* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
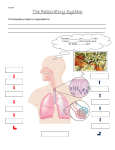
Download The Respiratory System
Biofluid dynamics wikipedia , lookup
Circulatory system wikipedia , lookup
Homeostasis wikipedia , lookup
Intracranial pressure wikipedia , lookup
Hemodynamics wikipedia , lookup
Haemodynamic response wikipedia , lookup
Cushing reflex wikipedia , lookup
Pre-Bötzinger complex wikipedia , lookup
Alveolar macrophage wikipedia , lookup
Common raven physiology wikipedia , lookup
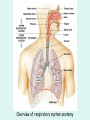
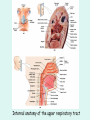
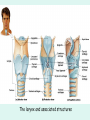
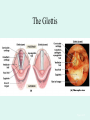
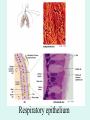
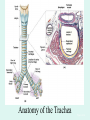
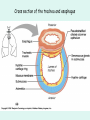
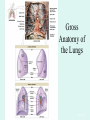
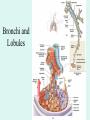
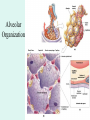
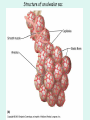
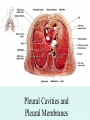
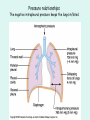
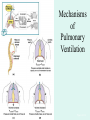
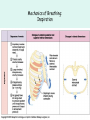
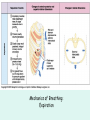
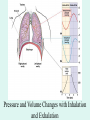
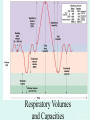
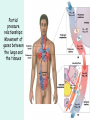
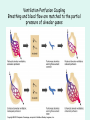
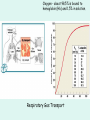
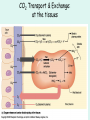
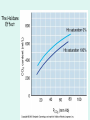
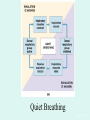
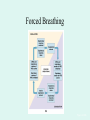
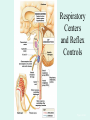
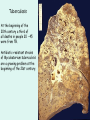
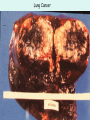
The Respiratory System Chapter 23 (6th edition chapter 22) Functions of the Respiratory System 1. Supply oxygen to the circulatory system for delivery to the tissues 2. Remove CO2 (and some other wastes) from blood. There are 4 processes that we call “respiration”. 1. Pulmonary ventilation - Movement of air into and out of the lungs (also referred to as “breathing”). 2. External respiration - Gas exchange in the lungs between the blood of the capillaries and the spaces in the air sacs (alveoli) 3. Transport - The movement of gases by the circulatory system Strictly speaking, a function of the blood. 4. Internal respiration - Gas exchange between the blood and the tissues of the body Overview of respiratory system anatomy External Structures of the nose Internal anatomy of the upper respiratory tract The larynx and associated structures The Glottis Figure 23–5 Respiratory epithelium Anatomy of the Trachea Figure 23–6 Cross section of the trachea and esophagus Gross Anatomy of the Lungs Figure 23–7 Bronchi and Lobules Figure 23–9 Secondary Bronchi • Branch to form tertiary bronchi, also called the segmental bronchi • Each segmental bronchus: – supplies air to a single bronchopulmonary segment Bronchopulmonary Segments • The right lung has 10 • The left lung has 8 or 9 Bronchial Structure • The walls of primary, secondary, and tertiary bronchi: – contain progressively less cartilage and more smooth muscle – increasing muscular effects on airway constriction and resistance The Bronchioles Figure 23–10 The Bronchioles • Each tertiary bronchus branches into multiple bronchioles • Bronchioles branch into terminal bronchioles: – 1 tertiary bronchus forms about 6500 terminal bronchioles Bronchiole Structure • Bronchioles: – have no cartilage – are dominated by smooth muscle Asthma • Excessive stimulation and bronchoconstriction • Stimulation severely restricts airflow Alveolar Organization Figure 23–11 Alveolar Epithelium • Consists of simple squamous epithelium • Consists of thin, delicate Type I cells • Patrolled by alveolar macrophages, also called dust cells • Contains septal cells (Type II cells) that produce surfactant Surfactant • Is an oily secretion • Contains phospholipids and proteins • Coats alveolar surfaces and reduces surface tension Respiratory Distress • Difficult respiration: – due to alveolar collapse – caused when septal cells do not produce enough surfactant Respiratory Membrane • The thin membrane of alveoli where gas exchange takes place 3 Parts of the Respiratory Membrane 1. Squamous epithelial lining of alveolus 2. Endothelial cells lining an adjacent capillary 3. Fused basal laminae between alveolar and endothelial cells Alveoli and the respiratory membrane Structure of an alveolar sac Pleural Cavities