* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Rheumatology
Ulcerative colitis wikipedia , lookup
Rheumatic fever wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Anti-nuclear antibody wikipedia , lookup
Germ theory of disease wikipedia , lookup
Kawasaki disease wikipedia , lookup
Signs and symptoms of Graves' disease wikipedia , lookup
Systemic lupus erythematosus wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Autoimmunity wikipedia , lookup
Globalization and disease wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Myasthenia gravis wikipedia , lookup
Behçet's disease wikipedia , lookup
Autoimmune encephalitis wikipedia , lookup
Neuromyelitis optica wikipedia , lookup
Management of multiple sclerosis wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Systemic scleroderma wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Multiple sclerosis signs and symptoms wikipedia , lookup
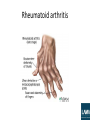
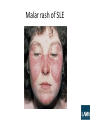
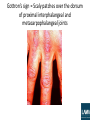
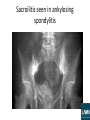
Rheumatology ALL RIGHTS RESERVED. This book contains material protected under International and Federal Copyright Laws and Treaties. Any unauthorized reprint or use of this material is prohibited. No part of this book may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying , recording, or by any information storage and retrieval system without express written permission from LAMA Immunologic Markers Found in Rheumatic Diseases Disease Systemic lupus erythematosus (SLE) Drug-induced lupus Rheumatoid arthritis (RA) Immunologic Markers ANA (95% of patients) Anti-dsDNA antibodies (60% of patients) Anti-Sm antibodies False–positive RPR (syphilis test) Anti-histone antibodies Ankylosing spondylitis RF (75% of patients) ANA (<50% of patients) HLA-DR4 common ANA Anti-Jo-1 antibodies HLA-B27 (90% of patients) Psoriatic arthritis Possible HLA-B27 Scleroderma Anti-scl-70 ANA CREST syndrome Anti-centromere antibodies Mixed connective tissue disease (MCTD) Anti-RNP ANA Sjögren's syndrome Anti-Ro (anti-SSA) ANA Anti-LA (anti-SSB) ANA Polymyositis or dermatomyositis Rheumatoid arthritis (RA) • Chronic inflammatory disorder, with infiltration of synovial joints by inflammatory cells and progressive erosion of cartilage and bone • Synovial hypertrophy, with granulation tissue formation on articular cartilage (i.e., pannus formation) caused by joint inflammation • Most commonly seen in middle-aged women; increased frequency in people with HLA-DR4 serotype • PIP and metacarpophalangeal (MCP) joints usually first involved; symmetric polyarthropathy develops, involving ankles, knees, shoulders, hips, elbows, and spine • H/P = – Malaise, weight loss, insidious onset of morning stiffness with pain, decreased mobility – Warm joints, joint swelling, fevers, ulnar deviation of fingers; MCP hypertrophy, swan neck deformities (i.e., flexed DIP plus hyperextended PIP), boutonniere deformities (i.e., flexed PIP), subcutaneous nodules, pleuritis, pericarditis, scleritis, chorea Rheumatoid arthritis • Labs = – Rheumatoid factor (RF) positive in 75% of patients, but not specific for the disease – Positive antinuclear antibodies (ANA) in 40% of patients (see Table 9-5) – Increased ESR, increased anticitrulline-containing protein IgM antibodies – Joint aspiration shows 5,000–50,000 leukocytes • Radiology = x-rays may demonstrate soft tissue swellings, joint space narrowing, marginal bony erosions, or subluxation; MRI is more sensitive than x-ray for detecting similar findings • Treatment = – Initially, NSAIDs and physical therapy, as needed – Patients still mildly symptomatic following NSAID use may be started on sulfasalazine or hydroxychloroquine and analgesics, as needed – Moderate disease can be treated with methotrexate; anti-tumor necrosis factor (TNF) drugs (e.g., infliximab) or corticosteroids may be considered – Anti-TNF drugs and corticosteroids combined with other regimens in severe disease Rheumatoid arthritis • RA is a systemic disease, two-thirds of the patients present with constitutional symptoms: fatigue, anorexia, weight loss, generalized weakness before onset of the arthritis; diagnostic criteria (need four of the following): – – – – – – – • • • • Morning stiffness (>1hr) for 6wks Swelling of wrists, MCPs, PIPs for 6wks Swelling of three joints for 6weeks Symmetric joint swelling for 6 wks Joint erosions on x-rays RF positive Rheumatoid