* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Emerging Infections: Perfect Storm of Vulnerability and
Survey
Document related concepts
Onchocerciasis wikipedia , lookup
Epidemiology of HIV/AIDS wikipedia , lookup
Ebola virus disease wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Tuberculosis wikipedia , lookup
Marburg virus disease wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Bioterrorism wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Antiviral drug wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Transcript
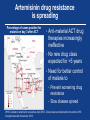
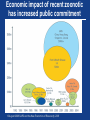
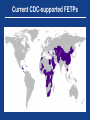
Emerging Infections: Perfect Storm of Vulnerability and Unprecedented Opportunity for Progress Thomas R. Frieden, MD, MPH Director Centers for Disease Control and Prevention December 11, 2012 “Pathogenic microbes can be resilient, dangerous foes. Although it is impossible to predict their individual emergence in time and place, we can be confident that new microbial diseases will emerge.” – IOM, 1992 Perfect storm Something old Rates per 100,000 population Despite progress, TB sickens 8.7 million people a year and kills 1.4 million … and incidence is declining only slowly Estimated incidence rate including HIV-positive TB Stop TB Partnership targets Stop TB Partnership targets Estimated incidence rate of HIV-positive TB WHO. Global Tuberculosis Control: WHO Report 2012. Why is TB incidence falling only gradually? • Bad DOTS? Continued spread (rain) • Implication: Improve diagnosis, treatment, and infection control • Reactivation: Waves crashing on beach • Implication: • Preventive treatment, with research into new ways to identify and treat those most likely to reactivate past infection • Persistence and recognition that results may not be immediate • Need for social change • Implication: Sustainable long-term change Infectious diseases continue to spread from food, water, and health care • Food- and waterborne disease • Billions of illnesses and >4M deaths/year • Healthcare-associated infections (lack of basic hygiene, e.g., hand washing, sterilization) • Affects ~1 in 20 patients in U.S. (hundreds of millions of people/ year) • Increasingly resistant organisms Something new Enormous costs of AIDS • Detection delayed 80 years • Detected only after imported to and established in U.S. • Epidemic 30 years and counting • 30M lives lost, another 33M living with HIV • $100B in costs to low- and middle-income countries alone • HIV deaths in U.S. have decreased – but HIV has already killed more Americans than died in every war since the Civil War PEPFAR: Creating an AIDS-free Generation PEPFAR now • Gives life-saving treatment to >4.5M people • Has prevented >800,000 infants from becoming infected • Is supporting scale-up of voluntary male medical circumcision for nearly 2M by end of year, preventing hundreds of thousands of infections in future years • Has strengthened health systems, increased vaccination rates and decreased maternal and child mortality Declining per-patient treatment costs to PEPFAR with scale-up, 2005‒2011 $1,200 4,500,000 PEPFAR per-patient annual treatment cost 4,000,000 $1,000 3,500,000 $800 3,000,000 2,500,000 $600 2,000,000 $400 1,500,000 1,000,000 $200 No. of PEPFAR direct ART patients 500,000 $- 0 2005 2006 2007 2008 2009 2010 2011 Note: Per-patient cost to PEPFAR is estimated as total treatment allocation divided by the lagged count of PEPFAR directly supported patients West Nile virus spread nearly nationwide, 1999—2002 Aedes aegypti range expanded greatly after control programs ended Illustration: PAHO/WHO 2002 Zoonoses cause more than 2 billion illnesses and 2 million deaths per year Zoonotic pathogens passed from wildlife to humans. From lowest occurrence (green) to highest (red) Jones KE, et al. Global trends in emerging infectious diseases. Nature 451, 990-993(21 February 2008) Outbreaks reported by WHO, 1996—2009 More than half occurred in Africa Source: Chan EH, et al. Global capacity for emerging infectious disease detection, December 14, 2010, 107:50, pp. 21701-21706; www.pnas.org/cgi/doi/10.1073/pnas.1006219107 Note: Points mark reported origin of outbreak or, if unknown, where highest reported morbidity/mortality rates were recorded. Global aviation network Disease can spread nearly anywhere within 24 hours Source: Kilpatrick AM, et al. Drivers, dynamics, and control of emerging vector-borne zoonotic diseases. The Lancet 380:9857, 1-7 Dec 2012, pp. 1946-55. www.sciencedirect.com/science/article/pii/S0140673612611519 Note: Air traffic to most places in Africa, regions of South America, and parts of central Asia is low. If