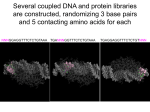
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download CD4 T-Cell Th1 Response
Survey
Document related concepts
Neonatal infection wikipedia , lookup
DNA vaccination wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Infection control wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Adaptive immune system wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Transcript
Chronic Yeast Infection: Why and What to do about it Paul Summers, M.D. Department of Obstetrics and Gynecology University of Utah School of Medicine Severe Yeast Satellite lesions Summers PR. Topical therapy for mucosal yeast infections in: Topical Applications and the Mucosa (Current Problems in Dermatology volume 40), Surber C, Elsner P, Farage MA eds. Karger New York 2011 World War II 50 to 80 million deaths world wide USA cost $4 trillion (current value) World War II Advances in Technology Jet engine Guided rockets Nuclear Radar Synthetic rubber Sonar (ultrasound) * Colposcope * History of Colposcopy Developed by Dr. Hans Hinselmann in Hamburg Germany (first described in1925) Dr. Helmut Wirts was Hinselman’s partner in Hamburg Dr Eduard Wirts (Helmut’s brother) was the chief doctor for the notorious Jewish “medical block 10” of Auschwitz Concentration camp In 1943 Eduard published his unethical colposcopy prisoner experimentation, “Carcinom: die Geissel der Frauen der Welt is Heilbar” HIV Thrush Currently 2.6 million children, 37 million total living with HIV worldwide 1.7 million deaths in 2013 30 years of Advances in HIV Research Dynamics of an Epidemic Antiretrovirals Better understanding of the Immune System *Better * understanding of the pathophysiology of infection Vaginal Immune Defenses Skin Barrier Cell mediated immunity Innate immunity Key Immune Elements *Langerhans cells *CD4 T-helper cells Macrophages vaginal and oral mucosa are similar vaginal innate response Is stronger Cytokines *Innate elements mannose binding lectin (MBL) human beta defensin 2 and 3 (HBD 2 or 3) secretory leukocyte protease inhibitor (SLPI) 40 others Vulvovaginal Skin Physiology human beta defensins (HBD-2, 3) Stratum Corneum or human cathelicidin (LL-37) Surface glycoproteins (mucus) superficial Mannose binding lectin intermediate parabasal basal lipids and free fatty acids fill the intercellular space Langerhans cells Skin is the Body’s Primary Immune Organ! The immune system of the skin: Langerhans cells (2-5% of cells in the skin) recognize and process antigens The highest concentration of Langerhans cells is in the cervical transformation zone (Pudney. Biol Reprod. 2005;73:1253) The most likely site of entry of HIV is the transformation zone Langerhans Cells Bone marrow-derived cells residing in the skin Consume foreign antigens that appear in the skin Activate an important defense against bacteria, viruses, yeast, and cancer cells Microbes are killed and processed for antigens that are transported to the immune system Cancer cells that randomly appear in the skin have abnormal surface proteins and are recognized by the Langerhans cells CD4 T-Cell Th1 Response T-helper cell type 1 response (Th1) eliminates infection and individual malignant cells Auto-immune skin disease is an excessive Th1 response Rejection of a transplanted organ is a Th1 response CD4 T-Cell Th2 Response Mediates allergy Does not effectively eliminate bacteria, yeast, viruses or cancer cells in the skin A Th2 response down-regulates the ability to have a good Th1 response A persisting Th2 response increases the risk for viral and yeast infection, as well as skin cancer * Infection is worse if there is no good Th1 Response Diagram: Abbas and Lichtman. Basic Immunology 2nd Edition Saunders 2006:116 Good Bad (vulvovaginal allergy or estrogen) Skin Microbicides The intermediate layer of the skin produces over 800 chemicals important for growth, healing, etc. Human beta defensins and cathelecidin are the most