* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Must be present!
West Nile fever wikipedia , lookup
United States biological defense program wikipedia , lookup
Trichinosis wikipedia , lookup
Yersinia pestis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Hepatitis B wikipedia , lookup
Typhoid fever wikipedia , lookup
Anthrax vaccine adsorbed wikipedia , lookup
Steven Hatfill wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
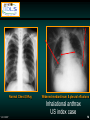
Onchocerciasis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
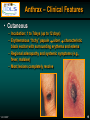
Oesophagostomum wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Schistosomiasis wikipedia , lookup
Biological warfare wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Marburg virus disease wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Leptospirosis wikipedia , lookup
® “Preparing Our Communities” Welcome! V 2.9 04/07 ® BDLS is a registered trademark of the American Medical Association 1 Faculty Disclosure • For Continuing Medical Education (CME) purposes as required by the American Medical Association (AMA) and other continuing education credit authorizing organizations: – In order to assure the highest quality of CME programming, the AMA requires that faculty disclose any information relating to a conflict of interest or potential conflict of interest prior to the start of an educational activity. – The teaching faculty for the BDLS course offered today have no relationships / affiliations relating to a possible conflict of interest to disclose. Nor will there be any discussion of off label usage during this course. V 2.9 04/07 2 Biological Events Chapter 5 V 2.9 04/07 3 Objectives • Describe the difference between biological events and bioterrorism (BT) • Discuss public health BT surveillance • Identify the CDC BT Category A agents • Identify emerging infectious diseases • Compare and contrast BT and other CBRNE WMD utilizing the DISASTER paradigm V 2.9 04/07 4 Biological Events Biological events: Natural vs. Intentional Outbreak of monkey pox in pet prairie dogs Release of anthrax in mail Avian Flu pandemic Salmonella sprayed on food bar Natural occurrence of anthrax Smallpox infection Bubonic plague outbreak Aerosolized botulinum toxin V 2.9 04/07 5 Bioterrorism Release Types: Overt or Covert Covert or Overt ? Overt –Notice of release provided –May contain a threat –Designed to create panic or fear –May be hoax (white powder) or credible threat Letter sent to the New York Post and NBC News: Containing “white powder” V 2.9 04/07 Covert or Overt ? Covert Release (1763)Captain Simeon Ecuyer had sent –No notice or threat smallpox-infected blankets and handkerchiefs to the Indians surrounding the fort (as a supposed peace offering)-but actually an to early example of –Difficult detect biological warfare -- which started an •Persons care at usual epidemic amongseek the Indians. medical care facilities •Early symptoms non-specific so detection may be delayed •Focus: Astute clinician make diagnosis and notify health department (Detection) 6 Potential Methods of Detection Public Health Surveillance • • • • • • • • • • • Increased number of patients Increased unexplained deaths Unusual patient age distribution Unusual seasonality Unusual manifestation of disease Animal die-off Notifiable disease reporting by physicians & other providers Automated reporting of laboratory results Number and type of 911 calls Number and type of EMS runs Syndromic surveillance V 2.9 04/07 7 CDC Categories BT Agents Divided into Categories A, B,C based on: • Quantity of agent available • Ability to disseminate the agent • Person-to-person transmission • Severity of disease • Public response, panic, etc.. • Overall risk to national security V 2.9 04/07 8 Category A Agents • • • • • • V 2.9 04/07 Anthrax Smallpox Plague Botulinum