* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Sample Chapter 36 from Runge: Netter`s Cardiology, 2nd Edition
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Infective endocarditis wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiac surgery wikipedia , lookup
Jatene procedure wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Rheumatic fever wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Aortic stenosis wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
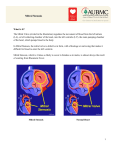
Mitral Valve Disease 36 c00036 Thomas R. Griggs s0010 s0015 itral valve leaflets consist of thin, pliable, fibrous material. The two leaflets—anterior and posterior—open by unfolding against the ventricular wall and close by apposition when the pressure in the left ventricle becomes greater than that in the left atrium. Mitral stenosis occurs when the mitral valve leaflets become stiffened, calcified, and unable to open completely during diastole. This process often involves the chordae tendineae in addition to the mitral valve leaflets. Mitral valve regurgitation occurs when the leaflets are unable to close completely in systole. In the United States, more than 20,000 patients annually require surgery for manifestations of mitral stenosis and mitral regurgitation, and thousands more require monitoring and treatment. Etiology and Pathogenesis Mitral Stenosis p0015 Rheumatic fever is responsible for a majority of cases of mitral stenosis. The initial infection and its sequelae result in thickened valve leaflets and fusion of the commissure between the leaflets. Chordae tendineae are also affected and become thickened, fused, and shortened. Most valves that are affected by rheumatic fever show abnormalities of all these structures. Few patients with rheumatic mitral valve disease have pure mitral stenosis; most have a combination of stenosis and regurgitation, and many have aortic and tricuspid involvement. Approximately two thirds of mitral stenosis cases in the United States occur in women. p0020 The normal mitral valve cross-sectional area in diastole is 4 to 6 cm2. Blood flow is impaired when the valve orifice is narrowed to less than 2 cm2, creating a pressure gradient with exertion. A valve area smaller than 1 cm2 is considered critical mitral stenosis and results in a significant pressure gradient across the valve at rest with chronically increased left atrial (LA) pressures (Fig. 36-1). p0025 Chronically increased LA pressures associated with mitral stenosis, along with ongoing rheumatic inflammation, result in LA enlargement and a predisposition for atrial fibrillation. Valves affected by mitral stenosis are also vulnerable to recurrent thrombosis and implantation of bacteria that lead to infective endocarditis. p0030 The hemodynamic effects of chronic mitral stenosis include pulmonary venous and arterial hypertension; right ventricular (RV) hypertrophy, dilation, and failure; peripheral edema; tricuspid regurgitation; ascites; and hepatic injury with cirrhosis (Fig. 36-2). s0020 Dysfunction of any component of the mitral apparatus can cause mitral regurgitation. Mitral regurgitation also frequently occurs in the absence of primary mitral valve disease in patients with cardiomyopathy and ventricular dilation. When the cause of mitral regurgitation is primarily a valve defect, valve repair or replacement can correct the mitral regurgitation and improve long-term prognosis. When the valve leaks because the ventricle is dysfunctional and dilated, mitral repair or replacement may have little or no effect on symptoms or prognosis. With mitral regurgitation, blood is discharged during systole p0040 into the left atrium in addition to traveling its usual route through the aortic valve and into the aorta. If the regurgitant volume is large, LA remodeling occurs with dilation to accommodate increased volumes without intolerable LA hypertension (Fig. 36-3). Over time, as an increasing fraction of ventricular volume is regurgitant, the “forward” ventricular output is reduced, and symptoms and other findings of mitral regurgitation become obvious (Fig. 36-4). Patients are generally clinically well if the regurgitant fraction (regurgitant volume/total ejection volume) is less than 0.4. Patients with regurgitant fractions greater than 0.5 predictably develop left ventricular (LV) failure and have high morbidity and mortality. Any evidence of LV failure (LV ejection fraction <60%) is also a critical marker of poor