* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The Hypothalamus and Pituitary Gland
Survey
Document related concepts
Triclocarban wikipedia , lookup
Hormonal contraception wikipedia , lookup
Endocrine disruptor wikipedia , lookup
Neuroendocrine tumor wikipedia , lookup
Bovine somatotropin wikipedia , lookup
Vasopressin wikipedia , lookup
Hormone replacement therapy (menopause) wikipedia , lookup
Menstrual cycle wikipedia , lookup
Xenoestrogen wikipedia , lookup
Mammary gland wikipedia , lookup
Hyperthyroidism wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Bioidentical hormone replacement therapy wikipedia , lookup
Breast development wikipedia , lookup
Transcript
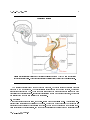
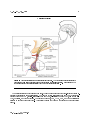
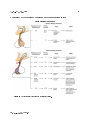
OpenStax-CNX module: m56734 1 The Hypothalamus and Pituitary Gland ∗ Steven Telleen Based on The Pituitary Gland and Hypothalamus† by OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0‡ Abstract By the end of this section, you will be able to: • Explain the interrelationships of the anatomy and functions of the hypothalamus and the posterior and anterior lobes of the pituitary gland • Identify the two hormones released from the posterior pituitary, their target cells, and their principal actions • Identify the six hormones produced by the anterior lobe of the pituitary gland, their target cells, their principal actions, and their regulation by the hypothalamus The hypothalamuspituitary complex can be thought of as the command center of the endocrine system. This complex secretes several hormones that directly produce responses in target tissues, as well as hormones that regulate the synthesis and secretion of hormones of other glands. In addition, the hypothalamus pituitary complex coordinates the messages of the endocrine and nervous systems. In many cases, a stimulus received by the nervous system must pass through the hypothalamuspituitary complex to be translated into hormones that can initiate a response. The hypothalamus is a structure of the diencephalon of the brain located anterior and inferior to the thalamus (Figure 1 (HypothalamusPituitary Complex )). It has both neural and endocrine functions, producing and secreting many hormones. In addition, the hypothalamus is anatomically and functionally related to the pituitary gland (or hypophysis), a bean-sized organ suspended from it by a stem called the infundibulum (or pituitary stalk). The pituitary gland is cradled within the sellaturcica of the sphenoid bone of the skull. It consists of two lobes that arise from distinct parts of embryonic tissue: the posterior pituitary (neurohypophysis) is neural tissue, whereas the anterior pituitary (also known as the adenohypophysis) is glandular tissue that develops from the primitive digestive tract. The hormones secreted by the posterior and anterior pituitary, and the intermediate zone between the lobes are summarized in Table 1. ∗ Version 1.2: Jul 6, 2015 1:33 pm -0500 † http://cnx.org/content/m46699/1.3/ ‡ http://creativecommons.org/licenses/by/4.0/ http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 2 HypothalamusPituitary Complex Figure 1: The hypothalamus region lies inferior and anterior to the thalamus. It connects to the pituitary gland by the stalk-like infundibulum. The pituitary gland consists of an anterior and posterior lobe, with each lobe secreting dierent hormones in response to signals from the hypothalamus. Pituitary Hormones Pituitary lobe Associated hormones Chemical class Eect Anterior Growth hormone (GH) Protein Promotes growth of body tissues Anterior Prolactin (PRL) Peptide Promotes milk production from mammary glands continued on next page http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 Anterior 3 Thyroid-stimulating Glycoprotein hormone (TSH) Stimulates thyroid hormone release from thyroid Anterior Adrenocorticotropic Peptide hormone (ACTH) Anterior lease by adrenal cortex Follicle-stimulating hor- Glycoprotein mone (FSH) Anterior Luteinizing Antidiuretic hormone Glycoprotein Stimulates androgen production by gonads hormone Peptide (ADH) Posterior Stimulates gamete production in gonads (LH) Posterior Stimulates hormone re- Stimulates water reabsorption by kidneys Oxytocin Peptide Stimulates uterine contractions during child- birth Intermediate zone Melanocyte-stimulating Peptide hormone Stimulates melanin formation in melanocytes Table 1 1 Posterior Pituitary The posterior pituitary is actually an extension of the neurons of the paraventricular and supraoptic nuclei of the hypothalamus. The cell bodies of these