* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
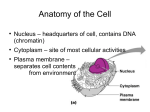
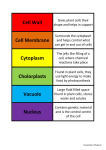
Download Cytoplasm - Austin Community College
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Lymphopoiesis wikipedia , lookup
X-linked severe combined immunodeficiency wikipedia , lookup
Innate immune system wikipedia , lookup
MLAB 1415- Hematology Keri Brophy-Martinez Chapter 7: Leukocytes Terms Myelopoiesis - the production and development of myeloid cells in the bone marrow Leukocytes Function Protect the host from infectious agents or pathogens Innate=Natural Immune response 1st response to pathogens (nonself) Always available Adaptive Immune response Starts in lymphoid tissue Slow Long-lasting immunity (memory) Lymphocytes become “activated” Differentiation & Maturation 1. 2. 3. Leukocytes develop from HSC (hematopoietic stem cell) Common Myeloid progenitor (CMP) cell gives rise to the committed precursor cells for the neutrophilic, eosinophilic, basophilic and monocytic lineages. Once lineage commitment has occurred, maturation begins. Maturation Changes Nucleoli disappear Chromatin condenses Nuclear mass indents and segments Cytoplasm becomes granular & pinkens Neutrophil Lifespan Three areas Bone marrow Peripheral blood Differentiation, proliferation, maturation Circulate for a few hours Tissues Work in host defense Regulation Neutrophil production primarily regulated by cytokines Interleukin-3 Granulocyte -monocyte-colony stimulating factor (GM-CSF) Granulocyte-colony-stimulating factor (G-CSF) Maturation of the granulocytic series **Least mature to mature** Myeloblast Size: 14-20µm Cytoplasm Nucleus Slight amount/blue No granules ((possible Auer rods to be discussed in another section) Round/Central or eccentric Reddish purple 1-3 nucleoli Fine meshlike/lacy chromatin with no clumping N:C ratio = 4:1 Maturation of the granulocytic series Promyelocyte (progranulocyte) Size: 15-21 µm Cytoplasm Increased amount/blue Fine, azurophilic, nonspecific granules present Nucleus Round/Central or eccentric Reddish-purple Fine, meshlike/lacy chromatin beginning to clump 1-2 nucleoli N:C ratio = 3:1 Maturation of the granulocytic series Myelocyte Last myeloid cell capable of division Size: 12-18µm Cytoplasm Nucleus Increased, bluish-pink (“dawning of neutrophilia”) Fine azurophilic, specific granules Secretory vesicles Round or oval/eccentric Reddish-purple Chromatin loosely clumped No nucleolus N:C ratio = 2:1 or 1:1 Maturation of the granulocytic series Metamyelocyte Also called “meta” or “juvenile” Size: 10-18µm Cytoplasm Nucleus Moderate amount Specific granules (neutrophilic, eosinophilic or basophilic) Tertiary granules Secretory vesicles Indented (kidney-bean shaped) Central or eccentric Purple Clumped chromatin No nucleolus N:C ratio = 1:1 Maturation of the granulocytic series Band 1st stage found in P.B Size: 9-15µm Cytoplasm Moderate amount Specific granules (see meta) Nucleus Elongated, narrow band (sausage) shape with uniform thickness Central or eccentric Clumped, coarsely granular chromatin Maturation of the granulocytic series Segmented neutrophil, eosinophil or basophil Size: 10-16µm Cytoplasm Neutrophil - Granules stain equally with eosin and methylene blue, causing a pinkish appearance Eosinophil - Granules stain mainly red, due to reaction with eosin in stain Nucleus Normal in circulation = 0-5% Basophil - Granules stain mainlyblue, due to the reaction with methylene blue in stain Normal in circulation = 40 - 80% Normal in circulation = 0-1% Mast cell is a tissue basophil Neutrophil - purplish-red, clumped granular chromatin, 2-5 distinct nuclear lobes connected by a filament of chromatin Eosinophil - deep blue purple, coarsely granular chromatin, 2 distinct lobes Basophil - deep blue purple, coarsely granular chromatin, 2 nuclear lobes (sometimes obscured by cytoplasmic granules) Maturation of the granulocytic series Basophil Eosinophil Function of the granulocytic series Neutrophils Eosinophils Defense against bacterial infections Regulate inflammation Respond to antigenic stimulation in chronic allergies Interact with larval stages of some helminthic parasites Basophils Histamine in granules plays a role in acute, systemic allergic reactions (sudden release of histamine can cause anaphylactic shock) Granules also contain heparin Granulocytes Why are they called granulocytes? The granules are lysosomes created by lipids that contain hydrolytic enzymes such as peroxidase, acid phosphatase, lysozyme and specific esterase. MONOCYTES Monopoiesis - the production and development of monocytes, macrophages and their precursors. Monocytes are produced in the bone marrow. MONOCYTES Function Protect the host from infectious agents or pathogens via innate and adaptive immune response Phagocytosis Scavengers MONOCYTES Differentiation & maturation Lifespan Produced from CFU-GM Can further differentiate into macrophages in the tissues P.B ~ 8 hours Tissue Regulation Production primarily regulated by cytokines GM-CSF IL-3 M-CSF Maturation of the monocytic series Monoblast Size: 12-20µm Cytoplasm Nucleus Blue, moderate amount No granules Round, oval or slightly folded Eccentric Reddish-purple Chromatin fine and lacy Vacuoles may be present 1-2 nucleoli N:C ratio = 4:1 Maturation of the monocytic series Promonocyte (difficult to discern) Size: 12-20µm Cytoplasm Nucleus Paler gray-blue and abundant “Bleb-like” pseudopods at periphery May contain fine red “dust-like” particles, azurophilic granules