* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Acute hibernation decreases myocardial pyruvate carboxylation and
Cryobiology wikipedia , lookup
Adenosine triphosphate wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Biochemistry wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Lactate dehydrogenase wikipedia , lookup
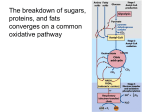
Am J Physiol Heart Circ Physiol 281: H1613–H1620, 2001. Acute hibernation decreases myocardial pyruvate carboxylation and citrate release ASHISH R. PANCHAL,1 BLANDINE COMTE,2 HAZEL HUANG,1 BASIL DUDAR,1 BRIDGETTE ROTH,1 MARGARET CHANDLER,1 CHRISTINE DES ROSIERS,3 HENRI BRUNENGRABER,2 AND WILLIAM C. STANLEY1,2 Departments of 1Physiology and Biophysics and 2Nutrition, Case Western Reserve University, Cleveland, Ohio 44106-4970; and 3Department of Nutrition, University of Montreal, Montreal, Quebec H3C 3Y7, Canada Received 3 April 2001; accepted in final form 25 May 2001 THE HIBERNATING MYOCARDIUM is defined by reversible myocardial contractile dysfunction due to reduced coronary flow and decreased oxygen supply to the myocardium (26). The hallmarks of hibernation are the retention of viable myocardial tissue with residual mitochondrial functions such as pyruvate and fatty acid oxidation, electron-transport-chain flux, and oxidative phosphorylation to generate ATP (1, 29). Little is known about the function of the citric acid cycle (CAC) in myocardium during hibernation. Ischemia in isolated perfused rat hearts causes an increase in the net efflux of the CAC intermediate succinate (15, 24, 25). Although this suggests a net loss of CAC intermediates during ischemia, it is not clear whether ischemia results in depletion of the pool of CAC intermediates (11, 15, 24). The tissue content of CAC intermediates is small compared with the flux through the cycle, and loss of CAC intermediates from the cycle must be balanced by the entry of intermediates into the CAC if the pool size is to be maintained (see Fig. 1). With normal myocardial blood flow, the loss of CAC intermediates is balanced by the entry of newly synthesized intermediates into the cycle; this process is termed anaplerosis (7, 8, 11, 14, 21). The effects of acute myocardial hibernation on the rate of anaplerosis and the tissue content of CAC intermediates are not known. Pyruvate carboxylation is a major anaplerotic pathway in normal myocardium in vivo (21) and generates malate and oxaloacetate (OAA) via malic enzyme and pyruvate carboxylase, respectively (2, 8, 23, 35, 36) (see Fig. 1). We recently developed a method to measure in the heart of anesthetized swine the rate of pyruvate carboxylation and decarboxylation using [U-13C3]lactate and [U-13C3]pyruvate tracers and mass isotopomer analysis of tissue pyruvate and citrate (21). In isolated rat hearts and in vivo swine myocardium, we found that pyruvate carboxylation accounted for 2.5–8% of the citrate synthase flux (7, 8, 21, 39). We also found that the rate of pyruvate carboxylation was not significantly altered when the rate of pyruvate decarboxylation (i.e., flux through pyruvate dehydrogenase) was inhibited by ⬎90% by infusion of octanoate. Thus constitutive pyruvate carboxylation appears to be essential for normal cardiac function as was demonstrated in isolated working rat hearts where there was a dramatic fall in ventricular power when pyruvate carboxylation was pharmacologically inhibited (28). Constitutive pyruvate carboxylation balances the loss of CAC intermediates (11, 15, 21, 39) including citrate (21, 39). Under aerobic conditions, citrate efflux from rat, swine, and human hearts ranges from 5 to 20 nmol䡠g⫺1 䡠min⫺1 (21, 38, 39). Net citrate Address for reprint requests and other correspondence: W. C. Stanley, Dept. of Physiology and Biophysics, School of Medicine, Case Western Reserve Univ., 10900 Euclid Ave. Cleveland, OH 44106-4970 (E-mail: [email protected]). The costs of publication of this article were defrayed in part by the payment of page charges. The article must therefore be hereby marked ‘‘advertisement’’ in accordance with 18 U.S.C. Section 1734 solely to indicate this fact. cardiac; citric acid cycle; dehydrogenase; metabolism; ischemia http://www.ajpheart.org 0363-6135/01 $5.00 Copyright © 2001 the American Physiological Society H1613 Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 Panchal, Ashish R., Blandine Comte, Hazel Huang, Basil Dudar, Bridgette Roth, Margaret Chandler, Christine Des Rosiers, Henri Brunengraber, and William C. Stanley. Acute hibernation decreases myocardial pyruvate carboxylation and citrate release. Am J Physiol Heart Circ Physiol 281: H1613–H1620, 2001.