* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download CAR
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Myocardial infarction wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Rheumatic fever wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Aortic stenosis wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Atrial septal defect wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
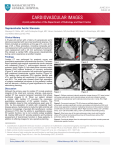
CAR/01(P) UNUSUAL COMPLICATIONS AND MANAGEMENT OF AMPLATZER DEVICE CLOSURE N Chitra, I.B.Vijayalaskhmi, Rajasri, Usha, C.N. Manjunath Children’s Heart Care Centre, Sri Jayadeva Institute of Cardiology, Bangalore [email protected] Introduction: Transcatheter percutaneous device closure of ASD, VSD, PDA, PFO and other unusual shunts like AP window, RSOV is safe, effective, attractive alternative to surgery. Successful closure rate is very high and complication rate is very low. Aim of our study is to know the incidence of very rare and unusual complications of Amplatzer device closure and their management. Material and results: Out of total 136 cases, 42 males, 94 females, youngest - 4 months old, case of PDA weighing 3.9 kgs. Oldest - 65 years old case of ASD. Device closure done in 97 cases of PDA, 33 cases of ASD, 5 cases VSD, one case of ALVT. Thrombus on the device occurred in 2 cases (1.6 %). The patient who developed acute thrombus soon after deployment, developed convulsions, occulogyric crisis, died of shower of emboli to brain within 18 hours after the procedure .Another one, presented with headache and persistent vomiting, 3 weeks after device closure, made complete recovery with antiplatelet and anticoagulants. One patient with multiple VSD closed with single large 14 mm Amplatzer septal occluder, through Jugular approach, developed transverse sinus thrombosis (0.8%). CT angio showed, complete recovery with medical management. Severe intravascular hemolysis after transcatheter closure of a large PDA using the ADO is reported in literature. But none of our PDA patients had this complication. However, severe hemolysis occurred in a case of Aortico ventricular tunnel closed with 16 x14 ADO (0.8 %). Hemolysis subsided after 5 days. Device embolisation into aorta is very rare, as aortic pressure is higher than pulmonary artery. In a case of PDA, severe PH, as soon as the screw was released the device shot into aorta. Device was pushed into left common iliac artery, screw fastened into device and retrieved in a novel way. Though kinking of the sheath occurs often it is overcome easily but multiple acute kinking of introducer sheath making the device closure impossible (0.8%), occurred in a case of Hemivertebrae, absent ribs, severe kyphoscoliosis. Kinking problem was overcome by using Cook’s sheath over the Mullin’s dilator. The device was negotiated by side of guide wire. The wire was withdrawn just before deployment of the device. Conclusion: Success rate of Amplatzer device closure in usual and unusual shunts is very high. The complications are extremely rare. Timely detection of unusual complications and management is crucial in further reducing morbidity and mortality. CAR/02(O) EFFICACY OF ECHOCARDIOGRAPHIC CRITERIA FOR DIAGNOSIS OF CARDITIS IN ACUTE RHEUMATIC FEVER N Chitra, I.B. Vijayalakshmi, O.R.Vishnu Prabhu, R Rajasri, Anuradha Children’s Heart Care Centre, Sri Jayadeva Institute of Cardiology, Bangalore, Karnataka [email protected] Background: Early and precise diagnosis of carditis in Acute Rheumatic Fever (ARF) though difficult is very important to prevent the serious consequences, morbidity and mortality in young. Despite the fact, that echocardiography (ECHO) can diagnose carditis more accurately than traditional auscultatory findings and can prevent both over diagnosis and under diagnosis, it is not included in Jones’ criteria. Therefore there is a great need for ECHO criteria for the precise and early diagnosis of both clinical and subclinical Carditis. Aim: Our study is to propose Echocardiographic criteria and test its efficacy to make precise and early diagnosis of carditis and/or subclinical valvulitis. Material and Methods: 333 Consecutive, suspected cases of ARF, 165 males and 168 females (M:F Ratio 1:1) from January 2005 to June 2006, underwent a detailed