* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download GASTROINTESTINAL DRUGS
Psychedelic therapy wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
Orphan drug wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Pharmacognosy wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Prescription costs wikipedia , lookup
Drug interaction wikipedia , lookup
Neuropharmacology wikipedia , lookup
Psychopharmacology wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
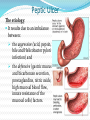
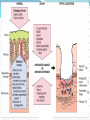
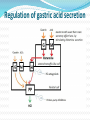
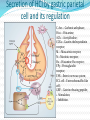
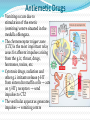
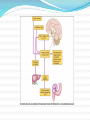
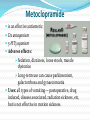
Peptic Ulcer The etiology: It results due to an imbalance between: the aggressive (acid, pepsin, bile and Helicobacter pylori infection) and the defensive (gastric mucus and bicarbonate secretion, prostaglandins, nitric oxide, high mucosal blood flow, innate resistance of the mucosal cells) factors. Regulation of gastric acid secretion Secretion of HCl by gastric parietal cell and its regulation C.Ase.—Carbonic anhydrase; Hist.—Histamine; ACh.—Acetylcholine; CCK2—Gastrin cholecystokinin receptor; M.—Muscarinic receptor; N—Nicotinic receptor; H2—Histamine H2 receptor; EP3—Prostaglandin receptor; ENS—Enteric nervous system; ECL cell—Enterochromaffin-like cell; GRP—Gastrin releasing peptide; + Stimulation; – Inhibition. Peptic ulcer Peptic ulcer is a chronic remitting and relapsing disease lasting several years. The goals of antiulcer therapy are: Relief of pain Ulcer healing Prevention of complications (bleeding, perforation) Prevention of relapse. Drugs for Peptic Ulcer 1. Reduction of gastric acid secretion H2 antihistamines: Cimetidine, Ranitidine, Famotidine Proton pump inhibitors (PPIs): Omeprazole, Lansoprazole, Pantoprazole, Rabeprazole Anticholinergic drugs: Pirenzepine Prostaglandin analogue: Misoprostol 2. Neutralization of gastric acid (Antacids) Systemic: Sodium bicarbonate, Sod. citrate Nonsystemic: Magnesium hydroxide, Mag. trisilicate, Aluminium hydroxide gel, Magaldrate, Calcium carbonate 3. Ulcer protectives: Sucralfate, Colloidal bismuth subcitrate (CBS) 4. Anti-H. pylori drugs: Amoxicillin, Clarithromycin, Metronidazole, Tinidazole, Tetracycline H2 ANTAGONISTS These are the highly effective drugs for acid-peptic disease. Their interaction with H2 receptors has been found to be competitive. Cimetidine was the first H2 blocker to be introduced clinically and is described as the prototype, though other H2 blockers are more commonly used now. Pharmacological actions 1. H2 blockade All H2 antagonists block histamine-induced gastric secretion. They are highly selective: have no effect on H1 mediated responses. 2. Gastric secretion The only significant action of H2 blockers is marked inhibition of gastric secretion. The H2 blockers have antiulcerogenic effect. Gastric ulceration due to stress and drugs (NSAIDs, cholinergic, histaminergic) is prevented. Cimetidine Is absorbed orally Bioavailability is 60–80% It crosses placenta and reaches milk. t½ is 2–3 hr. Adverse effects Headache, dizziness, bowel upset, dry mouth, rashes. Cimetidine (but not other H2 blockers) has: antiandrogenic action, increases plasma prolactin, inhibits degradation of estradiol by liver. High doses given for long periods have produced: Gynaecomastia, Loss of libido, Galactorrhea, Impotence and temporary decrease in sperm count. Ranitidine About 5 times more potent than cimetidine. No antiandrogenic action, does not increase prolactin secretion or spare estradiol from hepatic metabolism—no effect on male sexual function or gynaecomastia. Overall incidence of side effects is lower: headache, diarrhoea/constipation, dizziness have an incidence similar to placebo. Famotidine It is 5–8 times more potent than ranitidine. Antiandrogenic action is absent. Incidence of ADR is low: only headache, dizziness, bowel upset, rarely disorientation and rash. H2 blockers indications The H2 blockers are used to suppress gastric acid secretion. H2 blockers control hyperacidity and symptoms in many patients, but PPIs are the drugs of choice (because of higher efficacy and equally good tolerability). 