nodules Joints never involved in RA: DIPs and joints of the lower back The axial skeleton occurs less than peripheral, cervical spine is the most frequently affected resulting in neck pain, stiffness and hyperreflexia. RA has ↑risk of developing septic arthritis, particularly Staph. Aureu→red. swollen joint and motion limited by pain. RA @ ↑ risk of developing osteopenia and osteoporosis Rheumatoid arthritis • Once patient has erosive joint disease: a clear-cut indication for disease modifying anti-rheumatic drugs (DMARD). Indomethacin or some other NSAID may be used as an adjunct. These agents slow down the progression of bony erosions and cartilage loss and therefore these agents are now, recommended to be used earlier in the course of disease. Other indications for their use are disease refractory to conservative treatment and dependence on steroids. These agents include methotrexate, hydroxychloroquine, sulfasalazine, leflunomide, etanercept, infliximab and azathioprine. – Methotrexate is the initial drug of choice and if not adequate, some other DMARDs drug may be used. Its side-effects include stomatitis, nausea, anemia and hepatotoxicity. – Hydroxychloroquine is inferior to methotrexate even though very safe than methotrexate. – Leflunomide has a role in patients who have contraindications to methotrexate such as significant pulmonary fibrosis. – Etanercept and infliximab are the new generation TNF inhibitors, and highly effective in patients who have refractory disease with methotrexate. They are very expensive and are not indicated as first line of treatment. Rheumatoid arthritis Still’s disease • Still’s disease (=systemic form of juvenile rheumatoid arthritis) – Systemic features: high-grade fever, leukocytosis, fleeting maculopapular rashes, hepatosplenomegaly, lymphadenopathy, pleuropericarditis and myocarditis are characteristic – Rheumatoid factor is rarely positive – Treat: NSAIDs and monitor of the liver enzymes→if not respond to NSAIDs or with myocarditis or anterior uveitis→corticosteroids • Adult still’s disease is a variant of rheumatoid arthritis. It usually presents in – 20-30yr – high spiking fevers – evanescent salmon colored maculopapular or macular rash that involves trunk and extremities. – arthritis or arthralgias and significant leukocytosis. – Rash typically develops along with fever. Temperature may show variation up to 4C. • To make the diagnosis of adult still’s disease, conditions like systemic lupus erythematosus (SLE), rheumatoid arthritis, malignancy, infectious mononucleosis and Parvovirus infection should not be present. Rheumatoid factor and ANA are usually negative. Systemic lupus erythematosus (SLE) • Multisystem autoimmune disorder involving a variety of autoantibodies affecting several body systems • Antibody-mediated cellular attack occurs with deposition of antigenantibody complexes in affected tissues • Risk factors = young women, blacks, Asians, Hispanics • Hydralazine, procainamide, isoniazid, methyldopa, quinidine, and chlorpromazine can cause similar symptoms that resolve when the drug is discontinued • H/P = – Common findings include malar and discoid rashes, serositis, oral ulcers, arthritis, photosensitivity, CNS symptoms, cardiac symptoms, and renal symptoms – Can also experience fevers, malaise, weight loss, abdominal pain, vomiting, conjunctivitis, blindness – Any combination of symptoms is possible and can change during the course of the disease SLE • Labs = – Positive ANA in 95% of patients (see Table 9-5) – Anti-double-stranded DNA (dsDNA) antibodies in 60% of patients, but not found in other rheumatologic disorders – Presence of anti-Sm antibodies is very specific for disease – Anti-histone antibodies may be seen for drug-induced, lupus-like symptoms – Patients frequently have a false–positive test for syphilis • Treatment = avoidance of sun, NSAIDs given for pain, hydroxychloroquine improves skin and renal symptoms, corticosteroids given for immunosuppression and to decrease exacerbations, other immunosuppressant drugs given in cases resistant to corticosteroids, anticoagulation required if patient considered hypercoagulable • Complications = lupus anticoagulant and anticardiolipin antibodies increase the risks of miscarriage and fetal death; disease follows variable course, with some cases remaining benign and others progressing rapidly; patient death results from progressive impairment of lung, heart, brain, and kidney function SLE • Systemic lupus erythematosus (SLE) is an autoimmune disorder involving multiple systems like musculoskeletal, cardiovascular, hematological, skin, lungs, kidney and serous membranes. If four or more of the diagnostic criteria set for SLE is met either serially or simultaneously diagnosis of SLE is made. Myositis can be a feature present in cases of SLE but it is not included in the diagnostic criteria of SLE – Systemic symptoms: Fatigue, fever, and weight loss. – Cutaneomucous symptoms: Malar rash, discoid rash, alopecia, oral or nasopharyngeal ulcers, and photosensitivity 3.Serositis: pericarditis, pleuritis – 4.Nephritis: which can be • -Mesangial, which is characterized by focal and segmental glomerular involvement with an increase in mesangial cells; • -Focal proliferative form; • -Diffuse proliferative form, which is characterized by a "wire loop" pattern resulting from immune complex deposition and subsequent thickening of the glomerular basement membranes. It can result in irreversible changes and chronic renal failure • -Membranous form, which is similar to primary membranous glomerulonephritis. 5.Neurologic symptoms: Depression, psychosis, seizures, and neuropathy. – 6.Non-erosive arthritis (>90% patients): like RA, mostly affects MCP and PIP, migratory and asymmetrical but non- erosive. – 7.Hematologic disease: Hemolytic anemia due to formation of autoantibodies against blood cells, a form of type II hypersensitivity reaction→pancytopenis (↓RBC, WBC, PLT); – 8. positive antinuclear antibodies; anti-dsDNA antibodies; anti-Sm antibodies; 6 subtypes of renal disorders in SLE • • • • • • • Type I: normal. Type II: Mesangial is the earliest and the least severe form and is present in 10-20 percent of cases. Anti-DsDNA titers are not very high. Type III: Focal proliferative is a severe form than Mesangial form and is present in 10-20 percent of cases. Urinalysis shows proteinuria and hematuria and serum creatinine is elevated. Histopathology shows proliferative changes with some areas of necrosis. Less than 50 percent of glomeruli are affected. Type IV: Diffuse proliferative is the most frequent pattern of renal involvement and unfortunately is the severest form. Hematuria, proteinuria, renal insufficiency, hypertension, marked hypocomplementemia and marked elevation of anti-DsDNA are all present. Histopathology shows changes that are similar but more severe than in focal proliferative type. More than 50 percent of glomeruli are affected. It has the worst of all prognosis. Type V: Membranous glomerulonephritis is present in 10-20% cases of SLE and usually presents with nephrotic syndrome. Renal function is preserved. Basement membrane is thickened and subepithelial deposits are present. It has better prognosis than diffuse proliferative type. Type VI: Sclerosing type represents healing of previous inflammatory damage and presents with renal insufficiency and normal urinary sediment. Immunosuppressive therapy is not effective in such patients as there is no active inflammation. Treatment of SLE renal problems • • • • • • • Type I (normal) and type II (mesangial proliferative) requires no treatment. Extensive type III (focal segmental proliferative), and all type IV (diffuse proliferative) require aggressive immunosuppression. Type V (membranous glomerulopathy) requires treatment when proliferative lesions are superimposed. Drugs: corticosteroids→cyclophosphamide→hydroxychloroquine (safe) Corticosteroids are the mainstay of treatment; usually IV methylprednisolone is used. Immunosuppressive agents, like Cyclophosphamide, may be needed when response to steroids is inadequate to improve renal disease or the disease is aggressive. Hydroxychloroquine is the safest drug for SLE. – However, rarely, it may cause serious eye disease including retinopathy like macular degeneration; corneal damage may also occur; so eye examinations at 6 months to 1 year intervals should be performed in all such patients who are taking this drug. Visual field defects, impaired color vision, bull’s eye pattern on funds and corneal whirls can all occur with its use. – The most common side effects of hydroxychloroquine are allergic skin reactions and nausea but they are not serious ones. The incidence of nausea can be reduced if it is taken after meals. – Contraindications to its use include G6PD deficiency, porphyria cutanea tarda, liver failure and hepatic failure. It is also need to be avoided in pregnancy. – Though