and Pleural Membranes • 2 pleural cavities: – are separated by the mediastinum • Each pleural cavity: – holds a lung – is lined with a serous membrane (the pleura) Pleural Cavities and Pleural Membranes Figure 23–8 The Pleura • Consists of 2 layers: – parietal pleura – visceral pleura • Pleural fluid: – lubricates space between 2 layers Respiratory Physiology Boyle’s law: P = 1/V or P1V1 = P2V2 Pressure relationships The negative intrapleural pressure keeps the lungs inflated Mechanisms of Pulmonary Ventilation Figure 23–14 Mechanics of Breathing: Inspiration Mechanics of Breathing: Expiration Compliance of the Lung • An indicator of expandability • Low compliance requires greater force • High compliance requires less force Factors That Affect Compliance 1. Connective-tissue structure of the lungs 2. Level of surfactant production 3. Mobility of the thoracic cage Gas Pressure • Can be measured inside or outside the lungs • Normal atmospheric pressure: – 1 atm or Patm at sea level: 760 mm Hg Pressure and Volume Changes with Inhalation and Exhalation Intrapulmonary Pressure • Also called intra-alveolar pressure • Is relative to Patm • In relaxed breathing, the difference between Patm and intrapulmonary pressure is small: – about —1 mm Hg on inhalation or +1 mm Hg on expiration Maximum Intrapulmonary Pressure • Maximum straining, a dangerous activity, can increase range: – from —30 mm Hg to +100 mm Hg Intrapleural Pressure • Pressure in space between parietal and visceral pleura • Averages —4 mm Hg • Maximum of —18 mm Hg • Remains below Patm throughout respiratory cycle Injury to the Chest Wall • Pneumothorax: – allows air into pleural cavity • Atelectasis: – also called a collapsed lung – result of pneumothorax Respiratory Physiology Resistance: F = P/R R = resistance P = change in pressure (the pressure gradient) Respiratory Volumes and Capacities Figure 23–17 Gas Exchange • Depends on: – partial pressures of the gases – diffusion of molecules between gas and liquid The Gas Laws • Diffusion occurs in response to concentration gradients • Rate of diffusion depends on physical principles, or gas laws – e.g., Boyle’s law Composition of Air • • • • Nitrogen (N2) about 78.6% Oxygen (O2) about 20.9% Water vapor (H2O) about 0.5% Carbon dioxide (CO2) about 0.04% Gas Pressure • Atmospheric pressure (760 mm Hg): – produced by air molecules bumping into each other • Each gas contributes to the total pressure: – in proportion to its number of molecules (Dalton’s law) Partial Pressure • The pressure contributed by each gas in the atmosphere • All partial pressures together add up to 760 mm Hg Respiratory Physiology: Dalton’s Law of Partial Pressures The total pressure of a mixture of gases is the sum of the partial pressures exerted independently by each gas in the mixture. Location Atmosphere at sea level Gas Approximate % Partial pressure in mmHg Approximate % Partial pressure in mmHg N2 78.6 597 74.9 569 O2 20.9 159 13.7 104 CO2 0.04 0.3 5.2 40 H2O 0.46 3.7 6.2 47 Total 100.0 760 100.0 760 Alveoli of lungs Partial pressure relationships: Movement of gases between the lungs and the tissues Henry’s Law • When gas under pressure comes in contact with liquid: – gas dissolves in liquid until equilibrium is reached • At a given temperature: – amount of a gas in solution is proportional to partial pressure of that gas Henry’s Law Figure 23–18 Diffusion and the Respiratory Membrane • Direction and rate of diffusion of gases across the respiratory membrane determine different partial pressures and solubilities Efficiency of Gas Exchange • Due to: – substantial differences in partial pressure across the respiratory membrane – distances involved in gas exchange are small Efficiency of Gas Exchange (2 of 2) – O2 and CO2 are lipid soluble – total surface area is large – blood flow and air flow are coordinated Solubility: Differential solubility of gases contributes to the balance of gas exchange Most soluble Least soluble CO2 >>>>>>>>>>>>>>>>> O2 >>>>>>>>>>>>>>>>>>> N2 CO2 is 20 times more soluble than O2 N2 is about half as soluble as O2 Ventilation-Perfusion Coupling Breathing and blood flow are matched to the partial pressure of alveolar gases The Oxyhemoglobin Saturation Curve • Is standardized for normal blood (pH 7.4, 37°C) • When pH drops or temperature rises: – more oxygen is released – curve shift to right • When pH rises or temperature drops: – less oxygen