* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Print this article - International Cardiovascular Forum Journal
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Cardiac surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
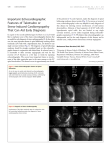
62 | Letters to the Editor International Cardiovascular Forum Journal 5 (2016) DOI: 10.17987/icfj.v5i0.260 Immersion Pulmonary Edema in the Setting of Takotsubo Cardiomyopathy Tara Reed1, Dante Sorrentino,2 Steven Azuma.3 1. University of Hawaii John A. Burns School of Medicine . 2. University of Hawaii Internal Medicine Residency Program. 3.Assistant Clinical Professor University of Hawaii John A. Burns School of Medicine, Kuakini Medical Center, Queens Medical Center Honolulu, HI Corresponding author: Tara Reed, 1241 Rycroft St. #301, Honolulu, HI 96814 Email: [email protected] Keywords: Pulmonary edema; acute coronary syndrome; takotsubo cardiomyopathy; apical ballooning; immersion Citation: Reed T, Sorrentino D, Azuma S. Immersion Pulmonary Edema in the Setting of Takotsubo Cardiomyopathy. International Cardiovascular Forum Journal. 2016;5:62-63. DOI: 10.17987/icfj.v5i0.260 Immersion Pulmonary Edema (IPE) is a unique medical condition being increasingly described in the medical literature as suddenonset pulmonary edema in the setting of scuba diving and/or swimming. We report on three patients with unique presentations of IPE with associated development of Takotsubo cardiomyopathy (TTC). All three cases occurred in Oahu, Hawaii and were seen by the same cardiologist within a span of seven years. Each patient was scuba diving with sudden onset dyspnea with pulmonary edema on chest x-ray. Cardiac catheterization revealed no significant epicardial stenosis or thrombosis. EKGs showed typical evolution of symmetric T wave inversion. Wall motion abnormalities resolved. IPE and TTC may occur together and may be more common than initially thought. Physical and emotional stressors are known to trigger TTC. TTC should be considered as a possible complication of IPE. Initial workup should include EKGs, cardiac enzymes, echocardiogram and, in the appropriate situation, cardiac catheterization. Takotsubo cardiomyopathy (TTC) was first described in Japan in 1991, named for the unique left ventricular morphological features.1,2 Takotsubo is a Japanese word that translates to “octopus pot.” Also known as Apical Ballooning Syndrome and Broken Heart Syndrome, TTC is a type of acquired stress cardiomyopathy. This syndrome is now being increasingly recognized in the literature and the American Heart Association has formally incorporated this disease in the class of acquired cardiomyopathies. Usually seen in perimenopausal or menopausal women, TTC is stimulated by a type of emotional or physical stress.4 Presentation often mimics ST-Elevation Myocardial Infarction, but without significant coronary artery stenosis. Based on retrospective studies, approximately 2% of all patients with suspected acute coronary syndrome were found to have TTC.3,4 There is no consensus on diagnostic criteria for TTC. The Mayo Clinic proposed diagnostic criteria in 2004 and this has been commonly adopted throughout the literature.5 This criterion is used by the International Takotsubo Registry (InterTAK Registry). * Corresponding author. E-mail: [email protected] Scuba divers’ pulmonary edema (SDPE) is a unique medical condition being increasingly described in the medical literature as sudden-onset pulmonary edema in the setting of scuba diving. SDPE is one type of Immersion Pulmonary Edema (IPE), which presents with shortness of breath, tachypnea, fatigue, and cough with frothy white or blood-tinged sputum.6 A 62-year-old Italian-Mexican female was in her normal state of health prior to a dive where she followed appropriate ascent rates of no more than one foot every two seconds (30ft/9m per minute) and made necessary decompression stops. On ascent, she experienced dyspnea and cough. When she reached the surface, she was given an oxygen mask and coughed up white frothy fluid with blood-tinged sputum. There was no aspiration of seawater, chest pain, or palpitations. She initially presented with an oxygen saturation of 82% on nonrebreather oxygen mask. Her lung examination was significant for diffuse bilateral rhonchi. Electrocardiogram showed deep pathologic Q waves in V1, V2, and V3 and T wave inversions in lead I, aVL, and V6. Initial troponin I value was 0.69 ug/L and peaked at 0.84 ug/L. Other significant lab values on admission were Creatine Kinase 523 U/L, Brain Natriuretic Peptide (BNP) 570 ng/L, and mild leukocytosis. Transthoracic echocardiogram (TTE) showed an ejection fraction of 32% and severe global hypokinesis of the left ventricle. She underwent left heart catheterization, selective coronary arteriography, and left ventriculography. There was no evidence of coronary artery disease. There were findings of apical ballooning with hyperkinetic base supportive of TTC (Figure 1). Her ejection fraction at that time was 45% measured by planimetry. The patient was discharged home in stable condition. One month later, she had a repeat TTE. There were no wall motion abnormalities, apical hypokinesis or apical ballooning. Ejection fraction improved to 55%. The next patient is a 60-year-old Caucasian male with no history of coronary artery disease and was in his normal state of health prior to the dive. When he reached the water’s surface, he was dyspneic ISSN: 2410-2636 © Barcaray Publishing International Cardiovascular Forum Journal 5 (2016) DOI: 