* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download VAN 504 Lecture 06
Adaptive immune system wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Myasthenia gravis wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Innate immune system wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
X-linked severe combined immunodeficiency wikipedia , lookup
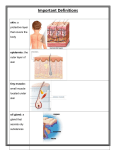
VAN 504 Lecture 06 Sense organs, Endocrines and lymphoid organs of domestic animals & birds Receptors • Mechanoreceptors: respond to touch, pressure, vibration, stretch, and itch • Thermoreceptors: sensitive to changes in temperature • Photoreceptors: respond to light energy (e.g., retina) • Chemoreceptors – respond to chemicals (e.g., smell, taste, changes in blood chemistry) • Nociceptors: sensitive to pain-causing stimuli • Osmoreceptors : detect changes in concentration of solutes, osmotic activity • Baroreceptors : detect changes in fluid pressure • Exteroceptors – sensitive to stimuli arising from outside the body – Located at or near body surfaces – Include receptors for touch, pressure, pain, and temperature • Interoceptors – (visceroceptors) receive stimuli from internal viscera – Monitor a variety of stimuli • Proprioceptors – monitor degree of stretch – Located in musculoskeletal organ Sense Organs • Chemical Senses • Chemical senses are those that detect particular molecules in the external or internal environment. • Chemical senses that detect molecules outside the body include gustation (taste) and olfaction (smell). • Within the body, the chemical senses include the detection of blood pH and carbon dioxide concentration. Gustation • Taste, or gustation, is the sensation associated with dissolved substances contacting specialized receptor cells on the tongue and throat region. The receptors, called taste cells, are arranged in a group with supporting cells, a cluster that constitutes the taste bud. Taste buds are not distributed evenly on the surface of the tongue; they are confined to specific forms of papillae (tiny projections), the vallate, foliate, and fungiform papillae, which are found on the tongue, soft palate, parts of the pharynx, and epiglottis of the larynx. • Somatic sensations (heat, cold, touch, pain) from the tongue are conveyed by branches of the trigeminal and glosso pharyngeal nerves. • Traditionally, four basic taste sensations have been identified. These are sweet, salt, bitter, and sour. Individual taste cells have membrane receptor to detect the chemical substances associated with these tastes. • For them to stimulate taste cells, chemicals must be in solution, an important function of saliva. Photomicrograph of a taste bud. Individual cells include taste cells and other non-neural supportive cells. Taste bud Olfaction • Olfaction is the sense of smell. • Olfactory sensory neurons are scattered among supporting cells through out the olfactory mucosa in the nasal cavity . The apex of each olfactory neuron bears a single dendrite with a tuft of several fine hair like projections, which bear the chemical receptors for the sense of smell. An axon from each olfactory neuron collectively constitutes the olfactory nerve which make up the olfactory tracts of the brain. • There is a subset of olfactory sensory neurons outside the olfactory epithelium that innervate the mucosa of the vomeronasal organ, a diverticulum of the nasal cavity in the hard palate. These olfactory neurons appear to be receptors for pheromones, chemical substances that can influence the behavior of other individuals. Pheromones are likely especially important in reproductive behaviors. Olfactory system. The view is of the equine head in sagittal section. Inset shows a microscopic view of the olfactory epithelium, which covers the ethmoid bone within the caudo dorsal nasal cavity. a, nasal cavity; b, palate; c, oral cavity; d, larynx; e, pharynx; f, vomero nasal organ; g, olfactory bulb of brain. Hearing EAR The ear can be divided into three main parts: 1.The external ear extends from the exterior as far as the tympanic membrane (eardrum). 