* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Respiratory Tract Infections
Herpes simplex virus wikipedia , lookup
Bioterrorism wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Swine influenza wikipedia , lookup
Trichinosis wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Orthohantavirus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
West Nile fever wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Hepatitis C wikipedia , lookup
Tuberculosis wikipedia , lookup
Oesophagostomum wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Henipavirus wikipedia , lookup
Influenza A virus wikipedia , lookup
Leptospirosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Antiviral drug wikipedia , lookup
Whooping cough wikipedia , lookup
Hepatitis B wikipedia , lookup
Gastroenteritis wikipedia , lookup
Neonatal infection wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
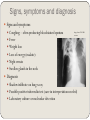
Respiratory Tract Infections Dr Lynne Lawrance 2A21 [email protected] Session Aims To give you an overview of a range of respiratory diseases that are predominantly infectious in nature To also link in to other module sessions to look at how microbes play a role in the pathology of diseases that have a more multi-factorial pathogenesis The Respiratory Tract – a microbiologists perspective! Same way in as out Has a normal flora in the upper region Many different environmental niches that different microbes could find suits their growth preferences Normal flora of one region of the tract can be a cause of disease if it gets somewhere else Public Domain Image from Wikipedia Some of the conditions with definite or possible microbial involvements Rhinitis Oral and oesophageal thrush Sinusitis Common cold Pharyngitis Diphtheria Whooping Cough Influenza Tonsillitis Epiglottitis Bronchitis Exacerbation of Cystic Fibrosis or other structural or mechanical disorders SARS Pneumonia Tuberculosis Bronchiolitis Plus the system is also linked to the ears and eyes and skin with no barriers It is suggested that the respiratory tract is the most common site of microbial infection However as there is a huge range of severities of these infections this almost goes unnoticed – after all just think how many coughs or mild flu like illnesses you have had! Upper respiratory tract infections (which includes most flu, coughs and colds) are the main reasons for GP visits in the US and probably in the UK as well But why?.... • Several reasons Air It has been estimated that indoors the air contains between 400 and 900 microbes per cubic metre, outside is less concentrated This is predominantly made up of non-pathogenic microbes However with an average ventilation rate of 6L per minute at rest this means that average person would inhale around 8 microbes per minute or >10,000 per day Fortunately the respiratory system is equipped with mechanisms for removing inhaled particles including microbes So normally the lungs are “almost sterile” due to the protective mechanisms Sneezing and Coughing When sneezing you eject around 20 000 water droplets derived from both the mouth and the nose During coughing microbes from the mouth predominate what is shed, but those from the lungs and the digestive tract can also be detected Larger droplet fall to the ground quite quickly, but smaller particles can become suspended in the air, almost like birds on thermal currents. These smaller particles are those we are most likely to inhale Being close to someone coughing and sneezing is recognised as a risk factor for acquiring the infection from them Survival of Microbes in the Air Some microbes can survive in the air for sometime e.g. TB, smallpox virus, foot and mouth virus (foot and mouth can cross the English Channel!!) Other dry out quickly and are inactivated e.g. measles, flu, meningococci (require close contact) Others fall in between e.g. Legionella (about 2km) Of course we also deposit these microbes on to tissue, hankies and hands which adds to transmission The Normal Flora The upper respiratory tract has a complex normal flora that resides on the many varied surfaces Amongst this normal flora a number of potential lower respiratory tract pathogens reside – especially it seems in the nasopharyngeal/oropharyngeal area Streptococcus pneumonaie, Haemophilus influenzae, Moraxella catarrhalis, Staphylococcus aureus However the normal flora also protect against other potential upper respiratory tract pathogens Selected Upper Tract Infections Whooping Cough - Pertussis Caused by Bordetella pertussis infecting the nasopharyngeal area Symptoms may start as similar to the common cold Starts as an irritating cough which gradually develops into outbursts of coughing (paroxysms) Spasms frequently followed by vomiting Patients often feel like they are choking Low grade fever and general fatigue Timeline of Illness Incubation of 7-10 days Spasms can start to occur rapidly, or can take up to 3 weeks to appear Cough can then last for several weeks In