* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lipids Simple by Dr Sarma
Amino acid synthesis wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Butyric acid wikipedia , lookup
Lipid signaling wikipedia , lookup
Metalloprotein wikipedia , lookup
Biochemistry wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Radical (chemistry) wikipedia , lookup
Wilson's disease wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
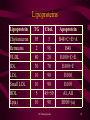
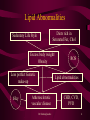
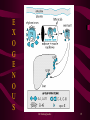
LIPIDS An over view of Normal and Abnormal Lipids Dr.Sarma@works 1 All are One • This not about the GOD • There is only one disease – Over nutrition • Its faces are many such as – – – – – Over weight / Obesity Diabetes mellitus, IR, Syndrome X Atherosclerosis – HT- CHD – CVD – RVD – PVD Hyper lipidemias – endothelial dysfunction Wear and tear of joints …. So on • What are we to do ? - Avoid over-indulgence Dr.Sarma@works 2 How much is much ? BMI = Weight in kgs Height2 in mts 70 BMI = = 25.71 1.65 x 1.65 Underweight < 20 Over weight > 25 to 30 Normal 20 to 25 Obesity >30 Waist / Hip ratio = 35” /38” = 0.92 Normal for Males < 0.90, Females <0.80 Dr.Sarma@works 3 Lipid Abnormalities Diets rich in Saturated Fat, Chol Sedentary Life Style Excess body weight/ Obesity Less perfect Genetic make-up tHcy ROS Lipid abnormalities Atherosclerotic vascular disease Dr.Sarma@works CHD, CVD, PVD 4 Why are lipids important ? • Complications of Atherosclerosis are – – – – – – CHD (Coronary Heart Disease) CVD (Cerebro Vascular Disease) RVD (Reno Vascular Disease) PVD (Peripheral Vascular Disease) These cause > 50% of all deaths - mortality The Angina, MI, - TIA, Stroke, - HT, RF, IC, Gangrene all reduce the Quality of Life morbidity Dr.Sarma@works 5 AVD – Clinical Manifestations Organ Condition Impairment Clinical Presentation Heart Coronary Heart Disease (CHD) Ischemia Infarction Angina Pectoris Myocardial Infarction Brain Cerebro vascular Disease (CVD) Ischemia Infarction Transient Ischemia attack Stroke Kidney Reno vascular Disease (RVD) Ischemia Infarction Reno vascular hypertension Renal impairment Renal Failure Ischemia Infarction Intermittent Claudication Gangrene Leg Peripheral Vascular Muscles Disease (PVD) For every thing the common denominator is ED Dr.Sarma@works 6 Lipid Transport TG EC Apoprotein boat Apo A = HDL Apo B100+C+E = VLDL, IDL Apo B100 = LDL Apo B48+C+A+E = Chylomicrons Dr.Sarma@works 7 Lipids and Lipoproteins • Lipids or Fats in our body are mainly • The non polar, hydrophobic, inner core of – Triglycerides (TG) – Cholesterol Esters (EC) • The polar, surface monolayer – Phospholipids (PL) and Free Cholesterol (C) • Apoproteins are the outer coat -amphiphatic Dr.Sarma@works 8 Lipoprotein Lipids or Fats (Hydrophobic) Size < RBC TG, EC Apoproteins A, B, C, E, (a) (Amphiphatic) Phospholipids Free Cholesterol (Hydrophilic) Dr.Sarma@works 9 Lipoproteins Lipoprotein Chylomicron Remnants VLDL IDL LDL Small LDL HDL Lp(a) TG 95 2 80 30 10 10 5 10 Chol. 5 98 20 70 90 90 45+50 90 Dr.Sarma@works Apoprotein B48+C+E+A B48 B100+C+E B100+E B100 B100 AI, AII B100+(a) 10 Major Lipoproteins Dr.Sarma@works 11 Lipoprotein Metabolism • Exogenous – Transport of dietary fats – TG to Adipose tissue, Muscle and Cholesterol to Liver as Chylomicrons • Endogenous – Transport of TG and CE from Liver to the peripheral tissues like muscle, adipose tissues and vascular endothelium via VLDL,IDL, LDL • Reverse Cholesterol transport –HDL Path – from the vessels and periphery to liver Dr.Sarma@works 12 Enzymes 1. Lipo Protein Lipase (LPL) – – – Synthesized in Adipose and Muscle tissues Essential for TG metabol – FFA and Glycerol Insulin activates LPL,- CII apo binds to LPL 2. Hepatic TG Lipase (HGTL) – – Removes TG from VLDL, IDL LDL Clears the Cholesterol remnants into liver – Converts HDL2 to HDL3 in the liver Dr.Sarma@works 13 Enzymes contd.. 