toxin Tularemia Viral hemorrhagic fevers 9 Category B Agents (examples) • Infectious Agents – Brucellosis – Glanders • Bio-toxins – Ricin toxin from Ricinus communis (castor beans) – Staphylococcal enterotoxin B • Water safety threats –Vibrio cholerae • Food safety threats –Salmonella species –Escherichia coli O157:H7 –Shigella • Viral encephalitis –Venezuelan Equine Encephalitis V 2.9 04/07 Why are these Category B Agents •Less quantity available than Category A •Harder to disseminate •Less person to person transmission- if any •Slightly less severity of disease •Less known to public therefore less likely to cause panic •Slightly less risk to National Security 10 Category C • Emerging infectious diseases as bioterrorism agents – Nipah virus – Hantavirus • Emerging infectious disease that posses a significant public health threat – Avian Flu – SARS V 2.9 04/07 11 Category A: Anthrax •Endemic in animals worldwide with occasional human cases – Handling infected animal products (especially cattle, sheep, horses, mules and goats) •Spores used for bioattack – Aerosolized directly or sent in mail/packages •Three forms –Cutaneous, Inhalation, GI Anthrax in CSF—US index case V 2.9 04/07 12 Anthrax – Clinical Features • Inhalation – Incubation: 2-43 days (may be longer) – Prodrome • Fevers, malaise, dry cough, chest pain, dyspnea, myalgia – Abrupt onset of fulminant illness • Sudden high fever, respiratory distress, shock • Meningitis in ~50% • Actual pneumonia uncommon V 2.9 04/07 13 Normal Chest X-Ray V 2.9 04/07 Widened mediastinum & pleural effusions Inhalational anthrax US index case 14 Anthrax – Clinical Features • Cutaneous – Incubation: 1 to 7days (up to 12 days) – Erythematous “itchy” papule ulcer characteristic black eschar with surrounding erythema and edema – Regional adenopathy and systemic symptoms (e.g., fever, malaise) – Most lesions completely resolve V 2.9 04/07 15 Anthrax – Clinical Features • Gastrointestinal – Incubation period 1-7 days – Not likely after a bioattack – Presents as febrile illness with bloody diarrhea – Eating undercooked infected meat V 2.9 04/07 16 Anthrax Diagnosis • Blood cultures – Usually positive in < 24h • Gram stain pleural fluid or CSF – Sputum gram stain/culture is usually NOT positive • Inhalational disease – Very suggestive if fever and widened mediastinum • Cutaneous disease – Culture fluid from under eschar • Nasal swabs are a poor test V 2.9 04/07 17 Anthrax –Treatment • Ciprofloxacin 400 mg IV q12h – 10-15 mg/kg for children – Other fluoroquinolones probably also effective OR • Doxycycline 100 mg IV q12h – 2.2 mg/kg for children PLUS • 1 or 2 additional antibiotics – Clindamycin, rifampin, vancomycin, penicillin, chloramphenicol, imipenem, or clarithromycin V 2.9 04/07 18 Prophylaxis and Infection Control • Prophylaxis – Ciprofloxacin 500 mg PO BID(Peds:10-15 mg/kg) or – Doxycycline 100 mg PO BID (Peds:2.2 mg/kg) – Continue for 60 days (? 100 days) – Vaccine available for DOD forces • Infection Control – Standard barrier precautions are needed – Not transmitted person-to-person • Only immunize / prophylaxis exposed at BT attack V 2.9 04/07 19 Anthrax Vaccination Schedule 1 2 3 4 5 6 • 6 shots over 18 months, then annual booster – Dosing schedule is 0.5 mL subcutaneously at each visit – Then yearly boosters V 2.9 04/07 20 Botulism Clostridium botulinum A Toxin Producing Obligate, Anaerobic, Spore Forming, Gram Pos. Bacillus V 2.9 04/07 21 Botulism - General • Caused by a toxin produced by Clostridium botulinum • Sporadic cases and outbreaks caused by tainted foods • For bioattack toxin could be delivered as an aerosol or used to contaminate food / water V 2.9 04/07 22 Botulism - Clinical Features • 12 to 36 hour “incubation” – Range 2 h to 8 days • Clinical recognition is key to diagnosis • Bulbar palsies: Must be present! – Ptosis, blurred vision, dry