2.The middle ear begins at the tympanic membrane; it is an air-filled space with in the temporal bone. 3.The inner ear is housed entirely in the temporal bone, forming an elaborate fluid-filled system of chambers and canals . External Ear • The part of the ear visible on the outside of the head, the auricle, or pinna, varies considerably in shape and size between and within species. Its shape and rigidity is due to the auricular cartilage, an elastic cartilage that is somewhat funnel shaped. • The pinna acts as a capturing device for air pressure waves, and its shape and mobility are structurally important for sound localization. The many skeletal muscles that move the pinna are loosely categorized as rostral and caudal auricular muscles. • A tubular extension of the pinna, the cartilaginous external acoustic canal, extends from the pinna to the tympanic membrane. • The external acoustic canal is lined with a modified skin possessing few hairs and abundant sebaceous and ceruminous glands. The combined secretion of these glands is called cerumen, a brown waxy substance that protects the canal. • A separate annular cartilage adjacent to the funnel-shaped base of the auricular cartilage forms most of the external acoustic canal. • A third cartilage, the scutiform cartilage, lies medial to the auricular Middle Ear • The middle ear is an air-filled space, the tympanic cavity, lined by mucous membrane and contained within the temporal bone. • In most domestic animals, the middle ear features a ventrally expanded cavity, the tympanic bulla, visible on the ventral surface of the skull. The middle ear is closed to the external acoustic canal by the intact tympanic membrane and communicates with the naso pharynx via the auditory tube (formerly eustachian tube). In the horse, the auditory tube is expanded to form the large air-filled guttural pouch. • Three auditory ossicles span the middle ear from tympanic membrane to the vestibular(oval) window. From superficial to deep, they are the 1.malleus (hammer), 2.incus (anvil), 3.stapes (stirrup) . These tiny bones provide a mechanical linkage from the tympanic membrane to the vestibular window, and through them vibrations are transmitted from the former to the latter. Middle ear There are also two striated muscles with in the middle ear, 1. m. tensor tympani 2. m. stapedius. These two small muscles damp vibrations of the auditory ossicles in the presence of excessively loud noises. The chorda tympani, a branch of the facial nerve, passes through the tympanic cavity. Infections of the middle ear (otitis media) can be associated with dysfunction of this nerve. In horses, cranial nerves VII and IX through XII and the continuation of the sympathetic trunk pass adjacent to the guttural pouch, separated from its interior only by mucous membrane. Diseases of the guttural pouch can therefore produce distinctive neurologic dysfunctions when these nerves are affected. Internal Ear • The internal ear is housed entirely within the petrous temporal bone. • It is a multi chambered membranous sac (the membranous labyrinth) closely surrounded by a sculpted cavity of bone (the osseous labyrinth). • The membranous labyrinth in the internal ear is a system of fluid-filled sacs and ducts. The primary anatomic features of the membranous labyrinth are 1. Two enlargements, the utriculus (utricle) and sacculus (saccule); 2.Three loops attached to the utriculus, the semicircular ducts; 3. The spiraled cochlear duct. These are filled with a fluid, the endolymph. Internal Ear The membranous labyrinth is housed in the osseous labyrinth. The osseous labyrinth is filled with perilymph. The inner ear may be divided into two functional parts. 1. In one, the osseous labyrinth forms a coiled, snail shell– shaped cochlea, inside of which is the cochlear duct, an extension of the membranous labyrinth. The cochlear duct houses the receptors for audition. 2. The second part constitutes the vestibular apparatus. Within the utriculus, sacculus, and semicircular ducts that constitute the vestibular apparatus are the receptors that detect accelerations of the head, including acceleration due to gravity. Accelerations of the head contribute to the sense of equilibrium or balance. Vision • The eye is an organ whose primary function is to collect and focus light upon the photosensitive retina. • It lies within a cone shaped cavity of the skull, the orbit, which houses the eyeball (globe) and a number of other soft tissue structures, the ocular adnexa(e.g., muscles, glands), that act upon the eye ball in service of its light-collecting function. • Unlike the human orbit, which is a complete bony cone, the ventral portion of the orbit of domestic species is bounded by soft tissues, notably the pterygoid muscles. Ocular Adnexa • Palpebrae. Two mobile folds of haired skin protect the anterior aspect of the eyeball. These are the eyelids, or palpebrae. The gap between the margins of the two palpebrae is the palpebral fissure, and its shape and size are controlled by the