regions rest in the hypothalamus, but their axons descend as the hypothalamichypophyseal tract within the infundibulum, and end in axon terminals that comprise the posterior pituitary (Figure 2 (Posterior Pituitary )). http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 4 Posterior Pituitary Figure 2: Neurosecretory cells in the hypothalamus release oxytocin (OT) or ADH into the posterior lobe of the pituitary gland. These hormones are stored or released into the blood via the capillary plexus. The posterior pituitary gland does not produce hormones, but rather stores and secretes hormones produced by the hypothalamus. The paraventricular nuclei produce the hormone oxytocin, whereas the supraoptic nuclei produce ADH. These hormones travel along the axons into storage sites in the axon terminals of the posterior pituitary. In response to signals from the same hypothalamic neurons, the hormones are released from the axon terminals into the bloodstream. 1.1 Oxytocin When fetal development is complete, the peptide-derived hormone ulates uterine contractions and dilation of the cervix. oxytocin (tocia- = childbirth) stim- Throughout most of pregnancy oxytocin hormone receptors are not expressed at high levels in the uterus. Toward the end of pregnancy the synthesis of oxytocin receptors in the uterus increases, and the smooth muscle cells of the uterus become more sensitive to its http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 5 eects. Oxytocin is continually released throughout childbirth through a positive feedback mechanism. As noted earlier, oxytocin prompts uterine contractions that push the fetal head toward the cervix. In response, cervical stretching stimulates additional oxytocin to be synthesized by the hypothalamus and released from the pituitary. This increases the intensity and eectiveness of uterine contractions and prompts additional dilation of the cervix. The positive feedback loop continues until birth when the stretching of the cervix ceases. Although the mother's high blood levels of oxytocin begin to decrease immediately following birth, oxytocin continues to play a role in maternal and newborn health. First, oxytocin is necessary for the milk ejection reex (commonly referred to as let-down) in breastfeeding women. As the newborn begins suckling sensory receptors in the nipples transmit signals to the hypothalamus. In response oxytocin is secreted and released into the bloodstream. Within seconds smooth muscle cells in the mother's milk ducts contract ejecting milk into the infant's mouth. In addition to its eect on smooth muscle, oxytocin also has been shown to aect behavior. In both males and females there is evidence that oxytocin contributes to parentnewborn bonding, known as attachment. Oxytocin also is thought to be involved in feelings of love, closeness, and the establishment of pair bonding when released as part of the sexual response. Experiments with a single dose of nasally administered oxytocin indicate that it also is involved in, at least temporarily, inducing trust, cooperation, and positive social behavior among adults. However, the way in which oxytocin works in clinical therapies is not well understood, and evidence shows that while some patients benet from extended, repeated use others do not, some even becoming less social and more aggressive. Oxytocin is an evolutionarily old hormone that is found even in the simple worm C. elegans, a popular organism for studying neurological circuits because its entire nervous system contains only 302 neurons. In this species oxytocin helps the individual worms nd and recognize mates. A function of oxytocin in the mammalian brain seems to be the enhancement of specic neuronal circuits over others. In the hippocampus of rats, oxytocin has been shown to selectively act on inhibitory interneurons reducing background noise and improving signal transmission within specic brain circuits. These studies indicate that oxytocin helps the brain focus in on socially relevant sensory input. It also is becoming clear that oxytocin often does not work alone but requires other permissive or synergistic neurotransmitters, like serotonin or ADH, which may be why some oxytocin-only clinical trials have had limited results. 