prognosis. Infectious endocarditis, spontaneous rupture of chordae ten- p0045 dineae, or ischemic injury of a papillary muscle may cause acute loss of mitral valve integrity and acute mitral regurgitation. In these cases of abruptly increased regurgitant flow, because there is no adaptation of the left atrium or pulmonary vasculature to the increased regurgitant volumes, acute pulmonary edema may suddenly occur. Aggressive use of vasodilators is the emergent treatment, but survival usually depends on emergency repair or replacement of the valve. AL M PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N p0010 Mitral Regurgitation p0035 Numerous etiologies contribute to mitral regurgitation, includ- ing mitral valve prolapse, rheumatic heart disease, bacterial or fungal endocarditis, and certain collagen-vascular diseases. Clinical Presentation s0025 Mitral Stenosis s0030 2 Patients notice the effects of moderate (valve area = 1–2 cm ) p0050 mitral stenosis with activity. With severe stenosis, dyspnea with minimal exertion and paroxysmal nocturnal dyspnea may occur. In some cases a sudden, dramatic onset of atrial fibrillation produces the first symptoms, occasionally resulting in fatal pulmonary edema. When the development of atrial fibrillation is clinically silent, the initial event may be a stroke or other thromboembolic event. The classic presentation of severe cor pulmonale with ascites and edema is rarely seen today except in medically underserved populations. Mitral valve disease increases the risk for bacterial endocarditis, which should always be considered when symptoms worsen in a previously stable patient with mitral valve disease. Auscultatory findings in a patient with mitral stenosis include p0055 a loud first heart sound, an opening snap after the second heart ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 305 2/26/2010 2:49:04 PM T1 306 SECTION V • Valvular Heart Disease RV LV AO LA AL PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N Mitral stenosis, viewed from below and left: Minor rheumatic involvement of aortic valve Echocardiogram demonstrating mitral stenosis. Valve located between LA and LV is thickened, with reduced orifice and intense signal due to excessive calcium. Thickened stenotic mitral valve: Anterior cusp has typical convexity; enlarged left atrium; “jet lesion” on left ventricular wall Enlargement of right ventricle with some thickening of wall resulting from mitral stenosis; pulmonary artery enlarged and thickened with scattered plaques of atheromas Thickened, calcified, stenotic mitral valve demonstrated in echocardiographic study above RV LV AO LA f0010 Figure 36-1 Mitral stenosis. AO, aorta; LA, left atrium; LV, left ventricle; RV, right ventricle. T1 sound, and a low-pitched diastolic murmur with presystolic accentuation if the patient is in sinus rhythm. The opening snap is the sound generated by sudden full opening of the mitral valve. It reflects the severity of the pressure gradient across the mitral valve, because greater LA pressures generate earlier opening than do lesser ones. Therefore, the shorter the interval from second heart sound to opening snap, the greater the pressure gradient, and the more severe the stenosis. p0060 The characteristic diastolic, low-frequency “rumble” or murmur associated with mitral stenosis is best heard at the apex with the patient in the left lateral decubitus position and the bell over the point of maximal ventricular intensity. The rumble occurs throughout diastole, with accentuation in late diastole (presystole) in patients who have preserved normal sinus rhythm. This murmur can be difficult to hear, and is soft and brief when the stenosis is minor. Therefore, heightened awareness of possible mitral stenosis is necessary. If the murmur is inaudible, it can be accentuated by having the patient exercise before auscultation or perform maneuvers such as isometric handgrip. This murmur sequence—loud first sound, opening snap, and diastolic rumble—is specific for mitral stenosis. Murmurs that mimic mitral stenosis include the Austin Flint murmur with aortic regurgitation, mitral diastolic murmurs in patients with large intracardiac shunts, and occasionally murmurs that are caused by an LA myxoma. However, none have all three components of classic mitral stenosis. Electrocardiographic changes in mitral stenosis may range p0065 from minor ST-segment and T-wave abnormalities to electrocardiographic evidence of severe pulmonary hypertension and RV enlargement. The