—In the wellperfused heart, pyruvate carboxylation accounts for 3–6% of the citric acid cycle (CAC) flux, and CAC carbon is lost via citrate release. We investigated the effects of an acute reduction in coronary flow on these processes and on the tissue content of CAC intermediates. Measurements were made in an open-chest anesthetized swine model. Left anterior descending coronary artery blood flow was controlled by a extracorporeal perfusion circuit, and flow was decreased by 40% for 80 min to induce myocardial hibernation (n ⫽ 8). An intracoronary infusion of [U-13C3]lactate and [U-13C3]pyruvate was given to measure the entry of pyruvate into the CAC through pyruvate carboxylation from the 13C-labeled isotopomers of CAC intermediates. Compared with normal coronary flow, myocardial hibernation resulted in parallel decreases of 65% and 79% in pyruvate carboxylation and net citrate release by the myocardium, respectively, and maintenance of the CAC intermediate content. Elevation of the arterial pyruvate concentration by 1 mM had no effect. Thus a 40% decrease in coronary blood flow resulted in a concomitant decrease in pyruvate carboxylation and citrate release as well as maintenance of the CAC intermediates. H1614 PYRUVATE CARBOXYLATION IN MYOCARDIUM DURING HIBERNATION Fig. 1. Scheme of the incorporation of pyruvate into the citric acid cycle (CAC) via pyruvate carboxylation and decarboxylation. Arrows going toward the CAC are anaplerotic fluxes (feeding in); arrows going out are CAC intermediate release. MATERIALS AND METHODS Chemicals. Chemicals, enzymes, and coenzymes were purchased from Boehringer Mannheim (Indianapolis, IN) and Sigma-Aldrich (Milwaukee, WI). [2H6]succinic acid, [U-13C3] lactate, and [U-13C3]pyruvate were obtained from Isotec (Miamisburg, OH). The derivatization agent N-methyl-N-(tert-butyldimethylsilyl)trifluoroacetamide was supplied by Regis AJP-Heart Circ Physiol • VOL Chemical (Morton Grove, IL). Intralipid solution was obtained from Baxter Healthcare (Deerfield, IL). Experimental model. A previously described in vivo technique was used to deliver 13C-labeled substrates directly into the left anterior descending (LAD) coronary artery of swine (31, 32). Overnight-fasted domestic swine (weight 27–38 kg) of either sex were sedated with Telazol (6 mg/kg im), anesthetized with pentobarbital sodium (25 mg/kg ⫹ 5 mg 䡠 kg⫺1 䡠 h⫺1 iv), intubated via a tracheotomy, and ventilated to maintain arterial blood gas values in the normal range (PO2 ⬎ 100 mmHg, PCO2 of 35–45 mmHg, and pH of 7.35–7.45). A 7-Fr high-fidelity pressure transducer catheter (Millar; Houston, TX) was positioned in the left ventricle via the carotid artery. The animal was then heparinized (300 U/kg bolus ⫹ 150 U 䡠 kg⫺1 䡠 h⫺1 iv) and infused with a 20% triglyceride emulsion (Intralipid 20%, 0.3 ml 䡠 kg⫺1 䡠 h⫺1 iv) to increase plasma free fatty acids (FFA) to 0.6 mM (32). Coronary blood flow in the anterior wall was controlled by an extracorporeal circuit as previously described (31, 32). The anterior interventricular vein was cannulated to collect venous blood samples from the perfusion territory of the LAD. The coronary perfusion pump flow was adjusted to give an interventricular venous Hb saturation of 35–40% (31, 32). Experimental protocols. Pigs were subjected to acute myocardial hibernation induced by decreasing the blood flow to the LAD bed by 40% (see Fig. 2). Pyruvate carboxylation and decarboxylation were measured with an intracoronary infusion of [U-13C3]lactate and/or [U-13C3]pyruvate for 60 min, with subsequent analysis of myocardial tissue for 13C isotopomers of pyruvate and CAC intermediates by gas chromatography-mass spectrometry (GC-MS) as previously described (21). Stock solutions of 99% [U-13C3]lactate and/or 99% [U-13C3]pyruvate were directly infused into the LAD perfusion circuit at a rate of 6.5 l/ml of LAD blood flow (see Fig. 2). Pyruvate carboxylation was measured in hibernating myocardium under either near-normal arterial lactate and pyruvate concentrations (HIB group, n ⫽ 8), or with elevated arterial pyruvate concentration (HIB ⫹ PYR group, n ⫽ 8). In HIB animals, the concentrations of [U-13C3]lactate and [U-13C3]pyruvate in the infusate were 154 and 15.4 mM, respectively, so that the lactate and pyruvate concentrations 281 • OCTOBER 2001 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 efflux from swine myocardium amounts to ⬃20% of the rate of pyruvate carboxylation (21). The extent of pyruvate carboxylation and citrate efflux in the hibernating or ischemic myocardium is not known. Opie (20) reported a 33% decrease in myocardial citrate content after 30 min of severe ischemia (an ⬃90% reduction in flow) in dogs; however, the actual rate of citrate efflux from the heart was not measured. Evidence for a role of CAC intermediate depletion in postischemic cardiac dysfunction was suggested by improved postischemic functional recovery when anaplerotic substrates (pyruvate, glutamate, or propionate) were administered to isolated rodent hearts (4, 6, 27, 28, 37). The functional benefits of elevated pyruvate concentration suggest that anaplerotic pyruvate carboxylation may play an important role in the correction of metabolic abnormalities during conditions of stress such as hibernation. The goals of the present study were to: 1) examine the effects of hibernation on the content