1.2 Antidiuretic Hormone (ADH) Antidiuretic hormone (ADH) was originally called vasopressin because it was rst identied for its role in regulating blood pressure. The release of ADH is controlled by two negative feedback loops, one where the regulated variable is blood pressure and the other where the regulated variable is blood osmolarity (solute concentration). Note that these two regulated variables are related. For example increasing water retention to respond to increased osmolarity will also increase blood volume and consequently blood pressure. This is a good example of the important role the hypothalamus plays in integrating competing needs in the attempt to optimize whole organism homeostasis. Blood pressure is monitored by baroreceptors (pressure receptors) in the aorta, the carotid arteries, and the aerent arterioles in the kidneys that respond to the mechanical stretching of the cell membrane of the sensory cells. A decrease in blood pressure reduces the stretching and triggers a signal to the hypothalamus (integration center). The ADH (messenger) that is released targets two eectors. It stimulates contraction of the smooth muscles in the blood vessels, increasing peripheral resistance. It also increases reabsorption of water in the kidney tubules (details on this eector response is discussed in more detail in the osmolarity section below) increasing blood volume. Both of these eects increase blood pressure which increases the stretching of the baroreceptors and reduces the signal to the hypothalamus, thus reducing the release of ADH. Interestingly, the hypothalamus also can trigger the release of ADH in anticipation of the need for increased blood pressure, for example to support the whole body needs in an emergency or excitement (ght/ight) response. This is why chronic stress, which also triggers this same anticipatory response, can http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 6 cause chronically high blood pressure. Blood osmolarity is monitored by osmoreceptorsspecialized cells within the hypothalamus and distal convoluted tubules in the kidneys that are particularly sensitive to the concentration of sodium ions and other solutes. Blood osmolarity may change in response to dehydration, the consumption of certain foods and uids, as well as in response to disease, injury, medications, or other factors. In response to high blood osmolarity the osmoreceptors signal the posterior pituitary (integration center) to release ADH (messenger). For this regulated variable the target cells of ADH (eectors) are the same tubular cells of the kidneys involved in responding to blood pressure. The eect is translocation of vesicles containing aquaporin channels into the epithelial cell membranes increasing permeability to water and therefore increased water reabsorption. The more channels added to the membranes the more water that is reabsorbed from the ltrate and returned to the blood leaving less to be excreted in the urine. The reabsorbed water dilutes the blood osmolarity. As blood osmolarity decreases, the osmoreceptor signal levels to the posterior pituitary change and prompt a corresponding decrease in the secretion of ADH. As a result, fewer aquaporin channels are maintained in the epithelial cell membranes so permeability decreases and less water is reabsorbed from the urine ltrate. Remember that, in the process of reducing osmolarity, the blood volume and with it blood pressure also increases. Drugs also can aect the secretion of ADH. For example, alcohol consumption inhibits the release of ADH, resulting in increased urine production that can eventually lead to dehydration, low blood pressure, and a hangover. A creative student intuitively noted this connection when he wrote on the wall above the urinal at a popular bar where I went to college: "You don't buy beer, you only rent it." Caeine is another commonly consumed drug that inhibits the release of ADH. A disease called diabetes insipidus is characterized by chronic underproduction of ADH that causes chronic dehydration. Because little ADH is produced and secreted, not enough water is reabsorbed by the kidneys. Although patients feel thirsty and increase their uid consumption this doesn't eectively decrease the solute concentration in their blood. Because ADH levels are not high enough to trigger water reabsorption in the kidneys, the additional water ingested just passes out with the urine. This can result in electrolyte imbalances in severe cases of diabetes insipidus. Note: diabetes does not refer to a glucose imbalance but refers to the symptom of high urine output. The more common form of diabetes, diabetes mellitus also is named after its symptom of higher than normal urine output. In this case the high urine output is not caused by low ADH levels but by excess glucose in the urine. This creates higher than normal urine osmolarity which pulls more water out with it. Mellitus means "honey-sweet" in Latin, referring to the sweet avor of the urine caused by the excess glucose. Before modern chemical techniques physicians would diagnose the disease using their built-in chemical analyzer, taste, to test the urine. Like oxytocin, ADH also has been shown to have behavioral eects in mammals. Many are related to behaviors mediating social interaction. There appear to be dierences in eect based on the sex of the individual. In voles increased ADH seems to increase pair bonding in females, while it increases territorial behavior in males. Likewise in Syrian hamsters, ADH appears to increase aggression in males while it decreases aggression in females. 