important but over 40 have been identified (Ichiro J Immunol 2003;171:3262) The MIC 90 of HBD3 against Saccharomyces cerevisiae is 13.2 micrograms / ml (Jose-Ramon. Cell and Tissue Research. Online publication, Springer-Verlag 11 Sept 2001) Mannose Binding Lectin The lectin Pathway Mannose binding lectin is produced by vaginal epithelial cells and the liver MBL binds microbes that have Mannose on their surface This activates microbe killing by the lectin complement pathway Bulla R, et al. Mannose-binding lectin is produced by vaginal epithelial cells and its level in the vaginal fluid is influenced by progesterone. Mol Immunol 2010:48(1-3);281-6 Vaginal Immune Deficiency Loss of skin barrier (flaking skin) Inhibition or loss of Th1 response Decrease in HBD3 in allergy Deactivation or congenital deficiency in MBL Who is at high risk for yeast infection? AIDS Eczema Pregnancy SGLT2 inhibitors (Invokana, etc) Diabetes Antibiotics (topical) estrogen HIV Basic Immunology of AIDS Compromised genital skin barrier Langerhans cells phagocytize HIV Langerhans cells activate and infect T-helper cells (CD4 cells) HIV destroys CD4 population of T-helper cells Resulting opportunistic infections and malignancies Kawamura et al. The role of Langerhans cells in the sexual transmission of HIV. J Dematol Sci 2005:40;147-55 Infection is worse if there is No CD4 Th1 Response Good X HIV Bad Herpetic Whitlow Herpetic Whitlow in AIDS with minimal Th1 response Severe herpes in AIDS with minimal Th1 response What to do for HIV with Recurrent Yeast Antiviral therapy to improve CD4 count Oral or topical antifungal Eczema Relative Sensitivity of Vulvar Skin Transepidermal water loss is higher on the vulva than elsewhere Elsner, Maibach. Acta Derm Venereol 1990;70:141-4 Vulvar friction coefficient is greater, making the vulva more susceptible to mechanical damage Elsner, Maibach. Dermatologica 1990;181:88-91 Hydration, occlusion, and tissue permeability heighten vulvar susceptibility to topical irritants Ferage. Arch Gynecol Obstet 2005;272:167-72 Universally high risk for irritant and allergic dermatitis Numerous Articles link Allergy to Yeast Moraes PS et al. Recurrent vaginal candidiasis and allergic rhinitis: a common association. Ann Allergy Asthma Immunol 1998:81;165-69 Neves NA et al. Association between atopy and recurrent vaginal candidiasis. Clin Exp Immunol 2005:142;167-71 White DJ et al. Zafirlukast for severe recurrent vulvovaginal candidiasis: an open label pilot study Sex Transm Infect 2004:80;219-22 Combination steroid / antifungal creams are commercially available but typically contain irritating propylene glycol Eczema and Yeast Infection Eczema favors staph, strep and yeast infection (impetigo and intertrigo) Obstetric and Gynecologic Dermatology Black M and McKay M, eds Mosby 2002:75, 201-203 Women with recurrent yeast generally have a vaginal baseline TH2 environment Witkin SS et al. Localized vaginal allergic response in women with recurrent vaginitis J Allergy Clin Immunol 1988:81;412-16 The Consequences of Allergic Dermatitis Deficient cathelicidin (LL-37) and beta defensin (hbd-2, 3) allows microbe colonization of the skin Nomura et al. Cytokine milieu of atopic dermatitis…prevents induction of innate immune response genes J Immunol 2003:171;3262-69 Flaking of the stratum corneum facilitates microbe entry into the skin Deficient cell-mediated Th-1 response allows microbe proliferation in the skin and increases cancer risk Skin flake probably due to interferon gamma compromises the skin barrier Vulvovaginal irritant and allergic response causes the skin to flake, as is seen frequently in the saline wet prep (spongiotic response) Contact dermatitis (spongiotic dermatitis) Hyperkeratosis and Spongiosis Severe Allergic Dermatitis Scratching here History of asthma, hay fever, eczema, sinusitis Deficient HBD2 and 3 Lichen Simplex Chronicus with Recurrent Yeast Infection Deficient HBD 2, 3 Therapy for