clinical examination; laboratory tests and meticulous Echocardiographic and Doppler study. Vijay’s Echo Criteria for the diagnosis of carditis/subclinical valvulitis was used by giving 2 points for each of the eight ECHO features of carditis. Results: Out of 333 cases, 220 (66.06%) were both Jones’ positive and ECHO positive [True +ve], 52 cases (15.61%) probably had subclinical carditis because though clinically murmur was not heard and Jones’-ve the Echo was Positive[False - ve]. Four cases though, clinically were diagnosed as carditis and were +ve by Jones’criteria ,on ECHO showed, Atrial Septal Defect, aorto arteritis with mitral regurgitation, subaortic membrane, myxomatous mitral valve prolapse (MVP) with mitral regurgitation. [False +ve]. Remaining 57 cases (17.11%) who, were Jones’-ve and clinically as well as echocardiographically negative were taken as control group (True –ve). Sensitivity is 81%, Specificity is 93%. Conclusions: Vijaya’s ECHO criteria plays an important role in precise diagnosis of both Carditis and subclinical Valvulitis. These subclinical changes detected only by ECHO, can persist. and probably belong to large group of patients who present later as rheumatic heart disease (RHD) without the past history of ARF and prophylaxis. Therefore ECHO should be included as a major criteria in Jones criteria. CAR/03(P) CHANGING SCENARIO OF CATHETERIZATION IN CONGENITAL HEART DISEASE IN THE LAST TWO DECADES N Chitra , I.B.Vijayalaskhmi, Rajasri, Usha, C.N. Manjunath Children’s Heart Care Centre, Sri Jayadeva Institute of Cardiology, Bangalore [email protected] Background: Recent developments in the field of Pediatric cardiac surgery and Pediatric Cardiology especially non surgical transcather interventions have changed the pre-operative or pre-procedure diagnostic workup of the cardiac malformations. In many centres, this is achieved and based exclusively on Echo findings in some patients. In our centre too, pattern of children taken up for cath study has changed in the 2 last decades. AIM: To determine the impact of changing trends due to advancement in Echo and interventions in children and to know the changing pattern of cath study in CHD . Materials: 2329 cases who underwent cardiac catherization between Jan 1998 to July 2007 formed the material for the study. The percentage of various heart diseases are given below and it was compared with the earlier data of 3790 cases of consecutive catheterizations done in 1981 to 1994 in the same centre. CONGENITAL HEART APRIL 1981- APRIL JAN 1998-July 2007 DISEASE 1994 (No.=3790) (No.=2329) ATRIAL SEPTAL DEFECT 1479 (39%) 225* (9.8%) VENTRICULAR SEPTAL 730 (19.3%) 569** ( 24.8%) DEFECT PULMONARY STENOSIS 377 (9.9%) 198*** (8.6%) PDA 177 (4.7%) 328**** (14.4%) TOF 334 (8.8%) 533 (23.3%) TAPVC/PAPVC 71 (1.9%) 80 (3.5%) COA 62 (1.6%) 47 (2.2%) CTGV 56 (1.5%) 27 (1.3%) RSOV 50 (1.3%) 7 (0.3%) MISCELLANEOUS 388 (10.2%) 270 (11.8%) 88 cases (40%) of ASD, underwent Device closure,** 228 cases (40%) of VSD had PH but operable. Only 49 cases (8.6%) had Eisenmenger complex, 23 cases(4.1%) of small VSDs had significant AR requiring early surgery. In our earlier study 195 (26.7%) cases had Eisenmenger complex, 42 (5.8%) patients had AR. *** 189 patients had Balloon Valvuloplasty, rest referred to surgery due to associated lesions. **** 106 cases of PDA had device closure,165 had coil closure. Intervenions was done in 27.7%. Conclusion: Patients who need cardiac catheterizations has come down drastically, due to improved Echo techniques, hence most are referred to surgery directly without the need for catheterization. However, number of Interventions done has increased tremendously and in a small subset of cases catheterization and angiogram continues to be gold standard. CAR/04(O) BALLOON VALVULOPLASTY FOR CRITICAL AORTIC STENOSIS: INITIAL RESULTS AND MID TERM FOLLOW UP N. Chitra , I.B. Vijayalakshmi, , Rajasri, Usha, C.N. Manjunath, Children’s Heart Care Centre, Sri Jayadeva Institute of Cardiology, Bangalore [email protected] Introduction: Aortic balloon valvuloplasty (ABV) is an effective procedure in critical aortic stenosis (AS), though the results are comparable to those of surgical aortic valvulotomy, the immediate and mid term follow up results vary from centre to centre. In