older patients (>15 years) the symptoms are more mild, possibly due to residual immunity Complications Secondary respiratory infections Lung collapse Convulsions – half of those who develop convulsions die For those who survive convulsions, paralysis, mental retardation and epilepsy are common Hernias, urinary tract problems, fractured ribs can be caused by the severity of the coughing The parents of a sick child will find they suffer severe sleep deprivation Transmission Inhalation of droplets from infected patients The bacteria do not survive long in the environment They are rarely isolated from the nasopharynx of healthy subjects They may be intracellular in carriers but this has not yet been proven No animal reservoirs have been identified Highly contagious in non-immune populations with an attack rate of ~90% in close contact groups such as a family Treatment and Prevention Vaccine preventable – part of UK routine vaccine schedule Antibiotic therapy may reduce the duration of the disease, but recovery is still quite slow Erythromycin is the drug of choice, with chloramphenicol sometimes used Unvaccinated close contacts of patients will be offered erythromycin prophylaxis Some resistance to erythromycin has been seen In moderate to severe cases hospitalisation may be required to protect the airway and monitor seizures Vaccination and Infection in the UK 70000 100 90 60000 Data from HPA – no longer accessible 80 Notification Vaccine Coverage 70 60 cases 40000 50 30000 40 vaccine coverage (%) 50000 30 20000 20 10000 10 0 0 2008 2007 2006 2005 2004 2003 2002 2001 2000 1999 1998 1997 1996 1995 1994 1993 1992 1991 1990 1989 1988 1987 1986 1985 1984 1983 1982 1981 1980 1979 1978 1977 1976 1975 1974 1973 1972 1971 1970 Prior to vaccination ~10,000 children died of pertussis in the UK each year Vaccination introduced in the late 1950s Vaccine uptake levels in the early 1970s reached about 80% Press coverage of side effects caused a dip in uptake to as low as 30% The resultant epidemic in 1982 meant >100,000 children developed whooping cough and 36 children died, and permanent brain damage occurred in a significant number of survivors Current vaccine coverage is around 94% and disease incidence is low However, in 2011 numbers started rising again – then in late 2012 maternal vaccination was introduced to protect newborn children – reasons for this are not yet clear – but the data may also be “skewed” https://www.gov.uk/government/collections/pertussis-guidance-data-and-analysis https://www.gov.uk/government/publications/whooping-cough-pertussis-statistics Respiratory Diphtheria Signs and Symptoms Sore throat Low grade fever Membrane formed across tonsils Swollen neck glands Incubation period of 5-9 days Symptoms are toxin mediated, and the toxin can go systemic causing complication in the circulatory system and the CNS Non toxigenic strains can cause a localised pharyngitis Epidemiology - basics Pre the introduction of mass immunisation 5-10% of cases of respiratory diphtheria died In the US there was 100-200 cases per 100,000 population in the 1920s (thus around 5 per 100,000 population died of diphtheria per year – at the time the population of the US was ~100,000,000 therefore ~ 5000 people per year died in the US of the disease In the post-vaccination era infections and subsequent deaths are rare Currently the infection level is just 0.001 per 100,000 and deaths are now very rare This picture is mirrored in the UK The disease is endemic in many countries where vaccination is not in place, and outbreaks have been reported in several of the former Soviet states- in these outbreaks, adults have been the predominantly affected group Image from the CDC PHIL Influenza (the proper “flu”) Enveloped, Single-stranded RNA virus First identified in 1933, but existed long before Three types A, B, & C B & C appear restricted to man – but C is less common A found in wide range of species including pigs and poultry as well as man Type A appears to be responsible for more severe disease Generally considered an infection of the bronchi That is to say influenza is effectively a form of bronchitis – i.e. it causes inflammation of the bronchi in the same way chemicals and other noxious agents can Influenza basics Transmission by aerosols Incubation ~2 days Contagious during first 3-5days of illness Symptoms – fever, myalgia, headache, dry cough, sore throat, hoarseness Recovery ~7-10 days for most Complications – most frequent secondary bacterial pneumonia, rarely viral pneumonia, myocarditis, encephalitis No specific treatment Vaccination for high risk groups including the elderly, health care workers, those with underlying respiratory conditions… With the recent interest in influenza the PHE have been trying to raise awareness that there are different “types” of “flu” Avian The main reservoir is wildfowl that are resistant to the disease Avian flu viruses do not usually affect animals other than poultry and pigs However some transfer events