* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download blood - I am biomed
Monoclonal antibody wikipedia , lookup
Cell theory wikipedia , lookup
Human embryogenesis wikipedia , lookup
Hematopoietic stem cell transplantation wikipedia , lookup
Developmental biology wikipedia , lookup
Homeostasis wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
Hematopoietic stem cell wikipedia , lookup
Regeneration in humans wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
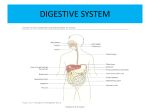
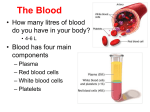
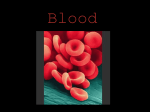
BLOOD Meghna.D.Punjabi 1 • Cells of human body cannot move around to obtain O2 and nutrients or eliminate CO2 & wastes. • These needs are met by 2 fluids: 1. Blood 2. Interstitial Fluid • Blood forms 7% of the body weight. • Blood in the vessel is always in motion because of pumping action of the heart, this continual flow maintains a fairly constant environment for the body cells. Meghna.D.Punjabi 2 Meghna.D.Punjabi 3 Functions of Blood 1. Transportation 2. Regulation 3. Protection Meghna.D.Punjabi 4 Transportation Blood transports O2 from the lungs to the cells of the body and CO2 from body cells to lungs for exhalation. Carries nutrients from GI trait to body cells & hormones from endocine glands to other body cells. Transports heat & waste products to lungs, kidney & skin for elimination from the body. Meghna.D.Punjabi 5 Regulation Circulating blood maintains homeostasis in all body fluids. Blood helps regulate pH through buffers. Maintains body temperature. Meghna.D.Punjabi 6 Protection Blood can clot which can protect against its excessive loss from the cardio vascular system after an injury. White blood cells protect against disease by carrying on phagocytosis. Meghna.D.Punjabi 7 Composition of Blood Meghna.D.Punjabi 8 Composition of Blood Composed of straw coloured transparent fluid plasma, in which different types of cells are suspended. Blood Volume Plasma Cells 45% 55% Meghna.D.Punjabi 9 Plasma • Constituents of plasma are water (90 to 92%) and dissolved substances including the following:• Plasma proteins (7% of plasma) • Inorganic salts • Nutrients, principally from digested foods • Waste materials • Hormones • Gases Meghna.D.Punjabi 10 Plasma Proteins Retained within blood because they are too large to escape through capillary pores into tissues. Responsible for creating osmotic pressure of blood (25mmHg). Plasma viscosity (thickness) is due to plasma proteins mainly albumins and fibrinogen. Meghna.D.Punjabi 11 Albumins Formed in Liver. Maintain normal plasma osmotic pressure. Act as carrier molecules for lipids & steroid hormones. Meghna.D.Punjabi 12 Globulins • Formed in liver & lymphoid tissue. • As antibodies (Immunoglobulins), complex proteins produced by lymphocytes that play an important part in immunity, by binding to & neutralizing foreign materials (antigens) such as micro organisms. • Transportation of some hormones & mineral salts. E.g. Thyroglobulin carries hormone thyroxine & transferrin carries the mineral iron. • Inhibition of some proteolytic enzymes E.g. macroglobulin inhibits trypsin activity Meghna.D.Punjabi 13 Clotting Factors Substances essential for clotting of blood. Senim is plasma from which clotting factors have been removed Synthesized in liver Essential for blood coag Fibrinogen Meghna.D.Punjabi 14 Inorganic Mineral Salts • They are involved in the following:A. Muscle contraction. B. Transmission of nerve impulses. C. Formation of secretions & maintenance of acid-base balance • pH is measure of the concentration of hydrogen ion • pH of blood is between 7.35 & 7.45. Meghna.D.Punjabi 15 Nutrients • Products of digestion pass into blood for distribution to all body cells. • These include amino acids (from proteins), glucose (from carbohydrates), fatty acids & glycerol (from triglycerides), vitamins & minerals. • Together with mineral salts they are required by all body cells to provide energy, heat, materials for repair & replacement, for synthesis of other blood components & secretions. Meghna.D.Punjabi 16 • Urea, creatinine & uric acid are waste products of protein metabolism. • Formed in liver and conveyed in blood to kidneys for excretion. • Substances synthesized by endocrine glands. • Influence cellular activity. Hormones Endocrine cells Blood Target tissue Meghna.D.Punjabi 17 Gases O2 associated with hemoglobin inside RBC’s. CO2 