muscles of the eyelids. • Tarsal plate (tarsus)- A layer of dense connective tissue in the palpebrae, that affords them a certain amount of rigidity. • The palpebrae have thin but otherwise typical haired skin on their superficial side. This skin ends at the lid margin with a sharp transition to mucous membrane. • The margin may have cilia (eyelashes). • Abundant modified sweat and sebaceous glands are associated with the lid margin. • Tarsal glands (meibomian glands ) A row of large modified sebaceous glands. The tarsal glands are present in both palpebrae and open into a shallow furrow near the muco cutaneous junction of the eyelid. The tarsal glands produce an important oil layer of the tear film. The conjunctiva is the mucous membrane that lines the inside of the palpebrae and part of the anterior surface of the eyeball (excluding the clear cornea). The conjunctiva is rich in mucusproducing glands, lymphocytes, nerves, and blood vessels. The very small space between the eyelids and the surface of the eye is the conjunctival sac. Membrane, or third eyelid. This is a fold of mucous membrane. It is given rigidity by a T-shaped cartilage within it, and it smoothes the tear film and protects the cornea. The third eyelid has at its base a serous gland, called simply the gland of the third eye lid, which normally contributes about 50% of the tear film. Ruminants, the pig, and laboratory rodents possess another deeper gland associated with the third eyelid. This is the harderian gland. It, too, contributes to the tear film. Lacrimal Apparatus. The lacrimal apparatus comprises a series of serous, seromucoid, and mucous glands and the duct systems that drain their secretions from the conjunctival sac. It provides a moist environment for the anterior surface of the eye. The lacrimal gland lies in the dorsolateral portion of the orbit; its secretion, together with that of the gland of the third eyelid, is the major contributor to the tear film. The tears drain from the conjunctival sac via two small openings on upper and lower palpebrae near the medial corner. These are the superior and inferior lacrimal puncta, which open into short ducts (superior and inferior canaliculi) that join one another at a small sac (lacrimal sac) near the medial corner of the eye that is the origin of the nasolacrimal duct. The nasolacrimal duct travels through the bones of the face to open into the nasal cavity and/or just in side the nostril. Moisture on the nose of domestic animals is largely derived from the tears Lacrimal Apparatus • The lacrimal apparatus. Tears produced by the lacrimal gland and gland of the third eyelid are drained at the medial corner of the eye at superior and inferior lacrimal puncta. The two canaliculi converge at the lacrimal sac, and from there tears flow via the nasolacrimal duct to the vestibule of the nostril. Extra ocular Muscles. The globe of the eye moves by the action of following striated muscles, designated extra ocular muscles . (Fig. 11-10). The m. retractor bulbi - Contraction of the m.retractor bulbi results in retraction of the eye ball into the orbit. Also, a series of four straight muscles originate at the apex of the orbit and project to the equator of the globe, superficial to the four bellies of the m. retractor bulbi. They are named for their insertion on the globe: m.rectus dorsalis, rectus ventralis, rectus medialis,and rectus lateralis. The m. obliquus dorsalis (dorsal oblique m.) l When the dorsal oblique muscle contracts, the dorsal part of the eyeball is pulled toward the medial portion of the orbit (i.e., the left eye ball rotates counter clock wise and the right rotates clockwise). The m. obliquus ventralis (ventral obliquem.) The ventral oblique muscle rotates the globe opposite to the rotation produced by the dorsal oblique muscle. The m. levatorpalpebrae superioris is the primary lifter of the upper eyelid. The periorbita is a cone-shaped connective tissue sheath that surrounds the eyeball and its muscles, nerves, and vessels. The peri orbita contains circular smooth muscle that squeezes its contents and places the eye ball forward in the orbit. Because of its location behind the eyeball, the adipose tissue is frequently called retrobulbar fat. Globe • The eyeball (globe) comprises three concentric layers: 1. Fibrous tunic, 2. Vascular tunic, 3. Nervous tunic • The three tunics of the eyeball surround several chambers filled with either liquid or a gelatinous material. The posterior 75% of the globe is filled with an a cellular gel, the vitreous body, and as a consequence this portion is also called the vitreous chamber. • The lens divides it from the anterior segment of the eyeball. The anterior segment of the eye is filled with a fluid called aqueous humor. 