of CAC intermediates in the heart; 2) measure pyruvate carboxylation, pyruvate decarboxylation, and citrate efflux in the myocardium during hibernation; and 3) determine the effects of pharmacological concentrations of pyruvate on the hibernating myocardium. We used [U-13C3] lactate and [U-13C3]pyruvate and isotopomer analysis of tissue pyruvate and citrate to measure pyruvate carboxylation and decarboxylation in the well-characterized swine model of acute myocardial hibernation (1, 18, 29). PYRUVATE CARBOXYLATION IN MYOCARDIUM DURING HIBERNATION H1615 Fig. 2. Experimental protocol was divided into equilibration and experimental periods. At time ⫺20, blood flow from the left anterior descending (LAD) coronary artery was reduced by 40%. Infusion of 13C isotopic substrates began at time 0 and continued to the end of the protocol. A large punch biopsy was taken at time 60 for measurement of pyruvate decarboxylation and carboxylation. Arrows designate sampling of arterial and venous blood and cardiovascular recordings. HIB, hibernating myocardium under near-normal arterial lactate and pyruvate concentrations; HIB ⫹ PYR, hibernating myocardium with elevated arterial pyruvate concentration. AJP-Heart Circ Physiol • VOL perfusion bed. Mass isotopomers of metabolites containing 0-n 13C atoms are identified as Mi, where i ⫽ 0, 1,. . .,n. The relative rates of pyruvate carboxylation and decarboxylation were calculated as previously described (7) from 1) the M3 enrichment of tissue pyruvate, and 2) the M2 and M3 enrichments of the acetyl-CoA and OAA moieties of citrate, respectively (21). Mass isotopomers were adjusted for the natural abundance measured in myocardial tissue samples from pigs (n ⫽ 4) that were not infused with labeled substrates (5, 9). The measured enrichment of the M3 OAA moiety of citrate was corrected for 1) the fraction of M3 OAA molecules coming from some citrate isotopomers metabolized in the CAC and 2) the dilution of 13C in the CAC, as described in detail by Comte and co-workers (Eqs. 8–10 in Ref. 7). The absolute rates of pyruvate carboxylation and decarboxylation were calculated from the relative rates of pyruvate carboxylation and decarboxylation and the absolute rate of CAC flux. The latter was calculated from the myocardial oxygen consumption (MV̇O2) and the stoichiometric relationships between oxygen consumption and citrate formation from fat and carbohydrate as previously described (21). Statistical analysis. Data are presented as means ⫾ SE. The hemodynamic variables were compared between the two protocols using repeated-measures ANOVA. Statistical significance was determined using paired and unpaired t-tests as appropriate. RESULTS Cardiovascular parameters. There were no significant changes over the course of the experiment or between groups at any time point in peak systolic LV pressure, peak LV dP/dt, heart rate (see Fig. 3), or LV end-diastolic pressure (data not shown). In the HIB and HIB ⫹ PYR groups, MV̇O2 decreased by ⬃38% after 80 min of flow reduction (see Fig. 3). Metabolite concentrations and enrichments. With the onset of flow reduction, there was a metabolic switch from net lactate uptake to lactate production (see Fig. 4). The arterial blood citrate concentrations were 56 ⫾ 3 and 56 ⫾ 2 M in the HIB and HIB ⫹ PYR groups, respectively, and did not change from the beginning to the end of the protocol. Net citrate release by the myocardium decreased significantly (P ⬍ 0.05) from the preischemic control period (11.3 ⫾ 3.8 and 12.4 ⫾ 281 • OCTOBER 2001 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 in LAD blood were raised by 1.0 and 0.1 mM, respectively. In the HIB ⫹ PYR group, the concentration of [U-13C3]pyruvate in the infusate was 154 mM, so that the pyruvate concentration in LAD blood was raised by 1.0 mM. Left ventricular pressure, end-diastolic pressure, peak first derivative of left ventricular (LV) pressure with time (dP/dt), heart rate, and arterial and venous blood samples were taken at all sample times (see Fig. 2). Plasma samples were stored at ⫺80°C until further analysis. At the end of each protocol, large punch biopsies (3 g) of the LAD and circumflex (CFX) beds were quickly taken, freeze-clamped, and stored at ⫺80°C until analysis. We have previously shown that the CFX biopsy receives normal myocardial blood flow and thus serves as control tissue (18, 31). The heart was excised, and black ink was infused down the right and left main coronary arteries to identify the LAD perfusion bed, which was dissected and weighed (37.1 ⫾ 2.7 g). Analytic methods. The concentrations of plasma FFA, blood glucose, lactate, pyruvate, and citrate, as well as tissue lactate, pyruvate, and malate were determined using spectrophotometric enzymatic assays (3, 33, 40). Tissue pyruvate concentrations were measured immediately after homogenization in neutralized perchloric acid extracts to prevent loss of pyruvate from freeze-thaw (40). Tissue concentrations of ATP and ADP were measured using the ATP