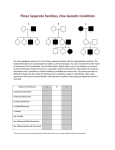
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Ante and Postnatal Screening
Survey
Document related concepts
Genetic engineering wikipedia , lookup
History of genetic engineering wikipedia , lookup
Genomic imprinting wikipedia , lookup
Hardy–Weinberg principle wikipedia , lookup
Population genetics wikipedia , lookup
Genetic drift wikipedia , lookup
Public health genomics wikipedia , lookup
Designer baby wikipedia , lookup
DNA paternity testing wikipedia , lookup
Medical genetics wikipedia , lookup
Genealogical DNA test wikipedia , lookup
Cell-free fetal DNA wikipedia , lookup
X-inactivation wikipedia , lookup
Genome (book) wikipedia , lookup
Genetic testing wikipedia , lookup
Microevolution wikipedia , lookup
Transcript
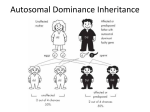
Ante- and Postnatal Screening https://www.twigonglow.com/film/b irth-936/ https://www.youtube.com/watch?v =DZsZ9vXFx04 Learning Intentions • Explain the use of antenatal care screening to identify risks and potential disorders • Describe antenatal screening techniques used – ultrasound, biochemical testing, diagnostic testing, rhesus antibody testing and PGD Antenatal Care • During pregnancy the mother is closely monitored. This includes checks on the mother’s : blood pressure blood type blood and urine general health Antenatal Care • An example of a potential complication that each assessment might reveal is: height and weight - obesity; blood pressure - hypertension; blood tests - diabetes; urine tests - renal failure; medical history - cystic fibrosis Antenatal Screening • Antenatal screening is carried out to monitor the health of a pregnant woman and her fetus • Antenatal screening identifies the risk of a disorder so that further tests can be carried out and a prenatal diagnosis can be given Screening Vs Diagnostic Tests Screening Test • A screening test detects signs and symptoms associated with a disorder • A degree of risk can be assessed Diagnostic test • A diagnostic test is a definite test which establishes, without doubt, whether a person is suffering from a specific condition or disorder Methods of Antenatal Screening • Ultrasound imaging • Biochemical tests • Diagnostic testing • Rhesus antibody testing Video Ultrasound • Dating scans (done at 8-14 weeks) give information about the stage of gestation and the due date. • Anomaly scans (done at 1820 weeks) take a close look at the fetus and the uterus. They can detect serious physical problems • Tests for marker chemicals which vary normally during pregnancy are used with dating scans Fetus at 12 weeks Biochemical Tests • Biochemical tests are used to detect the normal physiological changes of pregnancy through blood and urine samples • Changes can detect complications eg in the condition pre-eclampsia the concentration of urea in the plasma is significantly higher than normal and concentration of calcium in the urine is significantly lower Markers • At 16 – 18 weeks the pregnant woman is offered a series of biochemical tests that check for different chemical markers. • Medical conditions can also be detected by a range of marker chemicals that indicate a condition but need not necessarily be part of the condition. Markers • For example, the marker Human Chorionic Gonadotrophin normally HCG increases during weeks 6-10 then decreases to a steady low level • However, it remains high if the foetus has Down’s syndrome False Positives and Negatives • Measuring a substance at the wrong time could lead to a false positive or false negative result • For example, HCG results at 10 weeks could give a false positive and would be meaningless since both a normal pregnancy and a Down’s pregnancy would show elevated results at week 10 Diagnostic Tests They are carried out: • If routine screening has indicated an increased risk of a condition • for individuals already in high risk categories (eg women over 35) • If there is a family history of a harmful genetic disorder Risks of Diagnostic Testing • 2 main types of diagnostic testing are: Amniocentesis Chorionic Villus Sampling (CVS) • Both amniocentesis and CVS increase the risk of miscarriage • In deciding to proceed with these tests, the element of risk associated with the tests must be assessed by the parent(s) Amniocentesis • Amniocentesis is carried out at about 14-16 weeks of pregnancy • A small amount of amniotic fluid is withdrawn and this contains foetal cells • The cells are cultured to produce a karyotype, this usually takes about 2 weeks • A karyotype is a visual display of a person’s complete chromosome complement, arranged in pairs Normal Karyotypes Down’s Syndrome • A karyotype containing an extra copy of chromosome 