2 Anterior Pituitary The anterior pituitary originates from the digestive tract in the embryo and migrates toward the brain during fetal development. There are three regions: the pars distalis is the most anterior, the pars intermedia is adjacent to the posterior pituitary, and the pars tuberalis is a slender tube that wraps the infundibulum. Recall that the posterior pituitary does not synthesize hormones, but merely stores them. In contrast, the anterior pituitary does manufacture hormones. However, the secretion of hormones from the anterior pituitary is regulated by two classes of hormones. These hormones, secreted by the hypothalamus, are the releasing hormones that stimulate the secretion of hormones from the anterior pituitary and the inhibiting hormones that inhibit secretion. Hypothalamic hormones are secreted by neurons, but enter the anterior pituitary through blood vessels http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 7 (Figure 3 (Anterior Pituitary )). Within the infundibulum is a bridge of capillaries and veins that connect hypophyseal portal system, allows primary capillary plexus and be transported directly the hypothalamus to the anterior pituitary. This network, called the hormones secreted by the hypothalamus to enter the to the secondary capillary plexus in the anterior pituitary without rst entering the systemic circulation. Branches of the superior hypophyseal artery form the hypophyseal portal system (see Figure 3 (Anterior Pituitary )). Hypothalamic releasing and inhibiting hormones diuse into the primary capillary plexus and travel through the hypophyseal portal veins, which carry them to the secondary capillary plexus where they diuse out into the intracellular uid of the anterior pituitary. Hormones produced by target cells in the anterior pituitary (in response to the hypothalamic releasing hormones) diuse into the secondary capillary plexus and are carried into the systemic circulation via the http://cnx.org/content/m56734/1.2/ hypophyseal vein. OpenStax-CNX module: m56734 8 Anterior Pituitary Figure 3: The anterior pituitary manufactures seven hormones. The hypothalamus produces separate hormones that stimulate or inhibit hormone production in the anterior pituitary. Hormones from the hypothalamus reach the anterior pituitary via the hypophyseal portal system. The anterior pituitary produces seven hormones. These hormones are part of the three-level hypothalamicpituitary axis presented in an earlier section. They are the thyroid-stimulating hormone (TSH), adrenocorticotropic hormone (ACTH), follicle-stimulating hormone (FSH), luteinizing hormone (LH), growth hormone (GH), prolactin, and beta endorphin. The rst four hormones, TSH, ACTH, FSH, and LH are collectively referred to as tropic hormones (trope- = turning) because they turn on the function of other endocrine glands. http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 9 2.1 Thyroid Stimulating Hormone The activity of the thyroid gland is regulated by thyroid-stimulating hormone (TSH), also called thyrotropin. TSH is released from the anterior pituitary in response to thyrotropin-releasing hormone (TRH) from the hypothalamus. As discussed shortly, it triggers the secretion of thyroid hormones by the thyroid gland. In a classic negative feedback loop, elevated levels of thyroid hormones in the bloodstream then trigger a drop in production of TRH and subsequently TSH. 2.2 Adrenocorticotropic Hormone The adrenocorticotropic hormone (ACTH), also called corticotropin, stimulates the adrenal cortex (the more supercial layer of the adrenal glands) to secrete corticosteroid hormones such as cortisol. ACTH comes from a precursor molecule known as pro-opiomelanotropin (POMC) which produces several biologically active molecules when cleaved, including ACTH, melanocyte-stimulating hormone, and the brain opioid peptides known as endorphins. The release of ACTH is regulated by the corticotropin-releasing hormone (CRH) from the hypothalamus in response to normal physiologic rhythms. A variety of stressors can also inuence its release, and the role of ACTH in the stress response is discussed later in this chapter. 