* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Limitations of IABP in Pediatric Patients
Remote ischemic conditioning wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac surgery wikipedia , lookup
Jatene procedure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
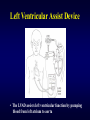
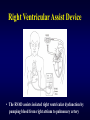
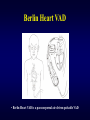
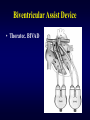
Ventricular Assist Device Seoul National University Hospital Department of Thoracic & Cardiovascular Surgery Acute Heart Failure in Child Etiology • Previous well child with structurally normal heart, most commonly, secondary to acute or fulminant myocarditis (lymphocytic myocarditis) or cardiomyopathy • Childrens, either in the early postoperative, or longstanding myocardial dysfunction with congenital heart disease Acute Heart Failure in child Non-pharmachologic treatment • Balance between myocardial oxygen demand and delivery • Temperature control • Mechanical circulatory support • Intraaortic balloon pump • Cardiopulmonary interaction; role of mechanical ventilation Mechanical Support Indications • • • • • • Acute myocarditis Low cardiac output state after cardiac surgery A bridge to transplantation Overwhelming systemic sepsis with circulatory failure Severe pulmonary hypertension Emergency management of intractable arrhythmia with severely compromised myocardial perfusion, subendocardial ischemia, and acute ventricular dysfunction Ventricular Assist Device Ideal requirements 1. Durable 2. Biocompatible 3. Nonthrombogenic 4. Resistant to infection 5. Reasonably priced 6. Available numerous size Ventricular Assist Device Recent available specification • Centrifugal pump • Implantable pneumatic pulsatile Heartmate(Thermo Cardiosystem) • Paracorporeal ABIOMED BVS 5000 pump(ABIOMED) • Paracorporeal pneumatic pulsatile Thoratec VAD(Thoratec Laboratories) • Paracorporeal pulsatile pediatric VAD System including Berlin Heart VAD(Mediport Kardiotechnik) & MEDOS HIA-VAD System(BYTEC GmbH) • Jarvik 2000 System( Jarvik Research) Intraaortic Balloon Pump Calculation of IABP volume • • • • • • • • CO = HR x SV SV = CO / HR CI = CO / BSA CO = CI x BSA SV = ( CI x BSA ) / HR IABP volume = 0.5 x SV = 0.5 x (CI x BSA)/HR Assume CI = 2.0L/min/square M Then, IABP volume = ( 1000 x BSA ) / HR Mechanical Circulatory Support ECMO 1) ACT time 180-220 sec( around 200 ) 2) Antifibrinolytic therapy Initiation ; 100mg/kg Maintain ; 30mg/kg 3) After congenital heart surgery with hypoxia, pulmonary hypertension, biventricular failure VAD 1) 50ml Biopump less than 10kg 2) 80ml Biopump above 10kg 3) ACT 150-180 seconds ( around 150 ) 4) Simple, less anticoagulative, less blood trauma 5) Platelets above 100,000, normal PT, fibrinogen above 200mg% Extracorporeral Membrane Oxygenation Advantages & disadvantages • Possibility of providing total cardiopulmonary support and allowing for cardiac and pulmonary healing, but needs for higher level of anticoagulation, leads to bleeding, increased blood loss, blood product requirement, multiple exploration, and potential infection Indications • • • • Neonatal respiratory failure Pediatric respiratory failure Neonatal and pediatric cardiac failure Adult cardiorespiratory failure Mechanical Circulatory Support Technical principles • In children, the most common form of VAD involves use of centrifugal pump • Atrial pressure lines are neccessory to monitor for adequate decompression and kept as close to zero as possible to ensure ventricular decompression • All inotropes should be withheld if possible during the recovery period • Serial stress echocardiography should be performed every 1-3 days to document progression of recovery • Decannulation should be performed by gradually weaning VAD support and be a team approach with preparation of volume & catecholamine infusion ready. Mechanical Assisted Circulation Control of blood activation • Surface modifications • Inhibition of initial events Platelet anesthesia Contact phase inhibition Complement inhibition Monocyte inhibition • End-point inhibition Antifibrinolytic drugs Modulation of neutrophil-mediated injury Surface Modifications Methods of modification • Physical modification • Chemical modification by grafting a hydrophilic component • Surface modification by inclusion of bioactive components • Biomembrane mimicry • Cellular seeding and lining Mechanical Circulatory Support Complications • Hemorrhage 1. Local bleeding 2. Major intracranial hemorrhage 3. Coagulopathy and clot formation • Sepsis • Multisystem organ failure • Failure of myocardial recovery • Mortality IABP in Pediatric Patients Limitations 1. Inadequate hemodynamics due to increased aortic elasticity 2. Rapid heart rate with small stroke volume 3. Technical difficulties related to insertion 4. Vascular occlusion of renal, mesenteric artery & limb ischemia 5. Limited applications d/t small balloon VAD for Pediatric Patients Limitations of development 1 Size constraints 2 Differences in pathophysiology of failure 1) Right ventricular failure 2) Biventricular failure 3) Pulmonary failure Ventricular Assist Devices Advantages • Providing good oxygen delivery to the tissue • Unloading the supported ventricle to allow time for ventricular healing • Lower levels of anticoagulation than the ECMO Disadvantages • Bleeding complication • Potential pulmonary dysfunction necessitating conversion to ECMO • Potential for infection • Require a median sternotomy for direct access Left Ventricular Assist Device • The LVAD assists left ventricular function by pumping blood from left atrium to aorta Right Ventricular Assist Device • The RVAD assists isolated right ventricular dysfunction by pumping blood from right atrium to pulmonary artery Berlin Heart VAD • Berlin Heart VAD is a paracorporeal air-driven pulsatile VAD Jarvik 2000 System • Javik 2000 is an intraventricular axial flow impeller pump requiring percutaneous electric power of possible implanted battery power Biventricular Assist Device • Thoratec. BIVAD Extracorporeral Membrane Oxygenation Cardiopulmonary Support System Cardiopulmonary Support System • Cardiopulmonary Support System are actually modified ECMO circuits, have been used for rapid resuscitation during acute cardiac and pulmonary failure, designed as highly mobile units that offer the high-risk cardiac patient a safety net especially in the interventional cardiac catheterization. • There are two potential disadvantages with this system; limited oxygenator durability and an increased potential for air embolism. • Advantages over conventional ECMO includes rapid set-up time with a bloodless prime, decreased postoperative blood loss, and simplified transport.