* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 16
Survey
Document related concepts
Transcript
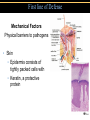
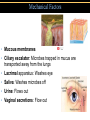
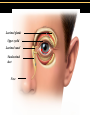
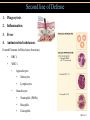
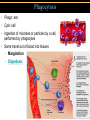
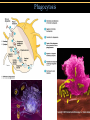
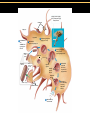
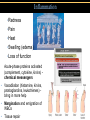
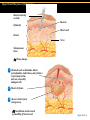
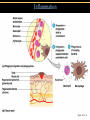
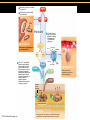
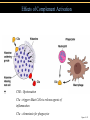
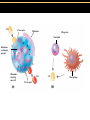
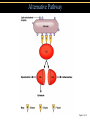
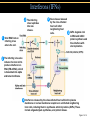
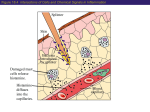
TORTORA • FUNKE • CASE Microbiology AN INTRODUCTION EIGHTH EDITION B.E Pruitt & Jane J. Stein Chapter 16 Nonspecific Defenses of the Host Nonspecific Defenses of the Host • Susceptibility Lack of resistance to a disease • Resistance Ability to ward off disease • Nonspecific resistance Defenses against any pathogen • Specific resistance Immunity, resistance to a specific pathogen • Native (innate) species specific immunity Figure 16.1 An overview of the body’s defenses. Host Defenses First line of defense • Intact skin • Mucous membranes and their secretions • Normal microbiota Second line of defense • Phagocytes, such as neutrophils, eosinophils, dendritic cells, and macrophages • Inflammation • Fever • Antimicrobial substances Third line of defense • Specialized lymphocytes: T cells and B cells • Antibodies First line of Defense Mechanical Factors Physical barriers to pathogens • Skin • Epidermis consists of tightly packed cells with • Keratin, a protective protein Mechanical Factors • Mucous membranes • Ciliary escalator: Microbes trapped in mucus are transported away from the lungs • Lacrimal apparatus: Washes eye • Saliva: Washes microbes off • Urine: Flows out • Vaginal secretions: Flow out Lacrimal glands Upper eyelid Lacrimal canal Nasolacrimal duct Nose Chemical Factors Chemical factors: • Low pH (3-5) of skin • Fungistatic fatty acid in sebum • Saltiness from perspirations • Lysozyme in perspiration, tears, saliva, and tissue fluids • Low pH (1.2-3.0) of gastric juice • Transferrins in blood bind iron • Cerumin – physical and chemical Blocks and low pH transplant? Normal Microbiota • Microbial antagonism/competitive exclusion: • Normal microbiota compete with pathogens. Second line of Defense 1. Phagocytosis 2. Inflammation 3. Fever 4. Antimicrobial substances Formed Elements In Blood (note functions) • RBC’s • WBC’s • • Agranulocytes • Monocytes • Lymphocytes Granulocytes • Neutrophils (PMNs) • Basophils • Eosinophils Table 16.1 Differential White Cell Count • Percentage of each type of white cell in a sample of 100 white blood cells (Never let monkeys eat bananas) Neutrophils 60-70% Basophils 0.5-1% Eosinophils 2-4% Monocytes 3-8% Lymphocytes 20-25% White Blood Cells • Neutrophils: Phagocytic • Basophils: Produce histamine • Eosinophils: Toxic to parasites, some phagocytosis • Monocytes: Phagocytic as mature macrophages • Fixed macrophages in lungs, liver, bronchi • Wandering macrophages roam tissues • Lymphocytes: Involved in specific immunity Phagocytosis • Phago: eat • Cyte: cell • Ingestion of microbes or particles by a cell, performed by phagocytes • Some travel out of blood into tissues: • Margination • Diapedesis Phagocytosis Figure 16.8a Toll like Receptors and PAMPs A phagocytic macrophage uses a pseudopod to engulf nearby bacteria. Pseudopods Phagocyte Cytoplasm 1 CHEMOTAXIS and ADHERENCE of phagocyte to microbe 2 INGESTION of microbe by phagocyte 4 Fusion of phagosome with a lysosome to form a phagolysosome Microbe or other particle Details of adherence 3 Formation of phagosome (phagocytic vesicle) Lysosome PAMP (peptidoglycan in cell wall) Digestive enzymes Partially digested microbe 5 DIGESTION of ingested microbes by enzymes in the phagolysosome Indigestible material 6 Formation of the residual body containing indigestible material TLR (Toll-like receptor) Plasma membrane 7 DISCHARGE of waste materials Microbial Evasion of Phagocytosis • Inhibit adherence: M protein, capsules • Kill phagocytes: Leukocidins Streptococcus pyogenes, S. pneumoniae • Lyse phagocytes: Membrane attack complex • Escape phagosome Listeriamonocytogenes • Prevent phagosome-lysosome fusion • Survive in phagolysosome HIV Staphylococcus aureus Shigella Coxiella burnetti and Mycobacteria spp