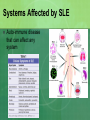
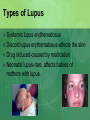
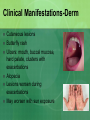
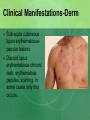
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Nursing Care of the Adult with Rheumatic Disorders
Osteochondritis dissecans wikipedia , lookup
Inflammation wikipedia , lookup
Ulcerative colitis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Anti-nuclear antibody wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Periodontal disease wikipedia , lookup
Molecular mimicry wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Kawasaki disease wikipedia , lookup
Inflammatory bowel disease wikipedia , lookup
Behçet's disease wikipedia , lookup
Germ theory of disease wikipedia , lookup
Management of multiple sclerosis wikipedia , lookup
Globalization and disease wikipedia , lookup
Neuromyelitis optica wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Multiple sclerosis signs and symptoms wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Rheumatic fever wikipedia , lookup
Autoimmunity wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Ankylosing spondylitis wikipedia , lookup
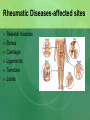
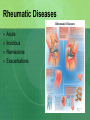
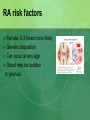
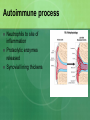
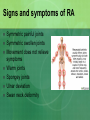
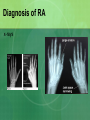
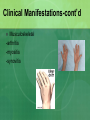
Joint Disorders - Autoimmune Zelne Zamora, DNP, R.N. Rheumatic Diseases- Inflammatory Process Series of steps causing: -swelling, pain and stiffness -warmth, effusion, decreased ROM, increasing pain -increasing severity -joint instability, contractures, systemic complications (vessels, lungs, heart, kidneys) Rheumatic Diseases-Inflammatory Process Immune system response to antigens or damaged cells T and B cells react to the antigen response Rheumatic Diseases- Autoimmune Process Body reacts against own tissue Treats as a foreign body Can affect all systems HLA genes (human leukocyte antigen)-linked to immune response Rheumatic Diseases-Degenerative Process Poorly understood Genetics? Hormones? Prior joint damage? Mechanical? Inflammation is a secondary process Degradation of joint Rheumatic Diseases-affected sites Skeletal muscles Bones Cartilage Ligaments Tendons Joints Rheumatic Diseases Limitations in mobility Pain Fatigue Altered self image Sleep disturbance Organ failure Death Rheumatic Diseases Minor vs. life threatening Primary vs. Secondary Monoarticular vs. Polyarticular Inflammatory vs. Non-inflammatory Rheumatic Diseases-Clinical Manifestations Skin Hair Eyes Ears Mouth Chest Cardiovascular Rheumatic Diseases-Clinical Manifestations Abdomen Genitalia Neurologic Musculoskeletal Surrounding tissue Rheumatic Diseases Acute Insidious Remissions Exacerbations Rheumatic Diseases Diarthroidial /Synovial joints Rheumatic disease - Arthritis Ankylosing spondylitis Rheumatoid arthritis Osteoarthritis Bursitis Carpel tunnel Fibromyalgia Gout Crohns’s disease Juvenile arthritis Lupus Lyme disease Marfan’s syndrome Paget’s disease Raynauds’s disease Scleroderma Myositis Common Lab Studies-Rheumatic Diseases Creatinine-increase may indicate renal disease (dz) in SLE, scleroderma ESR-increase in inflammatory dz Hct-decreased in anemia of chronic dz RBC-decreased in RA, SLE WBC-decreased in SLE VDRL-false positive in SLE Labs (cont’d) ANA-positive in SLE, RA\ CRP-positive indicative of inflammation: RA and SLE RF- positive in 80% of those with RA. Positive in SLE Complement levelsC3 and C4-decreased in RA and SLE Management goals for Rheumatic Diseases Decrease inflammation Control pain Maintain or increase mobility Maintain or increase function Increase client knowledge Promote self-management Rheumatologic DiseasesGerontology Considerations Disability Cognitive changes Co-morbid conditions M/S conditions most common Rheumatoid Arthritis Chronic, systemic, inflammatory disease that’s mediated by the immune system Autoimmune disease Affects 1% Diffuse connective tissue disease Rheumatoid Arthritis: Pathophysiology Originates in synovial tissue Breaks down collagen Edema Proliferation of synovial membrane Pannus formation Cartilage destruction Bone erosion Cartilage Connective tissue RA risk factors Female: 2-3 times more likely Genetic disposition Can occur at any age Onset may be sudden or gradual Proposed causes of RA Bacteria? Virus? Heredity? Error in antigen formation? Environmental factors? Diet? All of the above? Unknown cause Rheumatoid Arthritis: Systems Affected Arterial walls Endothelium Nervous system HDL production Autoimmune process Immune response to antigen Formation of IgG Rheumatoid factor; autoantibodies against IgG RF combines with IgG Autoimmune process Deposit on synovial membranes Activation of complement Inflammatory response Autoimmune process Neutrophils to site of inflammation Proteolytic enzymes released Synovial lining thickens Signs and symptoms of RA Symmetric painful joints Symmetric swollen joints Movement does not relieve symptoms Warm joints Spongey joints Ulnar deviation Swan neck deformity Signs and symptoms of RA Stiffness lasting > 1 hour in the a.m. Fatigue, malaise, fever Loss of ROM Weight loss Anemia Lymphadenopathy Typically starts in small joints Advances to larger joints Signs and Symptoms: RA Disfigured joints-late Rheumatoid nodules Onset acute Co-morbidities: RA Arteritis Neuropathy Pericarditis Splenomegaly Sjogrens Diagnosis of RA H&P Rheumatoid factor (positive) CBC (anemia) ESR -elevated C4 complement –decreased Anti CCP- positive antibodies. 95% diagnostic CRP- elevated Diagnosis of RA x-rays Diagnosis of RA ANA- positive Synovial fluid- cloudy, yellow, +leukocytes, +complement Treatment goals/RA Early intervention Control inflammatory disease Prevent joint damage Relieve pain Find optimal drug regimen Improve function Achieve remission DMARD’s-disease modifying antirheumatic drugs – First line Cyclophosphamide (Cytoxan) Methotrexate (Rheumatrex)** Sulfasalazine (Azulfidine) Hydroxyxholoroquine (Plaquenil) Azathioprine (Imuran) Cyclosporine (Prograf) These are the gold standard of care: early use!! NSAIDs – now adjunctive therapy only COX-1 vs COX-2 COX-1 GI irritation is common; risk for ulcer COX-2 reduce swelling, no GI upset; decreased risk of bleeding; increased risk of CV disease NSAIDs used to control swelling and inflammation NSAIDs – now adjunctive therapy only NSAID’s: Ibuprofen, Naproxen COX-2 inhibitors: Celebrex Gold salts (Less used DMARD’s) Auranofin (oral gold)/Ridaura Gold sodium thiomalate (inj)/Myochrysine) Biologic response modifiers Inhibits production of cytokines Etanercept (Enbrel): given SQ Inflisimab (Remicade): IV Dyridimine(Arava) Opioids: long acting OxyContin Fentanyl patch Corticosteroids Prednisone: po, IM, joint injections Short duration Lowest dose possible CAM/Alternative Copper bracelets Devil’s claw Gin-soaked raisins Colonics Coffee enemas Shark cartilage Snake venom Prosorba therapy Severe RA-not responsive to DMARD’s Device used during apheresis therapy to bind IgG Surgery Arthroscopic Joint fusion Joint replacement Tendon reconstruction Nursing care considerations Promote comfort Facilitate independence and self care Reduce fatigue Promote mobility Injury prevention Patient education Dietary considerations Assess for depression Systemic Lupus Erythematosus (SLE) Lupus is a chronic, autoimmune disease Immune system becomes hyper active and attacks normal tissue Increased production of autoantibodies Results in inflammation and brings about symptoms Systemic Lupus Erythematosus Combination of genetic, hormonal, environmental and immunologic interactions (B cells and T cells) Medications: Apresoline, Pronestyl, INH, Thorazine Onset insidious or acute Systems Affected by SLE Auto-immune disease that can affect any system Who gets Lupus? Can occur at any age Nine out of ten people with lupus are women In women ages 15-44, lupus strikes women 10-15 times more frequently than men Who gets Lupus? African American women have a 3 times higher incidence and mortality A.A. tend to develop disease at a younger age and to develop