ECG pattern of LA and RV enlargement is a classic indicator. Atrial fibrillation is common. Mitral Regurgitation s0035 Mitral regurgitation following sudden catastrophic failure of the p0070 valve apparatus is almost always immediately and severely symptomatic. In this situation, the regurgitant volume competes for systemic blood flow and is simultaneously filling a small, noncompliant left atrium. This results in pulmonary edema often coupled with hypotension or shock. The physical examination will reflect the respiratory distress and evidence of poor systemic perfusion such as tachycardia, cool extremities, and diaphoresis. Importantly, however, the cardiac examination may not be helpful. Any systolic murmur may be difficult to hear or be absent. Emergent diagnosis usually requires echocardiography. Conversely, even severe chronic mitral regurgitation may be p0075 tolerated without symptoms for years. Many cases of chronic mitral regurgitation are discovered during routine examinations ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 306 2/26/2010 2:49:04 PM CHAPTER 36 • Mitral Valve Disease 307 Dyspnea Elevated “wedge” pressure Hemoptysis Pulm. arteriolar constriction and/or sclerosis Elevated pulm.-artery pressure Elevated pulm. venous pressure Pulmonary congestion Elevated left atrial pressure Edema Pulmonary atherosclerosis Parasternal lift Pulmonary fibrosis I Sounds II R. ventricle dilated Fibrillation frequently L. atrium enlarged Opening snap Thrombosis (embolism) I Hypertrophy Failure Diminished left ventricular filling Liver enlarged, tender AL Diastolic–presystolic rumbling murmur 4th. L. interspace Fixed leftheart output PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N Gradient (Ascites) Left ventricular pressure (Portal hypertension) Elevated venous Edema pressure Portal circulation Systemic circulation Slight cyanosis aVR I V1 R V2 V3 V5 V6 S II aVL V4 III aVF S Left atrial abnormality (P “mitral”) and evidence of right ventricular hypertrophy (S in leads I and V5, R in V1) Atrial fibrillation Figure 36-2 Pathophysiology and clinical aspects of mitral stenosis. when the characteristic holosystolic murmur is noticed. Symptoms usually begin as dyspnea on exertion. Patients may also present with acute pulmonary edema or evidence of RV failure. Sudden decompensation can occur with the onset of atrial fibrillation or the development of bacterial endocarditis. p0080 With chronic mitral regurgitation, the precordial cardiac impulse may be normal or may show a displaced, sustained LV impulse with a rapid filling wave. On auscultation the most prominent feature is a holosystolic murmur that classically radiates to the axilla. The intensity may not correlate with the severity of the mitral regurgitation; even severe mitral regurgitation can be associated with virtually no murmur. ECG changes in mitral regurgitation are nonspecific and are primarily changes of LV hypertrophy and strain; atrial fibrillation is common. Differential Diagnosis f0015 s0040 Primary pulmonary diseases (pneumonia, tuberculosis, chronic p0085 obstructive lung disease, and pulmonary thromboembolism) may present similarly to mitral valve disease, with dyspnea on exertion or pulmonary edema. Dyspnea may also be present in chronic interstitial pulmonary diseases, pulmonary hypertension, and malignancies that involve the chest. Other cardiovascular conditions that present similarly include ischemic heart disease, congenital heart disease, dilated cardiomyopathy, and hypertrophic cardiomyopathy. Chronic pericardial disease with restriction can cause RV failure that mimics the pulmonary hypertension associated with mitral valve disease. ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 307 2/26/2010 2:49:05 PM T1 308 SECTION V • Valvular Heart Disease Mitral regurgitation: Mitral valve viewed from below; marked shortening of posterior cusp, with only slight commissural fusion, and little fusion and shortening of chordae tendineae RV AO LV LA AL Color Doppler study demonstrating systolic aortic outflow (blue/red) and multicolored jet of regurgitant flow through incompetent mitral valve into LA PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N In time, left ventricle dilates to accommodate increased volume. Shortened, thickened mitral cusps Systolic aortic outflow Left atrial enlargement due to mitral regurgitation RV Regurgitant jet through incompetent mitral valve Calcific plate at anterolateral commissure of mitral valve, contributing