1. Duodenal ulcer 2. Gastric ulcer 3. Stress ulcers and gastritis 4. Zollinger-Ellison syndrome (It is a gastric hypersecretory state due to a rare tumour secreting gastrin). But PPIs are the drugs of choice. 5. Gastroesophageal reflux disease (GERD) PROTON PUMP INHIBITORS (PPIs) Omeprazole, Lansoprazole, Pantoprazole, Rabeprazole The PPIs have overtaken H2 blockers for acid-peptic disorders. The only significant pharmacological action of PPIs are suppression of gastric acid secretion; without anticholinergic or H2 blocking action. PPIs are a powerful inhibitors of gastric acid: can totally abolish HCl secretion. PPIs inactivate the H+K+ATPase enzyme irreversibly. The specific localization of H+K+ATPase to parietal cells confer high degree of selectivity of PPIs action. Acid secretion resumes only when new H+K+ATPase molecules are synthesized (reactivation half time - 18 hours). At steady-state all PPIs produce 80–98% suppression of 24 hour acid output with conventional doses. Secretion resumes gradually over 3–5 days of stopping the drug. PPIs indications 1. Peptic ulcer: More effective than H2 blockers. Relief of pain is rapid and excellent. PPIs are the drugs of choice for NSAID induced gastric/duodenal ulcers. 2. Bleeding peptic ulcer 3. Stress ulcers 4. Gastroesophageal reflux disease (GERD) 5. Zollinger-Ellison syndrome Adverse effects PPIs produce minimal adverse effects: Nausea, Loose stool, Headache, Abdominal pain, Dizziness On prolonged treatment - atrophic gastritis. Because of marked and long-lasting acid suppression, compensatory hypergastrinemia has been observed. If possible, avoid long-term use of PPIs. No harmful effects of PPIs during pregnancy are known. Though manufacturers advise to avoid, PPIs have often been used for GERD during pregnancy. ANTICHOLINERGICS Atropinic drugs reduce the volume of gastric juice without raising its pH. Effective doses (for ulcer healing) of nonselective antimuscarinic drugs (atropine, etc.) invariably produce intolerable side effects. Introduction of H2 blockers and PPIs has sent them into oblivion. Pirenzepine It is a selective M1 anticholinergic that has been used in Europe for peptic ulcer. Gastric secretion is reduced by 40–50% without producing intolerable side effects, but side effects do occur with slight excess. It has not been used in the USA. PROSTAGLANDIN ANALOGUE PGE2 and PGI2 are produced in the gastric mucosa and appear to serve a protective role by inhibiting acid secretion and promoting mucus as well as HCO3¯ secretion. “Cytoprotective” action - to reinforce the mucus layer covering gastric and duodenal mucosa. Misoprostol is a longer acting synthetic PGE1 derivative which inhibits acid output Reduction of acid production is less than H2 blockers. Is poorer in relieving ulcer pain. Indication: the prevention and treatment of NSAID associated gastrointestinal injury and blood loss. However, it is seldom employed now because PPIs are more effective, more convenient, better tolerated and cheaper. ADR Diarrhoea, Abdominal cramps, Uterine bleeding, Abortion, Need for multiple daily doses. ANTACIDS These are basic substances which neutralize gastric acid. Antacids do not decrease acid production; A single dose of any antacid taken in empty stomach acts for 30–60 min only. Uses Antacids are no longer used for healing peptic ulcer, because they are needed in large and frequent doses. Antacids are now employed only for intercurrent pain relief and acidity, mostly self-prescribed by the patients as