is dissolved in plasma. N2 no known function. Meghna.D.Punjabi 18 Cellular content of blood Meghna.D.Punjabi 19 • All originate from pluripotent stem cells (pluri=several). Pluripotent stem cells are cells that have the capacity to develop into several different types of cells. • Stem cells in red bone marrow(which is highly vascularized connective tissue located in the microscopic spares between trabeculae of spongy bone tissue) reproduce themselves into proliferate & differentiate cells that give rise to old cells. • Process of blood cell formation called haemopoiesis (poiesis= making). Meghna.D.Punjabi 20 DEVELOPMENT OF BLOOD CELLS Meghna.D.Punjabi ALL 21 Erythrocytes (RBC’s) Biconcave discs, no nucleus, 8micron diameter. Main function is gas transport mainly of O2 but some carry CO2. Biconcavity increases surface area for gas exchange & slim structure of the central portion allows fast entry & exit of gases. Cells are flexible so they can squeeze through capillaries & contain no intracellular organelles leaving more space for haemoglobin, large pigmented protein responsible for gas transport. Produced in red bone marrow, present in ends of long bones & in flat and irregular bones. Lifespan in circulation = 120 days Development takes about 7 days called erythropoiesis. Meghna.D.Punjabi 22 O2 Transport Haemoglobin large complex protein containing globular protein (Globin) & a pigmented iron containing complex called haem. Each haemoglobin molecule contains 4 globin chains & 4 haem units, each with one atom of iron. Each atom of iron can combine with an oxygen molecule, this means that a single haemoglobin molecule can carry up to 4 molecules of oxygen. Meghna.D.Punjabi 23 When all 4 O2 binding sites on a haemoglobin molecule are full means it is saturated. Hb binds reversibly to O2 to give oxyhaemoglobin. O2 of blood increases & gives bright red colour due to high levels of oxyhaemoglobin as the level of O2 falls it results in dark bluish colour because it is not saturated. Meghna.D.Punjabi 24 Association of O2 and Hb is loose so oxyhaemoglobin releases O2 readily under certain conditions. Meghna.D.Punjabi 25 Low pH Metabolically active tissues e.g. exercising muscle, release acid waste products, so local pH falls. Oxyhaemoglobin readily breaks down to provide additional O2 for tissue use. Meghna.D.Punjabi 26 Low O2 levels As O2 levels fall oxyhaemoglobin breaks down to form O2 e.g. in body tissues which constantly consume O2 keeping levels low. At higher O2 levels as in lungs, the oxyhaemoglobin formation is favoured. Meghna.D.Punjabi 27 Temperature • Actively metabolizing tissues which have higher than normal O2 needs are warmer than less active ones. • This drives the equation to the left such that O2 dissociation increases & ensures that active tissues receive a higher O2 supply than less active tissues. • Lungs, alveoli exposed to inspired air, temperature lower, oxyhaemoglobin formed. Meghna.D.Punjabi 28 Control of Erythropoiesis • Number of red cells fairly constant i.e. Bone marrow produces erythrocytes @ at which they are destroyed. • Due to homeostatic negative feedback mechanism. • Increase erythropoiesis due to hypoxia i.e. Deficient O2 supply to body cells. • O2 carrying power of blood is reduced by hemorrhage. • O2 tension in air reduced at high altitudes. Meghna.D.Punjabi 29 Destruction of erythrocytes Meghna.D.Punjabi 30 Destruction of erythrocytes • Life span = 120 days • Breakdown, or haemolysis carried out by phagocytic reticuloendothelial cells. • Main sites of haemolysis = spleen, bone marrow & liver • Erythrocytes age results in changes in cell membrane which is susceptible to haemolysis. • Iron released by haemolysis retained in bone marrow to form new haemoglobin molecules. • Biliverdin formed from haem part of haemoglobin • This is reduced to yellow pigment bilirubin, before being bound to plasma globulin & transported to liver where it is changed from a fat soluble to a water soluble form to be excreted as a constituent of bile. Meghna.D.Punjabi 31 ERYTHROCYTES NORMAL VALUES Meghna.D.Punjabi 32 ABO SYSTEM Meghna.D.Punjabi 33 BLOOD GROUPS • 1) Depends on types of antigen on red blood cells • 2) Individuals make antibodies to these antigen, but not to their own type of antigen, since if they did the antigen and anti bodies would react causing transfusion reaction which can be fatal. • 3) Individuals that are transfused with blood of