occur Seasonal Incidence highest in winter, peaking December to March Strains vary from year to year Pandemic Can be caused by any strain that has not been seen in the human population for some time We are effectively due a large pandemic Pandemic Influenza New strains evade the herd immunity that exists to previously encountered strains 1918 /19 –( Spanish) estimated 40-50 million deaths worldwide 1957 – Influenza A/H1N1 (Asian) 1968 – Influenza A/H3N2 (Hong Kong) Pandemics occur at long, unpredictable intervals (decades), when a strain emerges to which the population have little or no immunity Is not seasonal in nature – pandemics will run “all year round” – for example the 1918/19 pandemic took just 2 or 3 months to circumnavigate the world but then stayed around for two years Eventually the virus runs out of susceptible hosts and the epidemic fizzles out Predicting Pandemics Experts generally agree a pandemic is inevitable, and may be imminent – maybe we have had some minor pandemics 16000 confirmed H1N1 deaths in 2009 affecting over 200 countries Consensus is that the prompt action of the Hong Kong authorities probably prevented a pandemic in 1997 The prediction is scary! For industrialised countries they predict 57-132 million GP visits 1.0 – 2.3 million hospitalisations 280,000-650,000 deaths All in a two year time frame A network of 112 centres monitor flu isolates to identify unusual strains that can then be examined further The WHO has a Pandemic Preparedness Plan in place http://www.who.int/influenza/preparedness/pandemic/en/ Diagnosis Generally based on GP diagnosis Virus isolation / virus demonstration from nasopharyngeal secretions during acute phase Demonstration of viral antigen in secretions Antibody rise using paired sera ( 1st sample taken between days 13 of illness, 2nd taken around day 12 of illness) by haemagglutination inhibition or complement fixation test Molecular methods evolving rapidly – in particular in response to the recent epidemic/pandemic strains emerging A range of respiratory illnesses have the same symptoms, only laboratory testing can confirm the aetiological agent Treatment & Therapy In the UK NICE argue that immunisation against predicted strains is the best form of defence – traditionally focused on the elderly and those with underlying lung problems, but recently started rolling out a childhood vaccine (nasal spray) http://www.nhs.uk/conditions/vaccinations/pages/child-flu-vaccine.aspx Vaccines generally based on the H & N surface structures which mutate, however hopes of an M protein based vaccine which will give longer lasting protection raised recently In general they advise against the use of antivirals in otherwise healthy people (also that amantadine should not be used at all). However when the incidence of flu-like illness reaches a certain level then zanamivir and oseltamivir should be used in those considered high risk for the development of complications – PROVIDED THAT TREATMENT IS STARTED WITHIN 48 HOURS OF ONSET OF SYMPTOMS Zanamivir should not be used in children Under certain circumstances NICE approve the use of antivirals as prophylaxis post exposure in high risk people Resistance is becoming an issue Reference: NICE (2009) - https://www.nice.org.uk/guidance/ta168 Pneumonias and other selected Lower Tract Infections Pneumonia – a leading cause of death “Pneumonia is called the old man's friend because, left untreated, the sufferer often lapses into a state of reduced consciousness, slipping peacefully away in their sleep, giving a dignified end to a period of often considerable suffering.” Dr John Pillinger http://www.netdoctor.co.uk/ate/cancer/202478.html Intro to pneumonia Pneumonia is a major cause of morbidity and mortality worldwide It is 6th in the list of causes of death in the USA It is also economically costly in terms of antibiotics, time off work, hospitalisation In half the cases the cause is not identified In those where a cause is identified, S. pneumoniae is the most common cause The reservoir is usually humans (oneself or a contact) and spread is through respiratory droplets Pneumonia intro continued Community acquired Main causes: Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis, Mycoplasma pneumoniae, Chlamydia pneumoniae Noscomial Main causes: Enterobacteriaceae, Staphylococcus aureus, Anaerobes, Pseudomonas aeruginosa Many patients have an underlying condition, e.g. bronchitis, asthma, a viral infection, tumours Characterised by the alveolar sacs filling up with pus, giving rise to a purulent sputum Results in chest tightness or pain, difficulty in breathing, fever, reduced blood oxygen, coughing to clear mucus, chest will sound “dull” when tapped Pneumonia Pathogenesis Causative agents can enter the lungs through 5 possible routes Inhalation (most common?), aspiration, spread across mucous membrane (some viruses), haematogenous spread (occasionally, e.g. IV drug users with S. aureus septicaemia) and penetrating injury (rare) Immune response