2.3 Follicle-Stimulating Hormone and Luteinizing Hormone The endocrine glands secrete a variety of hormones that control the development and regulation of the reproductive system (these glands include the anterior pituitary, the adrenal cortex, and the gonadsthe testes in males and the ovaries in females). Much of the development of the reproductive system occurs during puberty and is marked by the development of sex-specic characteristics in both male and female adolescents. Puberty is initiated by gonadotropin-releasing hormone (GnRH), a hormone produced and secreted by the hypothalamus. GnRH stimulates the anterior pituitary to secrete gonadotropinshormones that regulate the function of the gonads. The levels of GnRH are regulated through a negative feedback loop; high levels of reproductive hormones inhibit the release of GnRH. Throughout life, gonadotropins regulate reproductive function and, in the case of women, the onset and cessation of reproductive capacity. The gonadotropins include two glycoprotein hormones: follicle-stimulating hormone (FSH) stimu- lates the production and maturation of sex cells, or gametes, including ova in women and sperm in men. FSH also promotes follicular growth; these follicles then release estrogens in the female ovaries. hormone (LH) Luteinizing triggers ovulation in women, as well as the production of estrogens and progesterone by the ovaries. LH stimulates production of testosterone by the male testes. 2.4 Growth Hormone The endocrine system regulates the growth of the human body, protein synthesis, and cellular replication. A major hormone involved in this process is growth hormone (GH), also called somatotropina protein hormone produced and secreted by the anterior pituitary gland. Its primary function is anabolic; it promotes protein synthesis and tissue building through direct and indirect mechanisms (Figure 4 (Hormonal Regulation of Growth )). GH levels are controlled by the hypothalamus through the release of GHRH and GHIH (also know as somatotropin and somatostatin respectively). While the balance of GHRH and GHIH released from the hypothalamus is the primary determinant for synthesis and release of Growth Hormone (GH), regulation of this balance is complex as the hypothalamus integrates input from many dierent sources. No single negative feedback loop has been identied as the primary controller, although Insulin-like Growth Factor (IGF-1) has been shown to reduce GH secretion in placebo-controlled experiments. IGF-1, which is released by the liver in response to GH, accounts for or enhances many of the eects attributed to growth hormone. Generally, the actions of the combined GH/IGF1 axis promote cell growth and inhibit cell apoptosis. Therefore, it should be no surprise that higher levels of IGF-1 are found in many cancers. http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 10 Hormonal Regulation of Growth Figure 4: Growth hormone (GH) directly accelerates the rate of protein synthesis in skeletal muscle and bones. Insulin-like growth factor 1 (IGF-1) is activated by growth hormone and indirectly supports the formation of new proteins in muscle cells and bone. The feedback control is not as simple as the gure makes it look. The circulating IGF-1 level is only one of many inputs integrated by the hypothalamus to establish the set point that maintains the balance between GHRH and GHIH, and consequently the circulating levels of both hormones (GH and IGF-1) at any given time. Other inputs include: • • • • • Genetic makeup Time of day (more is released during sleep) Age Sex Exercise status http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 • • • • • • 11 Stress levels Nutrition levels Body Mass Index (BMI) Disease status Estrogen status Exposure to xenobiotic substances (articial signal molecules) Because the amount of GH released is dependent on the relative balance between releasing and inhibiting antagonists, the actual circulating levels can be increased either by increasing the levels of the agonist (releasing signals) or decreasing the levels of the antagonist (inhibiting signals). The reverse also is true. The circulating levels of GH can be reduced either by decreasing the levels of the agonist or increasing the levels of the antagonist. Specic factors known to stimulate release of GH are: • • • • • • • • • • • GHRH Fasting (which may be connected to calorie restriction aects seen in aging experiments) Ghrelin (the hunger hormone