* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Resistant Staphylococcus Aureus THE EVOLUTION
Leptospirosis wikipedia , lookup
Tuberculosis wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Foodborne illness wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Herpes simplex wikipedia , lookup
Hepatitis B wikipedia , lookup
Gastroenteritis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Antibiotics wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Anaerobic infection wikipedia , lookup
Neonatal infection wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Methicillin-resistant Staphylococcus aureus wikipedia , lookup
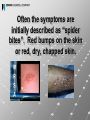
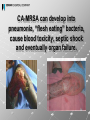
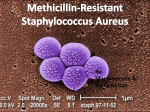
I. MethicillianResistant Staphylococcus Aureus THE EVOLUTION OF BACTERIA© Drug-resistant staph lurks in many places By Anita Manning, USA TODAY Antibiotic-Resistant Staph More Common June 25, 2007; Page B5 Increase In CommunityAssociated Staph Infections Involving Antibiotic-Resistant Bacteria 02 Jun 2007 'Superbugs' Could 'Dwarf' AIDS, Flu CHICAGO and NEW YORK, June 22, 2006 (CBS) Public health officials are becoming increasingly alarmed by the growing number of illnesses caused by antibiotic-resistant staph bacteria. Drug Resistant Staph Bacteria a Global Problem Wednesday, June 21, 2006 Sunday, Jun 18, 2006 Surviving the New Killer Bug A nasty, drug-resistant staph infection--the kind usually seen in hospitals--is racing across the U.S. By CHRISTINE GORMAN MSNBC.com Drug-resistant germs on the rise, doctors warn Study: More Americans acquiring hard-to treat staph infections The Associated Press Updated: 1:59 p.m. ET April 8, 2005 'Superbugs' spread fear far and wide Drug-resistant staph infections no longer threaten just hospital patients, for reasons unknown, they're striking even healthy children and adults Staph infections spreading across the United States as key antibiotic loses punch Posted: Wednesday, Jun 21, 2006 - 03:04:36 pm CDT ASM: Resistant Staph Bacteria Survive on Bed Linen for Days, Keyboards for Weeks By Katrina Woznicki , MedPage Today Staff Writer Reviewed by Robert Jasmer, MD; Assistant Professor of Medicine, University of California, San Francisco Source News Article: CNN, MSNBC, Yahoo! News HICPAC/SHEA Guidelines Debate New Research Estimates MRSA Infections Cost U.S. Hospitals $3.2 Billion to $4.2 Billion Annually Posted on: 05/16/2005 National Prevalence Study of MethicillinResistant Staphylococcus aureus (MRSA) in U.S. Healthcare Facilities June 25, 2007, 12:01 am EDT EXECUTIVE SUMMARY In October and November 2006, the Association for Professionals in Infection and Epidemiology (APIC) conducted a national MRSA prevalence study. … Data show that 46 out of every 1,000 patients in the study were either infected or colonized with MRSA. This rate is between 8 and 11 times greater than previous MRSA estimates. Source: Association for Professionals in Infection and Epidemiology (APIC) II. MRSA ENTERS THE COMMUNITY STAPH (Staphylococcus aureus) In existence for as long as we know, very common and normally harmless. Approx. 35% of population are carriers MRSA (Methicillian-Resistant Staphylococcus aureus) Also called Hospital Acquired (HA-MRSA). Traditionally confined to healthcare settings, first identified in the 1960’s. Requires use of “last resort” antibiotics. CA-MRSA (Community Acquired - Methicillian-Resistant Staphylococcus Aureus) Identified in late 1990’s. No healthcare exposure necessary. Infects normally healthy people. Penetrates skin through open wounds and abrasions. Evolving rapidly. Produces deadly toxin (panton-Valentine leukocidin) in bones, joints, bloodstream and major organs. Current est. up to 52 million carriers - today. Often the symptoms are initially described as “spider bites”. Red bumps on the skin or