to insufficiency LV Diagram of mitral regurgitation shown in Doppler color study above AO LA f0020 Figure 36-3 Mitral regurgitation. AO, aorta; LA, left atrium; LV, left ventricle; RV, right ventricle. s0045 Diagnostic Approach p0090 Many pulmonary diseases can be differentiated from mitral T1 valve disease by means of chest imaging, including both radiography and CT scanning. When an initial evaluation has focused the differential diagnosis on mitral valve disease, the most helpful clinical tool is echocardiography (see also Chapter 6). p0095 In rheumatic mitral valve disease, echocardiography can demonstrate thickening, calcification, poor valve mobility, and thickening of subvalvular structures. The degree of valvular stenosis or regurgitation can be estimated using Doppler ultrasonography. When necessary, the anatomy of the valve and subvalvular apparatus can be further defined by transesophageal echocardiography. The goals of echocardiography are to evaluate the severity of the stenosis or regurgitation, the mobility of the valve, the involvement of subvalvular structures, and the degree of calcification, as well as to detect intracardiac thrombi. Echocardiography provides information about LV contractile function and an accurate estimation of pulmonary artery pressure and RV function. It can also identify bacterial and fungal vegetations, intracardiac masses (especially LA myxoma), and intraventricular septal defects, conditions that can complicate diagnosis of mitral valve disease. p0100 Cardiac catheterization is indicated when there is a questionable diagnosis, when clinical and echocardiographic findings are inconsistent, and in many patients for whom surgical treatment is contemplated. Catheterization is performed to quantify the mitral valve area, to document key elements of hemodynamics such as cardiac output and systemic resistance, to define the degree of pulmonary hypertension, and to determine whether coronary artery disease is also present. Management and Therapy s0050 Mitral Stenosis s0055 Asymptomatic patients in normal sinus rhythm with mild, p0105 uncomplicated mitral stenosis require only periodic monitoring for symptoms and prophylaxis against rheumatic fever. In symptomatic patients, diuretics can help reduce pulmonary congestion. With mitral stenosis, ventricular filling time is critically important; the heart rate should be maintained as low as is practical with a β-blocker or a rate-affecting calcium channel blocker. Patients with atrial fibrillation must be treated with warfarin anticoagulation, unless it is contraindicated. Optimum Treatment s0060 Symptomatic mitral stenosis can be improved by percutaneous p0110 mitral balloon valvotomy (PMBV), surgical valvotomy, or ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 308 2/26/2010 2:49:05 PM CHAPTER 36 • Mitral Valve Disease 309 Elevated pulm. vein pressure Dyspnea Elevated “wedge” pressure Systolic regurgitation Pulmonary arteriolar constriction Pulmonary Pulmonary artery dilated; pressure elevated Diminished left heart output Edema Right ventricle slightly enlarged I Sounds II III Soft, blowing pansystolic murmur at apex L. ventricular pressure PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N Left Lifting ventricle apex dilated beat L. atrial pressure AL Failure L. atrium enlarged (fibrillation common) I Hypertrophy Failure Portal circulation Systemic circulation S R Left and right ventricular enlargement Electrocardiographic evidence of L. ventricular hypertrophy (large S in V1, large R in V4) and minor atrial abnormality (broad P) Figure 36-4 Pathophysiology and clinical aspects of mitral regurgitation. surgical replacement of the mitral valve. PMBV is the treatment of choice in selected patients in whom there is little valvular calcification, little involvement of the subvalvular apparatus, and minimal or no mitral valve regurgitation. It is essential to exclude LA thrombi by transesophageal echocardiography in patients being considered for PMBV. The results of PMBV depend in great part on operator experience. Longitudinal studies in expert centers have documented event-free survival to be greater than 70% at 7 years. p0115 Open valvotomy is a repair procedure that involves direct visualization of the valve by the surgeon and facilitates debridement of valve structure and reconstruction of subvalvular apparatus. This approach also permits valve replacement per the surgeon’s judgment. Mitral valve replacement is indicated for patients with