produced in the GI tract) Androgen, both from male testes and the adrenal cortex in both sexes Estrogen Nicotinic agonists Deep sleep Niacin (vitamin B3) Vigorous exercise Clonidine and L-DOPA, both directly stimulate GHRH release Hypoglycemic arginine and propranolol, both directly inhibit GHIH release Specic factors known to inhibit release of GH are: • • • • • GHIH Circulating GH and IGF-1 (negative feedback on the pituitary and hypothalamus) Hyperglycemia Glucocorticoids (adrenal stress hormones) Dihydrotestosterone (DHT) Growth hormone has a number of eects on the body related to growth and metabolism; however, many of these eects may be more related to its stimulation of IGF-1 release than the direct results of the GH itself. In general the GH/IGF-1 axis stimulates growth of all internal organs, including the brain. This hypertrophy (increase in cell size) and hyperplasia (increase in cell number) via transcription activation (activating protein synthesis) and by optimizing the nutrient and energy resources needed to carry out both types of growth. is accomplished both by directly stimulating cell The GH/IGF-1 axis causes an increase in calcium retention by the body and stimulates bone mineralization. IGF-1 receptors have been identied on osteocytes, which likely play a role in these anabolic and mineralization aects related to bone growth. Additionally, IGF-1 promotes the uptake of amino acids by all cells, which are the required building blocks for protein synthesis. Increasing amino acid uptake is one of the "insulin-like" eects of IGF-1, as insulin also promotes the uptake of amino acids. Skeletal muscle and cartilage cells are particularly sensitive to stimulation from IGFs. Cell growth and division require energy, and GH/IGF-1 promote mobilization and management of the body's energy resources to support these functions. In addition to glucose as an energy source, most cells in the body can also use fatty acids and a few other molecules as an energy source. The exception are the cells of the nervous system, which also are the biggest consumer of body energy. Under normal circumstances muscles (the other large consumer of energy) and other cells rely mostly on fatty acids as their energy source, leaving most of the glucose for the nervous system. However, when whole body energy needs increase, so does the utilization of other energy molecules, like glucose. To protect the nervous system from depletion of http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 12 glucose by uptake from other parts of the body both a glucose sparing eect and a diabetogenic eect are activated. GH/IGF-1 create the glucose sparing eect by targeting the adipose cells causing them to initiate lipolysis (the breakdown of lipids back into fatty acids). This increases the level of fatty acids in the blood and therefore reduces the uptake of glucose by non-neuronal cells. The diabetogenic eect is a result of GH activity and refers to the active inhibition of glucose uptake by liver and muscle cells and the creation and release of "new" glucose molecules into the blood from other sources, primarily glycogen and non-carbohydrate molecules such as amino acids, pyruvate, lactate, and glycerol. Conversion of glycogen back to glucose is molecules is gluconeogenesis. glycogenolysis, while conversion of non-carbohydrate This combination of eects, while not caused by insulin reactions, results in elevated blood glucose levels similar to those seen in diabetes mellitus, hence the name diabetogenic eect. Dysfunction of the endocrine system's control of growth can result in several disorders. gigantism For example, is a disorder in children that is caused by the secretion of abnormally large amounts of GH, resulting in excessive growth. A similar condition in adults is acromegaly, a disorder that results in the growth of bones in the mandible, hands, and feet in response to excessive levels of GH in individuals whose other bones have stopped growing. Abnormally low levels of GH in children can cause growth impairment, a disorder called : pituitary dwarsm (also known as growth hormone deciency). Growth hormone is the focus of much popular attention and controversy. Human growth hormone (hGH) is an anabolic agent, and as such is one of the performance enhancing hormones banned for use by athletes. Anyone who has followed sports is aware of the many titles and awards that have been stripped from athletes in a wide variety of sports, both professional and amateur, because articial growth hormone (or an articial growth hormone stimulator or precursor) was detected in the athlete's blood. In