the same group that is processing the same antigens on the surface of the cells, their immune system will not recognize them as foreign and will not reject them. • 4) However, if individual is given different blood type (Different type of antigen on red blood cells) , their immune system will mount an attack upon them and destroy the transfused cells. This is the basis of the TRANSFUSION REACTION: the two blood types , the donor and recipient are incompatible . Meghna.D.Punjabi 34 THE ABO SYSTEM 55% of the population has either A-type antigens (Blood group A), or B-type antigens (Blood group B), or both (Blood group AB) on their red cell surface. Remaining 45% have neither A nor B type antigens. (Blood group O ) The corresponding antibodies are called anti-A and anti-B. Meghna.D.Punjabi 35 ABO SYSTEM Blood group A individuals cannot make anti-A, since otherwise a reaction to their own cells would occur, however they make anti-B. Blood group B individuals, for the same reasons , make only anti A. Blood group – AB make neither anti-A nor anti-B, therefore they are known as UNIVARSAL RECIPIENTS: Transfusion of either type A or type B blood into these individuals is likely to be safe, since there are no antibodies to react with them. Blood group O make both anti-A and anti-B but do not have neither A nor B antigens on their red cell membranes, and their blood may be safely transfused into A, B,AB or O types : group O is known as the UNIVARSAL DONOR Meghna.D.Punjabi 36 RHESUS SYSTEM The red blood cell membrane antigen important here is the Rhesus (Rh) antigen, or Rhesus factor. About 85% of people have this antigen: they are Rhesus +ve (Rh +) and do not therefore make antiRhesus antibodies Remaining 15 % have no Rhesus antigen : they are Rhesus –ve (Rh –), therefore are capable of making antRhesus antibodies, but are stimulated to do so only in certain circumstances, Ex. In pregnancy or as the result of an incompatible blood transfusion. Meghna.D.Punjabi 37 Leukocytes (white blood cells) Function: Defending the body against microbes and other foreign bodies. They are the largest blood vessels. They account for 1% of the blood volume. They contain nuclei and some have granules in their cytoplasm. Meghna.D.Punjabi 38 Types of WBC’s Granulocytes (polymorphenuclear leukocytes) Basophils Neutrophils Eosinophils Meghna.D.Punjabi 39 Types of WBC’s Agranulocytes Lymphocytes Monocytes Meghna.D.Punjabi 40 WBC’S Meghna.D.Punjabi 41 WBC’S Formation: Granulopoiesis Follow a common line of development through myeloblast to myelocyte before differentiating into 3 types. All granules have multilobed nuclei in their cytoplasm. Their names represent the dyes they take up when stained in the laboratory, Meghna.D.Punjabi 42 WBC’S EOSINOPHILS (RED ACID DYE-EOSIN) BASOPHILS (ALKALYINE METHYLENE BLUE) NEUTROPHILS (BOTH DYES) Meghna.D.Punjabi 43 NEUTROPHILS-DIAPEDESIS Meghna.D.Punjabi 44 PHAGOCYTIC ACTION OF NEUTROPHILS Meghna.D.Punjabi 45 NEUTROPHILS • Main Function: Protect against any foreign material entering the body mainly microbes and to remove waste materials e.g cell debris • Attracted in large numbers to any area of infection by chemical substances released by damaged cells called CHEMOTAXINS. • Are Highly mobile, and squeeze through the capillary walls in the affected area by diapedesis. • Thereafter they engulf and kill the microbes by phagocytosis. Meghna.D.Punjabi 46 NEUTROPHILS • Their nuclei are characteristically complex with up to six lobes and their granules are lysosomes containing enzymes to digest infected material. • Physiological Increase in circulating neutrophils: • A) Strenuous exercise • B) Later stages of normal pregnancy. • C)Microbial Infection • D)Extensive tissue damage e.g. inflammation,myocardial infarction,burns. • E)Metabolic Disorders e.g. diabetic ketoacidosis,acute gout. • F) Leukaemia. G) Heavy Smoking. H) Use of oral contraceptives. Meghna.D.Punjabi 47 EOSINOPHILS They leave capillaries and enter tissue fliuds. Although capable of phagocytosis, are less active in this than neutrophils;their specialized role appears to be in elimination of parasites,such as worms,which are too big to be phagocytosed. They have certain toxic chemicals stored in their granules,which they release when the eosinophils binds an infecting organism. Found at sites of allergic inflammation such as asthmatic airways and skin allergies. They are believed to release enzymes, such