over-the-counter drugs. They continue to be used for non-ulcer dyspepsia and minor episodes of heartburn. Systemic Antacids Sodium bicarbonate It is a potent neutralizer, acts instantly, but the duration of action is short. However, it has several demerits: Absorbed systemically: induce alkalosis. Produces CO2 in stomach → distention, discomfort, belching, risk of ulcer perforation. Acid rebound occurs, but is usually short lasting. Increases Na+ load: may worsen edema and CHF. Use of sod. bicarbonate is restricted to casual treatment of heartburn. It provides quick symptomatic relief. Nonsystemic Antacids These are insoluble and poorly absorbed basic compounds. Mag. Hydroxide Magnesium trisilicate About 5% of administered Mg is absorbed systemically— may cause toxicity if renal function is inadequate. All Mg salts have a laxative action. Aluminium hydroxide The Al3+ ions relax smooth muscle. Thus, all Al3+ salts causes constipation. Small amount of Al3+ is absorbed systemically— may cause aluminium toxicity (encephalopathy, osteoporosis) if renal function is inadequate Antacid combinations A combination of two or more antacids is frequently used. 1) Fast (Mag. hydrox.) and slow (Alum. hydrox.) acting components yield prompt as well as sustained effect. 2) Mag. salts are laxative, while alum. salts are constipating: combination may annul each other’s action and bowel movement may be least affected. 3) Gastric emptying is least affected; while alum. salts tend to delay it, mag./cal. salts tend to hasten it. 4) Dose of individual components is reduced; systemic toxicity (dependent on fractional absorption) is minimized. ULCER PROTECTIVES Sucralfate It preferentially and strongly adheres to ulcer base only at acidic pH . Surface proteins at ulcer base are precipitated, together with which it acts as a physical barrier preventing acid, pepsin and bile from contact with the ulcer base. Its action is local(minimal absorption). Sucralfate has no acid neutralizing action. Antacids should not be taken with sucralfate because its polymerization is dependent on acidic pH. ADR are few: constipation, dry mouth and nausea Colloidal bismuth subcitrate (CBS) It is a colloidal bismuth compound; The mechanism of action of CBS: May precipitate (only at pH < 5) mucus glycoproteins and coat the ulcer base. May inhibit H.pylori directly. Uses: as a component of triple drug anti-H. pylori regimen Milk and antacids should not be taken concomitantly. Side effects: Blackening of tongue, dentures and stools Diarrhoea Headache and dizziness ANTI-HELICOBACTER PYLORI DRUGS 90% patients of ulcer have tested positive for H. pylori. All H. pylori positive ulcer patients should receive H. pylori eradication (“extermination”) therapy. Single antibiotic is ineffective (Resistance develops rapidly) Triple therapy: PPIs + 2 antimicrobials oPPI + Amoxicillin+ Clarithromycin oPPI + Amoxicillin+ Metronidazole Quadruple therapy: PPIs + 2 antimicrobials + CBS oPPI + Tetracycline + Metronidazole + CBS Antiemetic Drugs Vomiting occurs due to stimulation of the emetic (vomiting) centre situated in the medulla oblongata. The chemoreceptor trigger zone (CTZ) is the most important relay areas for afferent impulses arising from the g.i.t, throat, drugs, hormones, toxins, etc. Cytotoxic drugs, radiation and other g.i. irritants release 5-HT from enterochromaffin cells → acts on 5-HT3 receptors → send impulses to CTZ The vestibular apparatus generates impulses → vomiting centre EMETICS These are drugs used to evoke vomiting: 1. Act on CTZ : Apomorphine 2. Act reflexly and on CTZ : Ipecacuanha Vomiting needs to be induced only when an undesirable substance (poison) has been ingested. Powdered mustard suspension or strong salts solution may be used in emergency. They act reflexly by irritating the stomach. ANTIEMETICS 1. Anticholinergics Hyoscine 2. H1 antihistaminics Promethazine Diphenhydramine 3. Neuroleptics (D2 blockers) Chlorpromazine Haloperidol 4. Prokinetic drugs Metoclopramide Domperidone Cisapride 5. 