livestock production growth hormone is creating controversy for its use to increase meat (muscle) and milk production bound for human consumption. Testing of milk from dairy cows that have been given bovine growth hormone (BGH) shows that the hormone does not show up in the milk. Nevertheless, many people still avoid milk from cows given BGH, and advertising milk and milk products as BGH-free has become a popular marketing strategy. Growth hormone currently is approved by the FDA only for use in cattle (beef ), so all legally sold poultry and eggs are "hormone free," even when they are not advertised as such. An additional o-label use of hGH is as a purported anti-aging supplement. While the research does show an increase in muscle mass and a decrease in fat deposits in elderly users, overall antiaging eects have not been supported. Additionally, at least one study at Stanford University indicated that muscle mass increases were not accompanied by muscle strength increases and may be a result of water retention by muscle cells rather than additional contractile protein synthesis. 2.5 Prolactin As its name implies, prolactin (PRL) promotes lactation (milk production) in women. During pregnancy, it contributes to development of the mammary glands, and after birth, it stimulates the mammary glands to produce breast milk. However, the eects of prolactin depend heavily upon the permissive eects of estrogens, progesterone, and other hormones. And as noted earlier, the active ejection of milk occurs in response to stimulation from oxytocin. In a non-pregnant woman, prolactin secretion is inhibited by prolactin-inhibiting hormone (PIH), which is actually the neurotransmitter dopamine, and is released from neurons in the hypothalamus. Only during pregnancy do prolactin levels rise in response to prolactin-releasing hormone (PRH) from the hypothalamus. http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 13 3 Intermediate Pituitary: Melanocyte-Stimulating Hormone The cells in the zone between the pituitary lobes secrete a hormone known as melanocyte-stimulating hormone (MSH) that is formed by cleavage of the pro-opiomelanocortin (POMC) precursor protein, the same precursor protein that gives rise to ACTH. Local production of MSH in the skin is responsible for melanin production in response to UV light exposure. The role of MSH made by the pituitary is more complicated. For instance, people with lighter skin generally have the same amount of MSH as people with darker skin. Nevertheless, this hormone is capable of darkening of the skin by inducing melanin production in the skin's melanocytes. Women also show increased MSH production during pregnancy; in combination with estrogens, which commonly leads to darker pigmentation of the skin of the areolas and labia minora. http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 14 4 Summary of the pituitary hormones and their principal eects Major Pituitary Hormones Figure 5: Major pituitary hormones and their target organs. http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 15 : 1 Visit this link to watch an animation showing the role of the hypothalamus and the pituitary gland. Which hormone is released by the pituitary to stimulate the thyroid gland? 5 Chapter Review The hypothalamuspituitary complex is located in the diencephalon of the brain. The hypothalamus and the pituitary gland are connected by a structure called the infundibulum, which contains vasculature and nerve axons. The pituitary gland is divided into two distinct structures with dierent embryonic origins. The posterior lobe houses the axon terminals of hypothalamic neurons. It stores and releases into the bloodstream two hypothalamic hormones: oxytocin and antidiuretic hormone (ADH). The anterior lobe is connected to the hypothalamus by vasculature in the infundibulum and produces and secretes six hormones. Their secretion is regulated by releasing and inhibiting hormones from the hypothalamus. The six anterior 1 http://openstaxcollege.org/l/roleofhypo http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 16 pituitary hormones are: growth hormone (GH), thyroid-stimulating hormone (TSH), adrenocorticotropic hormone (ACTH), follicle-stimulating hormone (FSH), luteinizing hormone (LH), and prolactin (PRL). 6 Interactive Link Questions Exercise 1 (Solution on p. 18.) 2 Visit this link to watch an animation showing the role of the hypothalamus and the pituitary gland. Which hormone is released by the pituitary to stimulate the thyroid gland? 