* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cancer and the Immune System
Immune system wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Molecular mimicry wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Adaptive immune system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Innate immune system wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
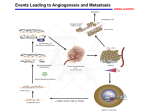
Cancer and the Immune System Immunology Chapter 22 April 22, 2003 Amar Bhatt Shirley Masand Jaime Warmkessel A Look Ahead • • • • • Tumors and Metastasis Oncogenes and Cancer Induction Tumor Antigens Tumors and the Immune Response Immunotherapy FATAL SYSTEM ERROR An exception error has occurred at AP222003C22. A virus has been detected. Quarantine has failed but the virus has been identified. Press the Any key to return to windows in safe sesame mode. Cancer and the Immune System Cancer “altered self-cells that have escaped normal growth regulation mechanisms” neoplasm: tumor benign vs. malignant metastasis: spreading of cancerous cells via blood or lymph to various tissues Metastasis 22.1 Types of Cancers carcinoma: endodermal/ectodermal tissue leukemia/lymphoma: hematopoeitic stem cells sarcoma: mesodermal connective tissues What makes cancer “cancer”? 1. decreased requirements for growth factors and serum 2. are no longer anchorage dependent 3. grow independently of density normal cells: eventually enter Go confluent monolayer contact inhibition CHECKPOINT FAILURE Malignant Transformation are like in vitro cancers two phases 1. initiation (changes in genome) 2. promotion (proliferation) Malignant Transformation chemical and physical carcinogens virally induced transformation cultured tumors: good models for study cancer cells are basically immortal Oncogenes… oncogene: “cancer gene”; often found in viral genomes proto-oncogene: cellular counterpart which can be turned into an oncogene What can go right? induction of cellular proliferation inhibition of cellular proliferation, a.k.a. tumorsuppressor genes regulation of programmed cell death What can go wrong? chromosomal translocations tandem repeats: HSRs mutations in proto-oncogenes viral integration growth factors and their receptors Induction of Cancer Fig. 22.2 Induction of Cancer Lets Visualize! http://science.education.nih.gov/supplem ents/nih1/cancer/activities/activity2_anim ations.htm Tumors of the Immune System Lymphomas Solid tumors w/in lymphoid tissue (bone marrow, lymph nodes, thymus) Hodgkin’s & non-Hodgkin’s http://www.lymphomainfo.net/ Leukemias Proliferate as single cells Acute or Chronic depending on the progression of disease Acute- appear suddenly and progress rapidly; arise is less mature cells (ie ALL, AML) Chronic- much less aggressive and develop slowly; mature cells (ie CLL and CML) Tumor Antigens TSTAs Tumor Specific Transplantation Antigen TATAs Tumor Associated Transplantation Antigen TSTAs Unique to tumor cells DO NOT occur on normal cells in the body Novel proteins created my mutation presented on class I MHC Can either be chemically/physically induced or virally induced tumor antigens Chemically/Physically Induced •Specific Immunologic Response that can Protect against later challenge by live cells Of the same line but not other tumor-line Cells. •Methylcholanthrene / UV light Fig 22.7 Virally Induced Express tumor antigens shared by all tumors induced by the same virus Burkitt’s Lymphoma Epstein Barr HPV Fig 22.9 TATAs NOT unique to tumor cells DO occur on normal cells in the body So where’s the problem? Fetal/adult presence Concentration of Growth Factors and Growth Factor Receptors TATAs cont’d Oncofetal Tumor Antigens (AFP & CEA) Normally appear in fetus before immunocompetence Later recognized as non-self Oncogene Proteins Human Melanomas Virally Induced Tumors Virally induced tumors have the same antigens for each tumor caused by that virus. HPV Immune Response to Tumors Mostly a cell-mediated