Bioluminescent Assay Kit (Sigma-Aldrich). Isotopic enrichments of plasma lactate and pyruvate were determined from the GC-MS analysis of the corresponding tert-butyldimethylsilyl (TBDMS) derivatives as previously described (7, 8, 21). The mass isotopomer distribution of tissue lactate, pyruvate, citrate, succinate, fumarate, and malate and the OAA moiety of citrate were also assayed as TBDMS derivatives (7, 8, 15, 39). Analyses were performed on a Hewlett-Packard 5890 Series II GC with an HP-5 capillary column (length 50 m, inside diameter 0.2 mm, and film thickness 0.3 m) coupled to a mass-selective detector (model 5970). Helium gas flow in the capillary column was 0.8–1.0 ml/min. Individual enrichments are averages of two or three GC-MS injections. The tissue concentrations of citrate, succinate, and fumarate were also assayed by GC-MS as previously described (7, 21). Enzyme activity of malic enzyme was measured using the methods described by Lin and Davis (17). Activity of pyruvate carboxylase was measured as per a modification of the original method by Struck and colleagues (34). Calculations. The myocardial blood flow was calculated as the LAD perfusion pump flow divided by the mass of the LAD H1616 PYRUVATE CARBOXYLATION IN MYOCARDIUM DURING HIBERNATION 5). Thus myocardial hibernation resulted in an ⬃80% reduction in citrate release by the heart. The arterial plasma FFA level was stable for the HIB and HIB ⫹ PYR groups at 0.54 ⫾ 0.05 and 0.56 ⫾ 0.06 mM, respectively. Net FFA uptake values during the Fig. 3. Left ventricular (LV) peak systolic pressure (A), peak first derivative of LV pressure with time (dP/dt, B), heart rate (C), and myocardial oxygen consumption (D). 2.1 nmol 䡠 g⫺1 䡠 min⫺1 for HIB and HIB ⫹ PYR groups, respectively) to the hibernation period (2.5 ⫾ 2.3 and 1.4 ⫾ 2.1 nmol 䡠 g⫺1 䡠 min⫺1 for HIB and HIB ⫹ PYR groups, respectively) in both the HIB and HIB ⫹ PYR groups. The rate of citrate release during hibernation was significantly lower than our previously published values (21) from animals subjected to the same isotope infusion but with normal coronary blood flow (see Fig. AJP-Heart Circ Physiol • VOL Fig. 5. Rate of citrate release (A) and pyruvate carboxylation (B). Data for the aerobic values are from previous work (21); *P ⬍ 0.05. 281 • OCTOBER 2001 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 Fig. 4. Net myocardial lactate production from ⫺40 to 0 min. *P ⬍ 0.05 compared with samples at ⫺40 to ⫺25 min. H1617 PYRUVATE CARBOXYLATION IN MYOCARDIUM DURING HIBERNATION Table 1. Tissue pyruvate and lactate concentrations in tissue from left anterior descending artery beds Table 3. Tissue concentration of citric acid cycle intermediates in LAD and CFX beds Tissue Concentration, mol/g wet wt Group HIB HIB ⫹ PYR Lactate 2.29 ⫾ 0.12 2.00 ⫾ 0.12 Pyruvate 0.17 ⫾ 0.02 0.19 ⫾ 0.02 Tissue Concentration, mol/g wet wt Group 15.5 ⫾ 2.3 11.4 ⫾ 1.9 Values are means ⫾ SE. HIB, hibernating conditions; PYR, high arterial pyruvate. Table 2. Tissue concentrations of ATP and ADP and ratio of ATP/ADP in left anterior descending and circumflex artery beds Succinate Fumarate Malate ATP ADP ATP/ADP 3.71 ⫾ 0.29 3.88 ⫾ 0.31 1.16 ⫾ 0.19 1.42 ⫾ 0.28 4.08 ⫾ 0.90 4.50 ⫾ 1.64 3.68 ⫾ 0.36 3.93 ⫾ 0.34 1.19 ⫾ 0.26 1.30 ⫾ 0.13 4.35 ⫾ 1.05 3.34 ⫾ 0.51 Values are means ⫾ SE. LAD, left anterior descending artery; CFX, circumflex artery. AJP-Heart Circ Physiol • VOL 1.61 ⫾ 0.075 0.098 ⫾ 0.008 0.109 ⫾ 0.009 0.165 ⫾ 0.016 1.41 ⫾ 0.074 0.093 ⫾ 0.004 0.104 ⫾ 0.005 0.153 ⫾ 0.015 1.55 ⫾ 0.114 0.112 ⫾ 0.011 0.115 ⫾ 0.007 0.170 ⫾ 0.016 1.40 ⫾ 0.105 0.096 ⫾ 0.010 0.107 ⫾ 0.005 0.151 ⫾ 0.008 Values are means ⫾ SE. The tissue contents of citrate, succinate, fumarate, and malate were not different between the LAD and CFX beds, nor was there a difference between the HIB and HIB ⫹ PYR groups for a given bed (see Table 3). These values are similar to those previously measured in aerobic animals and aerobic animals with elevated pyruvate (21). Thus hibernation induced by a 40% reduction in LAD flow did not result in a change in the concentration of the CAC intermediates. Pyruvate carboxylation and decarboxylation. The relative rates of pyruvate decarboxylation and carboxylation were calculated as previously described (7, 21). There were no changes in pyruvate decarboxylation between the groups (see Table 4) nor were these values different from values obtained in aerobic hearts (21). The relative rates of pyruvate carboxylation during hibernation were unaffected by elevated arterial pyruvate concentrations; however, values from hibernating myocardium were 50% lower than those previously found in aerobic and aerobic ⫹ pyruvate animals (see Table 4). Because there was not a significant change in pyruvate decarboxylation, the ratio of carboxylation to decarboxylation was significantly decreased by hibernation in both groups (see Table 4). Absolute rates of pyruvate decarboxylation and carboxylation were calculated from the rate of CAC flux, which was estimated from