mouth, dysarthria, trouble swallowing • Afebrile,“AAO x 3”, difficulty speaking • Descending skeletal muscle paralysis • Death: Respiratory muscle paralysis V 2.9 04/07 23 17 Year-Old with Mild Botulism V 2.9 04/07 24 Botulism - Treatment • Supportive care • Respiratory failure – Prolonged Ventilator support • Antitoxin – State health department obtained – Prevents further damage – Does not alter current damage V 2.9 04/07 25 Botulism – Infection Control Prophylaxis • No proven prophylaxis at this time • Investigational Vaccine Isolation • Standard precautions (not P-to-P) Need to contact public health authority immediately: Others may be exposed to contaminated food source or agent V 2.9 04/07 26 Yersinia pestis Plague Yersinia pestis Source: www.cdc.gov Gram Neg., Anaerobic, Rod Shaped Bac. V 2.9 04/07 “Safety Pin” Bipolar on Wright Staining 27 Plague - General • Endemic in animals throughout the world – Prairie dogs in the Southwestern US • High potential as a BT agent • Endemic form – Spread to humans via a flea vector – Results in bubonic form of the disease • Bioattack – Most likely aerosolized – Results in pneumonic plague – Release of infected fleas V 2.9 04/07 Buboes Source: www.cdc.gov 28 Plague – Clinical Features • Following Aerosolized Bioattack – 1- 6 day incubation – Abrupt onset • High fever, chills, and malaise • Cough with bloody sputum • Sepsis – Severe rapidly progressive pneumonia – Untreated 100% mortality V 2.9 04/07 29 Plague - Diagnosis • CXR with patchy infiltrates • Culture of blood and sputum – Need to inform the laboratory if you suspect plague … special techniques • May show characteristic “safety-pin” bipolar staining • Sudden # Gm(neg) pneumonia V 2.9 04/07 30 Normal Chest X-Ray V 2.9 04/07 Plague pneumonia 31 Plague - Treatment Preferred: Start within first 24 hours for 10 days • Streptomycin 1 g IM q12h – 15 mg/kg/dose for children – Avoid in pregnant women • Gentamicin 5 mg /kg IM or IV qd – Or 2 mg/kg load the 1.7 mg/kg q8h – For children use 2.5 mg/kg q8h Alternative • Doxycycline 100 mg IV q12h – 2.2 mg/kg/dose q12h for children • Ciprofloxacin 400 mg IV q12h – Other fluoroquinolones probably effective – For children 15 mg/kg/dose q12h V 2.9 04/07 32 Plague - Infection Control Prophylaxis: Treat for 7 days • Doxycycline 100 mg PO bid – 2.2 mg/kg for children • Ciprofloxacin 500 mg PO bid – 20 mg/kg for children – other fluoroquinolones probably effective Isolation • Droplet precautions (Yes, P-to-P) V 2.9 04/07 33 Smallpox Source: www.cdc.gov V 2.9 04/07 34 Smallpox - General • One of the deadliest disease – Mortality rate of 30% • US stopped vaccinating in 1972 • Declared eradicated by WHO – In 1980, however... • Bioattack – Aerosolized virus or by exposure to purposefully infected terrorists V 2.9 04/07 35 Smallpox - Clinical Features • Incubation period – 7-17 day (average 12d), Weaponized 3-5 d • Severe prodrome Key difference! – 2-3 day of fever, severe myalgias, prostration, occ. n/v, delerium – 10% with light facial erythematous rash • Distinctive rash – Initially on face and extremities – Including palms and soles – Spreads to trunk V 2.9 04/07 36 Small Pox - Clinical Features • Rash – Macules papules vesicles pustules – Unlike chicken pox, lesions don’t appear in “crops” • All lesions in an area are in the same stage of development • Lesions are firm, deep, frequently umbilicated • Rash scabs over in 1-2 weeks Chickenpox V 2.9 04/07 Smallpox Source: www.cdc.gov 37 Smallpox The main diagnostic tool for smallpox Source: www.cdc.gov V 2.9 04/07 is the history and physical! 