increased severity of complications Also more common in women of Hispanic, Asian and Native American decent Types of Lupus Systemic lupus erythematosus Discoid lupus erythematosus-affects the skin Drug induced-caused by medication Neonatal lupus-rare, affects babies of mothers with lupus. Diagnosis of Lupus can be Difficult Thorough H&P Same blood tests as RA: -increased Cr -RF/positive -increased ESR -IgA, IgM, IgG-elevated -anemia -no one test confirms!! -leukopenia -results only support Dx -ANA positive -CXR/ -anti-DNA-titers elevated -echo -compliment C3/C4-decreased Classic Signs and Symptoms of SLE Fever Weight loss Arthritis Fatigue Pleurisy Pericarditis Clinical Manifestations-Derm Cutaneous lesions Butterfly rash Ulcers: mouth, buccal mucosa, hard palate, clusters with exacerbations Alopecia Lesions worsen during exacerbations May worsen with sun exposure Clinical Manifestations-Derm Sub acute cutaneous lupus erythematosuspapular lesions Discoid lupus erythematosus-chronic rash, erythematous papules, scarring, in some cases only this occurs. Clinical Manifestations-M/S Musculoskeletal -polyarthralgia with morning stiffness/acute or slow onset -joint swelling/tenderness/pain -swan neck deformity -ulnar deviation -prolonged, extreme fatigue Clinical Manifestations-cont’d Musculoskeletal -arthritis -myositis -synovitis Clinical Manifestations: C/P Cardiopulmonary -tachypnea -pleurisy -dysrhythmias -accelerated ASHD in women with SLE -pericarditis-MOST COMMON cardiac problem!! Clinical Manifestations/Renal Renal -hematuria -proteinuria -glomerulonephritis -early detection important to prevent kidney damage and HTN Clinical Manifestations/Hematology Hematological -anemia -leukopenia -antibodies against blood cells -thrombocytopenia -coagulopathy/clots -lymphadenopathy -spleenomegaly Clinical Manifestations/GI Gastrointestinal -abdominal pain -diarrhea -dysphagia -nausea/vomiting -reproductive -menstrual abnormalities Clinical Manifestations/CNS CNS -widespread!! -photosensitivity -seizures -peripheral neuropathy -cognitive dysfunction -subtle changes in behavior Clinical Manifestations/Misc Miscellaneous -Raynaud’s syndrome -persistent high fever >100 degrees F -alopecia Warning Signs of SLE Flare Increased fatigue New or higher fever Increased pain Development or worsening of a rash Upset stomach Headache or dizziness Development of s/s client has not had before SLE Flare Triggers Overwork Emotional crisis Exposure to sunlight Infection Injuries or surgery SLE Flare Triggers Pregnancy/post partum Sudden withdrawal of medications Sensitivities or allergies Certain prescription drugs-sulfa OTC medications-herbs Immunizations-live vaccines Treatment Goals/SLE Prevent flares Treat flares when they occur Minimize complications/loss of organ function Minimize disabilities/improve functional status Prevent complications from therapy/treatment Promote self management Manage psychological implications Treatment Goals of SLE Management of acute and chronic disease Acute-controlling flares in disease to prevent organ damage Chronic-periodic monitoring with recognition of subtle changes in condition Treatment/SLE Treatment always dependent on severity Treatment/SLE Corticosteroids: most important, beware of side effects, topical for derm, low dose oral for minor disease, high dose po, IM or IV for severe Treatment SLE NSAID’S-used with steroids to allow for lower dosage of steroid Treatment SLE Anti-malarials: Plaquenil. Used for mild symptoms and/or systemic involvement. Treatment SLE Immunosuppressant Drugs: Imuran, Cytoxan, Methotrexate. Reserved for severe SLE. Suppress autoimmune response. Treatment SLE B cell Depleting Therapies: Newer treatment option. Severe SLE. Rituxan. CAM/Alternative Treatment SLE Acupuncture Biofeedback/ meditation Massage Herbs/Supplements -flax seed, fish oil, DHEA, calcium, Vit. D Nursing Management/SLE Patient education disease process Regular health screenings Self management Maintain skin integrity Body image disturbance Medications Diet: high in antioxidants, avoid refined foods, red meat, coffee