18 indicates Edward’s Syndrome • The condition is characterised by unusual skull shape and small chin. The sufferer also has heart and kidney malformations • Very few sufferers live beyond their first year and have profound delay in all aspects of development • It occurs in 1 in 3000 live births Chorionic Villus Sampling (CVS) • This involves taking a sample of placental cells • The cells are cultured and used for karyotyping • Has an increased risk of miscarriage compared to amniocentesis but it can be carried out earlier - as early as 8 weeks into pregnancy and allows immediate karyotyping Rhesus Antibody Testing • Generally mothers show no immune response to their fetus although sensitisation to rhesus antigens can occur. • This can happen when a rhesus negative mother is first pregnant with a rhesus positive fetus and a mixing of blood at birth occurs causing sensitisation of the mother to rhesus antigens Rhesus Antibody Testing • The immune system of the mother then makes anti-rhesus antibodies and memory cells • A second rhesus positive fetus will be attacked through the placenta by the anti-rhesus antibodies from the mother • The fetus can be given saved by replacing the rhesus positive blood with rhesus negative via a transfusion • Or the mother can be injected with anti-rhesus antibodies, just after the birth of the first child, this destroys the rhesus antigen PGD • Pre-implantation genetic diagnosis (PGD) is used to identify eggs with genetic disorders. It is available to couples, in conjunction with IVF, that are at risk of having a child with a specific genetic or chromosome disorder. Learning Intention • Describe the use of post-natal screening using PKU as an example Phenylketonuria (PKU) The amino acid phenylalanine is found in the diet. enzyme C enzyme A phenylalanine enzyme B Intermediate metabolites melanin (Skin pigment ) tyrosine (an amino acid) In a PKU sufferer the gene that codes for enzyme 1 is defective – what will this result in? Phenylketonuria (PKU) enzyme C melanin enzyme A phenylalanine enzyme B Intermediate metabolites tyrosine (an amino acid) Phenylalanine builds up in the blood . (Skin pigment ) Phenylketonuria (PKU) • PKU is an autosomal recessive inherited metabolic disorder. • Phenylalanine builds up in the blood and causes mental development to be restricted • It is fairly common in the UK – about 1 in 10,000 live births. • PKU is routinely tested for in newly born babies using a Heel prick test. • PKU can be treated by following a low phenylalanine diet Phenylketonuria (PKU) Sufferers usually have a lighter skin pigment than normal, but will not be albino as some tyrosine will be present in their diet and this can re-instate the end of the pathway so some melanin is still made. enzyme C enzyme B tyrosine (an amino acid) Intermediate metabolites melanin (Skin pigment ) Albinism • Albinos cannot make enzyme C and are therefore unable to make melanin. • This protein is the dark pigment in skin and other organs, including the retina Learning Intention • To revise genetic definitions and genetic crosses What can you remember about genes, inheritance and genetic crosses? Definitions Revision 1. 2. 3. 4. 5. Haploid Diploid Alleles Recessive Dominant 6. Homozygous 7. Heterozygous 8. Genotype 9. Phenotype 10. Gene Monhybrid Cross Revision Use the following genes and symbols • T = tall plants, t = dwarf; • G = grey body flies, g = black; • R = tongue roller, r = non roller; Draw out a punnett square and work out ratios of phenotypes for the following crosses a) Tt x Tt b) Rr X rr c) Gg x Gg d) Gg x gg e) Rr x Rr a) Tt x Tt T t T TT Tt t Tt tt r r R Rr Rr r rr rr 1 roller : 1 non roller 3 tall : 1 dwarf c) Gg x Gg G g G GG Gg g Gg gg 3 grey : 1 black b) Rr x rr e) Gg x gg g g G Gg Gg g gg gg 1 grey : 1 black f) Rr x Rr R r R RR Rr r Rr rr 3 rollers : 1 non roller Learning Intention • Explain the use of pedigree charts to analyse patters of inheritance in genetic screening and how these could be used in counselling Pedigree Chart Pedigree Charts and Counselling • Pedigree charts (family trees) are used to analyse patterns of inheritance in genetic screening • Once the phenotype for a characteristic is known and a family tree is constructed most of the genotypes can be determined • This information is used by genetic counsellors to advise parents of the possibility of passing on a genetic condition to their child Different Patterns of Inheritance • • • • Autosomal recessive Autosomal dominant Autosomal incomplete dominance Sex linked recessive trait Remember X and Y chromosomes are sex chromosomes. All other chromosomes are called autosomes. William Bateson and patterns of inheritance Learning Intention • Describe the pattern of autosomal recessive inheritance Autosomal Recessive Inheritance • The trait is: – Expressed relatively rarely – May skip generations – Males and females equally affected – All sufferers homozygous recessive – Non-sufferers homozygous dominant or heterozygous Ryan’s story Female sufferer of cystic fibrosis Male non-sufferer of cystic fibrosis Autosomal Recessive Inheritance A = normal b= cystic fibrosis What is the probability of these parents’ children having cystic fibrosis? 