3. Lecithin Chol Acyl Transferase (LCAT) • • Secreted into plasma by the liver Binds to HDL and transfers linoleate from lecithin to free Chol and converts it into EC- 4. Cholesterol Ester Transfer Protein (CETP) – – – Secreted into plasma from liver Transfers EC from HDL to VLDL Converts LDL to small Dense LDL Dr.Sarma@works 14 E X O G E N O U S Dr.Sarma@works 15 E N D O G E N O U S Dr.Sarma@works 16 H D L P A T H W A Y Dr.Sarma@works 17 Lipid Peroxidation LDL, IDL Not normally taken up by the vessel wall ROS – Free radicals and Pro-oxidants Oxidized LDL, IDL Freely enters the vessel wall Endothelium Scavenger pathway Foam Cells Macrophages Cytokines, GF Atherosclerosis Dr.Sarma@works 18 Synthesis of VLDL (TG) • In the liver VLDL is synthesized – – – – – – – – It is dependent on substrate flow Obesity Excessive consumption of simple sugars Increased intake of saturated fats Inactivity Alcoholism Insulin resistance Low HDL Dr.Sarma@works 19 Primary Hyperlipidemia Dr.Sarma@works 20 Secondary Hyperlipidemia TG EC Obesity Nephrotic syndrome. Diabetes Hypothyroidism Uraemia Obstr. liver disease Alcoholism Anorexia nervosa Oral contraceptives Acute Int. Porphyria Beta blockers Progestogens Pregnancy Thiazides Steroids, Thiazides Dr.Sarma@works 21 Clinical Action • Presence of secondary causes of Hyperlipidemia – Order for full lipid profile (LP) – HT also • Presence of Hyperlipidemia – increased TG or EC – Investigate for all secondary causes • For all above 20 years once in every 5 years – LP • For those above 45 yrs – once in 2 years • For those with already known lipid abnormality follow-up every 3-6 months Dr.Sarma@works 22 Lipid Profile Report LIPID TYPE TC = 250 TG = 150 LIPOPROTEIN Remarks HDL = 50 N LDL = 170 Abnormal VLDL = 30 N VLDL = 135 N Chylomicron=15 N Dr.Sarma@works 23 LDLc Calculation LDLc = TC – (HDLc + TG/5) e.g. if TC = 250, HDLc = 50, TG = 150 LDLc = 250 – (50 + 150/5) = 250 – (50+30) = 250 – (80) LDLc = 170 Dr.Sarma@works 24 Risk Factors for CHD Dr.Sarma@works 25 Treatment Plan - LDLc Clinical Status Diet Drugs Goal No CHD < 2 RF >160 >190 <160 No CHD 2 or more RF >130 >160 <130 CHD Present >100 >130 <100 Dr.Sarma@works 26 Therapeutic Goals Dr.Sarma@works 27 Cholesterol Levels Dr.Sarma@works 28 Triglycerides TG Level Classification Treatment < 200 mg% Normal TG No Rx. 200 to 400 mg% Borderline high Diet alone 400 to 1000 mg% High Diet + drugs > 1000 mg% Very high Diet + Intensive Rx NCEP Guidelines by expert panel on TG Dr.Sarma@works 29 Diet Regimen Nutrient Step I Step II Total Fats < 30% < 30% Saturated < 10% < 5% PUFA < 10% < 10% MUFA < 10% 15% CHO 55% 55% Protein 15% 15% Cholesterol < 300 mg < 200 mg Dr.Sarma@works 30 Treatment Options • • Diet – Two step approach Drug therapy 1. 2. 3. 4. 