is triggered in the lung and there are local defence factors in the respiratory secretions Cilia if functioning will move material up the respiratory tract, but if damaged this physical defence is impaired The lungs also have a resident macrophage population (alveolar macrophages) but they are of limited use against several respiratory pathogens that possess a capsule some organisms can even replicate in these cells Pathogenesis cont. Damage to the lung is caused by the microbes and the immune response Enzymes released by the bacteria Factors released by immune cells that cause local irritation and cell apoptosis Systemic manifestations follow Oxygen deprivation – thickening of the membranes reduces transfer Systemic shock – especially with Gram-negative bacilli such as Haemophilus influenzae Pneumonia classification and risks Pneumonia is subdivided in a number of ways that are relevant to patient management even before a pathogen is identified Acute v Chronic Community Acquired v Nosocomial Typical v Atypical Patient risk factors can also help suggest possible causative agents whilst waiting for laboratory confirmation Animal or environmental exposure (Chlamydia psittiaci, Yersinia pestis, Bacillus anthracis, Legionella pneumophila) Some pastimes expose you to specific risks – for example some of the unusual fungal agents are associated with pastimes that disturb soil and expose you to animal droppings Immunocompromised state - much higher risk of Mycobacteria and fungi Diagnosis & Treatment Diagnosis X-ray showing infiltrates Elevated temperature Changes in WBC counts Culture confirmation Treatment May require supportive therapy even to ITU level Tailored antimicrobials if possible – limited options for viruses Atypical pneumonia Patients present with less obvious symptoms – Dryish, non-productive cough, slightly raised temperature, drowsiness, nasal discharge – i.e. almost “flu-like” symptoms Causative organisms include Legionella pneumophila, Mycoplamsa pneumoniae, Chlamydiae pneumoniae, Coxiella burnetti and various viruses Legionellosis – atypical pneumonia Legionellosis is the collective term for diseases caused by members of the family such as Legionnaires’ disease and Pontiac fever 48 species and >60 serogroups in the Legionellaceae family, although infections in man usually caused by L. pneumophila First reported outbreak in 1976 – identified as an outbreak of pneumonia at a conference in Philadelphia (The American Legion Convention). 221 cases 34 deaths Transmission by inhalation of aerosols The pneumonia ranges from mild to life-threatening Incubation 2-10 days Abrupt onset with rapid development of symptoms including fever, muscle aches, headache and dry cough. Diarrhoea may also be observed. Pontiac fever is a milder form that resembles flu – diagnosis is serological or by antigen as the microbe is not recovered from respiratory samples in these cases UK Epidemiology of Legionellosis 600 Total Cases Male Cases Female Cases 500 Deaths Travel Associated 400 300 200 100 0 2006 2005 2004 2003 2002 2001 2000 1999 1998 1997 1996 1995 1994 1993 1992 1991 1990 1989 1988 1987 1986 1985 1984 1983 1982 1981 1980 Data from HPA – no longer accessible Image from the CDC PHIL SARS and MERS Sudden Acute Respiratory Syndrome Viral infection – Coronavirus Recognised cause of acute URTI, first identified in humans in late 1960’s through work at the common cold unit in Salisbury – but really emerged in 2002-3 Stable in the environment for 36 hours on paper, formica, plaster 72 hours on plastic and steel 96 hours on glass In Canada, evidence of environmental contamination was found including walls and the ventilation system MERS: a newer Coronavirus http://www.nhs.uk/news/2012/09september/pages/new-sars-like-virus- detected.aspx http://www.nhs.uk/news/2014/07July/Pages/Deadly-MERS-camel-flu-maynow-be-airborne.aspx SARS continued Incubation period ~4-6 days but up to 14 days reported Transmission from an infected patient appears greatest from the most severely ill and those undergoing dramatic deterioration The virus is shed in faeces (peaking at day 12-14) as well as nasal secretions (peaking at day 9-11) The case fatality ratio on average was 15%, however it varied greatly with age group – most fatalities were in the elderly, diabetes also appears a possible factor for increased mortality There is limited evidence that the disease killed proportionally more men then women, but numbers are too small for certainty A number of domestic pets were found to carry the virus Focal points for transmission included a hotel and an aeroplane A modern day pandemic Mid-Nov 2002 – first cases in Guangdong Province, China 28th Feb 2003 – first case in Vietnam by 11th of March ~30 cases in the cluster 12th March 2003 –WHO issue global alert 14th March 2003 – Canadian cluster reported 15th March 2003 – Case in Singapore 15th March 2003 –WHO issue global travel alert due to spread 17th April 2003 – the identity of the virus confirmed April and