* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Dr - Cases Journal
Heart failure wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
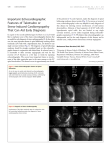
Dr. Rishard Sear Cases Journal Dear Dr. Richard Sear, we have some considerations about your comments. Recently Hahn et al. showed some differences between patients with apical and non apical ballooning; the firth (non apical ballooning syndrome) have cardiogenic shock or pulmonary edema on admission less frequently than the typical apical syndrome; furthermore they suggested that wall motion abnormalities in patients with non apical ballooning resolve more rapidly than in those with apical ballooning. Moreover they showed that atypical transient left ventricular ballooning may develop in patients with fewer coronary risk factors than classic left ventricular apical ballooning. Some authors have reported in the past that vasospasm of the coronary artery caused acute and reversible cardiomiopathy in a few patients (Tsuchihashi et al. J Am Coll Cardiol 2001; Karisu et al Am Heart J 2002). In our case report the total absence of changes of aspect of the right coronary artery at the ostial tract, before and after injection of nitrates, is not in favour of a ostial spasm. Furthermore the hypothesis that the ventricular ballooning syndrome is an expression of an acute myocarditis is not confirmed be the rare cases in which endomyocardial biopsy (Abe et al. J Am Coll Cardiol 2003) and CMR were performed (Sharkey et al. Circulation 2005) As described in the text the apical preponderance of ballooning is not understood. Although myocardial responsiveness to adrenergic stimulation is increased in the apical myocardium, norepinephrine content is lower in the apex than in the base; furthermore heterogeneous nerve distribution exists in the human heart. The apex may not be more vulnerable to cathecolamine excess than mid ventricle, the base or other walls in all patients. Rather, individual variation in the regional myocardial vulnerability may determine the location of regional wall motion abnormality. This evidence can explain the atypical localization of ventricular ballooning. In our case the diagnosis of atypical “tako – tsubo – like” syndrome was based on many factors: sex, age, clinical picture, mild elevation of myocardial markers, ttoal absence of coronary lesions, akinesia of a little district of the left ventricle with absolute normalization after the acute phase. In the cases so far described the absence of coronary artery was defined as “absence of significant angiographic stenosis”; Ibanez et al (Heart 2005) have documented, through an intravascular ultrasound, plaque rupture in a limited number of patients. Finally in the literature we found two cases with atypical ventricular ballooning involving the anterior wall described by Suzuki et al. (Intern Med 2004) after discontinuation of intake of alcohol in a person from ethanol and Mazzarotto et al. (Ital Heart J Suppl 2005) in a young woman. So, according to all these data, we confirm our diagnosis of atypical left ventricular ballooning involving the inferior wall