1.Fibrous Tunic. The outer fibrous tunic of the eye ball is made up of a posterior opaque sclera and an anterior transparent cornea. Both are composed of very dense collagenous tissue. The sclera is white, variably tinged gray or blue; it meets the clear cornea at a transitional region called the limbus. The axons of the optic nerve pierce the sclera at the posterior pole of the eye, the area cribrosa. The tough sclera is the site of insertion for the extra ocular eye muscles. • The cornea is the transparent anterior part of the fibrous tunic. It is the most powerful refracting layer of the eye; its transparency and regular curvature are therefore critical elements for focusing of light on the retina. Corneal transparency is a function of 1. lack of vascular elements and cells, 2. lack of pigment, 3.relative dehydration of the collagenous tissue, 4. a smooth optical surface (provided in conjunction with the tear film), 5. a highly regular, laminar pattern of collagen fibers that reduces light scatter. • The cornea’s anterior and posterior surfaces are covered with specialized epithelium, but most of its thickness is composed of collagen fibers. • Vascular Tunic (uvea) -The middle tunic of the eye ball, is composed of three parts, 1. The choroid 2. ciliary body 3. iris. Choroid. The posterior portion of the eye. It is highly vascular and possesses multiple layers. The deepest of these is the tapetum. The tapetum of animals is a reflective surface that bounces incoming light back on to the retina and enhances vision in low light. The ventral portion of the choroid is usually not reflective. The pig and most primates lack a tapetum. Ciliary body is the anterior continuation of the uvea. It is a circumferential thickening of the vascular tunic, and it gives rise to many fine suspensory ligaments that support the lens. When the muscles in the ciliary muscle contract, they allow the lens to assume a more spherical shape; this increases its refractive power, a change that brings close objects into focus on the retina. This process of focusing on near objects is called accommodation. Iris is the most anterior portion of the uvea and the only part of the • • • • vascular tunic normally visible in the living animal. It consists of a pigmented ring of tissue, perforated in its center by the pupil. The iris divides the aqueous filled anterior segment of the eye into anterior and posterior (between the iris and lens) chambers. The iris controls the amount of light entering the posterior part of the eye by changing the size of the pupil. The iris derives its color from pigmented epithelial cells primarily on the posterior surface of the iris. In herbivores, the pigmented epithelium of the posterior surface of the iris forms nodular masses along the margin of the pupil that are visible in the anterior chamber. These are often very large in horses, in which species they are called corporanigra. In cattle the same structures are usually smaller and are called iridial granules. The site where the anterior surface of the iris meets the fibrous tunic is the iridocorneal angle (filtration angle); there the aqueous produced by the ciliary body is reabsorbed into the venous circulation. The deepest layer of the eye ball is the internal (nervous) tunic or retina. The light- sensitive part of the retina extends from just posterior to the ciliary body to the site at which nerve fibers exit the eyeball near the posterior pole of the globe. • • • • In clinical practice the retina is routinely viewed through the pupil with an ophthalmoscope; the portion of the retina that can be viewed in this manner is called the fundus. The retina has many layers. One of these is the photoreceptor layer, in which are found the specialized neural receptor cells of the visual system, the rods and cones. Photoreceptors have one of two basic shapes: 1.The cylindrical photoreceptors are rods, equipped with a photo pigment that renders them sensitive to very low levels of light. 