* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Stroke Volume - emseducation.info
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Jatene procedure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Artificial heart valve wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Myocardial infarction wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
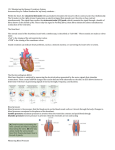
CARDIAC EMERGENCIES Anatomy • Cardiovascular System's two major components • Size • • • • Location The heart and peripheral blood vessels Size of a closed fist Center of chest in the Mediastinum Position • Approximately 2/3 is to the left of the midline • Apex Bottom; above the diaphragm • Base: Top; lies approximately at the level of the second rib Great Vessels connect here Layers Endocardium • Inner most layer • Lines the heart’s chambers • Bathed in blood Layers Myocardium • Thick middle layer of the heart • Cells are unique Cells physically resemble skeletal muscle, But have electrical properties similar to smooth muscle. Contain specialized structures to help to rapidly conduct electrical impulses from one muscle to another enabling the heart to contract Layers Pericardium • Protective sac • Consists of two layers – Visceral aka epicardium: Epicardium: Inner layer in contact with the heart muscle itself – Parietal outer fibrous layer Contains: Layers Pericardial Fluid • Between the two layers • 25 ml • Straw colored • Reduces friction as the heart beats and changes position • Epicardium: Inner layer in contact with the heart muscle itself Chambers 4 Chambers • Atria – separated by the interatrial septum • Ventricles – separated by the interventricular septum Valves • The heart contains two pairs of valves • Atrioventricular Valves • Semilunar valves Made of endocardial and connective tissue Valves • Atrioventricular Control blood flow between atria and ventricles Trisucspid Valve • Between the right atrium and right ventricle • Has three leaflets or cusps; Mitral Valve • Between the left atrium and left ventricle • Two leaflets Atrioventricular Valves • The valves are connected to specialized papillary muscles in the ventricles • When relaxed they open the valves to allow for blood flow Chordae Tendoneae • Specialized fibers; connect the valve leaflets to the papillary muscle; prevents the valves from prolapsing into the atria, allowing back flow Valves • Semilunar Valves • Regulate blood flow between the ventricles and the arteries into which they empty • Left: Aortic valve; connects left ventricle to the aorta • Right: Pulmonic valve; connects right ventricle to the pulmonary artery Next: Cardiac Cycle CARDIAC CYCLE • Defined: The period of time from the end of one cardiac contraction to the end of the next • Diastole: First phase; The relaxation phase; Ventricular filling begins, blood enters through the mitral and tricuspid valves; Pulmonic and aortic valves are closed Encompasses: • Ejection Fraction • Stroke Volume • Preload • Starling’s Law • After Load Cardiac Cycle • Ejection Fraction The normal ventricle ejects about 2/3 of the blood it contains at the end of the diastole • Each time the ventricle pumps blood into the aorta, it generates pressure wave along the major arteries which we feel as a pulse The amount of blood ejected is the Stroke Volume Stroke Volume The amount of blood ejected by the heart in one cardiac cycle • Each time the ventricle pumps blood into the aorta, it generates pressure wave along the major arteries which we feel as a pulse • Stroke Volume varies between 60 and 100ml with the average being 70ml Stroke Volume Is dependent on three factors • Preload • Cardiac Contractility • Afterload Cardiac Cycle The heart can pump only the blood it receives from the venous system • Preload The pressure within the ventricles at the end of diastole Influences the force and amount of the next Contraction and is based on Starling’s Law of the Heart Cardiac Cycle • Starling’s law of the heart: The more the myocardial muscle is Stretched, the greater it’s force of contraction will be So……… Cardiac Cycle • The greater the volume of blood filling the chamber----the more forceful the cardiac contraction----the greater the venous return---the greater the preload----the greater the stroke volume Cardiac Cycle Afterload • Myocardial muscle has its limits. If stretched too far, it will not contract properly and will weaken Cardiac Cycle Afterload • The resistance against which the heart must pump • Increase in peripheral vascular resistance will decrease stroke volume • Decrease in Peripheral Vascular Resistance will increase stroke volume Cardiac Cycle • Cardiac Output • Volume of blood that the heart pumps in one minute • Stroke volume (mL) x heart rate (bpm) = cardiac output (mL/min) ?cardiac output using a value of 70 for heart rate? Cardiac Cycle • 70 mL x 70 bpm = 4,900 mL/min ELECTROPHYSIOLOGY • • • • • • • • • • • • • • • Overview Sinoatrial node Atrioventricular junction AV node Bundle of His His-Purkinje System Automaticity Excitablity Conductivity Contratility Action potential Depolarization Repolarization Excitability Thresholds Electrophysiology The heart is comprised of three types of cardiac muscle • Atrial • Ventricular • specialized excitatory and conductive fibers