38 Smallpox - Treatment • Vaccination – In the early stages of disease • Supportive care – Penicillinase-resistant antibiotics (for secondary infection) – Daily eye rinsing – Adequate hydration and nutrition • FDA has not approved specific therapy – Topical idoxuridine for corneal lesions (Dendrid) – Cidofovir ? V 2.9 04/07 39 Smallpox - Infection Control Prophylaxis • Vaccine is effective if given within 3 days of exposure Isolation • Airborne and contact precautions • Febrile illness after potential exposure should prompt isolation before rash starts Immediate contact your hospital epidemiologist and the public health authorities V 2.9 04/07 40 Francisella tularensis Tularemia Source: www.cdc.gov Gram Neg. Coccobacillus V 2.9 04/07 41 Tularemia - General • Endemic in North America and Eurasia • Sporadic human cases spread by ticks or biting flies – Occasionally from direct contact with infected animals (ulceroglandular) • Bioattack – Aerosolized bacteria – Typhoidal tularemia & (+ / - ) pneumonia V 2.9 04/07 42 Tularemia - Clinical Features • Bioattack – 3-5 day incubation (range 1-14 days) – Acute febrile illness with prostration – ~80% will have radiographic evidence of pneumonia – May have associated conjunctivitis or skin ulcer & regional adenopathy V 2.9 04/07 43 Tularemia - Diagnosis • Culture of blood and sputum – May take weeks to isolate and ID • Gram negative coccobacillus – Confirmation may require reference laboratory – Potential hazard to laboratory personnel Laboratory must be notified if tularemia is suspected V 2.9 04/07 44 Tularemia - Treatment Preferred Treatment time varies with Abx • Streptomycin 1 g IM q12h – 15 mg/kg for children • Gentamicin 5 mg / kg IM or IB q day – for children use 2.5 mg/kg q8h Alternative • Doxycycline 100 mg IV q12h – 2.2 mg/kg for children • Ciprofloxacin 400 mg IV q12h – Children 15 mg/kg – Other fluoroquinolones probably effective V 2.9 04/07 45 Tularemia - Infection Control Prophylaxis: Treat for 14 days • Doxycycline 100 mg PO bid – 2.2 mg/kg for children • Ciprofloxacin 500 mg PO bid – 15-20 mg/kg for children • Tetracycline Isolation: • Standard precautions (Not P-to-P) V 2.9 04/07 46 Viral Hemorrhagic Fevers Source: www.cdc.gov Ebola virus V 2.9 04/07 47 VHF - General • Naturally occurring disease – Transmitted to humans by contact with infected animals or arthropod vectors. – Sporadic outbreaks in Africa, parts of Asia and Europe (Outside of Africa, likely BT event) • VHF viruses as bioterrorism agents – Weaponized by several countries – Aerosolization • Case fatality rates – Omsk hemorrhagic fever – Ebola V 2.9 04/07 0.5% 90% 48 VHF - Clinical Features • Incubation 2 - 21days – Depends on virus • Initial presentation – Nonspecific prodrome (fever, myalgias, headache, abdominal pain, prostration) – Exam may show only flushing of face and chest, conjunctival injection, and petechiae • Disease progresses to generalized mucous membrane hemorrhage and shock occurs Marburg Disease V 2.9 04/07 Bolivian Hemorrhagic Fever 49 VHF - Diagnosis • Ancillary testing: – Thrombocytopenia, leukopenia, AST elevation common • Definitive diagnosis requires detection of antigens or antibodies – Testing done at CDC Do not wait to confirm the diagnosis before notifying the local public health authorities V 2.9 04/07 50 VHF - Treatment • Supportive care • Ribavirin may be useful – Best early in the course of illness – Adults and children: 30 mg/kg IV load (max 2 g) • then 16 mg/kg (max 1g) q6h x 4 days • then 8 mg/kg (max 500 mg) IV q8h for 6 days – Oral dosing regimen is available V 2.9 04/07 51 VHF - Infection Control Prophylaxis: None at this time Vaccine in primates being tested Isolation: Key! – Blood and bodily fluids extremely infectious – Liquid-impervious protective coverings, including leg and shoe coverings – Double gloves, Face shields or goggles – N-95 or better respirators – Negative pressure room V 2.9 04/07 52 Emerging Infectious Diseases V 2.9 04/07 53 Pandemic A Global Epidemic! V 2.9 04/07 54 Past flu pandemics Credit: US National Museum of Health and Medicine 1918: “Spanish Flu” A(H1N1) 1957: “Asian Flu” A(H2N2) 1968: “Hong Kong Flu” A(H3N2) 20-40 m deaths 1-4 m deaths 1-4 m deaths 675,000 US deaths 70,000 US deaths 34,000 US deaths V 2.9 04/07 55 Put another way … Life expectancy-USA, 1900-28 70 60 50 40 19 00 . 