7 Review Questions Exercise 2 (Solution on p. 18.) The hypothalamus is functionally and anatomically connected to the posterior pituitary lobe by a bridge of ________. a. blood vessels b. nerve axons c. cartilage d. bone Exercise 3 (Solution on p. 18.) Which of the following is an anterior pituitary hormone? a. ADH b. oxytocin c. TSH d. cortisol Exercise 4 (Solution on p. 18.) How many hormones are produced by the posterior pituitary? a. 0 b. 1 c. 2 d. 6 Exercise 5 (Solution on p. 18.) Which of the following hormones contributes to the regulation of the body's uid and electrolyte balance? a. adrenocorticotropic hormone b. antidiuretic hormone c. luteinizing hormone d. all of the above 2 http://openstaxcollege.org/l/roleofhypo http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 17 8 Critical Thinking Questions Exercise 6 (Solution on p. 18.) Compare and contrast the anatomical relationship of the anterior and posterior lobes of the pituitary gland to the hypothalamus. Exercise 7 Name the target tissues for prolactin. http://cnx.org/content/m56734/1.2/ (Solution on p. 18.) OpenStax-CNX module: m56734 18 Solutions to Exercises in this Module to Exercise (p. 16) Thyroid-stimulating hormone. to Exercise (p. 16) B to Exercise (p. 16) C to Exercise (p. 16) A to Exercise (p. 16) B to Exercise (p. 17) The anterior lobe of the pituitary gland is connected to the hypothalamus by vasculature, which allows regulating hormones from the hypothalamus to travel to the anterior pituitary. In contrast, the posterior lobe is connected to the hypothalamus by a bridge of nerve axons called the hypothalamichypophyseal tract, along which the hypothalamus sends hormones produced by hypothalamic nerve cell bodies to the posterior pituitary for storage and release into the circulation. to Exercise (p. 17) The mammary glands are the target tissues for prolactin. Glossary Denition 1: acromegaly disorder in adults caused when abnormally high levels of GH trigger growth of bones in the face, hands, and feet Denition 2: adrenocorticotropic hormone (ACTH) anterior pituitary hormone that stimulates the adrenal cortex to secrete corticosteroid hormones (also called corticotropin) Denition 3: antidiuretic hormone (ADH) hypothalamic hormone that is stored by the posterior pituitary and that signals the kidneys to reabsorb water Denition 4: follicle-stimulating hormone (FSH) anterior pituitary hormone that stimulates the production and maturation of sex cells Denition 5: gigantism disorder in children caused when abnormally high levels of GH prompt excessive growth Denition 6: gonadotropins hormones that regulate the function of the gonads Denition 7: growth hormone (GH) anterior pituitary hormone that promotes tissue building and inuences nutrient metabolism (also called somatotropin) Denition 8: hypophyseal portal system network of blood vessels that enables hypothalamic hormones to travel into the anterior lobe of the pituitary without entering the systemic circulation Denition 9: hypothalamus region of the diencephalon inferior to the thalamus that functions in neural and endocrine signaling http://cnx.org/content/m56734/1.2/ OpenStax-CNX module: m56734 Denition 10: infundibulum stalk containing vasculature and neural tissue that connects the pituitary gland to the hypothalamus (also called the pituitary stalk) Denition 11: insulin-like growth factors (IGF) protein that enhances cellular proliferation, inhibits apoptosis, and stimulates the cellular uptake of amino acids for protein synthesis Denition 12: luteinizing hormone (LH) anterior pituitary hormone that triggers ovulation and the production of ovarian hormones in females, and the production of testosterone in males Denition 13: osmoreceptor hypothalamic sensory receptor that is stimulated by changes in solute concentration (osmotic pressure) in the blood Denition 14: oxytocin hypothalamic hormone stored in the posterior pituitary gland and important in stimulating uterine contractions in labor, milk ejection during breastfeeding, and feelings of attachment (also produced in males) Denition 15: pituitary dwarsm disorder in children caused when abnormally low levels of GH result in growth retardation Denition 16: pituitary gland bean-sized organ suspended from the hypothalamus that produces, stores, and secretes hormones in response to hypothalamic stimulation (also called hypophysis) Denition 17: prolactin (PRL) anterior pituitary hormone that promotes development of the mammary glands and the production of breast milk Denition 18: thyroid-stimulating hormone (TSH) anterior pituitary hormone that triggers secretion of thyroid hormones by the thyroid gland (also called thyrotropin) http://cnx.org/content/m56734/1.2/ 19