Vulvar Atopic Dermatitis Avoid allergens (and irritants) Topical non irritating (compounded) corticosteroid ointment Moisturize daily with vaseline, Crisco, or coconut oil Antihistamine Consider the long-term risk of squamous cancer (Oral) yeast therapy for superimposed infection Lichen Sclerosus Complications of Lichen Sclerosus Poor skin barrier function (topical creams burn) Vulvar contact dermatitis (mixed vulvar dystrophy) Down-regulation of Th1, enhanced Th2 CD4 Tcell response Recurrent yeast infection and Squamous cancer Lichen Sclerosus Therapy Avoid irritants and allergens Not topical testosterone Treat any associated infection (oral fluconazole or topical clotrimazole) Apply non-irritating topical corticosteroid ointment Biopsy any suspicious areas (risk of cancer) Chronic Dermatitis leads to Nerve Proliferation Figure from Misery, Staender. Pruritus Springer 2010 p. 4 Nerve Proliferation in “Vulvar Vestibulitis” Bohm-Starke N, Hilliges M, Falconer C, Rylander E. Increased intraepithelial innervation in Women with vulvar vestibulitis syndrome. Gynecol Obstet Invest 1998;46:25660 Westrom LV, Willen R. Vestibular nerve fiber proliferation in vulvar vestibulitis syndrome. Obstet gynecol 1998;91:572-6 Bohm-Starke N, Hilliges M, Falconer C, Rylander E. Neurochemical characterization of the vestibular nerves in women with vulvar vestibulitis syndrome. Gynecol Obstet Invest 1999;48:270-5 Pregnancy Pregnancy and Eczema Eczema is more severe during menses and pregnancy Kemmett D, et al. The influence of the menstrual cycle and pregnancy on atopic dermatitis. Br J Dermatol 1991:125;59-61 Basic Immunology of Pregnancy Compromised genital skin barrier Estrogen down regulates Th1 response Any tendency for a Th2 response is enhanced Th2 response lowers human beta defensin 3 Yeast produce acid proteases that enhance the Th2 response Glucosuria deactivates mannose binding lectin What to do for Pregnancy and Recurrent Yeast Oral glucose challenge test Clotrimazole cream Possibly topical steroid Moisturize with vaseline, Crisco, coconut oil May prefer to avoid oral diflucan (fluconazole) Risk of Fluconazole in Pregnancy Increase in miscarriage (7 to 22 weeks gestation) Hazard ratio 1.48 Also increased rate of stillbirth but not statistically significant No increased risk with topical azoles * Moigaard-Nielsen et al. Association between use of oral fluconazole during pregnancy and risk of spontaneous abortion and stillbirth. JAMA 2016:315;58-67 SGLT2 inhibitors (prevent glucose reabsorption in the renal distal tubule for diabetic glucose control) Invokana, etc Mannose Binding Lectin Mannose binding lectin plays a crucial role in innate immunity against yeast by enhanced complement activation and enhanced uptake of polymorphonuclear cells. BMC Van Asbeck EC et al. Microbiol 2008:8;229 Why does Glucosuria cause yeast? The lectin Pathway Mannose binding lectin is produced by vaginal epithelial cells and the liver Progesterone enhances MBL production during the secretory phase of menses and pregnancy This can compensate for the downregulation of the CD4 T cell Th1 response Bulla R, et al. Mannose-binding lectin is produced by vaginal epithelial cells and its level in the vaginal fluid is influenced by progesterone. Mol Immunol 2010:48(1-3);281-6 Why does Glucosuria cause yeast? The lectin Pathway (Fucose is a plant sugar) MBL binds mannose, fucose, glucose, and all sugars with 3 or 4 hydroxyl groups in an “equatorial plane” Weiss WI et al. Structure of a c-type mannose binding protein complexed with an oligosaccharide. Nature 1992:360(6400);127-34 Mannose is found on the surface of Salmonella, Neisseria, yeast, and other mucosal pathogens Why does Glucosuria cause yeast? The lectin Pathway MBL binds pathogens that have mannose on the surface MBL activates pathogen killing by the lectin complement pathway Urine contacts the vulva and refluxes into the vagina A significant amount of glucosuria binds and