Vacuoles may be present Round with chromatin creases or brain-like folding Central Reddish-purple with light clumping of chromatin 0-2 nucleoli N:C ratio = 3:1 or 2:1 Promonocyte Maturation of the monocytic series Mature monocyte Normal in circulation: 2-9% Size: 12-20µm Cytoplasm Nucleus Pale gray-blue and abundant Bleb-like pseudopods at periphery, variable shape Numerous fine pale red dustlike granule scattered throughout Vacuoles common Increased folding or elongated Central Purplish with finer clumped chromatin No nucleoli N:C ratio = 2:1 or 1:1 Monocyte Macrophages Once the monocyte enters the tissues, it becomes a macrophage Size:15-80µm Cytoplasm Gray-blue and abundant Ragged edges Vacuoles common Nucleus Round with netlike appearance Purplish with finer clumped chromatin Nucleoli appear Macrophage alias’ Histiocytes in the loose connective tissue Kupffer cells in the liver Osteoclasts in the bone Microglial cells in the nervous system Also scattered throughout the body in all organ tissues (spleen, lung, abdomen, etc.) One monocytes have grown into macrophages, they do not normally reenter the bloodstream except in cases of inflammation Macrophage Lymphocytes Differentiation & Maturation Develop from HSC (hematopoietic stem cell) Common Myeloid progenitor (CMP) cell and Common lymphoid progenitor cell (CLP) gives rise to the committed precursor cells: T lymphocytes (60-80% of lymph population) B lymphocytes (10-20%) thymus Bone marrow Natural killer cells Lifespan Primary lymphoid tissue Bone marrow Secondary lymphoid tissue Lymph node, spleen, Peyer’s patches in intestine and mucosal tissues such as tonsils Active immune response occurs in above tissues where lymphs communicate and interact with antigen-presenting cells, phagocytes and macrophages LYMPHOCYTES: T cells Function Cellular immune response (they do not produce antibodies) Three subsets Helper T cells Instrumental in aiding B cells in antibody production Suppressor T cells Act as a “thermostat” to shut off the system or keep it under control Cytotoxic T cells Destroy by lysis of target cells (such as tumor cells) Play a role in inflammatory response Host defense when stimulated by interferon against certain viruses (cytomegalovirus - CM, and hepatitis) by killing the virally infected target cell before the virus replicates Responsible for chronic organ graft rejection. (T cells have many unique antigens on their cell surfaces, some of which are the HLA - human lymphocyte antigen - markers. HLA markers are instrumental in chronic graft rejection and that is why tissue typing is done to establish a good donor match.) LYMPHOCYTES: B cells Function Humoral immune response by transforming into antibody-producing plasma cells Defense against encapsulated bacteria such as Streptococci Mediate hyperacute organ rejection Lymphocytes: NK cells Function Recognize and kill tumor cells Recognize and kill cells infected with a virus Maturation sequence of lymphocytes Lymphoblast Cell size: 10-18µm Cytoplasm Nucleus Blue/scanty No granules, Auer rods are never present Purple, smooth chromatin Smudged Round, central or eccentric 1-2 nucleoli N:C ratio = 4:1 Maturation sequence of lymphocytes Prolymphocyte (difficult to distinguish) Size: 9-18µm Cytoplasm Nucleus Blue, scanty Usually granules are absent, but a few azurophilic granules may be present Purple, condensed chromatin Round or indented, eccentric 0-1 nucleoli N:C ratio = 3:1 Maturation sequence of lymphocytes Mature lymphocyte Normal adult value: 2535% Cell size: 7-10µm (a typical normal lymph has a nucleus that is the size of a normal RBC) Cytoplasm Light blue, scanty to moderate Few azurophilic granules may be present Nucleus Purple, dense, clumped chromatin Round or indented, eccentric No nucleoli Large lymphocytes versus monocytes Size Nucleus Large lymph: clumped, condensed Mono: lacy, brainlike folds Granules Large lymph: 12-15µm Mono: 15-18µm Large lymph: large azurophilic, easy to count Mono: red, fine Cytoplasm Large lymph: clear, nongranular, may be indented by red cells Mono: “ground glass” appearance, projection of blunt pseudopod blebs Maturation sequence of lymphocytes Variant lymphs Other terms used are reactive, atypical, activated, Downey cell, transformed, virocyte, plasmacytoid Can be T or B cells Caused by antigenic stimulants such as viruses, post-transfusion reactions and organ transplants General characteristics Increased size due to DNA activity in the nucleus and RNA activity in the cytoplasm Enlarged and/or monocytoid nucleus Variation in nuclear chromatin pattern Nucleus may contain 1-3 nucleoli Abundant, sometimes foamy or vacuolated cytoplasm Variation in cytoplasmic color - gray-blue to intense blue Absence of granules in cytoplasm Reactive lymphocyte Plasma cells Plasma cells Function is the synthesis and excretion of antibodies (immunoglobulins) Normally not present in the peripheral blood; comprise 2% of bone marrow cells. (May be seen in the peripheral blood in the disease called multiple myeloma, a disease of uncontrolled production of immunoglobulins.) End stage of the B lymphocyte Appearance Size: 10-18µm Cytoplasm is dark blue with perinuclear halo and may contain vacuoles indicating antibody synthesis Nucleus is round, eccentric, dark purple with dense clumped chromatin Variant plasma cells Grape or Mott cell - cytoplasm completely filled with red, pink or colorless globules called Russell bodies Flame cell - cytoplasm stains bright red-staining proteinaceous material Plasma cells