 Atrial fibrillation Signs of raised pulmonary capillary pressure Crepitations, pulmonary oedema, effusions Signs of pulmonary hypertension RV heave, loud P2 Auscultation: Loud S1 P2 component accentuated. A2-P2 Split. S2 to OS interval inversely proportional to severity Diastolic rumble: length proportional to severity In severe MS with low flow- S1, OS & rumble may be inaudible Lab examination Chest x-ray Straightening of left border of cardiac silhouette. Prominent main pulmonary arteries. Dilation of the upper lob pulmonary veins. Backward displacement of the esophagus by enlarged left atria. ELECTROCARDIOGRAPHY The ECG may show LA enlargement, Manifest as a P wave lasting> 0.12 msec with prominent negative deflection of its terminal component (duration: > 0.04 msec; amplitude: >0.10 mV) in V1; Broad, notched P waves in lead II; or both. Low voltage in V1, Right axis QRS deviation, and tall R waves in V1 suggest RV hypertrophy Echocardiography Diagnosis of Mitral Stenosis Assessment of hemodynamic severity ◦ mean gradient, mitral valve area, pulmonary artery pressure Assessment of right ventricular size and function. Diagnosis and assessment of concomitant valvular lesions Reevaluation of patients with known MS with changing symptoms or signs. F/U of asymptomatic patients with mod-severe MS Diagnosis History Symptoms Signs on physical examination X-ray chest Electrocardiogram Echocardiography Anesthetic management The main objectives are- To maintain sinus rhythm To avoid tachycardia To avoid large increase in cardiac output To avoid hypovolemia and fluid overload. A thorough history and examination to be done. Investigation- Hemogram Blood sugar ,blood urea ,s.creatinine x-ray chest Electrocardiogram Echocardiography PREOPERATIVE MEDICATIONS Antianxiety drugs decrease tachycardia associated with anxiety. Drugs used for heart rate control should be continued until the time of surgery. If diuretics are used treat hypovolemia and hypokalemia if associated. For minor procedures continue the anticoagulant therapy. For major surgery discontinue. For regional anesthesia anticoagulant tests should be performed. ANESTHESIA TECHNIQUE-Patients may be very sensitive to the vasodilating effect of spinal and epidural anesthesia. Epidural is preferable over spinal anesthesia because of the more gradual onset. General Anesthesia Premedication -Avoid premedication with anticholinergics to avoid tachycardia. opioiods like fentanyl are used to give analgesia. Induction –Induction can be achieved with any available iv induction agent except KETAMINE as it increases heart rate and blood pressure. For muscle relaxation agents that do not release histamine are preferred as histamine causes tachycardia and hypotension. Steroidal group of muscle relaxants does not cause histamine release. Example are- VECURONIUM, ROCURONIUM, PANCURONIUM. Benzylisoquinolinium group causes histamine release. Example are – ATRACURIUM, CISATRACURIUM, MIVACURIUM. Succinylcholine also causes slight release in histamine. Maintenance Accomplished by use of drugs with minimal effects on heart rate, contractility, systemic and pulmonary vascular resistance. Achieved by –nitrous oxide & opioid. low conc. Of volatile anesthetic For muscle relaxation vecuronium is preferred. Avoid light anesthesia. Intra-op fluid administration should be carefully titrated because these patients are very susceptible to volume overload and the development of pulmonary edema. Monitoring Noninvasive monitoring like HR, BP , ECG, RR, SpO2. Invasive monitoring depends upon-Complexity of the operative procedure. -Magnitude of physiological impairment. Transesophageal echocardiography could be useful in patients with symptomatic mitral stenosis undergoing major surgery. In symptomatic patients and major surgery continuous monitoring of IBP , pulmonary artery pressure and left atrial pressure should be considered. If there is intra-op tachycardia –deepen the plane β-blocker eg. Esmolol and propranolol. If hypotension occurs phenylephrine is preferred over ephedrine because it lacks the β adrenergic activity. If atrial fibrillation occurs ventricular rate is controlled with diltiazem and digoxin. For sudden supraventricular tachycardia –cardioversion. Reversal of anesthesia. Reversal nondepolarising muscle relaxants is achieved slowly with neostigmine and glycopyrrolate to reduce drug induced tachycardia caused by glycopyrrolate. Post operative management . Proper pain management to avoid tachycardia. Risk of pulmonary edema and right heart failure continue so cardiovascular monitoring should be continued. Oxygen supplementation until adequate oxygenation is established. Management of post op hypothermia and shivering. Thank You……….