one centre the immediate mortality in infants with AS is as high as 25%. Many centres prefer to do surgery for fear of aortic regurgitation. AIM: of our study is to assess the safety, and efficacy of balloon dilatation of critical AS and to know the immediate and long term follow up. Material and Methods: From January 1997 to July 2007, a total of 156 cases of critical AS, who under went balloon dilatation with Mansfield/Tyshak balloon, formed the material for the study. The youngest patient was one month old and oldest was 25 years. Median age was 5.6 years. Male: Female ratio was 2:1. One full term pregnant lady of Achondroplasia had 178 mm of Hg peak gradient, underwent successful balloon valvuloplasty and on the same evening underwent LSCS. Most of the cases were bicuspid AS. In 5 cases of RHD – as patient had associated Mitral stenosis. They underwent ABV and PTMC simultaneously with good results. One patient had significant LVOT obstruction and on angiogram (akin to infundibular stenosis in PS), which disappeared after successful dilatation of valvar stenosis There were 2 mortalities, one was 1 month sick infant with severe LV dysfunction and another was 14 year old boy with 234 mm of Hg peak gradient, had sub optimal result with first dilatation and when attempt was made with bigger balloon, patient suddenly developed hypotension, bradycardia and died. Most of the cases of bicuspid aortic valve had severe stenosis, with eccentric orifice. The valves were thickened with reduced mobility and had suboptimal results. Mild aortic regurgitation occurred only in 5% of cases. No patient had severe AR. Only one patient came with significant restenosis after 3 years and was successfully redilated. Conclusions: Balloon valvuloplasty for critical aortic stenosis is feasible and safe. Rarely dynamic LVOT obstruction could be detected along with valvar stenosis. It disappears after ABV. ABV has significantly reduced the morbidity and mortality in these children who are at high risk for surgery, as annulus is very small. ABV not only prevents untimely death but also post pones surgery. The dictum in ABV is Good is better than Best. CAR/05(P) PERCUTANEOUS CARDIAC INTERVENTIONS IN INFANTS AND NEONATES IN A TERTIARY CARE CARDIAC INSTITUTE WITH SHORT AND MIDTERM FOLLOW UP Maitri Chaudhuri ,Manisha Chakrabarti,S. Radhakrishnan,Savitri Shrivastava. Escorts Heart Institute,Okhla , New Delhi [email protected] Introduction: Percutaneous cardiac intervention in infants and newborns is lifesaving. Aims and objectives : To study the patient profile, type of intervention,,complications, results & follow up of all infants undergoing percutaneous cardiac intervention in a tertiary cardiac centre between January 2004 to January 2007. Material and Methods : Study type – A nonrandomized , hospital based , retrospective study . Study population - 97 infants ( M-79, F-18), aged 91.69 ± 120. 49days ,weighing 4.6 ± 2.30 (2.2 -11.6 kg) analysed. 64 patients underwent definitive intervention while 33 had palliative procedures.Neonates comprised 47.4% of total. 4 babies were syndromic.Commonest intervention was Balloon atrial septostomy (32.9%) , followed by Balloon aortic valvotomy (21.6%), Balloon pulmonary valvotomy (19.6%), Balloon angioplasty of coarctation of aorta (10.3%) , PDA device /coil closure (14.42%) and post operative MAPCA coiling (1.03%). 20 cases had significant ventricular dysfunction preprocedure requiring inotropes. Preprocedure Prostaglandin E1 infusion required by 15.4% . Results and analysis: There was no procedural mortality. ICU stay was between 2 hours and 36 days due to LV dysfunction , persistent PAH and sepsis. Early follow up (£30 days) - moderate AR in 4 & restenosis requiring redilatation within 1 week in 2. Short term follow up (1month to 3 years) showed event free survival 58%.One death 45 days later from noncardiac cause . 24.74% underwent successful surgery - Arterial Switch (21), Senning’s (2) & BT shunt (1). 