* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Drugs for Parkinson`s disease
Survey
Document related concepts
Prescription costs wikipedia , lookup
Discovery and development of integrase inhibitors wikipedia , lookup
Atypical antipsychotic wikipedia , lookup
Pharmacognosy wikipedia , lookup
Discovery and development of ACE inhibitors wikipedia , lookup
Metalloprotease inhibitor wikipedia , lookup
Drug interaction wikipedia , lookup
Chlorpromazine wikipedia , lookup
Norepinephrine wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Transcript
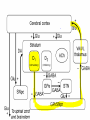
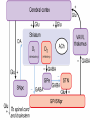
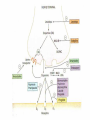
Drugs for Parkinson’s disease Pathogenesis of Parkinson’s disease Parkinson’s disease (PD) is a progressive disorder of movement that occurs mainly in the elderly. The chief symptoms are: H ypokinesia R igidity T remors 4/29/2017 3 Parkinson’s Disease A degenerative and progressive disorder Associated with neurological consequences of decreased dopamine levels produced by the basal ganglia (substantia nigra) Dopamine is a neurotransmitter found in the neural synapses in the brain Normally, neurones from the SN supply dopamine to the corpus striatum (controls unconscious muscle control) Initiates movement, speech and self-expression Balance, posture, muscle tone and involuntary movement depends on the roles of dopamine (inhibitory) and acetylcholine (Ach: excitatory) Basis to exploit by drugs: Restore dopamine function Inhibit Ach within corpus striatum Consequences of dopamine reductions Tremors – hands and head develop involuntary movements when at rest; pin-rolling sign (finger and thumb) Muscle rigidity – arthritis-like stiffness, difficulty in bending or moving limbs; poker face Bradykinesia – problems chewing, swallowing or speaking; difficulty in initiating movements and controlling fine movements; walking becomes difficult (shuffle feet) Postural instability – humped over appearance, prone to falls Clinical Presentation Altered body image (depression) Poor balance Bradykinesia (slow movement) Bradyphrenia (slowness of thought) Constipation Dribbling/drooling Dyskinesias (involuntary movements) Dysphagia (difficulty swallowing Dystonia (pain spasms) Excessive sweating (impaired thermoregulation) Festinating gait Hallucinations (visual) Postural hypotension Restless leg syndrome (leg aches, tingle, or burn) Rigidity Sleep disturbance Slurring/slowing of speech Tremor Causes number of factors: Environmental – toxins Free Radicals – there is a increase in postmortem brain sections Aging – age related decline in dopamine production Genetic – genes encode for -α-synuclein -Carboxy terminal hydroxylase of parkin & ubiquitin 4/29/2017 10 4/29/2017 11 Action of MPTP 1-methyl 4-phenyl 1,2,3,6tetrahydropyridine (MPTP) causes irreversible destruction of nigrostriatal dopaminergic neurons in various species, and produces a PD-like state in primates. MPP is taken up by the + MPTP MAO-B inhibit Selegiline MPP+ dopaminergic neurons, selective in destroying nigrostriatal neurons. It inhibits mitochondrial oxidation reactions, producing oxidative stress. Medication Rational Replace depleted levels of dopamine Stimulate the nerve receptors enabling neurotransmission Increase the effect of dopamine on nerve receptors (agonist) Counteract the imbalance of Ach and Dopamine The Drugs: Dopaminergic drugs (improving dopamine functioning) Levodopa Dopamine receptor agonists Amantadine Selective monoamine oxidase B inhibitors Catechol-O-methyltransferase inhibitors Antimuscarinic drugs (Ach inhibitors) Drugs Treatment of Parkinson’s Disease Dopamine precursor –levodopa Peripherally dopa decarboxylase inhibitor (carbidopa) COMT inhibitors ( entacapone, tolcapone) Drugs that mimic the action of dopamine ( bromocriptine, cabergoline, ropinirole, pramipexole) Drugs Treatment of Parkinson’s Disease MAO-B inhibitors (e.g. selegiline) Drugs that release dopamine (e.g. amantadine) Centrally acting antimuscarinic drugs (e.g. trihexyphenidyl, procyclidine, orphenadrine, benztropine) Levodopa Mechanism: (1) Because dopamine does not cross the blood-brain barrier levodopa, the precursor of dopamine, is given instead. (2) Levodopa is formed from L-tyrosine and is an intermediate in the synthesis of catecholamines. Levodopa Mechanism: (3) Levodopa itself has minimal pharmacologic activity, in contrast to its decarboxylated product, dopamine. (4) Levodopa is rapidly decarboxylated in the gastrointestinal tract. Prior to the advent of decarboxylase inhibitors (carbidopa), large oral doses of levodopa were required; thus, toxicity from dopamine was a limiting factor. Levodopa Pharmacokinetics: (1) Levodopa is well absorbed from the small bowel; however, 95% is rapidly decarboxylated in periphery. (2) Peripheral dopamine is metabolized in the liver to dihydroxyphenylacetic acid (DOPAC) and homovanillic acid (HVA), which are then excreted in urine. Levodopa Pharmacologic effects: The effects on bradykinesia and rigidity are more rapid and complete than the effects on tremor. Other motor defects in PD improve. The psychological wellbeing of patient is also improved. Levodopa Pharmacologic effects: Tolerance to both beneficial and adverse effects occurs with time. Levodopa is most effective in the first 2-5 years of treatment. wearing off effect On-off phenomenon Levodopa Adverse effect: Principal adverse effects include: (1) Anorexia, nausea, and vomiting upon initial administration, which often limit the initial dosage. (2) Cardiovascular effects, including tachycardia, arrhythmias, and orthostatic hypotension. Levodopa Adverse effect: (3) Mental disturbances, including vivid dreams, delusions, and hallucination. (4) Hyperkinesia (5) On-off phenomena Levodopa Adverse effect: Sudden discontinuation can result in fever, rigidity, and confusion. The drug should be withdrawn gradually over 4 days. Levodopa Drug interactions: Vit B6 reduces the beneficial effects of Levodopa by enhancing its extracerebral metabolism. Phenothiazines, reserpine, and butyrophenones antagonize the effects of levodopa because they lead to a junctional blockade of dopamine action. Carbidopa Carbidopa is an inhibitor of dopa decarboxylase. Because it is unable to penetrate the blood-brain barrier, it acts to reduce the peripheral conversion of levodopa to dopamine. As a result, when carbidopa and levodopa are given concomitantly. Carbidopa Virtue: a. It can decrease the dosage of levodopa. b. It can reduce toxic side effects of levodopa. c. A shorter latency period precedes the occurrence of beneficial effects. Selegiline A selective inhibitor of MAO-B, which predominates in DA-containing regions of the CNS and lacks unwanted peripheral effects of non-selective MAO inhibitors. It enhances and prolongs the antiparkinsonism effect of levodopa. It may reduce mild on-off or wearing-off phenomena. Selegiline Long-term trials showed that the combination of selegiline and levodopa was more effective than levodopa along in relieving symptoms and prolonging life. 31 COMT- inhibitors (entacapone) MoA: inhibits the breakdown of levodopa Pharmacokinetics: variability of absorption, extensive first-pass metabolism, short half-life Adverse effects: dyskinesias, hallucinations Amantadine Therapeutic uses and mechanism of action Amantadine is an antiviral agent used in the prophylaxis of influenza A2 . It improve parkinsonian symptoms by stimulating the release of DA from dopaminergic nerve terminals in the nigrostriatum and delaying DA reuptake. Anticholinergic agents Mechanism: Since the deficiency of dopamine in the striatum