0% Autosomal Recessive Inheritance A = normal b= cystic fibrosis What is the probability of these parents’ children having cystic fibrosis? 25% There is an autosomal blood disorder in which a faulty form of haemoglobin is produced. The allele for normal haemoglobin (H) is dominant to the allele for faulty haemoglobin (h). What is the genotype of person a) 1 in 1st generation hh a) 4 in 2nd generation Hh Learning Intention • Describe the pattern of autosomal dominant inheritance Autosomal Dominant Inheritance • Males and females affected equally • All non sufferers homozygous recessive • Sufferers homozygous dominant of heterozygous Luke’s story Female sufferer of Huntingtons Male non-sufferer of Huntingtons Autosomal Dominant Inheritance B = Huntington’s Disease sufferer b = normal What is the probability of these parents’ children having Huntington’s? 50% Learning Intention • Describe the pattern of autosomal incomplete dominance inheritance Incomplete Dominance • So far we have looked at situations where autosomal alleles are either dominant or recessive WW • In some cases dominant allele does not fully express itself, this is known as incomplete RW dominance RR RW RW RW RW Incomplete Dominance When writing out a incomplete dominance cross, both alleles have capitals and a different letter. WW RR P F1 RW RW RW RW RW Incomplete Dominance If red and a white short flowers are crossed, the offspring appear pink. Parents (P) Red RR R R x W RW RW White WW W RW RW All F1 offspring are pink. Incomplete Dominance If pink flowers were crossed with one another, what proportions of colours would you expect in the F2 generation? (Use a punnet square) x Sickle Cell • Haemoglobin S is much less efficient at carrying oxygen than normal haemoglobin. • People who are homozygous for the abnormal allele (SS) suffer from the condition sickle cell anaemia. • People who are homozygous for the normal allele (HH) produce normal haemoglobin and normal red blood cells. Sickle Cell • People who are heterozygous (HS) do not suffer from sickle cell anaemia, but from a milder condition known as the sickle cell trait. • Heterozygotes possess a phenotype 'in-between' the two homozygous phenotypes. In other words the normal allele is incompletely dominant to the sickle cell allele. Tamilore’s story Autosomal Incomplete Dominance • The fully expressed form of the disorder occurs relatively rarely • Partially expressed form occurs more frequently • Males and females equally affected Autosomal Incomplete Dominance • Non sufferers are homozygous for one incompletely dominant allele • Sufferers of the fully expressed form of the disorder are homozygous for the other incompletely dominant allele • Sufferers of the partly expressed form are heterozygous for the two alleles Learning Intention • Describe the pattern of sex linked recessive inheritance Sex linkage • The X chromosome is larger than the Y • As a result the X chromosome carries more genes • Genes which are carried on the same sex chromosome are said to be sexlinked. • Use X and Y to represent the sex chromosomes, and superscript letters to represent the alleles eg. XR Xr Sex Linked Recessive If being colour blind is recessive, cross a male colour blind with a female with colour vision who is a non carrier XbY Xb XBXB XB Y Y XB XB XBXb (1) XBY (2) XBXb (3) XBY (4) (1) (2) (3) (4) XB Female with normal colour vision Male with normal colour vision Female with normal colour vision Male with normal colour vision Sons get the Y from their dad, therefore they must inherit the disease from their mother Daughters have to get the recessive gene from both parents to inherit the condition Sex Linked Recessive • Sufferers of the trait are homozygous recessive, normally male XhY • Non sufferers are homozygous dominant XHY XHXH or are heterozygous female carriers XHXh – they don’t suffer form the condition but carry a copy of the. gene which thay can pass on to their offspring Carrier mother Carrier daughter Sex Linked Recessive • Many more males are affected than females • None of the sons of an affected male show the trait • Some of the grandsons of an affected male do show the trait Carrier daughter Carrier daughter