* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pituitary Disorders - Endocrinology
Hormonal breast enhancement wikipedia , lookup
Sex reassignment therapy wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Neuroendocrine tumor wikipedia , lookup
Growth hormone therapy wikipedia , lookup
Hypothalamus wikipedia , lookup
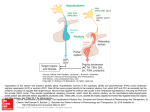
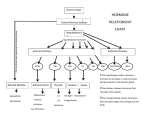
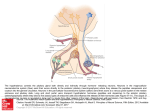
Anterior Pituitary Masses and Hyperprolactinemia Thomas Repas DO FACP CDE UW Hospital and Clinics Department of Medicine Section of Endocrinology, Diabetes & Metabolism H4/568 CSC (5148), 600 Highland Avenue, Madison, WI 53792 Thursday October 13, 2005 Objectives • • • • Causes of Pituitary Masses Evaluation of a Pituitary Incidentaloma Management of Pituitary Neoplasia Abnormal Anterior Pituitary Function Associated with Pituitary Masses • Hyperprolactinemia and Prolactinomas • Causes • Management I will not discuss in detail… • • • • Management of Cushing’s Disease Management of Acromegaly Management of Hypopituitarism Evaluation and Management of Posterior Pituitary Disorders and Diabetes Insipidus Normal Pituitary Anatomy Lechan RM. Neuroendocrinology of Pituitary Hormone Regulation. Endocrinology and Metabolism Clinics 16:475-501, 1987 Normal Pituitary Anatomy Modified from Lechan RM. Neuroendocrinology of Pituitary Hormone Regulation. Endocrinology and Metabolism Clinics 16:475-501, 1987 Development of Human Anterior Pituitary Cohen and Radovick, Endocrine Reviews 23: 431-442, 2002 Anterior Pituitary Function Hormone Stimulators Corticotroph Gonadotroph Thyrotroph Lactotroph Somatotroph POMC, ACTH FSH, LH TSH Prolactin GH TRH Estrogen, TRH GHRH, GHS T3, T4, Dopamine, Somatostati n, GH Dopamine Somatostatin, IGF-1, Activins Thyroid Breast and other tissues Liver, bone and other tissues CRH, AVP, gp130 cytokines Inhibitors Glucocorticoids Target Gland Adrenals Trophic Effects Steroid production GnRH, Estrogen Sex steroids, inhibin Ovary, Testes Sex Steroid, Follicular growth, Germ Cell maturation T4 synthesis and secretion Adapted from: William’s Textbook of Endocrinology, 10th ed., Figure 8-4, pg 180. Milk Productio n IGF-1 production, Growth induction, Insulin antagonis m Etiology of Pituitary Masses Etiology of Pituitary-Hypothalamic Lesions • Non-Functioning Pituitary Adenomas • Endocrine active pituitary adenomas – – – – – Prolactinoma Somatotropinoma Corticotropinoma Thyrotropinoma Other mixed endocrine active adenomas • Malignant pituitary tumors: Functional and non-functional pituitary carcinoma • Metastases in the pituitary (breast, lung, stomach, kidney) • Pituitary cysts: Rathke's cleft cyst, Mucocoeles, Others • Empty sella syndrome Etiology of Pituitary-Hypothalamic Lesions (continued) • Developmental abnormalities: Craniopharyngioma (occasionally intrasellar location), Germinoma, Others • Primary Tumors of the central nervous system: Perisellar meningioma, Optic glioma, Others • Vascular tumors: Hemangioblastoma, Others • Malignant systemic diseases: Hodgkin's disease, Non-Hodgkin lymphoma, Leukemic infiltration, Histiocystosis X, Eosinophilic granuloma, Giant cell granuloma (tumor) • Granulomatous diseases: Neurosarcoidosis, Wegner's granulomatosis, Tuberculosis, Syphilis • Vascular aneurysms (intrasellar location) Pituitary Adenoma Sellar Masses Pituitary Adenoma Snyder, P. UpToDate Craniopharyngioma Sellar Masses Pituitary Adenoma Snyder, P. UpToDate Lymphocytic Hypophysitis Infiltrative Disorders: Sarcoidosis From EndoText: http://www.endotext.com/neuroendo/neuroendo4/neuroendoframe4.htm Evaluation of a Pituitary Incidentaloma Evaluation of an Incidental Pituitary Mass • Radiologic Evaluation • Clinical