red, dry, chapped skin. Left untreated, these infections soon become far more severe, invading the body’s organs and bloodstream. At this point, these infections are life threatening. Following photos are very graphic CA-MRSA can develop into pneumonia, “flesh eating” bacteria, cause blood toxicity, septic shock and eventually organ failure. MRSA has developed a resistance to the most common antibiotics, such as; Penicillin Keflex Cephalexin Late 1990’s, MRSA infections were identified in non-healthcare environments, such as: Schools Correctional facilities Athletic teams Health and fitness clubs Military housing Other areas of close quartering APIC estimates that currently up to 5% of the population carries MRSA in their noses – POSSIBLY AS MANY AS 52 MILLION PEOPLE WORDWIDE Source: APIC (Association for Professionals in Infection and Epidemiology) MRSA spreads in the community through: Skin-to-skin contact Cuts and open wounds Abraded or chaffed skin Exacerbated by: Poor hygiene Overcrowded living conditions Communal or shared items Main risk factors: Age Living Conditions Weakened Immune System Activities (ie. contact sports, frequent skin abrasions, exposure to bodily fluids, …) Sharing personal items (ie. Towels, uniforms, clothing, athletic gear, razors, …) Contact with healthcare workers Recent hospitalization Use of certain antibiotics III. WHAT IS NEXT? The next pandemic? Avian (bird) flu SARS Clostridium difficile (C. Diff.) E. Coli Hepatitis A & B HIV Herpes Salmonella Parvo virus IV. PROACTIVE APPROACH “Best offense is a good defense” Where do you need protection? Wherever MRSA thrives! HANDS & SKIN CAFETERIA, COMPUTER ROOM, CLASSROOM … UNIFORMS & TOWELS BED LINENS, COMFORTERS, BLANKETS & PADDING SHOWERS, LOCKER ROOMS, EXERCISE & THERAPY EQUIPMENT How do we stop cross-contamination and infection from bacteria, viruses, spores, fungus …? At the source - we prevent the spread! CLEAN Wash hands Wash environmental contact surfaces Wash clothing, linens, towels, uniforms, equipment… SANITIZE Hands and skin with residual sanitizer Hard surfaces treated with active anti-microbial Washable textiles with residual, self-sanitizing finish HANDS & SKIN FDA Approved Alcohol-free Non- flammable No water or towels required Non-sticky and won’t dry out skin Does not remove protective body oils Greaseless, no-drip FOAM Residual anti-microbial activity Efficacy increases with use Benzalkonium Chloride-based products exhibit increased efficacy with use. Ethyl Alcohol-based products decline in performance! Ethyl Alcohol-based products fall below FDA Minimum Standards within 3 - 4 uses! SURFACES SureClean™ Hard Surface Disinfectant and Sanitizer EPA Registered Disinfectant, Sanitizer, Mildewstat, Fungicide Kills 99.9%, or more of infectious bacteria Broad spectrum (HIV, VRE, MRSA, HBV, HCV, Herpes (Type 1 & 2), Strep, Avian Influenza A) No rinsing required Convenient, Ready-to-use spray Non-acid formulation contains no bleach, phenolics or phosphates Effective in hard water (up to 400 ppm) CLOTHING, BED LINENS, UNIFORMS, TOWELS, … BacStop™ Fabric Sanitizer & Bacteriostat EPA Registered Liquid fabric sanitizer and mildewcide Self-sanitizing finish (continually kills minimum of 99.9% of newly acquired bacteria) Continues working after textiles are laundered (creates a Zone of Inhibition) Eliminates odors due to bacterial growth Easy to use, final rinse treatment Textiles treated with BacStop™ retain a self-sanitizing condition, creating a Zone of Inhibition around the surface area of the textile. Bacteria do not replicate on the surface – and therefore die. Infectious Bacteria Treated Fabric Zone of Inhibition Program for Infection Control Pro-Tex™ Foaming Hand & Skin Sanitizer SureClean™ Hard Surface Disinfectant and Sanitizer BacStop™ Fabric Sanitizer & Bacteriostat DeScent™ Concentrated odor neutralizer An once of prevention