is released – curve shifts to left Oxygen - about 98.5% is bound to hemoglobin (Hb) and 1.5% in solution. Respiratory Gas Transport pH, Temperature, and Hemoglobin Saturation Factors influencing Hb saturation: Temperature Factors influencing Hb saturation: Pco2 and pH The Bohr Effect (1 of 2) • Is the effect of pH on hemoglobin saturation curve • Caused by CO2: – CO2 diffuses into RBC – an enzyme, called carbonic anhydrase, catalyzes reaction with H2O – produces carbonic acid (H2CO3) The Bohr Effect • Carbonic acid (H2CO3): – dissociates into hydrogen ion (H+) and bicarbonate ion (HCO3—) • Hydrogen ions diffuse out of RBC, lowering pH 2,3-biphosphoglycerate (BPG) • RBCs generate ATP by glycolysis: – forming lactic acid and BPG • BPG directly affects O2 binding and release: – more BPG, more oxygen released BPG Levels • BPG levels rise: – when pH increases – when stimulated by certain hormones • If BPG levels are too low: – hemoglobin will not release oxygen Fetal and Adult Hemoglobin Figure 23–22 Fetal and Adult Hemoglobin • The structure of fetal hemoglobin: – differs from that of adult Hb • At the same PO : 2 – fetal Hb binds more O2 than adult Hb – which allows fetus to take O2 from maternal blood CO2 Transport • 7 % dissolved in the plasma • ~ 23% bound to the amine groups of the Hb molecule as carbaminohemoglobin • ~ 70% as bicarbonate ion in the plasma CO2 Transport & Exchange: at the tissues CO2 Transport & Exchange: in the lungs The Haldane Effect Control of Respiration • Gas diffusion at peripheral and alveolar capillaries maintain balance by: – changes in blood flow and oxygen delivery – changes in depth and rate of respiration Quiet Breathing • Brief activity in the DRG: – stimulates inspiratory muscles • DRG neurons become inactive: – allowing passive exhalation Quiet Breathing Figure 23–25a Forced Breathing Figure 23–25b The Apneustic and Pneumotaxic Centers of the Pons • Paired nuclei that adjust output of respiratory rhythmicity centers: – regulating respiratory rate and depth of respiration Respiratory Centers and Reflex Controls Figure 23–26 5 Sensory Modifiers of Respiratory Center Activities • Chemoreceptors are sensitive to: – PCO , PO , or pH 2 2 – of blood or cerebrospinal fluid • Baroreceptors in aortic or carotic sinuses: – sensitive to changes in blood pressure 5 Sensory Modifiers of Respiratory Center Activities • Stretch receptors: – respond to changes in lung volume • Irritating physical or chemical stimuli: – in nasal cavity, larynx, or bronchial tree 5 Sensory Modifiers of Respiratory Center Activities • Other sensations including: – pain – changes in body temperature – abnormal visceral sensations Chemoreceptor Responses to PCO2 Hypercapnia • An increase in arterial PCO 2 • Stimulates chemoreceptors in the medulla oblongata: – to restore homeostasis Hypoventilation • A common cause of hypercapnia • Abnormally low respiration rate: – allows CO2 build-up in blood Hyperventilation • Excessive ventilation • Results in abnormally low PCO 2 (hypocapnia) • Stimulates chemoreceptors to decrease respiratory rate Baroreceptor Reflexes • Carotid and aortic baroreceptor stimulation: – affects blood pressure and respiratory centers • When blood pressure falls: – respiration increases • When blood pressure increases: – respiration decreases The Hering–Breuer Reflexes • 2 baroreceptor reflexes involved in forced breathing: – inflation reflex: • prevents overexpansion of lungs – deflation reflex: • inhibits expiratory centers • stimulates inspiratory centers during lung deflation Protective Reflexes • Triggered by receptors in epithelium of respiratory tract when lungs are exposed to: – toxic vapors – chemicals irritants – mechanical stimulation • Cause sneezing, coughing, and laryngeal spasm Pathology and clinical considerations Common homeostatic imbalances: • COPD (chronic obstructive pulmonary disease) • Asthma • Tuberculosis • Lung cancer Respiratory Performance and Age Figure 23–28 COPD: Emphysema Results: Loss of lung elasticity, hypoxia, lung fibrosis, cyanosis. Common causes: Industrial exposure, cigarette smoking. Tuberculosis At the beginning of the 20th century a third of all deaths in people 20 - 45 were from TB. Antibiotic-resistant strains of Mycobaterium tuberculosis are a growing problem at the beginning of the 21st century. Lung Cancer 90% of lung cancer patients had one thing in common… …they smoked tobacco Fin