Evaluation • Hormonal Evaluation Radiologic Evaluation: MRI • Preferred imaging study for the pituitary • Better visualization of soft tissues and vascular structures than CT • No exposure to ionizing radiation • Images are generated based upon the magnetic properties of the hydrogen atoms • T1-weighted images produce high–signal intensity images of fat. Structures such as fatty marrow and orbital fat show up as bright images. • T2-weighted images produce high-intensity signals of structures with high water content, such as cerebrospinal fluid and cystic lesions Mulinda, J. Pituitary Macroadenomas, 9/19/05. http://www.emedicine.com/med/topic1379.htm Radiologic Evaluation: CT • Better at visualizing bony structures and calcifications within soft tissues • Better at determining diagnosis of tumors with calcification, such as germinomas, craniopharyngiomas, and meningiomas • May be useful when MRI is contraindicated, such as in patients with pacemakers or metallic implants in the brain or eyes • Disadvantages include: – less optimal soft tissue imaging compared to MRI – use of intravenous contrast media – exposure to radiation Mulinda, J. Pituitary Macroadenomas, 9/19/05. http://www.emedicine.com/med/topic1379.htm Craniopharyngioma on CT Kruskal, J. UpToDate Clinical Evaluation • All patients with macroadenomas should have formal visual field testing • In addition to radiographic and hormonal evaluation, patients should be asked and examined for any clinical signs suspicious for pituitary hyperfunction or hypofunction Hormonal Evaluation • May include of both basal hormone measurement and dynamic stimulation testing. • All pituitary masses should have screening basal hormone measurements, including: – – – – – Prolactin TSH, FT4 ACTH, AM cortisol, midnight salivary cortisol LH, FSH, estradiol or testosterone Insulin-like growth factor-1 (IGF-1) Mulinda, J. Pituitary Macroadenomas, 9/19/05. http://www.emedicine.com/med/topic1379.htm Hormonal Evaluation (continued) Dynamic stimulation/suppression testing may be useful in select cases to further evaluate pituitary reserve and/or for pituitary hyperfunction • • • • • • • • Dexamethasone suppression testing Oral glucose GH suppression test GHRH, L-dopa, arginine CRH stimulation Metyrapone TRH stimulation GnRH stimulation Insulin-induced hypoglycemia Mulinda, J. Pituitary Macroadenomas, 9/19/05. http://www.emedicine.com/med/topic1379.htm Management of Pituitary Tumors Management of Pituitary Neoplasia • • • • Observation Pharmacotherapy Surgery Radiation Therapy Pituitary Incidentaloma < 10 mm > 10 mm Evaluate for: Evaluate for Hormonal Hypersecretion • Hormonal Hypersecretion • Hormonal Hyposecretion • Normal Hormonal or Visual Abnormalities Observe Treatment Visual Changes/defects No Abnormalities Observe Observation and Follow-up • If less than 20 mm and no neurologic or hormonal abnormalities: – Monitor for adenoma size, visual changes, and hormonal hypersecretion in 6 and 12 months, then annually for a few years • Lesions less than 10 mm and proven to have no hormonal hypersecretion: – Lesions 2 to 4 mm: no further testing required – Lesions 5 to 9 mm: MRI can be done once or twice over the subsequent two years; if the lesion is stable in this period, the frequency can be decreased Peter J Snyder MD, “Pituitary incidentaloma” UpToDate November 25, 2003 Pharmacotherapy • Most useful in prolactinomas, alone or with other intervention. • May be used in certain other functioning tumors as adjunctive therapy along with surgical and/or radiotherapy Pharmacotherapy Which pharmacologic option to choose depends on type of tumor: • Dopamine agonists: bromocriptine, cabergoline- most useful for prolactinomas, less useful for GH secreting