it may cause hepatic failure, deafness and blood dyscrasias they are very rare and can be monitored by liver function tests (LFTs), hearing examination and CBC with differential respectively. This monitoring is not recommended regularly. MD SOAP CHAIR mnemonic for symptoms of SLE Malar rash of SLE Polymyositis and dermatomyositis • Progressive systemic diseases with skeletal muscle inflammation; one third of patients with polymyositis also have dermatomyositis (i.e., polymyositis with skin manifestations) • Risk factors = more common in women, blacks, elderly • H/P = – Symmetric progressive proximal muscle weakness (occurs in legs first) and myalgias, muscle atrophy in later stages of disease – Cutaneous manifestations of dermatomyositis are a red heliotropic rash on the face, upper extremities, chest, or back; violet discoloration of eyelids or scaly patches over hand joints – Patients with lung involvement have dyspnea and poor oxygenation saturation Polymyositis and dermatomyositis • Labs = – Increased creatinine, aldolase, CK, aspartate aminotransferase (AST), alanine aminotransferase (ALT), and lactate dehydrogenase (LDH) – ANA frequently positive – Anti-Jo-1 antibodies in patients with interstitial lung disease (see Table 9-5) – Muscle biopsy shows inflammatory cells and muscle degeneration, inflammatory cells within muscle fascicles in polymyositis and surrounding muscle fascicles in dermatomyositis • EMG = spontaneous fibrillations • Treatment = high-dose corticosteroids, methotrexate, or azathioprine for 4–6 wk followed by tapered dosing; IV immune globulin or other immunosuppressants can be added to regimen in resistant cases • Complications = possible interstitial lung disease, increased risk of several malignancies Gottron’s sign = Scaly patches over the dorsum of proximal interphalangeal and metacarpophalangeal joints Polymyalgia rheumatica (PMR) • Rheumatic disease with multiple sites of muscle pain and frequently associated with temporal arteritis; most common in elderly women • H/P = pain and stiffness in shoulder and pelvic girdle, difficulty raising arms and getting out of bed because of pain, malaise, unexplained weight loss; fever, minimal joint swelling, muscle strength maintained, although movement limited by pain • Labs = decreased Hct, markedly increased ESR, negative RF • Radiology = MRI demonstrates increased signal at tendon sheaths and synovial tissue outside of joints; positron emission tomographic (PET) scan shows increased uptake in large vessels • Treatment = low-dose corticosteroids, followed by tapered dosing • Weakness is a symptom of polymyositis, but not of polymyalgia rheumatica. Fibromyalgia • Disease causing chronic pain in muscles and tendons in absence of apparent inflammation • Unknown etiology, but frequently associated with depression, anxiety, and irritable bowel disease • Possible predisposition with hypothyroidism, RA, sleep apnea; more common in women, 20–50 yr of age • H/P = myalgias and weakness without inflammation; “trigger points” on examination (i.e., specific locations that when stimulated reproduce pain symptoms), fatigue; possible depression, sleep disturbances, dizziness, headaches, and mood disturbances • Treatment = stretching, antidepressants (e.g., tricyclic antidepressants [TCAs], selective serotonin reuptake inhibitors [SSRIs]), patient education, physical therapy modalities Age location Fibromyalgia Young adult Polymyalgia rheumatica >50 female Polymyositis 40-60 Proximal muscles ESR Diffuse, Pectoral and pelvic girdles, multiple tender neck points musculoskeletal Stiffness (>1hr) and pain pain, ↑↑↑↑↑↑ EMG/biopsy - Normal Classic findings Anxiety, stress, insomnia, point tenderness over affected muscle Antidepressants (amitrip tyline), NSAIDS, rest Temporal arteritis, great response to steroids, very high , elderly T cell damage myofibers→inflamm ↑, abnormal EMG/biopsy, high risk for cancer complain Treatment Low-dose steroids; if with giant cell arteritis→highdose prednisolone Dermatomyositis Muscle weakness Muscle weakness ↑ ↑ steroids heliotrope rash; Gottron’s sign; high risk for cancer (ovarian cancer) prednisone→ methotrexate Ankylosing spondylitis • • • Chronic inflammatory disease of the spine and pelvis that results in eventual bone fusion Risk factors = 20–40 yr of age, male > female, white > black H/P = – Hip and low back pain that is worse in the morning and following inactivity; pain improves over course of day – Possible