MV̇O2 as described previously (21). The rates of CAC flux were similar between the two groups (1.06 ⫾ 0.08 and 1.14 ⫾ 0.12 mol 䡠 g⫺1 䡠 min⫺1 for the HIB and HIB ⫹ PYR groups, respectively). The absolute rates of pyruvate decarboxylation (which is the flux through pyruvate dehydrogeTable 4. Relative fluxes through pyruvate decarboxylation and carboxylation per citric acid cycle flux and ratios of pyruvate carboxylation to decarboxylation Tissue Concentration, mol/g wet wt HIB LAD CFX HIB ⫹ PYR LAD CFX HIB LAD CFX HIB ⫹ PYR LAD CFX Relative Flux, % Group PD/CAC PC/CAC PC/PD Source Aerobic HIB Aerobic ⫹ PYR HIB ⫹ PYR 41.5 ⫾ 4.8 46.1 ⫾ 1.9 34.3 ⫾ 3.3 41.2 ⫾ 1.7 4.7 ⫾ 0.7 2.5 ⫾ 0.3* 5.7 ⫾ 0.6 2.7 ⫾ 0.5† 12.1 ⫾ 2 5.5 ⫾ 0.7* 17.7 ⫾ 3 6.5 ⫾ 1.2† Ref. 21 This investigation Ref. 21 This investigation Values are means ⫾ SE. PD, pyruvate decarboxylation; CAC, citric acid cycle; PC, pyruvate carboxylation. * P ⬍ 0.05 vs. aerobic group; † P ⬍ 0.05 vs. aerobic ⫹ PYR group. 281 • OCTOBER 2001 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 equilibration period were 0.12 ⫾ 0.02 and 0.12 ⫾ 0.03 mol 䡠 g⫺1 䡠 min⫺1 for the HIB and HIB ⫹ PYR animals, respectively, and were not different at the end of the protocol (0.09 ⫾ 0.01 and 0.09 ⫾ 0.03 mol 䡠 g⫺1 䡠 min⫺1 for the HIB and HIB ⫹ PYR groups, respectively). The rates of glucose uptake were similar at the end of the protocol compared with the equilibration period for the HIB animals (0.31 ⫾ 0.06 and 0.51 ⫾ 0.20 mol 䡠 g⫺1 䡠 min⫺1, respectively) and the HIB ⫹ PYR animals (0.26 ⫾ 0.04 and 0.47 ⫾ 0.19 mol 䡠 g⫺1 䡠 min⫺1, respectively). Tissue metabolites. Tissue lactate and pyruvate content and the lactate-to-pyruvate ratio were similar between the two groups (see Table 1) and were not different from previously published values from normal-flow animals subjected to the same isotope-infusion protocol (21). Thus despite lactate production at the onset of flow reduction, we observed normal lactate and lactate-to-pyruvate ratios after 80 min of reduced flow. Furthermore, the concentrations of ATP and ADP and the ATP-to-ADP ratio were unchanged between the hibernating LAD and CFX beds or between the two groups for a given bed (see Table 2), which confirms the observation of Schulz et al. (29) that there are normal ATP levels after ⬃80 min of moderate flow reduction in swine myocardium. The tissue M3 enrichments of lactate and pyruvate were not different between the two groups and were the same as previously published values with normal myocardial blood flow (21). There were no detectable M1 enrichments of pyruvate or lactate in either group, which demonstrates that there was no significant decarboxylation of malate to form pyruvate. Group Citrate Lactate/Pyruvate H1618 PYRUVATE CARBOXYLATION IN MYOCARDIUM DURING HIBERNATION DISCUSSION The key finding of this study is that a 40% reduction in MV̇O2 results in a decrease in both pyruvate carboxylation and citrate efflux with the maintenance of tissue levels of CAC intermediates. The absolute rate of pyruvate carboxylation decreased by 65% when there was only a 38% drop in MV̇O2 (see Fig. 3). If the decrease in malate and/or OAA supply to the CAC via pyruvate carboxylation were not matched by a decrease in the rate of the net efflux of CAC intermediates from the cycle, then the concentration of CAC intermediates in the myocardium would decrease. Hibernation had no effect on the tissue contents of citrate, succinate, fumarate, or malate, which suggests that the decrease in citrate release reflects a decrease in other efflux pathways for CAC intermediates, thus preserving the integrity of the CAC and the production of reducing equivalents, electron-transport-chain flux, and ATP formation, albeit at decreased rates. AJP-Heart Circ Physiol • VOL An acute reduction in coronary blood flow of ⬃40% results in an initial acceleration of glycolysis, a decrease in ATP, and a subsequent resetting of the metabolism to better match the reduced oxygen supply (1, 10, 22, 29). After 60–90 min of coronary blood flow reduction, the myocardium is in a relative state of hibernation with restored ATP content and reduced lactate production (1, 10, 29). The results of the present investigation extend the understanding of the acute phase of myocardial hibernation and demonstrate that the heart adjusts its metabolism to maintain the tissue content of CAC intermediates by a decrease in pyruvate carboxylation and citrate release. Thus the mitochondria conserve the constituents of the CAC. This is reflected in the greater degree of carbon recycling in the CAC as assessed by mass isotopomer analysis. It is important to note that prolonged hibernation may result in impaired CAC function, as recently suggested by Schulz and colleagues (30), who observed a progressive decrease in MV̇O2 during the course of 24 h of hibernation (an ⬃40% reduction in LAD flow) in a similar swine model. It has been suggested that with reduced coronary blood flow the rate of anaplerosis does not match the rate of CAC