augments the excitatory cholinergic system in the striatum, the blockade of this system by anticholinergic agents helps to alleviate the motor dysfunction. Improvement in the parkinsonian tremor is more pronounced than improvement in bradykinesia and rigidity. Therapeutic uses: Although not as effectives as levodopa, it may have an additive therapeutic effect at any stage of the disease when taken concurrently. Adverse effects: Mental confusion and hallucinations. It can occur as can peripheral atropine-like toxicity (e.g. cycloplegia, urinary retention, constipation) Huntington’s Chorea Inherited autosomal dominant disorder Error in huntingtin gene Synthesis of huntingtin protein (repeats of polyglutamine cause excitotoxicity and apoptosis in cortex and striatum) Degeneration of GABAergic neurons in the striatum Huntington’s Chorea Huntington’s Chorea Dance like movements of limbs Rhythmic movements of tongue and face Dementia Progressive brain degeneration Huntington’s Chorea Tx Chlorpromazine Haloperidol Olanzapine Alzheimer’s disease Progressive memory loss Disordered cognitive functions Reduced verbal fluency Bedridden as disease progresses Complications of immobility Alzheimer’s disease Amyloid plaque (extracellular deposits of β-amyloid protein) Intraneuronal neurofibrillary tangles (aggregates of highly phosphorylated neuronal protein) Loss of cholinergic neurons in brain (originates from nucleus basalis in forebrain and project to frontal cortex and hippocampus) Alzheimer’s disease Tx Anticholinesterases Tacrine (hepatotoxic) Donepezil Rivastigmine Galantamine Nootropics Anti-oxidants NMDA antagonist Memantine Piracetam Vit. A, C, Zinc, Selenium Miscellaneous Statins Ibuprofen Multiple Sclerosis Demylenation in brain, spinal cord, optic nerves autoimmune Weakness, numbness, spastic paraparesis, diplopia, sphincter disturbances Tx Interferon beta-1b Natalizumab Baclofen, Diazepam (for spasticity) Amyotropic Lateral sclerosis Neurodegenerative dis. of motor neurons Muscle wasting and atrophy Defective superoxide dismutase (defective scavenging of superoxide free radicals) Defective glutamate uptake (excitotoxicity) Spontaneous twitching of motor units Difficulty in chewing & swallowing Respiratory failure & death within 5 yrs Tx – Riluzole (↓es glutamate release) Psychostimulants Amphetamine & Methylphenidate (release NA & DA in brain) -ADHD Modafinilinc alertness & keep awake CaffeineMigraine, allay fatigue, apnoea in premature infants MCQs Q1. In parkinsonism, Carbidopa acts as: A. Dopamine agonist B. Dopamine precursor C. Peripheral decarboxylase inhibitor D. Dopamine reuptake blocker Ans- C Q2. In parkinsonism, Entacapone acts as: A. Dopamine agonist B. Dopamine precursor C. COMT inhibitor D. Dopamine reuptake blocker Ans- C Q 3.Which one of the following clinical features of parkinsonism is benefited more by central anticholinergic drugs? A. Hypokinesia B. Rigidity C. Tremors D. Festinating gait Ans C Q 4.Which one of the following clinical features of parkinsonism is resolved first by levodopa? A. Hypokinesia B. Rigidity C. Tremors D. Festinating gait Ans A and B Q5. Tolcapone is withdrawn due to A. Cadiotoxicity B. Nephrotoxicity C. Carcinogenecity D. Hepatotoxicity Ans D Thank you Bibliography Essentials of Medical Pharmacology -7th edition by KD Tripathi Goodman & Gilman's the Pharmacological Basis of Therapeutics 12th edition by Laurence Brunton (Editor) Lippincott's Illustrated Reviews: Pharmacology - 6th edition by Richard A. Harvey Basic and Clinical pharmacology 11th edition by Bertram G Katzung Rang & Dale's Pharmacology -7th edition by Humphrey P. Rang Clinical Pharmacology 11th edition By Bennett and Brown, Churchill Livingstone Principles of Pharmacology 2nd edition by HL Sharma and KK Sharma Review of Pharmacology by Gobind Sparsh 52