as histamine, that combine the effects of histamine and other mediators of inflammation in allergic reactions. They promote tissue inflammation by releasing their array of toxic chemicals. v Meghna.D.Punjabi 48 BASOPHILS They are closely associated with allergic reactions,contains cytoplasmic granules packed with heparin ( an anticoagulant); histamine (an inflammatory agent) and other substances that produce inflammation. Stimulus that causes basophils to release the contents of their granules is an allergen (an antigen that causes some kind of allergy) of some type. Mast cells found in connective tissue are similar to basophils. Meghna.D.Punjabi 49 AGRANULOCYTES Large nucleus and no granules in their cytoplasm. Called Monocytes and Lymphocytes. Make up 25% to 50% of all leukocytes. Meghna.D.Punjabi 50 MONOCYTES Large mononuclear cells that originate in red bone marrow. Some circulate in the blood and are actively motile and phagocytic while others migrate into the tissues where they develop into macrophages. Monocytes arrive in large numbers and destroy more microbes, upon arrival they enlarge and differentiate into wandering macrophages, which clean up cellular debris and microbes by phagocytosis after an infection. Meghna.D.Punjabi 51 MONOCYTES Both type of cells produce interlukin 1, which: A) Acts on hypothalamus, causing the rise in body temperature associated with microbial infections. B) Stimulates the production of some globulins by the liver. C) Enhances the production of T-lymphocytes. Meghna.D.Punjabi 52 Monocyte-Macrophage System Sometimes called reticuloendothelial system and consists of body’s complement of monocytes and macrophages. Some macrophages are mobile, whereas others are fixed i.e.they reside in a particular tissue. Some Fixed Macrophages include: 1)Histiocytes in connective tissues. 2)Synovial cells in joints. 3) Osteoclasts in bone. 4)Mesangial cells in the glomerulus of nephrons in the kidney. 5) Microglia in the brain. 6) Kupffer cells in liver. 7)Langerhans cells in skin 8) Alveolar macrophages in lungs. Meghna.D.Punjabi 53 MACROPHAGES Actively phagocytic and if they encounter large amounts of foreign or waste material, they tend to multiply at the site and ‘wall off’ the area, isolating the material, e.g. pockets of tubercular infection in the lungs. They synthesise and release an array of biologically active chemicals, called cytokines, including interlukin 1. They also have a central role linking the non-specific and specific (immune) systems of body defence, and produce factors important in inflammation and repair. Their numbers are increased in microbial infections, collagen diseases and some non-infective bowel conditions. Meghna.D.Punjabi 54 LYMPHOCYTES They are smaller than monocytes and have large nuclei. They circulate in blood and found in great numbers in lymphatic tissue such as lymph nodes and the spleen. They develop from pluripotent stem cells in red bone marrow and from precursors in lymphoid tissue, then travel in the blood to lymphoid tissue elsewhere in the body where they are activated, i.e. they become immunocompetent which means they are able to respond to antigens (foreign material). Meghna.D.Punjabi 55 LYMPHOCYTES Examples of antigens Include: A) Cells regarded by lymphocytes as abnormal, e.g. cells that have been invaded by viruses, cancer cells,tissue transplant cells. B) Pollen from flowers and plants. C) Fungi. D) Bacteria. E) Some large molecule drug, e.g. penicillin,asprin. Meghna.D.Punjabi 56 LYMPHOCYTES Although all lymphocytes originate from one type of stem cell, when they are activated in lymphatic tissue, two distinct types of lymphocytes are produced. Tlymphocytes Blymphocytes Meghna.D.Punjabi 57 T-Lymphocytes Processed by thymus gland, lies between heart and sternum. Hormone thymosin, produced by thymus, is responsible for promoting the processing, which leads to the formation of fully specialized (differentiated), mature, functional TLymphocytes. These T-Lymphocytes are programmed to recognize only one type of antigen, and during its subsequent travels through the body will react to no other antigen, however dangerous it might be. T-Lymphocytes provide cell mediated immunity. Meghna.D.Punjabi 58 CLONAL EXPANSION OF TLYMPHOCYTES Meghna.D.Punjabi 59 CELL-MEDIATED IMMUNITY T-lymphocytes are released into circulation . When they encounter their antigen for the first time they become sensitized to