intermediate efflux, and there is a significant depletion of CAC intermediates (11). This is clearly not the case in acutely hibernating swine myocardium (see Table 3). As noted above, the decrease in anaplerotic pyruvate carboxylation matched with a decrease in net citrate efflux suggests that the CAC intermediate release is balanced by anaplerosis during hibernation. We measured net citrate efflux values from the heart of 2.5 and 1.4 nmol 䡠 g⫺1 䡠 min⫺1, which account for 10% and 6% of the absolute pyruvate carboxylation flux for HIB and HIB ⫹ PYR animals, respectively. This suggests that a decrease in the efflux of other metabolites such as succinate (15) plays a role in maintaining the total pool size of CAC intermediates. It is important to note that net citrate release may underestimate the true rate of citrate loss from the CAC. Cytosolic ATP-citrate lyase could cleave citrate into OAA and acetyl-CoA (12); therefore citrate loss from the CAC may be greater than the net citrate release and account for a larger fraction of the pyruvate carboxylation unless the carbon of OAA returns to the mitochondria. Another possible site of release from the CAC is the decarboxylation of malate by malic enzyme (13). However, the energetics of the reaction toward decarboxylation are unfavorable (35), and ex vivo experiments suggest that malic enzyme is mainly a carboxylating enzyme (8, 36, 39). In addition, we observed no M1 labeling of pyruvate with either normal flow (21) or with hibernation, which indicates that malate was not being decarboxylated by malic enzyme to produce pyruvate. Myocardial hibernation did not affect the relative contribution of pyruvate decarboxylation (via pyruvate dehydrogenase) to the CAC flux (see Table 4). This confirms the work of Liedtke (16), which used 14Clabeled substrate to demonstrate that a 60% reduction 281 • OCTOBER 2001 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 nase) were similar between the HIB and HIB ⫹ PYR groups (488 ⫾ 44 and 457 ⫾ 47 nmol 䡠 g⫺1 䡠 min⫺1, respectively) and our previously published values from aerobic myocardium (21). The absolute rates of pyruvate carboxylation were again similar between the HIB and HIB ⫹ PYR groups; however, these fluxes were decreased by 65% compared with previously published data from aerobic and aerobic ⫹ pyruvate animals (see Fig. 5) (21). Analysis of the mass isotopomer distribution of the OAA moiety of citrate and succinate allow one to calculate the fraction of the OAA pool that is recycled after one turn of the CAC. The fraction that is lost has two components: loss of CAC intermediates from the cell, and isotopic exchanges between metabolites of the CAC and related compounds such as glutamate, glutamine, and aspartate. In the present investigation, the extent of recycling of citrate through the CAC was 72 ⫾ 3 and 70 ⫾ 4% for the HIB and HIB ⫹ PYR animals, respectively. These are significantly higher than our previously published values obtained during normal flow aerobic conditions (60 ⫾ 4% and 56 ⫾ 4% for normal and high-pyruvate conditions, respectively). Thus there is greater recycling of CAC carbon during hibernation as confirmed by the decrease in citrate release (see Fig. 5). Malic enzyme and pyruvate carboxylase activity. Owing to the lower rate of pyruvate carboxylation in hibernating myocardium, we examined the possibility that there was a decrease in the activity of malic enzyme and/or pyruvate carboxylase. The activity of malic enzyme was unchanged between the LAD perfusion bed (840 ⫾ 50 nmol 䡠 g⫺1 䡠 min⫺1) and the CFX bed (830 ⫾ 50 nmol 䡠 g⫺1 䡠 min⫺1) in the HIB group. There was also no difference between the LAD and CFX beds in the activity of pyruvate carboxylase (32 ⫾ 7 and 31 ⫾ 9 nmol 䡠 g⫺1 䡠 min⫺1, respectively) in the HIB group. Similar values were obtained in the HIB ⫹ PYR group. PYRUVATE CARBOXYLATION IN MYOCARDIUM DURING HIBERNATION The authors thank Dr. D. Kerr and M. Lusk of the Department of Pediatrics, Case Western Reserve University for assistance with the pyruvate carboxylase assay and F. David and T. McElfresh for technical assistance in conducting this study. This work was supported by National Institutes of Health Grants HL-58653 (to W. C. Stanley), HL-59219 (to H. Brunengraber), and HL-07887, and Grant-in-Aid 005031N from the American Heart Association National Center (to W. C. Stanley). REFERENCES 1. Arai AE, Pantely GA, Anselone CG, Bristow J, and Bristow JD. Active downregulation of myocardial energy requirements during prolonged moderate ischemia in swine. Circ Res 69: 1458–1469, 1991. AJP-Heart Circ Physiol • VOL 2. Attwood PV. The structure and the mechanism of action of pyruvate carboxylase. Int J Biochem Cell Biol 27: 231–249, 1995. 3. Bergmeyer HU. Method of Enzymatic Analysis: Metabolites 2. Weinhein: VCH Verlagsgesellschaft, 1989. 4. Bittl JA and Shine KI. Protection of ischemic rabbit myocardium by glutamic acid. Am J Physiol Heart Circ Physiol 245: H406–H412, 1983. 