adenomas • Somatostatin analog (Octreotide, Octreotide LAR)- most useful for acromegaly • Pegvisomant (GH receptor blocker)- useful in acromegaly refractory to somatostatin analogues • Other: ketoconazole, metyrapone, mitotane- for Cushings disease- use limited by side effects, expense and lack of efficacy Pituitary Surgery • Transsphenoidal approach: used for 95% of pituitary tumors • Endonasal submucosal transseptal approach • Septal Pushover/Direct Sphenoidotomy • Endoscopic approach Indications for Surgery • Surgery is the first-line treatment of symptomatic pituitary adenomas. • Useful when medical or radiotherapy fails • Surgery provides prompt relief from excess hormone secretion and mass effect. • Indicated in pituitary apoplexy with compressive symptoms Outcome of Transsphenoidal Surgery Tumor Remission (%) Recurrence at 10 years (%) Non-functioning adenoma Not applicable* 16 GH adenoma Microadenoma 88 1.3 Macroadenoma PRL adenoma Microadenoma Macroadenoma ACTH adenoma Microadenoma Macroadenoma 65 87 13 56 91 65 *Visual improvement occurs in 87% of those with preoperative visual loss. John A. Jane, Jr., MD Edward R. Laws, Jr., MD, SURGICAL MANAGEMENT OF PITUITARY ADENOMAS Chapter 13. http://www.endotext.com/neuroendo/neuroendo13/neuroendoframe13.htm 12 (Adults), 42 (Pediatric) Complications of Transsphenoidal Surgery Outcome Measure Mortality Incidence (%) <0.5 Major complication (CSF leak, 1.5 Minor complication (sinus 6.5 meningitis, ischemic stroke, intracranial hemorrhage, vascular injury, visual loss) disease, septal perforations, epistaxis, wound infections and hematomas) John A. Jane, Jr., MD Edward R. Laws, Jr., MD, SURGICAL MANAGEMENT OF PITUITARY ADENOMAS Chapter 13. http://www.endotext.com/neuroendo/neuroendo13/neuroendoframe13.htm Radiation Therapy • Reserved for patients with larger tumors and/or persistent hormonal hyperfunction despite surgical intervention – Conventional radiotherapy – Gamma knife radiosurgery Conventional Radiotherapy • Response is slow, may take 5 to 10 years for full effect • Successful in up to 80% of acromegalics and 55-60% of Cushing’s disease • High rate of hypopituitarism: up to 60% • Other complications: optic nerve damage, seizures, radionecrosis of brain tissue Basic and Clinical Endocrinology, 6th ed. Chapter 5 Hypothalamus and Pituitary, 100-162. Gamma Knife Radiosurgery • Stereotactic CT guided cobalt 60 gamma radiation to narrowly focused area • Long term data not yet available but suggest up to a 70% response rate for acromegaly and up to 70% for Cushing’s in some centers • Complication rate likely lower, but still high rate of hypopituitarism (~55%) Basic and Clinical Endocrinology, 6th ed. Chapter 5 Hypothalamus and Pituitary, 100-162. Abnormal Pituitary Function Associated with Pituitary Tumors Disorders of Pituitary Function • Hypopituitarism – Central hypoadrenalism, hypogonadism, hypothyroidism or GH deficiency – Panhypopituitarism • Hypersecretion of Pituitary Hormones – Hyperprolactinemia – Acromegaly – Cushing’s Disease Acromegaly http://www.endotext.com/neuroendo/neuroendo5e/neuroendoframe5e.htm Wright, V. UpToDate Clinical Findings of Acromegaly Symptoms and signs at presentation Overall prevalence (%) Facial change, acral enlargement, and soft-tissue swelling 100 Excessive sweating 83 Acroparesthesiae/ carpal tunnel syndrome 68 Tiredness and lethargy 53 Headaches 53 Oligo- or amenorrhea, infertility 55* Erectile dysfunction and/or decreased libido 42# Arthropathy 37 Impaired glucose tolerance/ diabetes 37 Goiter 35 Ear, nose throat and dental problems 32 Congestive cardiac failure/ arrythmia 25 Hypertension 23 Visual field defects 17 * percentage of female patients # percentage of male patients