it. If the antigen has come from outside the body, it needs to be ‘presented’ to the T-lymphocytes on the surface of an antigen presenting cell There are different types of antigen presenting cell, including macrophages Meghna.D.Punjabi 60 CELL MEDIATED IMMUNITY Macrophages are part of the non-specific defenses, b’coz they engulf and digest antigens indiscriminately, but they also participate in immune responses. To do this, after digesting the antigen they transport the most antigenic fragment to their own cell membrane and display it on their surface. On their movement around the body, still displaying the antigen fragment, they eventually come into contact with the T-lymphocyte that has been processed to target that particular antigen. If the antigen is an abnormal body cell, such as a cancer cell, it too will be displaying foreign (non-self) material on its cell membrane that will stimulate the T-lymphocyte. Whichever way the antigen is presented to the T-Lymphocytes, it stimulates the division and proliferation (clonal expansion) of the T-lymphocyte. Meghna.D.Punjabi 61 Types of T-Lymphocytes Memory T-Cells • These provide cell-mediated immunity by responding rapidly to another encounter with the same antigen. Cytotoxic T-Cells • These directly inactivate any cells carrying antigens. • They attach themselves to target cell and release powerful toxins, which are effective because the two cells are so close together. • The main role of cytotoxic T-lymphocytes is in destruction of abnormal body cells, e.g. infected cells and cancer cells. Meghna.D.Punjabi 62 Types of T-Lymphocytes Helper T-Cells Their central role in immunity is emphasized in situations where they are destroyed, as by the human immunodeficiency virus (HIV). When helper T-Lymphocytes fall significantly, the whole immune system is compromised. They are the commonest of the T-Lymphocytes; their main functions include: A) Production of special chemicals called cytokines,e.g. interleukins and interferons, which support promote cytotoxic T-Lymphocytes and macrophages. B) Co-operating with B-Lymphocytes to produce antibodies; although BLymphocytes are responsible for antibody manufacture, they require to be stimulated by a helper T-Lymphocyte first. Meghna.D.Punjabi 63 B-Lymphocytes • Processed in bone marrow. • Their role is in production of antibodies (immunoglobulins), which are proteins designed to bind to, and cause the destruction of, an antigen • Each B-lymphocyte targets one specific antigen: the antibody released reacts with one type of antigen and no other. • B-lymphocytes provide antibody-mediated immunity. Meghna.D.Punjabi 64 CLONAL EXPANSION OF B-LYMPHOCYTES Meghna.D.Punjabi 65 Antibody-Mediated (Humoral) Immunity • B-Lymphocytes are fixed in lymphoid tissue ( e.g. the spleen and lymph nodes). They recognize and bind antigen particles without having to be presented with them by an antigen presenting cell. Once its antigen has been detected and bound, and with the help of a helper T-Lymphocyte, the B-Lymphocyte enlarges and begins to divide (clonal expansion). It produces two functionally distinct types of cell,plasma cells and memory B-Cells. Meghna.D.Punjabi 66 Plasma Cells Secrete antibodies into the blood. Antibodies carried throughout the tissues, while the B-Lymphocytes themselves remain fixed in lymphoid tissue. Plasma cells live no longer than a day and produce only one type of antibody, which targets specific antigen that originally bound to BLymphocyte. Antibodies: A) Bind to antigens, labelling them as targets for other defence cells such as cytotoxic T-Lymphocytes and macrophages. B) Bind to bacterial toxins, neutralising them. C) Activate complement. Meghna.D.Punjabi 67 Memory B-Cells These cells remain in body long after the initial episode has been dealt with, and rapidly respond to another encounter with the same antigen by stimulating the production of antibody – secreting plasma cells. Meghna.D.Punjabi 68 INTERDEPENDANCE OF T AND B LYMPHOCYTE Meghna.D.Punjabi 69 LEUKOCYTE-COUNT Meghna.D.Punjabi 70 PLATELETS Meghna.D.Punjabi 71 PLATELETS (THROMBOCYTES) Very small non-nucleated discs, 2 to 4µm in diameter, derived from the cytoplasm of megakaryocytes in red bone marrow. They contain a variety of substances that promote blood clotting, which causes haemostasis (cessation of blood). Normal blood platelet count is between 200*109/l and 350*109/l (200000 to 350000/mm3). Meghna.D.Punjabi 