5. Brunengraber H, Kelleher JK, and Des Rosiers C. Applications of mass isotopomer analysis to nutrition research. Annu Rev Nutr 17: 559–596, 1997. 6. Bunger R, Mallet RT, and Hartman DA. Pyruvate-enhanced phosphorylation potential and inotropism in normoxic and postischemic isolated working heart. Near-complete prevention of reperfusion contractile failure. Eur J Biochem 180: 221–233, 1989. 7. Comte B, Vincent G, Bouchard B, and Des Rosiers C. Probing the origin of acetyl-CoA and oxaloacetate entering the citric acid cycle from the 13C labeling of citrate released by perfused rat hearts. J Biol Chem 272: 26117–26124, 1997. 8. Comte B, Vincent G, Bouchard B, Jette M, Cordeau S, and Des Rosiers C. A 13C mass isotopomer study of anaplerotic pyruvate carboxylation in perfused rat hearts. J Biol Chem 272: 26125–26131, 1997. 9. Des Rosiers C, Di Donato L, Comte B, Laplante A, Marcoux C, David F, Fernandez CA, and Brunengraber H. Isotopomer analysis of citric acid cycle and gluconeogenesis in rat liver. Reversibility of isocitrate dehydrogenase and involvement of ATP-citrate lyase in gluconeogenesis. J Biol Chem 270: 10027–10036, 1995. 10. Fedele FA, Gewirtz H, Capone RJ, Sharaf B, and Most AS. Metabolic response to prolonged reduction of myocardial blood flow distal to a severe coronary artery stenosis. Circulation 78: 729–735, 1988. 11. Gibala MJ, Young ME, and Taegtmeyer H. Anaplerosis of the citric acid cycle: role in energy metabolism of heart and skeletal muscle. Acta Physiol Scand 168: 657–665, 2000. 12. Huang WY and Kummerow FA. Cholesterol and fatty acid synthesis in swine. Lipids 11: 34–41, 1976. 13. Jeffrey FM, Storey CJ, Sherry AD, and Malloy CR. 13C isotopomer model for estimation of anaplerotic substrate oxidation via acetyl-CoA. Am J Physiol Endocrinol Metab 271: E788– E799, 1996. 14. Kornberg HL. Anaplerotic sequences and their role in metabolism. In: Essays in Biochemistry, edited by Campbell PN and Marshall RD. London: Academic, 1966, p. 1–31. 15. Laplante A, Vincent G, Poirier M, and Des Rosiers C. Effects and metabolism of fumarate in the perfused rat heart. A 13 C mass isotopomer study. Am J Physiol Endocrinol Metab 272: E74–E82, 1997. 16. Liedtke AJ. Alterations of carbohydrate and lipid metabolism in the acutely ischemic heart. Prog Cardiovasc Dis 23: 321–336, 1981. 17. Lin RC and Davis EJ. Malic enzymes of rabbit heart mitochondria. Separation and comparison of some characteristics of a nicotinamide adenine dinucleotide-preferring and a nicotinamide adenine dinucleotide phosphate-specific enzyme. J Biol Chem 249: 3867–3875, 1974. 18. Mazer CD, Cason BA, Stanley WC, Shnier CB, Wisneski JA, and Hickey RF. Dichloroacetate stimulates carbohydrate metabolism but does not improve systolic function in ischemic pig heart. Am J Physiol Heart Circ Physiol 268: H879–H885, 1995. 19. McNulty PH, Sinusas AJ, Shi CQ, Dione D, Young LH, Cline GC, and Shulman GI. Glucose metabolism distal to a critical coronary stenosis in a canine model of low-flow myocardial ischemia. J Clin Invest 98: 62–69, 1996. 20. Opie LH. Effects of regional ischemia on metabolism of glucose and fatty acids. Relative rates of aerobic and anaerobic energy production during myocardial infarction and comparison with effects of anoxia. Circ Res 38: I52–I74, 1976. 21. Panchal AR, Comte B, Huang H, Kerwin T, Darvish A, Des Rosiers C, Brunengraber H, and Stanley WC. Partitioning of pyruvate between oxidation and anaplerosis in swine hearts. Am J Physiol Heart Circ Physiol 279: H2390–H2398, 2000. 281 • OCTOBER 2001 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 in LAD flow in swine decreases CAC flux but does not alter the relative contributions of fatty acids and carbohydrates to oxidative metabolism. This same observation was made using 13C-labeled glucose and NMR analysis in dogs subjected to a 30% reduction in coronary flow for 3–4 h (19). Thus with acutely hibernating myocardium, there is no change in the contribution of carbohydrate to oxidative metabolism. The elevated pyruvate concentrations in the HIB ⫹ PYR group did not elicit an increase in tissue pyruvate, pyruvate decarboxylation, or pyruvate carboxylation (see Tables 1 and 4; Fig. 5) or an increase in tissue M3 enrichment of pyruvate (data not shown). The lack of effect of elevated arterial pyruvate may be attributed to a low uptake of pyruvate into the myocardium. Studies infusing pyruvate at higher concentrations (5 mM) have reported an increased contribution of pyruvate to citrate after ischemia and improved contractile function (6, 37). In this study, with an arterial pyruvate concentration of 1.21 mM, we did not see any effect of pyruvate on pyruvate carboxylation or decarboxylation compared with an arterial pyruvate concentration of 0.28 mM. Further experimentation will be necessary to determine whether higher arterial concentrations of pyruvate will increase the contribution of pyruvate to citrate during hibernation. The present results suggest that there is a fine interregulation among the rates of CAC flux, pyruvate carboxylation, and