Inflammation •Redness •Pain •Heat •Swelling (edema) •Loss of function Acute-phase proteins activated (complement, cytokine, kinins) chemical messengers • Vasodilation (histamine, kinins, prostaglandins, leukotrienes) bring in more help • Margination and emigration of WBCs • Tissue repair Chemicals Released by Damaged Cells • Histamine • Kinins • Prostaglandins • Leukotrienes Vasodilation, increased permeability of blood vessels Vasodilation, increased permeability of blood vessels Intensity histamine and kinin effect Increased permeability of blood vessels, phagocytic attachment Inflammation Figure 16.8a-b The process of inflammation. Bacteria entering on knife Bacteria Epidermis Blood vessel Dermis Nerve Subcutaneous tissue (a) Tissue damage 1 Chemicals such as histamine, kinins, prostaglandins, leukotrienes, and cytokines (represented as blue dots) are released by damaged cells. 2 Blood clot forms. 3 Abscess starts to form (orange area). (b) Vasodilation and increased permeability of blood vessels Figure 16.9a, b Inflammation Figure 16.9c, d Fever: Abnormally High Body Temperature • Hypothalamus normally set at 37°C • Gram-negative endotoxin cause phagocytes to release interleukin 1 • Hypothalamus releases prostaglandins that reset the hypothalamus to a high temperature • Body increases rate of metabolism and shivering to raise temperature • When IL-1 is eliminated, body temperature falls. (Crisis) The Complement System Serum proteins activated in a cascade. Increasing as previous catalyzes the next step Outcomes of Complement system 1. Chemotaxic 2. Opsonization 3. Cell lysis Figure 16.10 Figure 16.9 Outcomes of Complement Activation. 1 Inactivated C3 splits into activated C3 C3a and C3b. 2 C3b binds to microbe, resulting in opsonization. C3b C3a C3b proteins 3 C3b also splits C5 into C5a and C5b 5 C3a and C5a cause mast cells to release histamine, resulting in inflammation; C5a also attracts phagocytes. opsonization C5 Enhancement of phagocytosis by coating with C3b C5a C5b Histamine C5a Insert Fig 16.9 Mast cell 4 C5b, C6, C7, and C8 bind together sequentially and insert into the microbial plasma membrane, where they function as a receptor to attract a C9 fragment; additional C9 fragments are added to form a channel. Together, C5b through C8 and the multiple C9 fragments form the membrane attack complex, resulting in cytolysis. C5a receptor C6 C3a receptor C3a inflammation C7 C8 Increase of blood vessel permeability and chemotactic attraction of phagocytes C9 Microbial plasma membrane Channel C6 C7 C5b C8 C9 Formation of membrane attack complex (MAC) C6 C5b C7 C8 C9 Cytolysis cytolysis © 2013 Pearson Education, Inc. Bursting of microbe due to inflow of extracellular fluid through transmembrane channel formed by membrane attack complex Effects of Complement Activation • Opsonization or immune adherence: enhanced phagocytosis • Membrane attack complex: cytolysis • Attract phagocytes Figure 16.11 Effects of Complement Activation C3B - Opsinozation C3a - triggers Mast Cells to release agents of inflammation C5a - chemotaxic for phagocytes Figure 16.12 Figure 16.11 Inflammation stimulated by complement. C5a C5a receptor Histamine Phagocytes Neutrophil Histaminecontaining granule Insert Fig 16.11 Histaminereleasing mast cell C3a C3a receptor C5a Macrophage Classical Pathway Figure 16.13 Alternative Pathway Figure 16.14 Lectin Pathway Figure 16.15 Some bacteria evade complement • Capsules prevent C’ activation • Surface lipid-carbohydrates prevent MAC (membrane attack complex C5b - C9) formation • Enzymatic digestion of C5a Interferons (IFNs) Antiviral proteins • Alpha IFN & Beta IFN: Cause cells to produce antiviral proteins that inhibit viral replication • Gamma IFN: Causes neutrophils and macrophages to phagocytize bacteria Interferons (IFNs) 2 The infecting virus replicates into new viruses. 5 New viruses released by the virus-infected host cell infect neighboring host cells. 6 AVPs degrade viral m-RNA and inhibit protein synthesis and thus interfere with viral replication. 1 Viral RNA from an infecting virus enters the cell. 3 The infecting virus also induces the host cell to produce interferon on RNA (IFN-mRNA), which is translated into alpha and beta interferons. 4 Interferons released by the virus-infected host cell bind to plasma membrane or nuclear membrane receptors on uninfected neighboring host cells, inducing them to synthesize antiviral proteins (AVPs). These include oligoadenylate synthetase, and protein kinase. Figure 16.16