10.17987/icfj.v5i0.260 a) Letters to the Editor | 63 b) Figure 1. Left heart catheterization was performed. The above ventriculography showed apical ballooning with hyperkinetic base supportive of TCM a) diastole b) systole. and immediately began coughing up brown-tinged foamy sputum. There was no aspiration of seawater, chest pain, or palpitations. The patient led an active lifestyle and had a negative treadmill stress test (12 minutes on Bruce protocol) done two months prior. On admission, his Creatine Kinase-MB (CK-MB) was 4.7 ng/ml, Troponin-I 0.04 ug/L, BNP 137 ng/L. Troponin-I peaked at 0.53 ug/L and CK-MB levels at 8.7 ng/ml. Chest x-ray showed pulmonary edema suggestive of congestive heart failure. Electrocardiogram showed regular sinus rhythm with no ST or T wave changes. TTE showed a severe deterioration of left ventricular ejection fraction to 25% with global hypokinesis in his left chamber with characteristic apical ballooning. Subsequent cardiac catheterization showed an estimated ejection fraction of 60% with mild anterior hypokinesis and no significant coronary artery disease. The patient was discharged the next day in stable condition. The third patient is a 47-year-old Japanese female who ascended per diving protocol and was noted to be hyperventilating. She successfully surfaced, but lost consciousness while boarding the vessel. Oxygen saturation was found to be 88% on room air on arrival to the hospital. On admission, her CK-MB was 39 ng/ml, Troponin-I 0.49 ug/L, BNP 46 ng/L. Troponin-I peaked at 3.49 ug/L. Echocardiogram revealed normal sinus rhythm with mild increase in QTC to 479, left ventricular hypertrophy, 1-mm ST elevations in leads V1, V2, and V3, ST depressions in leads V4, V5, and V6, and T wave inversions in lead V2. Chest x-ray was significant for bilateral mild to moderate infiltrates. TTE showed an ejection fraction of 45% with diminished left ventricular compliance. Left heart cardiac catheterization revealed an anterior and inferior severe hypokinesis with diminished ejection fraction around 45%. There were no significant coronary calcifications found. She was discharged two days after admission in stable condition. The overall prognosis of TTC remains excellent, with a full recovery observed in 96% of cases although serious complications do occur, including ventricular rupture, thrombosis, arrhythmia, and chronic heart failure.8 In all three cases above, the physical stress of acute pulmonary edema likely triggered TTC. SDPE is a unique etiology of acute pulmonary edema discussed in the literature. One study by Coulange et al. examined 22 patients that had IPE with no underlying cardiac disease.7 They found that symptoms of IPE consistently started during the ascent to the water’s surface.7 At six-month followup, all patients were found to have normal respiratory function, echocardiograms, and exercise tolerance tests.7 This case series presents the possibility of TTC induced by IPE without any underlying cardiac disease. All three cases occurred in Oahu, Hawaii and were seen by the same cardiologist within a span of seven years. In this case series, minimal intervention was performed with complete resolution of symptoms and full restoration of cardiac function. IPE and TTC may be more common than initially thought. In the setting of scuba diving, IPE may be the initiating factor of the reversible cardiac dysfunction seen in TTC. TTC should be considered as a possible complication of IPE. Declarations of Interest The authors declare no conflicts of interest. Acknowledgements The authors state that they abide by the “Requirements for Ethical Publishing in Biomedical Journals”.9 References 1. Dote K, Sato H, Tateishi H, Uchida T, Ishihara M. Myocardial stunning due to simultaneous multivessel coronary spasms: a review of 5 cases. J Cardiol. 1991;21(2):203-214. 2. Gianni, M, Dentali F et al. Apical ballooning syndrome or takotsubo cardiomyopathy: a systematic review. Eur Heart J. 2006;27(13):1523–1529. DOI:10.1093/eurheartj/ehl032 3. Parodi G, Del Pace S, Carrabba N, Salvadori C, Memisha G, Simonetti I, Antoniucci D, Gensini GF. Incidence, clinical findings, and outcome of women with left ventricular apical ballooning syndrome. Am J Cardiol. 2007;99(2):182-5. DOI:10.1016/j.amjcard.2006.07.080 4. Eshtehardi P, Koestner SC, Adorjan P, Windecker S, Meier B, Hess OM, Wahl A, Cook S. Transient apical ballooning syndrome--clinical characteristics, ballooning pattern, and long-term follow-up in a Swiss population. Int J Cardiol. 2009;135(3):370-5. DOI:10.1016/j.ijcard.2008.03.088 5. Hurst RT, Prasad A, Askew JW 3rd, Sengupta PP, Tajik AJ. Takotsubo cardiomyopathy: a unique cardiomyopathy with variable ventricular morphology. JACC Cardiovasc Imaging. 2010 Jun;3(6):641-9. DOI:10.1016/j.jcmg.2010.01.009 6. Edmonds C, Lippman J, Lockley S, Wolfers D. Scuba divers’ pulmonary oedema: recurrences and fatalities. Diving Hyperb Med. 2012;42(1):40-4. 7. Elesber AA, Prasad A, Lennon RJ, Wright RS, Lerman A, Rihal CS. Fouryear recurrence rate and prognosis of the apical ballooning syndrome. J Am Coll Cardiol. 2007;50(5):448-52. DOI:10.1016/j.jacc.2007.03.050 8. Sharkey SW, Windenburg DC, Lesser JR, Maron MS, Hauser RG, Lesser JN, Haas TS, Hodges JS, Maron BJ. Natural history and expansive clinical profile of stress (tako-tsubo) cardiomyopathy. J Am Coll Cardiol. 2010;55(4):333-41. DOI:10.1016/j.jacc.2009.08.057 9. Shewan LG, Coats AJS, Henein M. Requirements for ethical publishing in biomedical journals. International Cardiovascular Forum Journal 2015;2:2 DOI: 10.17987/icfj.v2i1.4