2. The tapering photoreceptors are cones. Cones are color receptors. Most domestic animals have some color vision. Their retinal cones are primarily sensitive to blue and yellow wave lengths of light, with few or no red-sensitive cones. Vision in these species is probably rich in blue, green, and yellow tones. The flapping red cape wielded by the matador there fore attracts the bull by its movement and not by its color. • lens is a transparent proteinaceous biconvex disk suspended between the posterior chamber and the vitreous chamber. • It is surrounded by an elastic capsule. • Cells of the lens are called lens fibers, and they are generated continuously through out life. • As the animal ages, more lens fibers are added to the outside of the lens, compressing the fibers at the center. These old cell sharden and after middle age begin to lose their transparency. This change is lenticularsclerosis. Although the sclerotic lens looks milky, lenticular sclerosis does not usually interfere with vision. More severe changes in the lens fibers can produce significant opacity that interferes with transmission of light and therefore vision. These opacities are cataracts. Endocrine system • Endocrine system – Consists of ductless glands • Secrete hormones directly into bloodstream – Affect the function of specific body organs • Regulates many intricate body functions Endocrines organs Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Exocrine • Produce secretions transported through ducts to destination • Endocrine • Ductless • Secrete specific chemicals (hormones) into circulation • Target cells Pituitary Gland • Referred to as “master gland” – Secretes hormones that control functions of other glands – Known as hypophysis – Has two distinct lobes with specific functions Pituitary Gland • Anterior Pituitary Gland = Adenohypophysis – Secretes Growth Hormone (GH) • Also called Somatotropic Hormone (STH) • Regulates growth of bone, muscle, and other body tissues – Secretes Adrenocorticotropic Hormone (ACTH) • Stimulates normal growth and development of adrenal cortex and secretion of corticosteroids – Secretes Thyroid-Stimulating Hormone (TSH) • Promotes and maintains normal growth and development of the thyroid gland • Stimulates secretions of the thyroid hormones – Secretes Lactogenic Hormone (LTH) • Also called Prolactin • Promotes development of breasts/ udder during pregnancy • Stimulates secretion of milk from breasts/ udder after parturition Anterior Pituitary Gland Pituitary Gland • Anterior Pituitary Gland – Secretes Follicle-Stimulating Hormone (FSH) • Stimulates secretion of estrogen and production of eggs in the female ovaries • Stimulates production of sperm in the male testes – Secretes Luteinizing Hormone (LH) • Stimulates female ovulation and the secretion of testosterone in the male – Melanocyte-Stimulating Hormone (MSH) • Controls intensity of pigmentation in pigmented cells of the skin Pituitary Gland • Posterior Pituitary Gland = Neurohypophysis – Secretes Antidiuretic Hormone (ADH) • Decreases excretion of large amounts of urine • Increases reabsorption of water by the renal tubules – Secretes Oxytocin • Stimulates contraction of the uterus during parturition • Stimulates release of milk from the breasts/ udder of lactating female in response to the suckling reflex of the infant Pineal Gland • Tiny, pinecone-shaped gland – Located behind dorsal aspect of midbrain region – Plays a part in supporting body’s biological clock • Regulation of patterns of eating, sleeping, and reproduction – Secretes melatonin • Induces sleep Thyroid Gland • Largest true endocrine gland • Thyroid follicles – sacs that compose most of thyroid – follicular cells – simple cuboidal epithelium that lines follicles – secretes thyroxine (T4) and triiodothyronine (T3) – Increases metabolic rate, O2 consumption, heat production (calorigenic effect), appetite, growth hormone secretion, alertness and quicker reflexes • Parafollicular (C or clear) cells secrete calcitonin with rising blood calcium – stimulates osteoblast activity and bone formation Histology of the Thyroid Gland Colloid of thyroglobulin Follicular cells C (parafollicular) cells Follicle thyroid follicles are filled with colloid and lined with simple cuboidal epithelial cells (follicular cells). Parathyroid Glands • Secrete parathyroid hormone (PTH) – increases blood Ca2+ levels • promotes synthesis of calcitriol • increases absorption of Ca2+ • decreases urinary excretion • increases bone resorption Adipose tissue Parathyroid capsule Parathyroid gland cells Adipocytes Thymus • Thymus plays a role in three systems: endocrine, lymphatic, and immune • Bilobed gland in the mediastinum superior to the heart – goes through involution after puberty • T cell maturation • secretes hormones (thymopoietin, thymosin, and thymulin) that stimulate development of other lymphatic organs and activity of T-lymphocytes Adrenal Gland • small gland that