http://www.endotext.com/neuroendo/neuroendo5e/neuroendoframe5e.htm Complications of Acromegaly Cardiovascular • Ischemic heart disease • Cardiomyopathy • Congestive heart failure • Arrhythmias • Hypertension Respiratory • Kyphosis • Obstructive sleep apnea Metabolic • Diabetes mellitus/IGT • Hyperlipidemia http://www.endotext.com/neuroendo/neuroendo5e/neuroendoframe5e.htm Neurologic •Carpal Tunnel syndrome •Stroke Neoplastic •Colorectal •(Breast and prostate - uncertain) Musculoskeletal •Degenerative arthropathy •Calcific discopathy, pyrophosphate arthropathy Acromegaly: Causes of Death • Cardiovascular- 38 to 62 percent • Respiratory- 0 to 25 percent • Malignancy- 9 to 25 percent Diagnosis of Acromegaly • Random GH – not useful • Insulin like growth factor 1 (IGF-1) – best for screening • Oral glucose GH suppression testing – gold standard to confirm diagnosis Cushing’s Disease William’s Textbook of Endocrinology. 8th Ed. Foster, DW, Wilson, JD (Eds), WB Saunders, Philadelphia, 1996 Cushing’s Syndrome vs. Cushing’s Disease • Cushing’s syndrome is a syndrome due to excess cortisol from pituitary, adrenal or other sources (exogenous glucocorticoids, ectopic ACTH, etc.) • Cushing’s disease is hypercortisolism due to excess pituitary secretion of ACTH (about 70% of cases of endogenous Cushing’s syndrome) Cushing’s Syndrome • Moon facies • Facial plethora • Supraclavicular fat pads • Buffalo hump • Truncal obesity • Weight gain • Purple striae •Proximal muscle weakness •Easy bruising •Hirsutism •Hypertension •Osteopenia •Diabetes mellitus/IGT • Impaired immune function/poor wound healing Central Obesity in Cushing’s Disease William’s Textbook of Endocrinology. 8th Ed. Foster, DW, Wilson, JD (Eds), WB Saunders, Philadelphia, 1996 Progressive Obesity of Cushing’s Disease Age 6 Age 7 Age 8 Age 9 William’s Textbook of Endocrinology. 8th Ed. Foster, DW, Wilson, JD (Eds), WB Saunders, Philadelphia, 1996 Age 11 Buffalo Hump in Cushing’s Disease Orth, D. UpToDate Striae in Cushing’s Disease Orth, D. UpToDate Proximal Muscle Wasting in Cushing’s Syndrome William’s Textbook of Endocrinology. 8th Ed. Foster, DW, Wilson, JD (Eds), WB Saunders, Philadelphia, 1996 Diagnosis of Cushing’s Syndrome • • • • ACTH, AM cortisol 24 hour urine cortisol Dexamethasone suppression testing Midnight salivary cortisol Dexamethasone Suppression Test http://www.endotext.com/neuroendo/neuroendo7/neuroendoframe7.htm Circadian Studies of Serum Cortisol Levels http://www.endotext.com/neuroendo/neuroendo7/neuroendoframe7.htm Hyperprolactinemia and Prolactinomas Prolactin • Human prolactin is a 198 amino acid polypeptide • Primary function is to enhance breast development during pregnancy and to induce lactation • Prolactin also binds to specific receptors in the gonads, lymphoid cells, and liver • Secretion is pulsatile; it increases with sleep, stress, pregnancy, and chest wall stimulation or trauma Prolactin • Secretion of prolactin is under tonic inhibitory control by dopamine, which acts via D2-type receptors located on lactotrophs • Prolactin production can be stimulated by the hypothalamic peptides, thyrotropinreleasing hormone (TRH) and vasoactive intestinal peptide (VIP) Clinical Features of Hyperprolactinemia/Prolactinoma • Women may present with oligomenorrhea, amenorrhea, galactorrhea or infertility • Men often have less symptoms than women (sexual dysfunction, visual problems, or headache) and are diagnosed later • In both sexes, tumor mass effects may cause visual-field defects or headache Causes of Hyperprolactinemia • Hypothalamic Dopamine Deficiency – Diseases of the hypothalamus( including tumors, arterio-venous malformations, and inflammatory processes – Drugs (e.g. alpha-methyldopa and reserpine) • Defective