5-HT3 antagonists Ondansetron, Granisetron 6. Others antiemetics Dexamethasone Benzodiazepines Dronabinol ANTIEMETICS USES Hyoscine is the most effective drug for motion sickness. Antihistaminics are useful mainly in motion sickness, morning sickness, postoperative forms of vomiting. Neuroleptics act by blocking D2 receptors in the CTZ: Drug induced and postoperative vomiting Disease induced vomiting: gastroenteritis, uraemia, liver disease, migraine, etc. cancer chemotherapy induced vomiting. Radiation sickness vomiting (less effective). Metoclopramide is an effective antiemetic: D2 antagonism 5-HT3 agonism Adverse effects: Sedation, dizziness, loose stools, muscle dystonias Long-term use can cause parkinsonism, galactorrhoea and gynaecomastia Uses: all types of vomiting— postoperative, drug induced, disease associated, radiation sickness, etc, but is not effective in motion sickness. 5-HT3 ANTAGONISTS It is a class of antiemetic drugs to control cancer chemotherapy/radiotherapy induced vomiting Cytotoxic drugs/radiation produce vomiting by causing cellular damage → release of mediators including 5-HT from intestinal mucosa → activation of vagal afferents in the gut → emetogenic impulses to the NTS and CTZ. Side effects: Headache Dizziness constipation Hypotension Bradycardia LAXATIVES (Aperients, Purgatives, Cathartics) These are drugs that promote evacuation of bowels. A distinction is sometimes made according to the intensity of action. Laxative or aperient: milder action, elimination of soft but formed stools. Purgative or cathartic: stronger action resulting in more fluid evacuation. Many drugs in low doses act as laxative and in larger doses as purgative. CLASSIFICATION 1. Bulk forming Dietary fibre: Bran, Psyllium (Plantago), Ispaghula, Methylcellulose 2. Stool softener Docusates (DOSS), Liquid paraffin 3. Stimulant laxative Diphenylmethanes Phenolphthalein, Bisacodyl, Sodium picosulfate Anthraquinones (Emodins) Senna, Cascara sagrada Fixed oil Castor oil 4. Osmotic purgatives Magnesium salts: sulfate, hydroxide Sodium salts: sulfate, phosphate Lactulose MECHANISM OF ACTION Osmotic action- retaining water and electrolytes in the intestinal lumen—increase volume of colonic content and make it easily propelled. Acting on intestinal mucosa, decrease net absorption of water and electrolyte; intestinal transit is enhanced indirectly by the fluid bulk. Increasing propulsive activity as primary action—allowing less time for absorption of salt and water as a secondary effect. ADR Larger doses of stimulant purgatives can cause excess purgation resulting in fluid and electrolyte imbalance. Hypokalaemia can occur on regular intake. Routine and long-term use can produce colonic atony. Steatorrhoea Malabsorption syndrome Protein losing enteropathy. Spastic colitis Osmotic purgatives Saline purgatives are not used now for the treatment of constipation because they are inconvenient/ unpleasant, produce watery stools and after constipation. However, they may be preferred for preparation of bowel before surgery and colonoscopy; in food/drug poisoning and as after-purge in the treatment of tapeworm infestation. TREATMENT OF DIARRHOEAS Rehydration Specific antimicrobial drugs (only in severe disease) Probiotics (BIFILAC, BIFILIN, ENTEROGERMINA) Nonspecific antidiarrhoeal drugs: Absorbants (methyl cellulose) Adsorbants (kaolin, pectin) Antimotility drugs: Codeine Loperamide (IMODIUM) It is an opiate analogue with peripheral μ opioid property. As a constipating agent it is much more potent than codeine. Because of poor water solubility—little is absorbed from the intestines. Entry into brain is negligible—CNS effects occur only with high doses; no abuse liability. ADR: Abdominal cramps and rashes,Paralytic ileus, toxic megacolon.