release of CAC intermediates and the CAC pool size; however, the biochemical mechanisms are unclear. We did not observe a decrease in the in vitro activities of malic enzyme and/or pyruvate carboxylase, which suggests that there was not stable covalent modification of these enzymes, though it is possible that the effect of in vivo modification was lost when measured in vitro at near maximal activity. Hibernation does not appear to cause gross changes in some of the regulators of malic enzyme or pyruvate carboxylase such as pyruvate, NADP⫹/NADPH, ATP, ADP, malate, and acetyl-CoA (see Tables 1–3) (21, 32). Thus the biochemical mechanisms for the decrease in pyruvate carboxylation remain to be elucidated. In conclusion, the acute hibernation response is accompanied by a decrease in both pyruvate carboxylation and citrate efflux and the maintenance of tissue levels of CAC intermediates. Thus the integrity of the CAC is maintained during the early phase of myocardial hibernation. H1619 H1620 PYRUVATE CARBOXYLATION IN MYOCARDIUM DURING HIBERNATION AJP-Heart Circ Physiol • VOL 32. 33. 34. 35. 36. 37. 38. 39. 40. extraction but not glucose uptake. Am J Physiol Heart Circ Physiol 262: H91–H96, 1992. Stanley WC, Hernandez LA, Spires D, Bringas J, Wallace S, and McCormack JG. Pyruvate dehydrogenase activity and malonyl-CoA levels in normal and ischemic swine myocardium: effects of dichloroacetate. J Mol Cell Cardiol 28: 905–914, 1996. Stanley WC, Lopaschuk GD, Hall JL, and McCormack JG. Regulation of myocardial carbohydrate metabolism under normal and ischemic conditions. Potential for pharmacological interventions. Cardiovasc Res 33: 243–257, 1997. Struck E, Ashmore J, and Wieland O. Pyruvate carboxylase activity and glucose production in isolated perfused rat liver. Enzymol Biol Clin (Basel) 7: 38–52, 1966. Sundqvist KE, Heikkila J, Hassinen IE, and Hiltunen JK. Role of NADP⫹ (corrected)-linked malic enzymes as regulators of the pool size of tricarboxylic acid-cycle intermediates in the perfused rat heart. Biochem J 243: 853–857, 1987. Sundqvist KE, Hiltunen JK, and Hassinen IE. Pyruvate carboxylation in the rat heart. Role of biotin-dependent enzymes. Biochem J 257: 913–916, 1989. Tejero-Taldo MI, Caffrey JL, Sun J, and Mallet RT. Antioxidant properties of pyruvate mediate its potentiation of -adrenergic inotropism in stunned myocardium. J Mol Cell Cardiol 31: 1863–1872, 1999. Thomassen AR, Nielsen TT, Bagger JP, and Henningsen P. Myocardial exchanges of glutamate, alanine, and citrate in controls and patients with coronary artery disease. Clin Sci (Lond) 64: 33–40, 1983. Vincent G, Comte B, Poirier M, and Des Rosiers C. Citrate release by perfused rat hearts: a window on mitochondrial cataplerosis. Am J Physiol Endocrinol Metab 278: E846–E856, 2000. Williamson JR and Corkey BE. Assays of intermediates of the citric acid cycle and related compounds by fluorometric enzyme methods. In: Methods in Enzymology. New York: Academic, 1969, p. 434–516. 281 • OCTOBER 2001 • www.ajpheart.org Downloaded from http://ajpheart.physiology.org/ by 10.220.33.6 on May 15, 2017 22. Pantely GA, Malone SA, Rhen WS, Anselone CG, Arai A, Bristow J, and Bristow JD. Regeneration of myocardial phosphocreatine in pigs despite continued moderate ischemia. Circ Res 67: 1481–1493, 1990. 23. Peuhkurinen KJ and Hassinen IE. Pyruvate carboxylation as an anaplerotic mechanism in the isolated perfused rat heart. Biochem J 202: 67–76, 1982. 24. Peuhkurinen KJ, Takala TE, Nuutinen EM, and Hassinen IE. Tricarboxylic acid cycle metabolites during ischemia in isolated perfused rat heart. Am J Physiol Heart Circ Physiol 244: H281–H288, 1983. 25. Pisarenko OI, Studneva IM, Shulzhenko VS, and Kapelko VI. Relations between the energy state of the myocardium and release of some products of anaerobic metabolism during underperfusion. Pflügers Arch 416: 434–441, 1990. 26. Rahimtoola SH. A perspective on the three large multicenter randomized clinical trials of coronary bypass surgery for chronic stable angina. Circulation 72: 123–135, 1985. 27. Russell RR III, Mommessin JI, and Taegtmeyer H. Propionyl-L-carnitine-mediated improvement in contractile function of rat hearts oxidizing acetoacetate. Am J Physiol Heart Circ Physiol 268: H441–H447, 1995. 28. Russell RR III and Taegtmeyer H. Pyruvate carboxylation prevents the decline in contractile function of rat hearts oxidizing acetoacetate. Am J Physiol Heart Circ Physiol 261: H1756– H1762, 1991. 29. Schulz R, Guth BD, Pieper K, Martin C, and Heusch G. Recruitment of an inotropic reserve in moderately ischemic myocardium at the expense of metabolic recovery. A model of shortterm hibernation. Circ Res 70: 1282–1295, 1992. 30. Schulz R, Post H, Neumann T, Gres P, Luss H, and Heusch G. Progressive loss of perfusion-contraction matching during sustained moderate ischemia in pigs. Am J Physiol Heart Circ Physiol 280: H1945–H1953, 2001. 31. Stanley WC, Hall JL, Stone CK, and Hacker TA. Acute myocardial ischemia causes a transmural gradient in glucose