response NK Cells Not MHC restricted Fc receptor binds to antibody coated tumor cell ADCC Chedieak-Higashi syndrome Macrophages Not MHC restricted Elicits ADCC TNF-alpha Immune Surveillance Theory So, you have a tumor cell. Now what? You need three things: 1. “See” the cancer Ternary complex and costimulation by B7 2. Activate lymphocytes Release IL-2, IFN-gamma, and TNF-alpha 3. Cancer cells must be susceptible to killing CTL lysis, macrophages, NK cells Info From: http://www.brown.edu/Courses/Bio_160/Projects1999/cancer/imevstca.html#Introduction But if the body has all these defenses, why do so many people still have cancer? Conniving Cancer. Bad antibodies? Some antibodies do not protect against tumor growth, but also ENHANCE it. Release of immunosuppressive cytokines transforming growth factor-beta (TGF-beta), interleukin-10 (IL-10) and vascular endothelial growth factor (VEGF) Hide and go Seeking Antigen Antigens actually seem to “hide” in the presence of antibody Also, some cancer cells completely shed themselves of the antigen TGF-beta IL-10 VEGF Inhibition of T-cell growth + - + Inhibition of CTL differentiation + + + Inhibition of cytokine production + + - Induction of T-cell anergy + - - Downregulation of cytotoxic potential + + - Inhibition of antigen presentation + + - Shift in the Th1-Th2 balance towards Th2 + + - Downregulation of adhesion/costimulatory molecules + + - Resistance to CTL-mediated lysis - + - Effect Source: Chouaib et al 1997 Conniving Cancer cont. Reduction in Class I MHC Molecules And the final blow… Lack of CoStimulatory Signal Cancer Immunotherapy Manipulation of Co-Stimulatory Signal Enhancement of APC Activity Cytokine Therapy Monoclonal Antibodies Cancer Vaccines Manipulation of CoStimulatory Signal Tumor immunity can be enhanced by providing the co-stimulatory signal necessary for activation of CTL precursors (CTL-Ps) Fig. 22.11a Manipulation of CoStimulatory Signal Cont. Basis for Vaccine Prevent metastasis after surgical removal or primary melanoma in human patients Enhancement of APC Activity GM-CSF (Granulocyte-macrophage colonystimulating factor) remember: CSFs are cytokines that induce the formation of distinct hematopoietic cell lines Fig 22.11b Cytokine Therapy Use of recombinant cytokines (singly or in combination) to augment an immune response against cancer Via isolation and cloning of various cytokine genes such as: IFN-α, β, and γ Interleukin 1, 2, 4, 5, and 12 GM-CSF and Tumor necrosis factor (TNF) Cytokine Therapy Cont. I. Interferons • Most clinical trials involve IFN-α • Has been shown to induce tumor regression in hematologic malignancies i.e. leukemias, lymphomas, melanomas and breast cancer • All types of IFN increase MHC I expression • IFN-γ also has also been shown to increase MHC II expressionon macrophages and increase activity of Tc cells, macrophages, and NKs Cytokine Therapy Cont. II. Tumor Necrosis Factors • Kills some tumor cells • Reduces proliferation of tumor cells without affecting normal cells How? • Hemorrhagic necrosis and regression, inhibits tumor induced vascularization (angio-genesis) by damaging vascular endothelium Cytokine Therapy Cont. III. In Vitro-Activited LAK & TIL cells A. Lymphocytes are activated against tumor antigens in vitro • Cultured with x-irradiated tumor cells in presence of IL-2 • Generated lymphokine activated killer cells (LAKs), which kill tumor cells without affecting normal cells In Vitro-Activated LAK and TIF cells Cont. B. Tumors contain lymphocytes that have infiltrated tumor and act in anti-tumor response • via biopsy, obtained cells and expanded population in vitro with • generated tumor-infiltrating lymphocytes (TILs) Monoclonal Antibodies • Anti-idiotype • Growth Factors -HER2 • Immunotoxins Cancer Vaccines • Genetic Biochemical HPV Human Papilloma Virus E6 E7 From Normal to Abnormal: For more info HPV Cancer Vaccines This Day Has Been Brought to you By the Letter… C C is for Cancer!