* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download document
Coronary artery disease wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
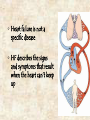
Heart failure wikipedia , lookup
Myocardial infarction wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial septal defect wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
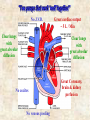
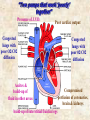
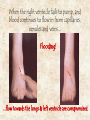
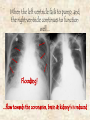
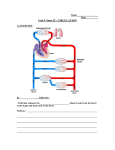
‘Need to knows’ • Review of pump physiology (two pumps) • Review of pump flow (backwards & forwards) • Review causes that effect C.H.F. (valves, M.I., clogged pipes/hard pipes, high b/p, C.A.D., C.O.P.D.) • Natural progression of C.H.F. • Signs and symptoms • What we can do about it No J.V.D. Clear lungs with great alveolar diffusion Great cardiac output ~ 5 L / Min Clear lungs with great alveolar diffusion No ascites No venous pooling Great Coronary, brain & kidney perfusion Presence of J.V.D. Poor cardiac output Congested lungs with poor O2/C02 diffusion Ascites & build-up of fluid in other areas build-up of interstitial fluid in legs Congested lungs with poor 02/C02 diffusion Compromised perfusion of coronaries, brain & kidneys When a lock on the Trent-Severn waterway doesn’t work, and water continues to flow from the feeder rivers and lakes... Flooding! up-stream Cities & Towns downstream lack water When the right ventricle fails to pump, and blood continues to flow in from capillaries, venules and veins... Flooding! ...flow towards the lungs & left ventricle are compromised When the left ventricle fails to pump, and the right ventricle continues to function well... Flooding! ...flow towards the coronaries, brain & kidney’s is reduced Ascites Right Ventricular Failure (RVF) • Occurs when the right ventricle fails as an effective forward pump, causing back-pressure of blood into the systemic venous circulation • Can result from: – Chronic hypertension (in which LVF usually precedes RVF) – COPD – Pulmonary embolism – Valvular heart disease – Right ventricular infarction • RVF most commonly results from LVF Left Ventricular Failure (LVF) and Pulmonary Edema • LVF occurs when the left ventricle fails to function as an effective forward pump, causing a back-pressure of blood into the pulmonary circulation • May be caused by a variety of forms of heart disease including ischemic, valvular, and hypertensive heart disease • Untreated, significant LVF culminates in pulmonary edema • Heart failure is not a specific disease • HF describes the signs and symptoms that result when the heart can’t keep up Not quite a ‘Cinderella’ story... Grandma Faccino 11:30 AM Needs a rest, mildly s.o.b. due to work in the garden. 8:30 AM, She woke-up this morning feeling well. 9:00 AM, Takes her water pills, 7 other meds & puffers. 8:30 PM 11:00 PM 5:00 PM Mild c/p relieved In bed, legs up, Complaint of with 2 sprays ntg. head elevated sore feet and legs, with her ntg on they seem more 2:15 AM Severe s.o.b. with bedside table. swollen. audible crackles 10:00 PM 7:00 PM Gets ready for Dinner & a water 3:30 PM bed with her pill with 3 meds Needs a rest, 4 pillows. & 2 puffers. due to s.o.b. 1:00 PM walking up stairs. 2:00 AM Chest pain resolved First onset Lunch & a water pill with 4 other with 2 ntg sprays. of s.o.b. with meds and puffers. Mild J.V.D. visible. c/p 2:30 EMS arrives, Grandma Faccino presents: • In severe respiratory distress (sitting forward and upright, with use of supraclavicular muscles and having 2 word dyspnea). • She is extremely diaphoretic, appears in severe distress and is becoming lethargic and cyanotic. •There is obvious external jugular venous distension, gross pitting edema and ascites. 2:30 EMS arrives, Grandma Faccino’s vitals are: • Respirations: 48b/m, shallow and decreasing from exhaustion. • Pulse of 156 weak and irregular. • Skin – diaphoretic x 3, warm core with cool extremities. She appears pale with cyanotic nail-beds. • O2 sat reads ‘84’ • Auscilltation: Course crackles in all air fields bilaterally. Audible adventitious sounds orally. • G.C.S. – Eyes open to loud verbal (2), spontaneous verbal with 3 word dyspnea (5), spontaneous motor (6). 2:45 AM EMS is still in Grandma Faccino’s residence new vitals are: • Respirations: 10b/m very shallow. • Pulse of 170 hardly palpable at radial. • Skin – diaphoretic x 3, warm core with cool extremities. She appears pale with cyanotic nailbeds. • O2 sat reads in 60’s • Auscilltation: Course crackles in upper air fields with decreased b/s in bases bilaterally. Froth in airway. • G.C.S. – Eyes closed (1), occasional moaning (3), withdraws from pain (4). History • • • • Why did you call? What has changed? How long has the dyspnea been present? Was the onset gradual or abrupt? Is the dyspnea better or worse with position? Is there associated orthopnea? • Has the patient been coughing? - If so, was the cough productive? - What was the character and colour? - Is there any hemoptysis? History (continued) • Is there pain associated with the dyspnea? - OPQRST for the pain • Pt’s past history? • Allergies • Current Medications (pay close attention to O2 therapy, oral bronchodilators, corticosteriods,Beta Blockers, Digitalis, ACE Inhibitors, Diuretics) Quick differentiation of Shortness of Breath Asthma Pulmonary edema (CHF) Pneumonia gradual & fast onset Quick onset & deterioration Slow onset Crackles that go from fine to course quickly, wheezes. B/p norm fine and course crackles. Congestion ‘one sided’ or two if both lungs effected. b/p elevated b/p norm No productive sputum Late – frothy red sputum Chronic cloudy yellow/green Wheezes History of Asthma History of c.h.f., History/signs-symptoms fluid retention, new of infection infarct, etc. Many Others Standard Assessment for all SOB calls • • • • • • ABC’s and Critical interventions Chief Complaint Incident History (OPQRST) Med History (SAMPLE) Vitals Physical Assessment Management of Respiratory Distress due to Pulmonary Edema • • • • • ABC’s (including O2 or BVM), Monitor, and Baseline Vital Signs Consider positive pressure ventilations Thorough History and Assessment of respiratory status (chest assessment) Carefully screen patient for indications and contraindications for Nitroglycerine™ Transport in the most appropriate position as per patient condition without delay Nitroglyerin for Pulmonary Edema 1. Indications: See new standing order!.