* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Myocardyal fibrosis markers: A new target in Cardiovascular
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac surgery wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
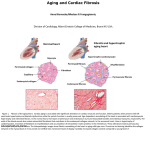
Myocardyal fibrosis markers: A new target in Cardiovascular Prevention? Ricardo Lopez Santi President of Comité de Epidemiolog ía y Prevención, Federaci ón Argentina de Cardiolog ía, and Director of PROCORDIS, Fundaci ón Bioquímica Gonnet, Buenos Aires, Argentina The constant evolution of medical strategies has determined that the concept of cardiovascular prevention becomes the flag of clinical investigation. This fact has been clearly shown during the last decades, in which we have seen a permanent effort to find important elements to determine the risk to suffer cardiovascular events both in primary and secondary prevention. The strong relationship between some of these elements and cardiovascular risk, in addition to their easy determination, have culminated in their usefulness for the clinical practice, being known as risk factors. However, in other cases, although they have generated great expectation, physicians have not been able to add these elements in the daily practice; researchers have observed and called them emergent risk factors. We can find two types of collagen fibers in the normal adult heart, type I and III, produced by fibroblasts and myofibroblasts. These fibers provide structural support and give the heart properties that include stiffness and resistance to deformation [1] . In addition, they have shown an important role as a link between contractile element of adjacent myocites, carrying some information useful for cell function. The fiber type I represents 80% of collagen protein in the heart, and type III is near to 10%. These concentrations increase with age and affect the myocardial function by incomplete ventricular relaxation [2] . In this way we find the myocardial fibrosis as a physiopathological substratum, determined by the abnormal increase of collagen fibers, and turned into the distinctive element of patients with structural damage and impairment of ventricular function. Thus the fibrosis becomes the main protagonist of some cardiovascular syndromes with more morbidity and mortality (Figure 1), such as hypertension, ischemic heart disease and heart failure [3] . For example we find that in particular processes such as myocardial hibernation, the collagen produced by local stimulation is the main characteristic of the fibrotic ventricular remodeling [4] . A disproportionate accumulation of fibrillar collagen in the extracelular matrix is the most important factor in this process [5] , and involves some alterations in essential aspects, such as cardiac function, coronary reserve and electrical activity. If we take hypertension as a model, the possibility to prove the presence of left ventricular hypertrophy is very important to determine the prognosis and therapy [6] . The hypertrophy involves not only the increase of myocites size, but the significant fibrillar collagen synthesis with ventricular remodeling, which play an interesting role in the changes of coronary flow, biochemical myocardial alterations and ventricular dysfunction [7] . Very strong evidence have shown the relationship between RAAS (mainly angiotensin II and aldosterone) [7-11], and ventricular remodeling, explaining why ACE inhibitors, angiotensin II type 1 receptors blockers and antagonist of aldosterone reduce the fibrotic process [7, 12-14] . Presently we are in the initial steps of genetic therapies and would see some evidence that particular genotype in essential hypertensive people could be associated with the increase of angiotensin, converting enzyme activity and the development of fibrosis [15]. Fibrosis assessment Different diagnostic methods could not assess this process, including the ultrasonic analysis, which anyway is the main tool to estimate heart elements in the clinical practice [16] . The echocardiography study is universally accepted to determine the left ventricular hypertrophy [17], but not the determination of fibrosis level, because the relation with the transvenous endomyocardial biopsies and anatomopathological determination is poor. However the current efforts of ultrasound to improve this assessment have been expressed in some techniques. One of them is the ultrasonic backscatter signal to detect the myocardial ultrasonic reflectivity [18] . Thus it is possible to increase the method's capacity and try to correlate the quantitative characterization of myocardial texture with the collagen content of the myocardial tissue [19] . The histopathologic analysis is the gold standard and the endomyocardial biopsy is an invasive tool. For this reason I has been necessary to find other less invasive and easy methods with good correlation to the amount of collagen in the extracellular space. In spontaneously hypertensive rats and in human beings with hypertension, we can find a selective increase of the two types of collagen fibers previously mentioned, type I and III, mainly the first one, as was observed in the normal myocardium by immunohistochemical techniques using specific monoclonal antibodies [20] . This fact was proposed as the cause of ventricular dysfunction and disturbs of electrical activities. The monitoring of fibrillar collagen synthesis and degradation [20 -23] appears today as an interesting possibility, and generates a good space for the development of myocardial fibrosis markers which importance can be seen in Figure 2. Now it is possible to determine the serum concentrations of the carboxy-terminal propeptide of procollagen type I (PIP), a marker of collagen type I synthesis, and the carboxy-terminal telopeptide of collagen type I (CITP) as a marker of extracellular collagen type I degradation. The first have showed better correlation to myocardial fibrosis with fiber concentration determined by histological observations [20] . The collagen type I is produced as procollagen with a small amino terminal, and a larger carboxy-terminal propeptide. After being secreted into the extracellular space, the propeptides are removed by specific endopeptidases and are released into the blood. We can find a very strong correlation between the fibers produced and the PIP in blood. Studies carried out in rats have demonstrated the possibility to determine by radioimmunoassay the different level of fibrosis with high sensitivity and specificity, in contrast to other methods as the ultrasound mentioned above, when it try to determine fibrosis level by anatomic characteristic. Based on these determinations the task to analyze the effect of some pharmacologic interventions has started. Recently we have known the results of investigations in human beings through the studies with ACE inhibitors, calcium channel blockers, and angiotensin II type 1 receptors blockers [13- 24]. In addition to the changes in the myocardial structure after some weeks since the beginning of treatment, we can see the excellent correlation published in some papers between serum levels of PPI by radioimmunoassay and collagen volume fraction by transvenous endomyocardial biopsies. Future perspectives The possibility to determine the level of fibrosis with a sample of blood and low cost, involves an optimistic expectation because we can see its potential utility and applications in the clinical practice such as: - To determine levels of risk related with the fibrosis magnitude - To obtain a new parameter for target organ damage in hypertensive and diabetic patients - To monitor therapeutic response to different drugs and other interventions - To become a new target for genetic therapies There can be no doubt that the interesting contribution that basic research has done in respect to the serum markers of fibrosis will open a new lines of clinical investigation, and certainly must involve a large number of patients to determine reference value, intraindividual variability and the therapeutic target. References 1. Gonzalez A, Lopez B, Querejeta R. Regulation of myocardial fibrillar collagen by angiotensin II: a role in hypertensive heart disease? J Mol Cell Cardiol 2002; 34(12):1585-93 2. De Souza RR. Anging of myocardial collagen. Biogerontology 2002; 3(6): 325-35 3. Delcayre C, Swynghedauw B. Molecular mechanisms of myocardial remodeling: the role of aldosterone. J Mol Cell Cardiol 2002; 34 (12):1577-84. 4. Frangogiannis NG. The pathological basis of myocardial hibernation. Histol Histopathol 2003; 18(2):647 -55. 5. Tanaka M. Quantitative analysis of myocardial fibrosis in normal, hypertensive hearts, and hypertrophic cardiomyopathy. Br Heart J 1986; 55:575-81. 6. The six report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Arch Intern Med 1997; 157: 2413-46. 7. Panizo A, Quinapril decreases myocardial accumulation of extracellular matrix components in spontaneously hypertensive rats. Am J Hypertens 1995; 8:815-22. 8. Alexander R, Dzau V, Vascular biology: the past 50 years. Circulation 2000; 102(IV):112-6. 9. Grana D, Angiotensina, arteriolas y miocardio. Rev Fed Argen Cardiol 2001; 30:521 -2. 10. Zannad F. Limitation of excessive extracellular matrix turnover may contribute to survival benefit of spironolactone therapy in patients with congestive heart failure: insights from the Randomized Aldactone Evaluation Study (RALES). Circulation 2000; 102: 2700-6. 11. Schmidt BM, Schmieder RE. Aldosterone -induced cardiac damage: focus on blood pressure independent effect. Am J Hypertens 2003; 16(1):80-6 12. Brilla C. Advanced hypertensive heart disease in spontaneously hypertensive rats. Hypertension 1996; 28:269-75. 13. López B. Usefulness of serum carboxy-terminal propeptide of procollagen type I in assessment of the cardioreparative ability of anti-hypertensive treatment in hypertensive oatients. Circulation 2001; 104:286-91.}14. Tachikawa H, Kodama M, Hui L. Angiotensin II type I receptor blocker, valsartan, prevented cardiac fibrosis rat cardiomiopathy after autoinmune myocarditis. J Cardiovasc Pharmacol 2003; 41(Suppl 1):S105-10 15. Takahashi T, Ueno H, Yasumoyo K. Angiotensin-converting enzyme-gene polymorphism is associated with collagen synthesis and QT dispersion in essential hypertension. J Hypertens 2003; 21:985-91 16. Picano E. In vivo quantitative ultrasonic evaluation of myocardial fibrosis in humans. Circulation 1990; 81:58-64. 17. Devereux RB. Detection of left ventricular hypertrophy by M -mode echocardiography: anatomic validation, standardization and comparision to other methods. Hypertension 1987; 9(suppl II): 19-26. 18. Maceira A, Barba J, Varo N. Ultrasonic backscatter and serum marker of cardiac fibrosis in hypertensives. Hypertension. 2002; 39:923-8 19. Kozakova M, Palombo C, Bernini G. Myocardial ultrasonic backscatter in hypertension: relation to aldosterone endothelin. Hypertension 2003; 41(2):230-6. 20. Querejeta R. Serum carboxy-terminal propeptide of procollagen type I is a marker of myocardial fibrosis in hypertensive heart disease. Circulation 2000; 101:1729 -35 21. Diez J. Increased serum concentrations of procollagen peptides in essential hypertension. Circulation 1995; 91:1450-6. 22. Diez J. Serum markers of collagen type I metabolism in spontaneously hypertensive rats. Circulation 1996; 93:1026-32. 23. Laviades C. Abnormalities of the extracellular degradation of collagen type I in essential hypertension. Circulation 1998; 98:535-40. 24. Diez J, Querejeta R, Lopez B. Losartan dependent regression of myocardial fibrosis is associated with reduction of left ventricular chamber stiffness in hypertensive patients. Circulation 2002; 105:2512-7. Your questions, contributions and commentaries will be answered by the lecturer or experts on the subject in the Hypertension list. Please fill in the form and press the "Send" button. Question, contribution or commentary : : Name and Surname: Country: : Argentina E-Mail address: @ Send Erase Top Updating: 09/19/2003