* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download COMMON INTOXICATIONS IN KIDS
Survey
Document related concepts
Discovery and development of beta-blockers wikipedia , lookup
Effects of long-term benzodiazepine use wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
Neuropharmacology wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Psychopharmacology wikipedia , lookup
Theralizumab wikipedia , lookup
Transcript
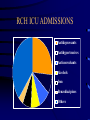
COMMON INTOXICATIONS IN KIDS Blake Bulloch, MD OBJECTIVES • Review new recommendations for GI decontamination • Review the common types of intoxications seen in children with recommendations on non-dialytic detoxifying therapies GI DECONTAMINATION • • • • • Ipecac Gastric Lavage Activated charcoal Cathartics Whole-Bowel irrigation IPECAC • 21% to 38% of drug is removed from the stomach if given in first hour • Average child presents 1.5 hours postingestion, 3.5 hours for adults • No evidence that ipecac improves outcome • Use in the ED should be abandoned GASTRIC LAVAGE • 32% of drug removed if performed 1 hour • In ED studies no difference in outcomes versus charcoal alone • Complication rate of 3% and includes: – aspiration pneumonia – dysrhythmias – hypoxia and hypercapnia / laryngospasm ACTIVATED CHARCOAL • Mean in drug absorption is 89% if given within 30 min and 37% if given at 1 hour • Complications minimal • Insufficient data to support or exclude its use after 1 hour post-ingestion CATHARTICS • Two reasons cited for use of cathartics which are NOT true: – 1) Prevent charcoal induced constipation – 2) Decrease bioavailability of the ingestant • Not recommended for GI decontamination WHOLE-BOWEL IRRIGATION • At 1 hour or longer after ingestion WBI decreases bioavailability 70% • Long procedure and labor-intensive • Limit to poisons not adsorbed by charcoal and to sustained release pharmaceuticals • Should not be used routinely in poisonings RCH POISONINGS (1997-2001) • 2637 ER visits for poisoning • 730 hospital admissions (28%) • 53 ICU admissions – 2% of all poisonings – 7% of all admissions RCH ICU ADMISSIONS Antidepressants Antihypertensives Anticonvulsants Alcohols Iron Benzodiazipines Others TRICYCLIC ANTIDEPRESSANTS PATHOPHYSIOLOGY Most toxic reactions are due to: (1) Anticholinergic effects (2) Excessive blockade of norepinephrine reuptake at the postganglionic synapse (3) Direct quinidine-like effects on the myocardium CLINICAL PRESENTATION • Quinidine-like effects depress myocardial conduction – Prolonged QRS, QT or PR intervals – Torsade de pointes • Ataxia, hallucinations, coma, seizures • Other anticholinergic effects MANAGEMENT • Sodium bicarbonate: – Increases the plasma protein binding of TCAs – May help overcome sodium channel blockade • If hypotensive may consider norepinephrine infusion (0.1-0.3 ug/kg/min) – Less ventricular arrhythmias than with dopamine? CARDIAC DRUGS Beta-Adrenergic Blockers and Calcium Channel Blockers PRESENTATIONS • • • • • • Bradycardia Hypotension Coma Convulsions Hypoglycemia: Beta-blockers Hyperglycemia: Calcium channel blockers MANAGEMENT • Atropine, fluid boluses and pressors to treat bradycardia and hypotension • Glucagon 3-5 mg/kg IV bolus up to 10 mg followed by an infusion of 2-5 mg/h • CCB: 10% Ca gluconate 0.6 ml/kg or 10% Ca chloride 0.2 ml/kg • Pacemaker CARBAMAZEPINE CLINICAL PRESENTATION • • • • • Coma Respiratory depression Seizures Ventricular arrhythmias Other anticholinergic effects (Ileus, hyperthermia, urinary retention) MANAGEMENT • Supportive • Seizures: – Benzodiazepines – Phenobarbital – Not phenytoin. • Charcoal hemoperfusion and hemodialysis have reduced [serum] by 25-50% METHANOL AND ETHYLENE GLYCOL PATHOPHYSIOLOGY • Metabolites cause the poisoning • Ethylene glycol glycoaldehyde glycolic oxalic acids • Methanol formaldehyde formic acid • These cause metabolic acidosis, blindness, and cardiovascular instability TRADITIONAL TREATMENT • Ethanol administration to occupy binding sites on alcohol dehydrogenase and prevent generation of toxic metabolites • Hemodialysis to eliminate parent compound • Sodium bicarbonate to treat metabolic acidosis FOMEPIZOLE • Competitively inhibits alcohol dehydrogenase • Loading dose 15 mg/kg followed by 10 mg/kg q12h for 4 doses then 15 mg/kg q12h • Doses given intravenously over 30 minutes FOMEPIZOLE VS ETOH • Does not require separate preparation • Adverse effects: HA, nausea and vertigo vs altered mental status and hypoglycemia • Hemodialysis still useful IRON PATHOPHYSIOLOGY • Excess iron is directly caustic to the GI mucosa hypovolemia and shock • Free unbound iron: – Increases capillary permeability – Accumulates mainly in the liver and concentrates in mitochondria disrupting oxidative phosphorylation lactic acidosis CLINICAL STAGES • • • • Stage 1: GI phase (within hours) Stage 2: Latent (6 - 24 hours) Stage 3: Shock phase (variable) Stage 4: GI tract scarring (days to weeks) MANAGEMENT • WBI unless ileus, obstruction, perforation or GI hemorrhage • Deferoxamine mesylate is a chelating agent that removes iron from tissues and free iron from plasma • Dose: 15 mg/kg/hour DFO INDICATIONS 1) Symptomatic patients with more than transient minor symptoms 2) Patients with lethargy, abdominal pain, hypovolemia or acidosis 3) Positive AXR 4) Any symptomatic patient with iron level > 300 ug/dl BENZODIAZEPINES PATHOPHYSIOLOGY • Benzodiazepines act on the CNS by potentiating gamma-aminobutyric acid which renders the postsynaptic receptor sites to be less excitable CLINICAL PRESENTATION • Most commonly; ataxia, lethargy and slurred speech • Respiratory depression and coma • Hypotension and hypothermia are rare MANAGEMENT • Flumazenil – Competitive BDZ receptor antagonist • Adult dose is 0.2 mg IV every minute until response achieved (maximum 3 mg) – Literature to support higher doses • Pediatric dose recommendation: – 10 ug/kg for 2 doses SULFONYLUREAS BACKGROUND • Sulfonylureas stimulate insulin secretion which results in hypoglycemia • Most common are glyburide, glipizide and chlorpropamide • Relatively uncommon poisoning but high morbidity and mortality TRADITIONAL TREATMENT • Routine treatments are often ineffective because they stimulate endogenous insulin secretion (dextrose and glucagon) • Corticosteroids are unreliable • Diazoxide (antihypertensive) is an inhibitor of insulin secretion and is effective • Concern exists over possible hypotension OCTREOTIDE • Inhibits the secretion of insulin • Stabilizes blood glucose levels and prevents rebound hypoglycemia • Dose is 50 ug subcutaneously q8-12h • Recommendation: Octreotide to all patients who remain hypoglycemic after a 1 g/kg dose of dextrose ACETAMINOPHEN PATHOPHYSIOLOGY • Metabolized in 3 ways: – Glucuronidation – Sulfation – Via cytochrome P450 pathway to a toxic intermediate that conjugates with glutathione • In OD glutathione becomes depleted MANAGEMENT • GI decontamination • Obtain 4 hour level • N-Acetylcysteine (NAC): – United States: 140 mg/kg P.O. then 70 mg/kg q4h for 17 doses (Total time 72 h) – Everywhere else: I.V. infusion x 3 (Total time: 21 h)