5.1% required reintervention for aortic & pulmonary valvar restenosis) & recoarctation of aorta .One patient had persistent PAH controlled with Sildenafil. Conclusion : Cardiac interventions in neonates and infants requires proper diagnosis, stabilization , prompt intervention, followup and surgical coordination for successful outcome. CAR/06(O) TIMELY CLOSURE OF VSD TO PREVENT SUSCEPTIBLE INFANTS FROM FAILURE TO THRIVE AND EISENMENGER SYNDROME - AN INSTITUTIONAL STUDY OF FIVE YEARS Manisha Chakrabarti,Savitri Shrivastava,Parvathi Iyer,K.S.Iyer. Escorts Heart Institute, New Delhi [email protected] Introduction:Ventricular septal defects is an important cause of recurrent pneumonia and failure to thrive in infants.Timely closure of the defect is safe and can prevent growth failure in infants and also Eisenmenger syndrome. Aim: This study was done to see the usefulness of VSD closure in infants . Material and methods:A total of 232 patients with ventricular septal defect,pulmonary arterial hypertension were studied between January 2002-December,2006.Age varied between 2 months to one year,, average of 6 months.Male /female ratio was 2.4:1.Association of Downs syndrome was found in 1 % of patients. Results. All patients were successfully operated. Average ICU stay was 41 hours and hospital stay was 6.5 days. Overall mortality was 0.03%.Predischarge echo and evaluation showed minor residual defects in 2% of cases and only one patient had significant residual defect needing redosurgery at a later date. Conclusion: Hence it can be concluded that VSDs causing large left to right shunts , PAH should be closed within one year of age preferably 6 months so as to improve their developmental outcome and also prevent them from Eisenmenger syndrome at a later date CAR/07(P) COR TRIATRIATUM WITH CONGENITAL VALVULAR PULMONARY STENOSIS AND ATRIAL SEPTAL DEFECT IN AN ASYMPTOMATIC PREADOLESCENT – A RARE CASE REPORT. Pradipta Kumar Swain Associate professor, Pediatrics, Paridasahi, shankarpur, A.D. market, Cuttack- 753012 [email protected] INTRODUCTION: - Cor triatriatum, first described in 1868 by Church1, is an uncommon congenital cardiac anomaly which is found in only 0.1% of patients with congenital heart disease 2. Cor triatriatum results from embryologic failure of the common pulmonary vein to become incorporated into the left atrium, this membrane attaches to the mid portion of the left atrium 3. CASE DISCUSSION: An 7-year-old boy was evaluated in pediatric out patient department for inadequate weight gain. He did not have any symptom related to cardiovascular system. Cardiac examination revealed a systolic ejection murmur on left upper sternal border, and thrill was present. A 2-dimensional transthoracic echocardiogram demonstrated a curvilinear membrane subdividing the dilated left atrium into two chambers with pulmonary veins draining into the proximal chamber; the two chambers were communicating with a single opening in the membrane(Figure1A). The 2 D echocardiogram clearly demonstrates doming and prominent pulmonary valves, typical of congenital pulmonary valvular stenosis(Figure 2). An interatrial communication in the form of small ASD is also noted between the right atrium and true left atrium (Figure 3). A diagnosis of cor triatriatum with ASD and pulmonary vavular stenosis was made. Due to financial constraints child has been waitlisted for surgery and is under regular cardiology follow-up with no symptoms. CONCLUSION:- Cor triatriatum has been associated with other congenital anomalies, but to our knowledge, this is the first case of this constellation in the English literature – cor triatriatum, atrial septal defect and pulmonary valvular stenosis. CAR/08(P) EARLY PICKUP OF RARE CONGENITAL HEART DISEASES SAVING LIVES. Kalyani Pillai, V K Parvathy, G Rajesh Department of Pediatrics, Amala institute of Medical Sciences, Amalanagar Thrissur, Kerala 680555 [email protected] Summary: This paper is presented to highlight the fact that a busy pediatrician should never discount a mother’s history, however improbable it sounds. On investigating these unusual complaints, both the cases had relatively rare congenital cardiac abnormalities. Early detection leads to early surgery & both children are thriving well. Both cases would have had a fatal outcome otherwise. Case 1: paroxysmal feeding difficulty in a neonate A day 28 old newborn was brought with history of feeding difficulty. The mother claimed that the child used to grunt after nursing for a few minutes & then leave the breast showing great discomfort ,cry a lot &become allright within a few minutes.The