5. HMG CoA Reductase Inhibitors Bile Acid binding Resins Nicotinic Acid Fibric Acid derivatives Probucol Dr.Sarma@works 31 HMG CoA Red. Inh. • Called Statins – Atorvastatin, Simvastatin, Lovastatin etc., • 10 mg of Atorvastatin/Simvastatin OD, up to 40mg/day • Synthesis of Cholesterol is blocked by inhibiting the enzyme hydroxy-methyl-Glutaryl Coenzyme A reductase • Increase in LDL receptors – traps LDL from plasma • Decrease in LDL by 25-45%, and VLDL TG by 10-20% • Increase HDL by 8-10%, No action on Lp(a) • Free of side effects - < 5%, Rise in Liver enzymes • Rare but serious complication is myopathy –CPK increase • Caution if combined with Gemfibrozil for combined hyperlipids. Dr.Sarma@works 32 Nicotinic Acid • • • • • • • Decrease the synthesis of VLDL and LDL in liver 50 – 100 mg t.i.d – increase up to 2 to 5g/day Do not use sustained release preparation Decreases TG by 25 to 85%, VLDL by 20-35% Decreases LDL by 10-15%, may increase HDL? Only agent – lowering Lp(a) by 25% Flushing, pruritus, dry skin – tachycardia and atrial arrythmias – hyper uricemia, peptic ulcer disease, glucose intolerance, hepatic dysfunction • Poor side effect profile is the limitation. • Can be combined with resins, fibrates, statins Dr.Sarma@works 33 Anion Resins • • • • • • • • Interrupt the enterohepatic circulation of bile acids Increased synthesis of bile acids–cholesterol sequestration Cholestyramine (Questran) 378g containers or 4g sachets Colestipol (Colestid) in 300g or 500g jars/5g packs/ 1g tab Decrease LDL by 20-30%, Increase HDL and TG Constipation, bloating, nausea, bleeding piles Contra ind. : Biliary obstruction, G.Outlet obst., Incr. TG Can be combined with Nicotinic acid, Statins Dr.Sarma@works 34 Fibric Acid derivatives • • • • • • • • Increase LPL activity – Increased hydrolysis of TG Decrease VLDL synthesis, Increase LDL catabolism Only Gemfibrozil is approved – 600mg b.i.d Decrease TG by 25-40%, LDL may rise, modest rise HDL Adv. Effects -Incr. Bile lithogenicity, abn. LFT, Myositis Contr. In hepatic or biliary disease, caution in renal failure Increase the anti-coagulant action of Warfarin Can be combined with bile acid binding resins Dr.Sarma@works 35 Probucol • Probucol (Lorelco) 500mg b.i.d with food • Third line drug – erratic effect on LDL & decrease of HDL • Lowers Cholesterol and only drug which regresses xanthomas • It is an antioxidant of LDL • Diarrohea, flatulence, nausea, increases QTc • Can be combined with bile acid sequestrating resins Dr.Sarma@works 36 What is for what • If LDLc is more – Hypercholesterilimia alone – – – – – Statins 1st line – Simvastatin – Atorvastatin Statins + Anion resin (Questron)– 2nd line Or Statins + nicotinc acid – 2nd line Probucol 3rd line specially for xanthomas But not Statins + gemfibrozil • If TG alone is elevated – Hypertriglyceridemia – Gemfibrozil – 1st line – Nicotinic acid with or without Gemfibrozil– 2nd line • For mixed – combination- Statin+Nicotinic acid Dr.Sarma@works 37 What’s in a name ? • Statins – Atorvastatin – Storvas, TG-tor, Avastin Simvastatin – Sim, Simvotin • Bile acid sequestering resins – Cholysteramine – Questron – Colistipal – Colestid • Nicotinic Acid – Niasyn • Fibric acid -Gemfibrozil– Lopid, Lipizyl • Probucol – Lorelco Dr.Sarma@works 38 The Research ADMIT Arterial disease multiple intervention trial (Niacin, Anti-oxidants, vitamins) CHAOS Cambridge heart anti-oxidant study MRC/BHF HPS MRC/BHF heart protection study (anti-oxidants) SU.VI.MAX Supplementation en Vitamines et Mineraux Antioxydants CELL Cost Effectiveness of Lipid Lowering (pravastatin) CIS Coronary Intervention Study (simvastatin) HHS Helsinki Heart Study (Gemfibrozil for TG) SSSS (4S) Scandinavian Simvastatin Survival Study (Land mark trial Dr.Sarma@works 39 The Future Research • We do not have yet any drug which increase the HDL • We do not know the precise role of Lp(a) and how to reduce it. • Small LDL needs further