sits on top of each kidney • they are retroperitoneal like the kidney • adrenal cortex and medulla formed by merger of two fetal glands with different origins and functions Connective tissue capsule Zona glomerulosa Adrenal cortex Zona fasciculata Zona reticularis Adrenal medulla Adrenal Medulla • adrenal medulla – inner core, 10% to 20% of gland • Neuroendocrine gland – innervated by sympathetic preganglionic fibers – Chromaffin cells – when stimulated release catecholamines and a trace of dopamine directly into the bloodstream • effect is longer lasting than neurotransmitters – increases alertness and prepares body for physical activity – • mobilize high energy fuels, lactate, fatty acids, and glucose • glycogenolysis and gluconeogenesis boost glucose levels • glucose-sparing effect because inhibits insulin secretion – muscles use fatty acids saving glucose for brain – increases blood pressure, heart rate, blood flow to muscles, pulmonary air flow and metabolic rate – decreases digestion and urine production Adrenal Cortex • surrounds adrenal medulla and produces more than 25 steroid hormones called corticosteroids or corticoids • mineralocorticoids – zona glomerulosa – regulate electrolyte balance – aldosterone stimulates Na+ retention and K+ excretion, water is retained with sodium by osmosis, so blood volume and blood pressure are maintained • glucocorticoids – zona fasciculata – regulate metabolism of glucose and other fuels – especially cortisol, stimulates fat and protein catabolism, gluconeogenesis (glucose from amino acids and fatty acids) and release of fatty acids and glucose into blood – helps body adapt to stress and repair tissues – anti-inflammatory effect becomes immune suppression with long-term use • sex steroids – zona reticularis – androgens – sets libido throughout life; large role in prenatal male development (includes DHEA which other tissues convert to testosterone) – estradiol – small quantity, but important after menopause for sustaining adult bone mass; fat converts androgens into estrogen Lymphatic Organ overview • Consists of two semi-independent parts – A network of lymphatic vessels. – Lymphoid tissues and organs scattered throughout the body. • Returns interstitial fluid and leaked plasma proteins back to the blood. • Lymph – interstitial fluid once it has entered lymphatic vessels • A one-way system in which lymph flows toward the heart. • Lymph vessels include: – Microscopic, permeable, blind-ended capillaries – Lymphatic collecting vessels – Trunks and ducts Lymph (lympha = clear fluid) • • • • • • • • • • Derived from tissue fluid Contains more white blood cells than plasma Enters lymph node through afferent lymphatic vessels Flows through node in one direction Flows through sinuses in lymph node cortex and then into the medulla Exits the lymph node through efferent lymphatic vessels Must be returned to blood stream to maintain blood volume and pressure Protects body against foreign material Assists in circulation of body fluids between cells and bloodstream Transports dietary fats Lymphatic System: Overview Lymphatic Capillaries • Similar to blood capillaries, with modifications – Remarkably permeable – Loosely joined endothelial mini valves – Withstand interstitial pressure and remain open • The mini valves function as one-way gates that: – Allow interstitial fluid to enter lymph capillaries – Do not allow lymph to escape from the capillaries • During inflammation, lymph capillaries can absorb: – Cell debris – Pathogens – Cancer cells • Cells in the lymph nodes: – Cleanse and “examine” this debris • Lacteals – specialized lymph capillaries present in intestinal mucosa – Absorb digested fat and deliver chyle to the blood Lymphatic Collecting Vessels • • • • • • Have the same three tunics as veins 1.Tunica intima 2. Tunica media 3. Tunica adventita Have thinner walls, with more internal valves Anastomose more frequently Collecting vessels in the skin travel with superficial veins Deep vessels travel with arteries Nutrients are supplied from branching vasa vasorum Lymphatic Trunks • Lymphatic trunks are formed by the union of the largest collecting ducts • Major trunks include: – Paired lumbar, broncho mediastinal, sub clavian, and jugular trunks – A single intestinal trunk • Lymph is delivered into one of two large trunks – Right lymphatic duct – drains the right upper arm and the right side of the head and thorax. – Thoracic duct – arises from the cisterna chyli and drains the rest of the body. Lymph Transport • The lymphatic system lacks an organ that acts as a