May –WHO restates the travel advisory notices 4th May 2003 – preliminary research on stability in the environment 15th June 2003 – last confirmed case in China 5th July 2003 –WHO issue statement that the first global epidemic of SARS had been contained 8th Sept 2003 – isolated case in a researcher – no spread from index observed >4000 cases and 813 deaths 21% of cases were amongst health care workers May 2004 WHO declare end of emergency with chain of transmission from last cases now broken SARS main centres of the pandemic 6000 5000 4000 Total 3000 Number of deaths 2000 Number of HCW affected 1000 0 Canada China Hong Kong Taiwan Data from WHO website Singapore Other “affected” areas 70 Total Number of deaths 60 Number of HCW affected 50 40 30 20 10 0 Viet Nam United States United Kingdom Thailand Switzerland Sweden Spain South Africa Russian Fed Romania Korea Eire Philippines New Zealand Mongolia Malaysia Kuwait Italy Indonesia India Germany France Macao Australia Data from WHO website Aspiration pneumonia Occurs when the stomach contents, saliva, oral debris etc get into the lungs Can cause chemical pneumonitis Can deliver “unusual” pathogens into the respiratory tract e.g. anaerobes Can occur with some neurological conditions, in those with swallowing problems, during anaesthesia (hence nil by mouth preop) or when drunk!! Tuberculosis The Genus – Mycobacterium The genus Mycobacterium are Aerobic bacilli 0.2 – 0.6μm wide x 1 - 10 μm long Non-motile They have a lipid rich cell wall, That differs from “standard” bacterial cell walls That increases their resistance to disinfectants That makes them nutritionally fastidious (fussy) That means they grow and divide slowly (12-24hours) Mycobacteria and disease There are at least 70 species in the genus They have animal and/or environmental reservoirs A number of have been associated with human disease including However, 95% of mycobacterial infections are caused by M. tuberculosis, M. avium-intracellulare, M. kansasii, M. fortuitum, M. chelonae, and M. leprae. Of these all but M. leprae cause respiratory infections They are a major cause of morbidity and mortality in the developing world, and also in immunocompromised patients in the developed TB has a long history Reports of disease that are almost certainly TB can be seen in historic texts (particularly those of Greek scholars) dating back centuries As recently as the 1800s TB was endemic in the UK (and Europe and the US) The annual death toll at this time was approaching 1% of the population of major cities As living standards improved, the incidence of TB declined without any specific action against it Vaccination was introduced in the UK in the 1950s and this resulted in a further substantial decline in infection Illustrious victims include – Orwell, Austen, Moliere, Keats and of course Satine in Moulin Rouge! Pathogenesis aspects Spread is via the respiratory route – it is estimated that each person with active TB will infect 10-15 others TB can evade the immune response by “hiding” inside pulmonary macrophages T cells and macrophages combine to try and prevent spread of infection by “walling off ” the bacteria – this lesion (called a tubercule) becomes hardened Much of the damage in the lung is caused by the phagocytes trying to kill the bacteria and releasing enzymes etc in to the environment The walled off lesions contain live bacteria, which grow and multiply. The bacteria alter the nature of the lesion over time, from caseous to liquefied. Once the lesion is liquefied both aerosol transmission (spread) and dissemination through the host become more likely Signs, symptoms and diagnosis Signs and symptoms Coughing – often producing bloodstained sputum Fever Image from CDC PHIL resource Weight loss Loss of energy (malaise) Night sweats Swollen glands in the neck Diagnosis Shadow infiltrate on lung x-ray Possible positive tuberculin test (care in interpretation needed) Laboratory culture or molecular detection Treatment There are a number of antibiotics that are either Specifically active against mycobacteria or On a restricted use list to preserve their effect Acute TB treatment in UK is usually based around Rifampicin and Isoniazid (for 6 months) with Ethambutol and Pyrazinamide (for the first 2 months). Streptomycin can also be used Latent TB may be left untreated in over 35s as the risk of the medications causing liver damage rises such that the risks of treatment may outweigh the benefits – patients will be monitored for reactivation and then treated at that point. Resistance occurs at a relatively high frequency, so even in a patient with no evidence of resistance or history of previous treatment it is usual to prescribe a dual or triple therapy approach Treatment takes around 6 months, and is a relatively complex regime for the patient to follow. Non-compliance is therefore a major problem. Prevention - vaccination BCG is the currently used vaccine. This is an attenuated live vaccine strain of Mycobacterium bovis (a close relative of M. tuberculosis) Billions of doses has been given worldwide and very few ill-effects have been reported (making it one of the safest vaccines known) However, its effectiveness is controversial. The vaccine prevents children form getting the disease but does not protect adults from reactivation of latent infections. Protection rates vary widely from trial to trial – possibly due to the genetic differences between trial populations Vaccination in the UK is now reserved for high risk individuals – e.g. children of migrants from endemic countries and those in high risk occupations Global picture Worldwide, TB kills approximately 2 million people each year The WHO state that the “epidemic is growing and becoming more dangerous” The breakdown of health services in a number of countries, the spread of AIDS and the emergence of multi-drug resistant strains are adding to the problem In 1993, the WHO declared TB a global emergency and they predict that between 2002 and 2020, approx 36 million people will die of TB, and a further 150 million will suffer infection WHO recently estimated that 2 billion people worldwide are infected with M. tuberculosis (~1/3rd of the population) In Eastern Europe and Africa, TB is on the rise after 40 years of decline The highest burden of TB currently is in Asia – with nearly ½ of all deaths happening there Trends in Europe Data from EuroTB.org (no longer accessible) Data from EuroTB.org – no longer accessible In the UK Predominately an imported condition – diagnosed within set period of arriving in the UK Major urban centres highest levels Age profile in first generation migrants is different to that seen in established populations Exacerbations of other lung pathologies Exacerbation of Bronchitis Bronchitis is production of excess sputum on most days for 3 consecutive months with more than one “bout” of illness Microbes can both cause bronchitis and exacerbate bronchitis caused by other conditions Many possible causes, microbial causes tend to be acute, whilst environmental causes are more likely to cause chronic illness Much more common in smokers Bacterial causes include all the possible causes of “simple” pneumonia, and viral causes as we have seen include influenza viruses – these can all also exacerbate. Treatment against cause, plus sufferer will be recommended to have the flu and pneumococcus jabs Exacerbation of bronchiectasis Bronchiectasis is chronic inflammation or degenerative condition of the bronchi, in which the bronchi and/or the bronchioles become distended and lack elasticity – including post-TB scarring Leads to excess production of secretions that must be cleared, through physio or postural drainage Sufferers prone to bacterial infection which also must be cleared as and when it arises – can be caused by many organisms we have talked about already Exacerbation of COPD (link to DL’s lectures) Chronic bronchitis and emphysema combined Infectious exacerbations are common and can be either mono- agent or multi-agent – about ¼ of infectious exacerbation will have both a bacterium and a virus present Any of the agents of bronchitis or pneumonia can be implicated Patients with COPD should receive the pneumococcal vaccine and the seasonal flu jab Exacerbation of Cystic Fibrosis (CF) CF is a genetic disease where a chloride channel protein is mutated – leads to altered secretions at a range of body sites including the lung Major pathogens of concern Staphylococcus aureus, Haemophilus influenzae, Pseudomonas aeruginosa, Burkholderia cepecia Other respiratory pathogens also need to be watched out for, although their role is less well defined Exacerbations of Asthma Viral infections in childhood can increase the risk of developing asthma Viruses and bacteria can also cause acute exacerbations of asthma Many asthmatics are also at increased risk of getting pneumonia and other infectious diseases Moderate – severe asthmatics should consider the flu jab and also possibly the pneumococcal jab Conclusion Wide range of possible infections are associated with the respiratory tract Wide range of infections can cause each of the different types of infection Patients with underlying lung pathology are at increased risk of infections and any infections are likely to cause an exacerbation of their underlying disease Recommended Additional Reading These URLs should take you to free access versions of these papers that show how any agent that causes infection of the middle and lower respiratory tracts can exacerbate pre-existing respiratory conditions Infectious Etiology of Acute Exacerbations of Chronic bronchitis – by Sethi http://journal.publications.chestnet.org/data/Journals/CHEST/21947/380S.pdf Exacerbations: etiology and pathophysiologic mechanisms – by Wedzicha http://journal.publications.chestnet.org/data/Journals/CHEST/21978/136S.pdf Bacterial infection in COPD in 2000: a state of the art review – Sethi & Murphy http://www.ncbi.nlm.nih.gov/pmc/articles/PMC88978/?tool=pubmed