child had 2-3 such attacks of paroxysmal discomfort. Examination in the outpatient was unremarkable except for a 2/6 systolic murmur.Xray chest revealed marked cardiomegaly—predominantly LA LV.An ECG showed the typical features of anteriolateral infarct (small q waves in lead 1, aVL, qs V2-V3, poor R wave progression). A 2 D Echo confirmed the diagnosis of anomalous origin of L coronary artery from pulmonary artery. Child was referred for surgery which was a success. Case 2: dyspnoea on exertion in a 2yr old. 2yr old child brought to OP by her grandmother.Noticed to get breathless after playing or climbing stairs .Physical examination was unremarkable.Doctor shopping ,as grandma not satisfied . Xraychest The chest X-ray shows evidence of pulmonary venous congestion, prominent pulmonary artery segment, right-sided heart enlargement, double cardiac shadow at right heart border.ECG showed right axis deviation and right ventricular hypertrophy and occasional right atrial hypertrophy.2 D ECHO showed a cortriatrium. In isolated cases of cortiatrium in which timely diagnosis is made surgical mortality is less than1%.This child underwent surgery & is doing well now. CAR/09(P) CLINICO – AETOLOGICAL PROFILE OF CARDIAC FAILURE IN CHILDREN (> 1 month) KK Locham, Manpreet Sodhi, Narinder Singh Deptt. Of Pediatrics, Govt. Medical College / Rajindra Hospital. Patiala.147001 [email protected] Objective: To study clinico-aetological profile of cardiac failure in children (>1 month) Setting and Methods: 31 children above age of 1 month with cardiac failure admitted in Deptt. of Pediatrics, Govt. Medical College Patiala were the subjects of the study. Age, sex, place of residence, chief complaints, detail history, general physical examination and systemic examination findings were noted. X-ray chest, ECG and Color Doppler of heart were done. Results: 18 children were in the age group of 1 month to 3 years followed by 5 cases in the age group of 3-6 years, 2 cases in 6-9 years and 6 cases in > 9 years category. 20 (65%) children presented with breathlessness, 8 had fever, fever and cough was present in 4 cases, 3 each had palpitation and swelling of body parts individually. Cause of cardiac failure was congenital heart disease in 11 (35.5%) children and bronchopneumonia in 10(32.2%) children. Severe anemia was cause of cardiac failure in 7 (22.2%) children. 4 children had acute rheumatic fever and 3 had rheumatic heart disease. Colour Doppler revealed abnormalities in 20 cases. ASD and VSD were reported in 4 and 5 cases respectively. Mitral Regurgitation (MR) alone was observed in 4 cases. MR with Mitral Stenosis (MS) and MR with Aortic Regurgitation (AR) were reported in 3 and 2 cases respectively. 2 children had Transposition of Great Vessels with ASD. Conclusion: Majority of Children presented with breathlessness. Congenital heart disease was cause of heart failure in 35.5% of cases. CAR/10(P) HAART INDUCED CARDIOMYOPATHY Saleha Dhaliat, Sandhya Khadse,Rekha Nair [email protected] Cardiomyopathy is known to occur in HIV positive patients.Zidovudine is largely seen to affect muscle fibres through damage to mitochondria, the energy regulating organelle of the cell.Although the association of AZT with decreased cardiac contractility has been debated , but the data indicates a strong correlation between AZT and development of decreased Left Ventricular performance in HIV patients.(Domanski MJ et al.J Pediatr.1995 Jul;127(1) 137- 46.) AZT withdrawal should be considered in whom cardiomyopathy develops. CASE; 12 years female child diagnosed to be seropositive after the death of the parents in May 2006 and started on HAART in view of CD4 count 114 cells/micrl. Patient was started on three drugs- Zidovudine, lamivudine and Nevirapine. Patient presented after 6 months with signs of cardiac failure. On investigation Hb 11.7 gm%, USG- hepatomegaly with ascites,2D ECHO – dilated LA,LV , with LVEF 20% and decreased Rt ventricular function. Chest skiagram showed cardiomegaly with CT ratio 0.75 ( dating back previous discharge reports cardiomegaly was not then evident) Patient never had any Opportunistic infections.The CD4+ had improved to 1132 cells/micrl. On HAART. So A diagnosis of HAART induced cardiomyopathy was made. So Zidovudine was replaced with Stavudine.