limited range of motion in spine, hip, or chest – Painful kyphosis that is relieved by bending forward – Possible self-limited anterior uveitis • • • Labs = positive HLA-B27 in 90% of patients, increased or normal ESR, negative RF, negative ANA Radiology = x-ray shows bamboo spine (multiple vertebral fusions); MRI shows increased signal in sacroiliac joints (sacroilitis) and vertebrae Treatment = physical therapy, NSAIDs; exercise helps to prevent or delay permanent deformities; sulfasalazine, methotrexate, or anti-TNF drugs may be beneficial in more significant disease; joint replacement may be needed in extremities Sacroilitis seen in ankylosing spondylitis Reiter’s syndrome or Reactive arthritis • Classic triad of urethritis, arthritis or arthralgias and eye disease of conjunctivitis and the presence of circinate balanitis (painless shallow ulcers present on the glans penis or urethra). • Onset of arthritis after infection with Chlamydia, Salmonella, Shigella, Yersinia and Campylobacter. E. Coli and Neisseria have not been implicated as possible causes of reactive arthritis. • Patients have negative rheumatoid factor. HLA-B27 positive • NSAIDs are the mainstay of treatment of Reiter’s syndrome/reactive arthritis. Reiter’s syndrome or Reactive arthritis • Typical skin lesion of Reiter’s syndrome is – Keratoderma blennorrhagicum - It is found on palms and soles. These lesions present as clear vesicles on red bases and later on develop into macules or papules. They resemble very closely to pustular psoriasis. Psoriatic arthritis • Arthritis that develops in approximately 1% of patients with psoriasis; DIP joints and spine most commonly affected • H/P = asymmetric joint pain and stiffness, symptoms worse in morning and improve with activity, symptoms usually less severe than RA, possible anterior uveitis; joint line pain, pain with stress on joints, pitting of nails • Labs = negative RF and ANA, possible positive HLA-B27 • Radiology = x-rays show findings similar to RA and highly destructive lesions of DIP and PIP joints (i.e., “pencil in cup” deformities); MRI is more sensitive in finding marrow edema • Treatment = NSAIDs, methotrexate, sulfasalazine, or antiTNF drugs, depending on severity Psoriatic arthritis • Psoriatic arthritis: DIP joints; psoriatic nail disease (pitting)→sausageshaped digit; typically: skin→joint; 15% joint→skin • It can present in 5 different forms. – – – – – Distal interphalangeal (DIP) joint involvement. Asymmetric oligoarthritis. Symmetric polyarthritis, similar to rheumatoid arthritis. Arthritis mutilans, characterized by deforming and destructive arthritis. Spondyloarthropathy, including both sacroiliitis and spondylitis. • These patients often have nail changes (pitting nails and onychodystrophy). Majority patients with psoriatic arthritis typically have skin lesions for years before the joint involvement. However, 15% of patients may develop joint disease prior to skin disease. DIP involvement and the presence of nail changes may be the only clue in these patients. Xray of the joints shows both combination of erosion and bone growth. Other changes include pencil cup deformity of fingers, fluffy periostitis, and bilateral asymmetrical fusiform soft tissue swelling. Psoriatic arthritis Scleroderma • Chronic multisystem sclerosis with accumulation of connective tissue, skin thickening, and visceral involvement • H/P = arthralgias, myalgias, hand swelling, Raynaud's phenomenon (i.e., blue distal extremities caused by arteriolar spasm), skin thickening, esophageal dysmotility, intestinal hypomotility, dyspnea, possible arrhythmias or heart failure • Labs = positive anti-scl-70 ANA (see Table 9-5) • CREST syndrome is a variant, with Calcinosis, Raynaud's phenomenon, Esophageal dysmotility, Sclerodactyly, and Telangiectasias – Skin thickening limited to distal extremities and face – Labs show anticentromere antibodies – Better prognosis than scleroderma • Treatment = supportive care; angiotensin-converting inhibitors (ACE-I) for malignant renal hypertension; calcium channel blockers and avoidance of caffeine, nicotine, and decongestants to relieve Raynaud symptoms; methotrexate or corticosteroids may improve skin thickening and pulmonary symptoms • Complications = pulmonary fibrosis, heart failure, acute renal failure caused by malignant renal hypertension Scleroderma Scleroderma • Diffuse scleroderma: diffuse fibrosis of skin and internal organs. – It usually occurs