* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download embryological development and dysmorphology
Survey
Document related concepts
Quantitative trait locus wikipedia , lookup
Genetic testing wikipedia , lookup
Genetic engineering wikipedia , lookup
Designer baby wikipedia , lookup
Saethre–Chotzen syndrome wikipedia , lookup
Genome (book) wikipedia , lookup
Down syndrome wikipedia , lookup
Microevolution wikipedia , lookup
Medical genetics wikipedia , lookup
DiGeorge syndrome wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Frontonasal dysplasia wikipedia , lookup
Cell-free fetal DNA wikipedia , lookup
Nutriepigenomics wikipedia , lookup
Public health genomics wikipedia , lookup
Transcript
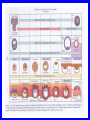
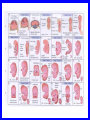
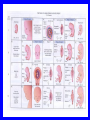
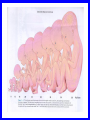
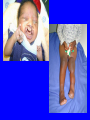
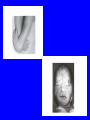
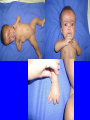
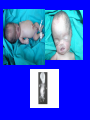
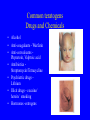
EMBRYOLOGICAL DEVELOPMENT AND DYSMORPHOLOGY Dr. E.M. Honey Department of Genetics University of Pretoria Introduction • Normal development from fertilization to birth (38 weeks) is an extremely complex process. • Divided into 3 stages: 1. Pre-embryonic – 1 to 19 days 2. Embryonic – 17 to 56 days 3. Fetal stage – 56 days till birth • All organs originates from three germ layers: a. Ectoderm b. Mesoderm c. Endoderm • All above processes under genetic and environmental control Causes of congenital abnormalities Genetic Chromosomal Single gene Multifactorial Subtotal Environmental Drugs and chemicals Infections Maternal illness Physical agents Subtotal Unknown Total 6% 7,5% 20-30% 30-40% 2% 2% 2% 1% 5-10% 50% 100% Aetiology of congenital abnormalities • 1. Single gene defects – unifactorial/ Mendelian inheritance(Autosomal dominant, autosomal recessive, Xlinked recessive) • 2. Multifactorial inheritance – genetic and environmental influences • 3. Chromosomal abnormalities – numerical or structural • 4. Teratogens • 5. Constraint Pathogenesis of congenital abnormalities • 1. Malformation – primary structural defect of an organ which results from an inherent abnormality in development Example: Cleft palate, neural tube defect Pathogenesis of congenital abnormalities • 2. Disruption – an abnormal structure of an organ or tissue as a result of external factors disturbing the normal developmental process – include ischaemia, infection or trauma Example: Amniotic band syndrome Pathogenesis of congenital abnormalities • 3. Deformation – an abnormal mechanical force which distorts an otherwise normal structure Example: Mild talipes(club foot) Pathogenesis of congenital abnormalities • 4. Dysplasia – an abnormal organisation of cells into tissue in all parts of the body in which that particular tissue is present Example: Ectodermal or skeletal dysplasia Clinical presentation of congenital malformations • Syndromes: Consistent patterns of abnormalities for which there will often be a known underlying cause Example: Down syndrome – chromosomal Van der Woude syndrome – single gene Amniotic band syndrome – disruption Clinical presentation of congenital malformations • Sequence: Consequence of a cascade of events initiated by a single primary factor Example: Potter sequence Clinical presentation of congenital malformations • Association: Certain malformations tend to occur together but can not be explained on the basis of a sequence or a syndrome Example: VACTERL association Susceptible stages of development • • • 1st trimester 0-17 days: pre-differentiation pre-implantation not susceptible 18-30 days:early differentiation highly susceptible 31-60 days: advancing organogenesis susceptibility continually lessening 2nd trimester decreasing susceptibility 3rd trimester minimal susceptibility Teratogen A teratogen is either a drug, chemical, infectious agent or physical agent, maternal disease or metabolic agent, that by acting on the developing fetus, causes a structural or functional abnormality( congenital malformation or birth defect) present at birth Teratology - Thalidomide as an example • Given as sedative to pregnant women in 1950s • Limb reduction defects in fetus when exposed between 4 and 8 weeks • Damaging tissue in progress zone of the developing limb bud • Effect is specific • Otherwise a safe drug Teratology - retinoic acid as example • Serious birth defects when fetus exposed in utero • Use in certain skin diseases(acne) and leukaemia - Ro-accutane • Endogenous retinoids component of signalling pathways used to pattern the brachial arches • Extreme caution in multivitamin supplementation Principles of teratology • Stage sensitivity - pre-implantation - embryonic period - fetal period • Organ susceptibility • Window of action • Dose response relationship • Genetic differences in susceptibility • Teratogenesis and malformation patterns Common teratogens • Maternal illness • Maternal infections • Drugs and toxins • Alcohol and smoking Common teratogens Maternal illness • • • • • • Diabetes mellitus Phenylketonuria Epilepsy Hyperthermia Hypothyroidism Hypertension Common teratogens Maternal infections • • • • • • • • Toxoplasmosis Rubella Cytomegalovirus Herpes simplex Varicella zoster Syphilis Human Parvovirus B19 HIV Common teratogens Drugs and Chemicals • Alcohol • Anti-coagulants - Warfarin • Anti-convulsants Phynetoin, Valproic acid • Antibiotics Streptomycin/Tetracycline • Psychiatric drugs Lithium • Illicit drugs - cocaine/ heroin/ smoking • Hormones -estrogens Fetal alcohol syndrome • Children born to mothers who have consistently consumed large quantities of alcohol during pregnancy • Unsure about the level that is “safe” • Recommended all women should try to abstain from alcohol intake completely • Genetic susceptibility Ionizing radiation • Survivors of the Japanese atomic bomb and large doses for therapeutic purposes • Causes breaks in DNA • Variety of anomalies - central nervous system - cleft palate - malformations of limbs, skeleton or viscera Conclusion • Different teratogens often cause very specific patterns of birth defects. • Exposure to environmental agents should be avoided during pregnancy. • Benefit of giving a drug should be weighed againt the possible harmfull effects.