Transport Mechanisms – Section of the pituitary stalk – Pituitary or stalk tumors Causes of Hyperprolactinemia (continued) • Lactotroph Insensitivity to Dopamine – Dopamine-receptor-blocking agents: phenothiazines (e.g. chlorpromazine), butyrophenones (haloperidol), and benzamides (metoclopramide, sulpiride, and domperidone) • Stimulation of Lactotrophs – Hypothyroidism- increased TRH production (acts as a PRF) – Estrogens: stimulate lactotrophs – Injury to the chest wall: abnormal stimulation of the reflex associated with the rise in prolactin that is seen normally in lactating women during suckling REMEMBER: Not all hyperprolactinemia is due to a prolactinoma Am J Obstet Gynecol 1972; 113:14; N Engl J Med 1977; 296:589; Clin Ther 200; 22:1085; Clin Endocrinol 1976; 5:273; J Clin Endocrinol Metab 1976; 42:1148; J Clin Endocrinoll Metab 42: 181; J Clin Endocrinol Metab 1982; 54:869; Br Med J 1976; 1:1186; JAMA 1976; 235:2316; Am J Cardiol 1983; 51:1466; J Clin Endocrinol Metab 1985; 60:144. Work up of Patient with Hyperprolactinemia • In females, pregnancy must always be ruled out • Get a TSH- hypothyroidism is another common cause of elevated prolactin: • Obtain detailed drug history- rule out medication effects • Rule out other common causes including: – – – – – – Nonfasting sample Nipple stimulation or sex Excessive exercise History of chest wall surgery or trauma Renal failure Cirrhosis • If no cause determined or tumor suspected, consider MRI, especially if high prolactin levels (> 100 ng/mL) http://www.emedicine.com/Med/topic1915.htm Prolactinomas • Most common of functional pituitary adenomas • 25-30% of all pituitary adenomas • Some growth hormone (GH)–producing tumors also co-secrete PRL • Of women with prolactinomas- 90% present with microprolactinomas • Of men with prolactinomas- up to 60% present with macroprolactinomas http://www.emedicine.com/Med/topic1915.htm Treatment • Pharmacotherapy • Surgical resection • Radiotherapy Pharmacotherapy of Prolactinomas • Dopamine agonists are treatment of choice for most prolactinomas • Choices include Bromocriptine, Pergolide and Cabergoline • Side effects include: postural hypotension, dizziness, nasal stuffiness, GI side effects. Dopamine Agonist Therapy Webster, J et al. N Engl J Med 1994; 331:904. Long-term Effects of Bromocriptine Therapy J Clin Endocrinol Metab 50:1026 1033 Success Rate of Bromocriptine in Amenorrhea • After 1 month of treatment, one woman in four will return to normal menstrual cycling; • In 2 months, this number will increase to six out of 10 • After 10 months, eight out of 10 women will be menstruating normally • Of the remaining 20%, most are hypogonadal due to pituitary surgery or irradiation http://www.endotext.com/neuroendo/neuroendo6/neuroendoframe6.htm Decrease in Size of Prolactinoma after Bromocriptine Abrahamson, M. UpToDate Dopamine Agonists • Bromocriptine- start low dose at 1.25- 2.5 mg day at night before increasing to 2.5 – 10 mg per day in divided doses. Take with food to reduce side effects. • Cabergoline- more effective and with less side effects than Bromocriptine but also more expensive- given once or twice a week with a starting dose of 0.25 mg 2 x week Titrate these based on prolactin levels and tolerability Conclusion • Pituitary microadenomas are common, not all are of clinical concern • ALL pituitary tumors require evaluation of hormonal status • Follow up and monitoring will depend on size and other features of tumor • Dopamine agonists are the treatment of choice for most prolactinomas • Surgical intervention is initial TOC for large tumors and other hyperfunctional tumors (GH, ACTH secreting) • Not every patient with hyperprolactinemia has a prolactinoma!!!