in women in their third to fifth decades. – These patients have thickening of the skin begins in acral sites (hands and feet) with loss of folds and wrinkles giving a mask like appearance. Some areas may show both depigmentation and hyper pigmentation. – Raynaud’ s phenomena and calcinosis cutis are commonly seen. – Polyarthralgia is an early symptom. – Kidney: involvement→HT→scleroderma renal crisis – Pulmonary arterial HT→RH failure – Esophageal and gastric dysmotility→GERD – Patients with scleroderma have positive ANA and anti Scl 70, anti-topoisomerase-I Ab. Mixed connective tissue disease (MCTD) • Overlapping features of SLE, scleroderma, and polymyositis • Can progress to a single diagnosis • H/P = Raynaud's phenomenon, polyarthralgias, arthritis, swollen hands, proximal muscle weakness, esophageal hypomotility, pulmonary symptoms; absence of renal and neurologic symptoms • Labs = positive anti-ribonucleoprotein (RNP) ANA • Treatment = NSAIDs, corticosteroids, ACE-I, supportive measures Sjögren's syndrome • Autoimmune disorder, with lymphocytic infiltration of exocrine glands • Can be seen in association with RA, SLE, or primary biliary cirrhosis • H/P = dry eyes, dry mouth, enlarged parotid glands, purpura on legs, peripheral neuropathy, possible symmetric arthritis associated with other autoimmune conditions • Labs = positive anti-Ro (anti-SSA) and anti-La (anti-SSB) antibodies • Treatment = supportive care, corticosteroids for significant symptoms • Sicca syndrome is Sjögren's syndrome without a secondary autoimmune association Gout • • • Peripheral monoarthritis caused by deposition of sodium urate crystals in joints Risk factors = renal disease, male gender, urate underexcretion, diuretic use, cyclosporine use, cancer, hemoglobinopathies, excessive alcohol consumption H/P = – Sudden severe pain and swelling in one joint that frequently starts at night – First metatarsophalangeal joint most commonly affected (i.e., podagra); ankle, knee, and foot joints also common sites – Possible concurrent fever, chills, or malaise • • • Labs = serum uric acid can be normal or increased; joint aspiration shows needleshaped, negatively birefringent crystals and several white blood cells (WBCs) Radiology = x-ray may show punched-out bone lesions in chronic cases Treatment = – NSAIDs (especially indomethacin), colchicine, corticosteroids – Decreasing alcohol and diuretic use and avoiding foods high in purines (e.g., red meats, fish) help prevent exacerbations – Probenecid (inhibits kidney uric acid resorption) or allopurinol (inhibits uric acid formation) used in cases of chronic gout to prevent flare-ups • • Complications = long-standing disease leads to chronic tophaceous gout with formation of nodular tophi (large deposits of crystals in soft tissues), leading to permanent deformity Allopurinol should not be administered in acute attacks of gout. Synovial aspirate from patient with gout; under polarized light Pseudogout (calcium pyrophosphate dihydrate deposition disease, or CPPD) • Calcium pyrophosphate dehydrate crystal deposition in joints • Familial condition associated with other endocrine diseases (e.g., DM, hyperparathyroidism) • H/P = similar presentation to gout, but less severe symptoms; knee and wrist most commonly initially affected joints • Labs = joint aspiration shows positively birefringent, rhomboid crystals • Radiology = x-ray may show chondrocalcinosis (i.e., calcification of articular cartilage in joints) • Treatment = NSAIDs, colchicine • Podagra rules out CPPD and suggests a diagnosis of gout. Synovial aspirate from patient with pseudogout; under polarized light Pseudogout • Hemochromatosis is clearly associated (50%) with pseudogout. Pseudogout also occurs more frequently in patients with transfusion hemosiderosis, hyperparathyroidism, hypomagnesemia, hypophosphatemia and hypothyroidism. • Pseudogout: acute inflammatory changes of the large joints, most commonly the knee joint. It is associated with fever, chills, and leukocytosis. Synovial fluid analysis may show a leukocyte count as high as 100,000/cmm. Do not confuse with septic arthritis. Gram stain is usually negative in pseudogout. Episodes may be precipitated by surgery or trauma and can last up to 10 days if not treated. The diagnosis is confirmed by the finding of positively birefringent calcium pyrophosphate crystals released from sites of chondrocalcinosis (calcification of articular cartilage) into joint space.