* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Uncomplicated Acute Myocardial Infarction Results in Protracted
Survey
Document related concepts
Transcript
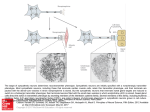
16P Medical Research Society M39 Uncomplicated Acute Myocardial Infarction Results in Protracted Sympathetic Hyperactivity After Discharge From Hospital LN Graham, PA Smith, JB Stoker, AF Mackintosh, DA Mary. Department of Cardiology, St James’s University Hospital, Leeds, UK Background: No information exists on the magnitude of sympathetic nerve activity and its changes over time following acute myocardial infarction (AMI). This information is required because activation of sympathetic drive is important in relation to morbidity and mortality. It is known that elevated levels of plasma catecholamines occur following uncomplicated AMI. However, this is an indirect index of sympathetic drive and returns to normal values within a week, despite the persistence of autonomic dysfunction for longer. Therefore we planned to quantify the central sympathetic output to the periphery following uncomplicated AMI, and investigate its progress up to six months after discharge from hospital. Methods: We examined 12 patients (age range 48 to 71 years) 2-4 days following AM1 and again after 3 and 6 months. None had clinical complications. All were on conventional therapy which remained unchanged throughout the study. Twelve healthy control subjects matched for age and body mass index were also studied. Muscle sympathetic nerve activity was measured from the peroneal nerve by microneurography. We quantified the central sympathetic output as the mean frequency of single units with defined vasoconstrictor properties. This was expressed in terms of impulses per 100 cardiac beats (imp1100b). Data were expressed as mean f SEM. Results: The sympathetic activity early after AM1 (95 f 6 . 3 imp/100b) did not change at 3 months (92 k4.7 imp/100b) but decreased after 6 months (80 f 4 . 8 imp/100b; p<O.Ol, ANOVA). These were still greater (p<O.OI) than control group values (57 f 4.8 imp/100b). There were no significant changes in arterial pressure or body mass index. The sympathetic hyperactivity was inversely correlated to left ventricular ejection fraction (at least r=-0.65; p<0.02). Conclusions: It was shown that a protracted state of sympathetic hyperactivity occurs following uncomplicated AMI.This could arise because of impairment of reflexes from cardiac receptors and may at least in part explain delayed morbidity and mortality following AMI. M40 Hypertrophic Cardiomyopathy fibrosis imaging by MRI J. Moon. Department of MRI, Royal Brompton Hospital, London, SW6 3LL Background: Hypertrophic Cardiomyopathy (HCM) is complicated by sudden death and cardiac failure. Characteristic autopsy histology includes myocardial disarray and macroscopic fibrosis. We hypothesised that gadolinium enhanced CMR could demonstrate fibrosis in HCM and be linked to clinical events. Methods: A blinded, case matched prospective study with predefined primary statistical analysis. 40 HCM patients were matched for the number of clinical risk factors for sudden death and for the presendabsence of adverse remodelling (progressive disease). Gadolinium enhanced CMR was performed. LV function, mass, total myocardial enhancement and enhancement pattern were assessed. Results: 31 (77%) of patients had contrast enhancement representing fibrosis. The mean percentage of myocardial fibrosis in the LV was 10.7% (04%).There was more fibrosis in patients with progressive disease (21% vs 9.196, p=0.002). In patients without progressive disease, patients at high risk of sudden death had more fibrosis (9.7% vs 5.2796, pd.05) as did patients with a history of VT/VF (12.1% vs 5.91%, pd.04). Different patients had different patterns of fibrosis (figure 1) and may have different clinical outcomes. Conclusion: Gadolinium enhanced CMR identifies and quantifies HCM fibrosis in-vivo. Fibrosis represents the abnormal myocardial substrate of HCM which may be a final common pathway for morbidity and mortality. Figure 1: a short axis contrast enhanced view in 4 patients; left to right: normal, fine diffuse fibrosis, subendocardial and confluent block fibrosis. M41 Genetic variation of the beta-1 adrenoceptor affects left ventricular mass T Stanton, S Padmanabhan, A G Jardine, A McConnachie, M Upton, G Watt, A F Dominiczak, J M C Connell. Left ventricular (LV) mass is an important cardiovascular risk factor. The beta-I adrenoceptor (BIAR) is a key cell surface signalling protein expressed in the heart and it’s variation may, therefore, affect LV mass. The gene of the BlAR has two known functional polymorphisms; one of these changes the nucleic acid sequence from guanine(G) to cytosine(C) at position 1165, conferring an amino acid change at position 389 from glycine to arginine. This area is critical for G-protein coupling and so cell signalling. The arginine-form of the receptor has been demonstrated to have increased GTP binding’. We therefore examined the relationship between this variation in the DlAR gene and the effect on LV mass in 2 populations. The first study consisted of 262 patients attending a renal clinic, 40% of whom were on renal replacement therapy(RRT). LV mass index (LVMI) was calculated from echocardiography and b l d drawn for DNA extraction. Individuals were categorised CC if both alleles encoded for arginine at position 389, GG if both alleles encoded for glycine. There was a highly significant difference in LV mass between the GG group when compared to the other 2 groups, CGGG p= 0.022 and CC:GG p=0.009. This relationship strengthened further when patients on RRT were omitted (CC:GG p <O.OoOl). In a second study, the effect of genotype on electrocardiographically measured LV mass was studied. 2280 subjects were genotyped for the PlAR polymorphism. No significant difference was found between LVMI and genotype after correction for age, BP and height and analysing separately for sex. In summary, no influence of the genotype on ECG defined LV mass was noted. In contrast, positive findings were obtained when echocardiography was used to measure LV mass in renal patients. It is therefore possible that genetic variation of the beta-1 adrenoceptor is of greater importance in defining LV mass in pathological circumstances. Reference: 1. Mason DA et al. J B i d Chem, 1999,274, 12670-4.