19 03 . 19 06 . 19 09 . 19 12 . 19 15 . 19 18 . 19 21 . 19 24 . 19 27 . 30 V 2.9 04/07 56 Pandemic Influenza www.cdc.gov V 2.9 04/07 57 Pandemic Influenza V 2.9 04/07 58 Pandemic Influenza Healthcare Workforce • Who is going to show up for work? • The reports, articles and plans are alarming! • Will you? V 2.9 04/07 59 Containment • • • • • Limit travel Isolate ill and quarantine exposed Trace contacts Curfews & cancel public gatherings Prophylaxis & treatment – Neuramidase inhibitors ? – Vaccine ? V 2.9 04/07 60 D: Detection I: Incident Command S: Safety & Security A: Assess Hazards S: Support T: Triage & Treatment E: Evacuation R: Recovery V 2.9 04/07 61 Detection There may not be a “scene” May be hard to detect Long Incubation period Symptoms manifest slowly Non-specific symptoms Beware of multiple people with similar Complaints, particularly in the “healthy” population V 2.9 04/07 62 D: Detection I: Incident Command S: Safety & Security A: Assess Hazards S: Support T: Triage & Treatment E: Evacuation R: Recovery V 2.9 04/07 63 Incident Command • Absence of a “scene” if covert • Lead role of law enforcement • Unified command of law enforcement and public health • Special public health emergency powers V 2.9 04/07 64 Security • Hospital ingress and egress – Must be able to secure hospital • Most bioattacks likely covert – Patients will come in through ER – ER becomes the “scene” V 2.9 04/07 65 Suspicious Package • Do not open suspicious packages • Secure area – Shut off ventilation if possible • Alert appropriate authorities V 2.9 04/07 66 Assessing Hazards • Protective isolation & quarantine • Epidemiologic assessment • Environmental assessment • Laboratory diagnosis of ill persons • Role of immunization, prophylaxis and treatment • Little role for decontamination V 2.9 04/07 67 Personal Protective Equipment • Degree of protection – Controversial • CDC guidelines – Very conservative • N-95 respirators, gloves, fluid-impervious gowns – Better than nothing V 2.9 04/07 68 Support • • • • Initially, local management issue! Local hospital capacity Local healthcare providers Is your local community ready? V 2.9 04/07 69 Support Local Hospital Capacity Coordination & Augmentation • • • • Pre-event planning essential for “surge” Surge facilities for medical care expansion Expect being overrun with “worried well” Involvement of local pharmacies V 2.9 04/07 70 Support: Strategic National Stockpile • Pre-positioned material managed by CDC and DHS • Medications, antidotes, vaccines, PPE, equipment,et al. • 12 hour Push Packages • Vendor managed inventory • Local coordination of receipt critical V 2.9 04/07 71 Triage Three types of patients: (1). Ill and need definitive treatment (2). Exposed but not ill: may need prophylaxis and quarantine (3). Not exposed: need reassurance Difficult to distinguish between groups 2 & 3! V 2.9 04/07 72 Evacuation • • • • Dedicated treatment facilities Isolation of patients Surge capacity implications Hospital becomes a “scene” V 2.9 04/07 73 Recovery • Law enforcement • Evidence, apprehension, prosecution,... • Public health • Stop spread, identify source, treatment options,... • Mental health • Wide-spread panic, “worried-well”, responders,... • Environmental health • Viability of weaponized release, “nature” effects, soiled materials,... V 2.9 04/07 74 Summary Now you can: • Describe the difference between biological events and bioterrorism (BT) • Discuss public health BT surveillance • Identify the CDC BT Category A agents • Identify emerging infectious diseases • Compare and contrast BT and other CBRNE WMD utilizing the DISASTER paradigm V 2.9 04/07 75 Questions? V 2.9 04/07 76