evaluation • RCTs to prove that the anti-oxidants have a real role to play both in treatment and in prevention of AVD Dr.Sarma@works 40 Risk Factors for AVD • • • • • Hyperhomocyst(e)inemia Diabetes mellitus Hypertension Dyslipidemia Positive family history, Smoking, obesity and physical inactivity Dr.Sarma@works Oxidative Stress AVD 41 Free Radical Formation Homolytic fission of a covalent bond Single covalent bond A B Homolytic fission Heterolytic fission B A A B Ions Free radicals Dr.Sarma@works 42 ROS damage biological tissues- membranes Reactive Oxygen Species Lipid peroxidation Protein denaturation DNA Damage Free radicals released Cell Dysfunction and death Dr.Sarma@works 43 Classification • Preventive antioxidants -Ceruloplasmin, transferrin, lactoferrin • Enzyme antioxidants -Superoxide dismutase, catalase, glutathione peroxidase • Scavenging or ‘chain-breaking’ or ‘sacrificial’antioxidants -Vitamins A,C, and E Dr.Sarma@works 44 ROS and their Antioxidants ROS Antioxidants O2 Superoxide free radical Superoxide dismutase Vitamin E, -carotene OH Hydroxyl free radical Vitamin C Hydrogen peroxide Glutathione peroxidase Singlet Oxygen Vitamin A, E H2O2 O2 Dr.Sarma@works 45 Reactive Oxygen Species (ROS) Free Radicals Superoxide O2 Hydroxyl OH Non Radicals Hydrogen peroxide H2O2 Singlet oxygen O2 ROS are highly reactive….and can damage biological tissues and membranes Dr.Sarma@works 46 What is Homocysteine ? Protein diet Metabolism Digestion Methionine 1)Homocysteine Auto-oxidation Protein synthesis 2)Homocystine 3) Homocysteine thiolactone HS-CH2-CH2-CH-COOH Generation of ROS NH2 Homocysteine • 1+2+3= homocyst(e)ine • Sulfur-containing amino acid •homocyst(e)ine = tHcy •By product of methionine metabolism •Homocyst(e)inemia=hyper - tHcy Dr.Sarma@works 47 Homocysteine : Metabolic Pathways Remethylation Cycle Diet Tetra hydrofolate Folic acid MTHFR Demethylation Cycle Methionine Vitamin B6 (MS) Methyl tetrahydrofolate MS – Methionine synthase MTHFR – Methyl tetrahydro folate reductase C beta S – Cystathionine beta synthase Homocysteine Cystathionine Vitamin B6 (C beta S) Cysteine Sulphate Glutathione Dr.Sarma@works 48 Hyperhomocyst(e)inemia Blood Homocyst(e)ine Levels Values in mmol/L Classification 05 – 15 16 – 30 31 – 100 > 100 Normal Moderate Intermediate Severe • Moderate to severe hyper – tHcy : established risk factor for AVD 1-4 • Hyper – tHcy - 5-7 % of the general population - 12-47 % of patients with AVD Dr.Sarma@works 49 Causes of Hyperhomocyst(e)inemia A. Nutritional : Vitamin deficiency Folic Acid Vitamin B12 Vitamin B6 B. Genetic : Enzyme Abnormality C. Drugs : Methotrexate, Phenytoin, Theophylline Dr.Sarma@works 50 Homocysteine & Pathogenesis of AVD Homocysteine Auto-oxidation Generation of ROS H2O2 Damages endothelium OH/O2 Lipid peroxidation Exposure of smooth Nitric Oxide formation muscle, subendothelium Vasodilation Proliferation of SM cells, Chemotaxis Hypertension ATHEROSCLEROSIS Dr.Sarma@works Oxidizes LDL Foam cells (chol) 51 New Year Best Wishes We wish you to be blessed always with • BMI of < 25; W/H ratio of 0.80 • FBG of 60 to100 • Blood pressure of about 120/80 • LDLc of <100 • TG of <200 • Normal ECG and Treadmill test All these mean a very healthy and Happy HEART Dr.Sarma@works 52 True ! Eat Drink Indulge Think Be quiet Have high Chol Be high spirited Smoke but not over-eat but not alcohol but not in junk food but not worry but with exercise but not LDL Cholesterol but not be on ‘spirits’ any brand of incense stick, but not cigarettes Dr.Sarma@works 53