severe mitral stenosis who are not candidates for f0025 percutaneous commissurotomy or surgical repair (Tables 36-1, 36-2, and 36-3) (see Chapter 41). Avoiding Treatment Errors s0065 Many patients unknowingly minimize mitral stenosis symptoms p0555 by adopting a sedentary lifestyle. This situation may be suspected following a careful history and documented with exercise testing. These patients may benefit greatly from PMBV. Alternatively, patients may report severe symptoms despite echocardiographic data suggesting mild mitral stenosis. Exercise testing with simultaneous echocardiography or catheterization is indicated in this situation and may disclose dramatic worsening of atrial and pulmonary hypertension and the need for intervention. ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 309 2/26/2010 2:49:06 PM T1 310 SECTION V • Valvular Heart Disease Table 36-1 Management Approach for Patients with Asymptomatic Mitral Stenosis Yearly Follow-up Consider Percutaneous Mitral Balloon Valvotomy Mild stenosis (MVA >1.5 cm ) or MVA <1.5 cm2 but valve morphology not favorable for PMBV 2 Moderate or severe stenosis (MVA <1.5 cm2) and Pulmonary artery systolic pressure >50 mm Hg or Exercise test results: Pulmonary artery pressure >60 mm Hg Pulmonary artery wedge pressure >25 mm Hg or New-onset atrial fibrillation and No LA thrombus or significant mitral regurgitation (3+ or 4+) AL Asymptomatic t0010 p0560 PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N LA, left atrial; MVA, mitral valve area; PMBV, percutaneous mitral balloon valvotomy. Recommendations are from Bonow RO, Carabello B, Chatterjee K, et al. Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients With Valvular Heart Disease). J Am Coll Cardiol. 2008;52:1–142. Rheumatic fever can affect all heart valves. Therefore, multiple valve disease must be considered in all patients. Special attention should be given to the possibility that echocardiography can underestimate the degree of aortic regurgitation in patients with severe mitral stenosis. Tricuspid stenosis may be similarly underestimated or even undetected and may complicate the immediate postoperative recovery after mitral valve repair or replacement. Atrial fibrillation is a frequent cause of decompensation in p0565 patients with mitral stenosis and must be anticipated and Table 36-2 Management Approach for Patients with Symptomatic Mitral Stenosis Mildly symptomatic (NYHA class II) Moderately to severely symptomatic (NYHA class III–IV) T1 t0015 Consider Open Valvotomy or Mitral Valve Replacement Periodic Follow-up Consider PMBV Mild stenosis (MVA >1.5 cm2) and Exercise test results: PASP <60 mm Hg PAWP <25 mm Hg MVG <15 mm Hg or Valve morphology not favorable for PMBV Mild stenosis (MVA >1.5 cm2) and Exercise test results: PASP >60 mm Hg PAWP >25 mm Hg MVG >15 mm Hg and Valve morphology favorable for PMBV and No LA thrombus or significant mitral regurgitation (3+ to 4+) Moderate or severe stenosis (MVA <1.5 cm2) and Valve morphology favorable for PMBV and No LA thrombus or significant mitral regurgitation (3+ to 4+) Moderate or severe stenosis (MVA <1.5 cm2) and Valve morphology not favorable for PMBV and Pulmonary pressure >60–80 mm Hg Moderate or severe stenosis (MVA <1.5 cm2) and Valve morphology favorable for PMBV or High-risk surgical candidate with less than favorable morphology for PMBV and No LA thrombus or significant mitral regurgitation (3+ to 4+) Moderate or severe stenosis (MVA <1.5 cm2) and Valve morphology not favorable for PMBV and Acceptable surgical risk Moderate or severe stenosis (MVA <1.5 cm2) and Valve morphology not favorable for PMBV and Pulmonary pressure <60 mm Hg Mild stenosis (MVA >1.5 cm2) and Exercise test results: PASP <60 mm Hg PAWP <25 mm Hg MVG <15 mm Hg LA, left atrial; MVA, mitral valve area; MVG, mitral valve gradient; NYHA, New York Heart Association; PASP, pulmonary artery systolic pressure; PAWP, pulmonary artery wedge pressure; PMBV, percutaneous mitral balloon valvotomy. Recommendations are from Bonow RO, Carabello B, Chatterjee K, et al. Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients With Valvular Heart Disease). J Am Coll Cardiol. 2008;52:1–142. ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 310 2/26/2010 2:49:06 PM CHAPTER 36 • Mitral Valve Disease 311 Table 36-3 Management Approach for Patients with Chronic Severe Mitral Regurgitation No subjective symptoms and no suggestion of symptoms by exercise testing Mitral Valve Replacement LV dysfunction (EF <60%, ESD >40 mm) or Pulmonary hypertension or New-onset atrial fibrillation LV dysfunction (EF <60%, ESD >40 mm) and Mitral valve repair not possible EF >30% ESD <55 mm Intervention indicated but mitral valve repair not possible PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N Symptoms Normal LV function (EF >60% and ESD <40 mm) and No new-onset atrial fibrillation and No pulmonary hypertension and Mitral valve repair unlikely* Severe LV dysfunction (EF <30% and/or ESD >55 mm) and Chordal preservation not likely Mitral Valve Repair AL Follow-up with Echo Every 6 Months or Medical Therapy t0020 EF, ejection fraction; ESD, end-systolic dimension of the left ventricular chamber; LV, left ventricular. *Mitral valve repair may be an option for asymptomatic patients with normal LV function in an experienced center. Recommendations are from Bonow RO, Carabello B, Chatterjee K, et al. Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients With Valvular Heart Disease). J Am Coll Cardiol. 2008;52:1–142. managed aggressively. Similarly, pregnancy increases requirements for cardiac output and requires special planning and management. In women with rheumatic or congenital mitral stenosis, initial symptoms often manifest with pregnancy. Bacterial endocarditis should be considered whenever symptoms worsen in patients with mitral stenosis. s0070 Mitral Regurgitation p0570 Primary mitral regurgitation is a structural problem causing valve incompetency that can only be corrected adequately by valve repair or replacement. Therefore, the physician’s primary role is to monitor patients with mitral regurgitation for development of symptoms and evidence of LV dysfunction, events that portend the need for intervention. The most promising medical therapies for chronic mitral regurgitation, vasodilators and β-blockers, have not been adequately documented to delay the need for surgery and thus are not recommended for this purpose alone. Aggressive treatment of hypertension is useful in patients with chronic mitral regurgitation. s0075 Optimum Treatment p0575 The timing of surgical intervention for patients with chronic mitral regurgitation is critical. In most cases, mitral regurgitation is well tolerated, and patients are asymptomatic for many years. Delaying surgery as long as possible avoids the trauma, expense, and risk of surgery. However, every effort must be made to proceed with surgery before ventricular function has degenerated. LV systolic function is estimated using one of several methods for determining the LV ejection fraction. The unique accommodating effects of ventricular dilation and myocardial remodeling with chronic mitral regurgitation allow the ejection fraction to be preserved late into the disease course; therefore, any decrement in ejection fraction may represent a considerable decrease in myocardial functional reserve. In general, mitral valve surgery should be considered in patients with known moderate to severe mitral regurgitation when they are symptomatic or there is objective evidence of decreased LV function (LV ejection fraction <60%). Valve repair for severe mitral regurgitation lessens mortality p0580 and decreases the frequency of complications. Valves must be relatively free of calcification and have pliable leaflets with chordae tendineae that can be separated, reinforced, or reattached as needed. Placement of a reinforcing mitral ring is frequently included in the repair. Valve repair, as opposed to replacement, preserves functional subvalvular components, including the papillary muscles, and significantly improves postoperative LV function. Additionally, natural valves are resistant to thrombus formation, obviating the need for long-term anticoagulation. Avoiding Treatment Errors s0080 Mitral regurgitation resulting from dilated cardiomyopathy is p0585 caused by dilation of the mitral ring and ventricles with anatomic deformity of the spatial and functional relationship of the papillary muscles and chordae tendineae to the mitral valve leaflets. In severe LV dysfunction, mitral valve repair or replacement may fail to improve symptoms and is associated with a high risk of operative death. New surgical and percutaneous approaches for correction of mitral regurgitation in this circumstance are in clinical trials to determine safety and efficacy. Coronary heart disease can cause mitral regurgitation by p0590 several mechanisms. The mitral valve is tethered to papillary muscles that depend on myocardial blood flow. Acute ischemia of the papillary muscles can cause temporary mitral regurgitation and be corrected with coronary vascular interventions, either surgical or percutaneous. Acute myocardial infarction that involves a papillary muscle frequently causes acute, lifethreatening mitral regurgitation, with mortality rates near 30%. These are managed, usually surgically, with both repair of the valve and subvalvular apparatus and simultaneous revascularization. In some circumstances, an infarction results in rupture of the tip of the papillary muscle with acute mitral regurgitation. This is almost always fatal unless surgically corrected. ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 311 2/26/2010 2:49:06 PM T1 312 SECTION V • Valvular Heart Disease Bacterial vegetations first appear along “contact line” of mitral valve but spread to involve atria and chordae tendineae with subsequent rupture and shrinkage of the latter. Bacterial perforation of anterior mitral cusp AL Perforation of aortic valve cusp PR SA O M PE PL R E TY C O O F N E TE L N SE T V - N IE O R T FI N Thickening and erosion of mitral valve with stumps of ruptured chordae tendineae resulting in valvular incompetence, regurgitation, and atrial enlargement Valve adhesion to ventricular wall Acute Chronic Left ventricular hypertrophy Late sequelae of bacterial endocarditis may result in mitral regurgitation via destruction of mitral valve cusps or by widening of annular valve ring due to left ventricular enlargement due to aortic insufficiency Vegetations of bacterial endocarditis on underside as well as atrial surface of mitral valve Adhesion of mitral valve cusp to ventricular wall resulting from vegetations on undersurface of valve f0030 Figure 36-5 Bacterial endocarditis in mitral valvular disease. p0595 s0085 Any structural abnormality of the valve can result in flow aberrations that promote deposition of microthrombi. These can be the nidus for a bacterial or fungal infection resulting in further damage from endocarditis (Fig. 36-5). Endocarditis can affect valve competency because of interference in valve function by vegetations or by destruction or fenestration of the valve leaflets. Although endocarditis is usually managed with antibiotics, the damage effected by the bacteria is permanent, as is the resultant mitral regurgitation. Indications for surgery after cured bacterial endocarditis are identical to those for other causes for mitral regurgitation. In addition, acute surgical care is indicated for extremely large vegetations, when heart failure is otherwise unmanageable, when a myocardial abscess is documented, and for patients with persistent bacteremia. Future Directions p0600 Improving worldwide morbidity and mortality associated with T1 rheumatic heart disease necessitates better systems of hygiene and improved prophylactic treatment of streptococcal infection, especially the current drug-resistant strains. Mitral regurgitation’s prevalence will increase as the population ages, spurring improvements in several areas: imaging with more accurate estimates of ventricular reserve, surgical technology with early repair of severely regurgitant valves, balloon valvotomy with improved patient selection and equipment, and minimally invasive surgical techniques with reduced recovery time and morbidity. Better treatment for atrial fibrillation and improved therapies for prevention of thrombosis will greatly improve the quality of life for patients with mitral valve disease and valve prostheses. Additional Resources Carabello BA. Modern management of mitral stenosis. Circulation. 2005; 112:432–437. Carabello BA. The current therapy for mitral regurgitation. J Am Coll Cardiol. 2008;52:319–326. State-of-the-art reviews by a noted expert. p0605 Evidence Bonow RO, Carabello B, Chatterjee K, et al. 2008 Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients With Valvular Heart Disease). J Am Coll Cardiol. 2008;52:1–142. In this recently updated report from a panel of experts assembled by the ACC and AHA, the authors cite more than 1000 articles and provide a comprehensive review of the diagnosis and management of valvular heart disease. Tables and algorithms provide easy access to the practical aspects of patient care. p0610 ISBN: 978-1-4377-0637-6; PII: B978-1-4377-0637-6.00036-2; Author: Runge & Stouffer & Patterson; 00036 http://www.us.elsevierhealth.com/Netter/Netter-Clinical-Specialties/book/9781437706376/Netters-Cardiology Runge_Chapter 36_main.indd 312 2/26/2010 2:49:07 PM