pump • Vessels are low-pressure conduits • Uses the same methods as veins to propel lymph – Pulsations of nearby arteries – Contractions of smooth muscle in the walls of the lymphatics Lymphoid Cells • Lymphocytes are the main cells involved in the immune response • The two main varieties are T cells and B cells • T cells and B cells protect the body against antigens • Antigen – anything the body perceives as foreign – Bacteria and their toxins; viruses – Mismatched RBCs or cancer cells Lymphocytes • T cells – Manage the immune response – Attack and destroy foreign cells • B cells – Produce plasma cells, which secrete antibodies – Antibodies immobilize antigens • Macrophages – phagocytize foreign substances and help to activate T cells • Dendritic cells – spiny-looking cells with functions similar to macrophages • Reticular cells – fibroblast like cells that produce a stroma, or network, that supports other cell types in lymphoid organs Lymphoid Tissue • Diffuse lymphatic tissue – scattered reticular tissue elements in every body organ – Larger collections appear in the lamina propria of mucous membranes and lymphoid organs • Lymphatic follicles (nodules) – solid, spherical bodies consisting of tightly packed reticular elements and cells – Have a germinal center composed of dendritic and B cells – Found in isolation and as part of larger lymphoid organs Lymph Node • Lymph nodes are the principal lymphoid organs of the body • Nodes are imbedded in connective tissue and clustered along lymphatic vessels • Aggregations of these nodes occur near the body surface in inguinal, axillary, and cervical regions of the body • Their two basic functions are: 1.Filtration – macrophages destroy microorganisms and debris 2. Immune system activation – monitor for antigens and mount an attack against them Structure of a Lymph Node • Nodes are bean shaped and surrounded by a fibrous capsule • Trabeculae extended inward from the capsule and divide the node into compartments • Nodes have two histologically distinct regions: a cortex and a medulla • The cortex contains follicles with germinal centers, heavy with dividing B cells • Dendritic cells nearly encapsulate the follicles • The deep cortex houses T cells in transit • T cells circulate continuously among the blood, lymph nodes, and lymphatic stream • Medullary cords extend from the cortex and contain B cells, T cells, and plasma cells • Throughout the node are lymph sinuses crisscrossed by reticular fibers • Macrophages reside on these fibers and phagocytize foreign matter Lymph Node Spleen • Largest lymphoid organ, located on the left side of the abdominal cavity beneath the diaphragm • It extends to curl around the anterior aspect of the stomach • It is served by the splenic artery and vein, which enter and exit at the hilus • Functions – Site of lymphocyte proliferation – Immune surveillance and response – Cleanses the blood • Stores breakdown products of RBCs for later reuse – Spleen macrophages salvage and store iron for later use by bone marrow • Site of fetal erythrocyte production (normally ceases after birth) • Stores blood platelets Structure of the Spleen • Surrounded by a fibrous capsule, it has trabeculae that extend inward and contains lymphocytes, macrophages, and huge numbers of erythrocytes • Two distinct areas of the spleen are: – White pulp – area containing mostly lymphocytes suspended on reticular fibers and involved in immune functions – Red pulp – remaining splenic tissue concerned with disposing of worn-out RBCs and blood borne pathogens Structure of spleen Thymus • A bi lobed organ that secrets hormones (thymosin and thymopoietin) that cause T lymphocytes to become immuno competent • The size of the thymus varies with age – In infants, it is found in the inferior neck and extends into the mediastinum where it partially overlies the heart – It increases in size and is most active during childhood – It stops growing during adolescence and then gradually atrophies Internal Anatomy of the Thymus • Thymic lobes contain an outer cortex and inner medulla • The cortex contains densely packed lymphocytes and scattered macrophages • The medulla contains fewer lymphocytes and thymic (Hassall’s) corpuscles • The thymus differs from other lymphoid organs in important ways – It functions strictly in T lymphocyte maturation – It does not directly fight antigens • The stroma of the thymus consists of star-shaped epithelial cells (not reticular fibers) • These star-shaped thymocytes secrete the hormones that stimulate lymphocytes to become immuno competent