72 PLATELETS (THROMBOCYTES) The kidneys release a substance called thrombopoietin, which stimulates platelet synthesis, other cytokines may also be involved. Lifespan of platelets is between 8 and 11 days and those not used in haemostasis are destroyed by macrophages, mainly in spleen. About a third of platelets are stored within the spleen rather than in the circulation; this is an emergency store that can be released as required to control excessive bleeding. Meghna.D.Punjabi 73 HAEMOSTASIS When a blood vessel is damaged, loss of blood is stopped and healing occurs in a series of overlapping processes, in which platelets play a vital part. 1) VASOCONSTRICTION 2) PLATELET PLUG FORMATION 3) COAGULATION (BLOOD CLOTTING) 4)FIBRINOLYSIS Meghna.D.Punjabi 74 STAGES OF CLOTTING Meghna.D.Punjabi 75 BLOOD CLOTTING FACTORS Meghna.D.Punjabi 76 1-VASOCONSTRICTION When platelets come in contact with a damage blood vessel, their surface become sticky and they adhere to the damaged wall. They then release serotonin (5hydroxyptamine), which constricts (narrows) the vessel, reducing blood flow through it. Other chemicals that cause vasoconstriction, e.g. thromboxanes , are released by the damaged vessel itself Meghna.D.Punjabi 77 2-PLATELET PLUG FORMATION The adherent platelets clump to each other and release other substances, including adenosine diphosphate (ADP), which attract more platelets to the site. Passing platelets stick to those already at the damaged vessel and they too release their chemicals. This is a positive feedback system by which many platelets rapidly arrive at the site of vascular damage and quickly form a temporary seal – the platelet plug. Meghna.D.Punjabi 78 3-COAGULATION (BLOOD CLOTTING) Complex process that involves a positive feedback system. Blood clotting results in formation of insoluble thread-like mesh of fibrin which traps blood cells and is much stronger than the rapidly formed platelet plug. In the final stages of this process Prothrombin activator acts on plasma protein Prothrombin converting it to thrombin. Thrombin then acts on another plasma protein fibrinogen and converts it to fibrin. Meghna.D.Punjabi 79 EXTRINSIC/INTRINSIC PATHWAYS Prothrombin activator can be formed by two processes which often occur together: the extrinsic and intrinsic pathways. The extrinsic pathway occurs rapidly(within seconds) when there is tissue damage outside the circulation . Damaged tissue releases a complex of chemicals called thromboplastin or tissue factor, which initiate coagulation. Meghna.D.Punjabi 80 EXTRINSIC/INTRINSIC PATHWAYS The intrinsic pathway is slower (3-6 min) and is confined to the circulation. It is triggered by damage to the blood vessel lining (endothelium) and the effects of platelets adhering to it. After a time the clot shrinks, squeezing out serum, a clear sticky fluid that consists of plasma from which clotting factors have been removed. Meghna.D.Punjabi 81 CLOTTING OF BLOOD Meghna.D.Punjabi 82 4-FIBRINOLYSIS After the clot has formed the process of removing it and healing the damage blood vessel begins. The breakdown of the clot, of fibrinolysis, is the first stage. An inactive substance called plasminogen is present in the clot and is converted to the enzyme plasmin by activators released from the damaged endothelial cells. Plasmin initiates the breakdown of fibrin to soluble products that are treated as waste material and removed by phagocytosis. As the clot is removed, healing process restores the integrity of the blood vessel wall. Meghna.D.Punjabi 83 CONTROL OF COAGULATION The process of blood clotting relies heavily on several processes that are self-perpetuating-that is, once started , positive feedback mechanism promotes their continuation. For e.g. thrombin is a powerful stimulator of its own production. The body therefore possess several mechanisms to control and limit the coagulation cascade: otherwise once started the clotting process would spread throughout the circulatory system, far beyond requirements. Meghna.D.Punjabi 84 CONTROL OF COAGULATION The main controls are : 1) The perfect smoothness of normal blood vessel lining ; platelets do not adhere to this surface 2) The binding of thrombin to a special thrombin receptor on the cells lining blood vessels; once bound, thrombin is inactivated The presence of natural anticoagulants, e.g. heparin, in the blood, which inactivate clotting factors Meghna.D.Punjabi 85