deactivates MBL Do Yeast Thrive on Sugar? Ingredients in Sabourauds Agar 1% Tryptone (numerous peptides resulting from the digestion of casein by the protease trypsin) 4% Dextrose 1.5% Agar (inert galactose polymer) NO What to do for Glucosuria and Yeast Diflucan or clotrimazole once weekly Diflucan or clotrimazole with menses Avoid irritants Topical steroid or daily moisturizer if vulvar atopic changes Diabetes Immunology of Diabetes Active tuberculosis is 10X more common in juvenile and long duration diabetes Root HF The association of diabetes and pulmonary tuberculosis N Engl J Med 1943:210;127-47, 192-200 Administered insulin has an antiinflammatory action that shifts toward a Th2 response in insulin resistance Viardot A, Potential antiinflammatory role of insulin via the preferential polarization of effector T cells toward a T helper 2 phenotype Glucosuria neutralizes Mannose Binding Lectin Diabetic Recurrent Yeast treatment Maintain hemoglobin A1c less than 7 Moisturize with vaseline, Crisco, or coconut oil for any dermatitis May use oral fluconazole if not taking an oral hypoglycemic Antibiotics and Yeast Antibiotics and Yeast Vulvar dermatitis from mascerated genital skin Impetigo, intertrigo, infection under pannus Staph, Strep (GBS), yeast colonization Antibiotics eliminate staph and strep so yeast can move in Yeast replicate more slowly than bacteria What to do for Antibiotics and Yeast Use antifungal concurrently with antibiotic Treat any vulvar atopic tendency Estrogen Replacement Decreased Allergy after Menopause Asthma may become less severe after menopause Belzano. Asthma and sex hormones. Allergy 2001;56(1):13-20 Lower estrogen decreases risk for yeast infection after menopause Hormone replacement therapy after menopause may make asthma worse Kos-Kudla. Effects of hormone replacement therapy on endocrine and spirometric parameters in asthmatic postmenopausal women. Gynecol Endocrinol 2001;15(4):304-11 Yeast infection risk is restored Yeast Infection with Estrogen Replacement Adverse Event (Preferred Term) Vagifem® (n=91) Placebo (n=47) % % Headache 9 6 Abdominal Pain 7 4 Upper Respiratory Tract Infection 5 4 Moniliasis Genital 5 Statistically significant 2 Back Pain 7 source: Vagifem® [prescribing information]. Princeton, NJ: Novo Nordisk Inc.; 2006. 6 Resistant Yeast Candida albicans Resistant Non-albicans Yeast Blastospores, no hyphae May respond to butoconazole, terconazole, itraconazole (or oral combined with topical) Treatment for Resistant Yeast Topical 600 mg boric acid in a capsule BID Sobel JD et al. Treatment of vaginitis caused by Candida Glabrata: use of topical boric acid and flucytosine. Am J Obstet Gynecol 2003:189;1297-1300 Highly poisonous if boric acid is ingested orally Baker MD et al. Ingestion of boric acid by infants. Am J Emerg Med 1986:4;358-61 Flucytosine is expensive, impractical Horowitz BJ. Topical flucytosine therapy for chronic recurrent Candida Tropicalis infections J Reproduct Med 1986:31;821-24 Lactobacillus Probiotic Therapy Normal flora, lactobacilli Lactobacillus Therapy Lactobacillus therapy does not prevent post antibiotic yeast vaginitis (BMJ 2004;329:548) Lactobacillus therapy shortens pediatric diarrhea by .7 days with 1.6 fewer stools by day 2 (pediatrics 2002;109:678) Rafael CR, et al. Improved cure of bacterial vaginosis with single dose of tinidazole (2 g), lactobacillus rhamnosus GR-1, and lactobacillus reuteri RC-14: a randomized, double-blind, placebo-controlled trial. Can J Microbiol 55:2009;133-38 Vaginal pH and lactobacilli Normal vaginal pH is regulated by estrogen Vaginal pH of newborn is around 5 at birth Skin metabolizes glucose to lactate “acid mantle” of the skin is 4.5 Linhares IM, Summers PR, Larsen B, Giraldo PC, Witkin SS. Contemporary perspectives on vaginal pH and lactobacilli. Am J Obstet Gynecol 2011:204;120.e1-5 False but Popular Concept yeast Yeast True concept for some bacteria and trichomonas, but not yeast