travel increases in these regions, additional introductions of vector-borne pathogens are probable. Something resistant Artemisinin drug resistance is spreading Percentage of cases positive for malaria on day 3 after ACT • Anti-malarial ACT drug therapies increasingly ineffective • No new drug class expected for >5 years • Need for better control of malaria to • Prevent worsening drug resistance • Slow disease spread WHO. Update on artemisinin resistance, April 2012. Circles represent data before November 2010; triangles data after November 2010. Organisms with extensive or potentially complete resistance • M. tuberculosis • P. falciparum • N. gonorrhoeae • Carbapenem- resistant Enterobacteriaceae • K. pneumonia • Others Something to turn you blue Biological innovation – and risk • Potential intentional or unintentional creation or release of • More virulent • More resistant • Vaccine-evading • Higher Ro organisms • Both high-technology and low-technology means of creating • Barriers to entry and costs of bioengineering are dropping Unprecedented opportunity for progress 1. Global commitment • SARS and other infectious disease costs • International Health Regulations — window of opportunity for accountability for progress • Real progress – success leading to success 2. New technologies • Lab • Communication • Informatics “A robust public health system… is the best defense against any microbial threat.” – IOM, 2003 Global commitment Economic impact of recent zoonotic has increased public commitment 12 August 2008.SARS and the New Economics of Biosecurity, 2003 Many countries can contribute Influenza investments in Thailand $35 $30 Millions $25 $20 $15 $10 Thai investment $5 CDC investment $0 2004 2005 2006 2007 2008 2009 2010 2011 Progress: success to success Post 9/11 – progress in preparedness Before 1999-2001 After 2001 CDC doesn’t fund all states for public health preparedness CDC funds all states No national stockpile Few states have plans to handle stockpiled assets Strategic National Stockpile in place All states have plans CDC performs all tests to detect and confirm presence of biological threat agents No secure system to share information about emerging health threats CDC coordinates state and local response efforts from outdated emergency operations center 150+ labs can perform tests Secure, web-based system in place (Epi-X) CDC operates emergency operations center 24/7/365 to monitor health threats and coordinate emergency response Time from outbreak start to outbreak discovery is shrinking Source: Chan EH, et al. Global capacity for emerging infectious disease detection, December 14, 2010, 107:50, pp. 21701-21706; www.pnas.org/cgi/doi/10.1073/pnas.1006219107 H1N1 public health response saved lives • Tracking • 38M emergency department visits tracked: >100,000/day • ~650,000 virus specimens tested at participating WHO collaborating laboratories in U.S., with >4,000 H1N1 isolates sequenced • Communication: Up to 8M page views a day on cdc.gov • Vaccination and treatment • ~330,000 vaccine shipments to ~67,000 sites • Vaccination prevented >1M cases • Vaccination and treatment prevented ~17,000 hospitalizations and ~850 deaths Despite Haiti earthquake and cholera, HIV testing/treatment increased steadily APR 10 90,000 80,000 Earthquake 50,000 70,000 40,000 60,000 38,500 30,000 20,000 FY12 (Oct-Jun) 61,000 60,000 40,000 100,000 APR 11 Cholera peak 50,000 40,000 30,000 20,500 20,000 10,000 # cholera cases per month # of HIV tests completed per month # of patients on ART (current/cumulative) 70,000 10,000 0 0 April 2009 2009 Cholera cases Jan 2010 2010 Jan 2011 2011 Total HIV tests completed Jan 2012 2012 June 2012 Current # patients on ART Progress in Ebola outbreak detection and response, Uganda • Uganda Virus Research Institute upgraded biosecurity and biosafety • Improved testing/monitoring for Ebola outbreak Year Response timeline No. of cases 2000 38 days from 1st known case to preliminary investigation 425 2007 2.5 months from 1st known case to preliminary investigation 131 2011 1 day between case confirmation and response 1 confirmed case 2012 2 days between lab confirmation & response (but 38 days between index death & response – need for quicker response even in absence of lab confirmation) 24 cases, 16 deaths Increasing response capacity in Global Disease Detection Regional Centers 1000 400 Respond to outbreaks 800 911 Train public health leaders 376 300 376 600 200 400 100 200 147 0 2006 80 2007 2008 2009 2010 2011 Detect pathogens not previously known to be in the area 66 60 0 2006 34 220 2007 2008 2009 2010 Build laboratory diagnostic capacity 200 180 2011 202 160 140 120 40 100 80 60 20 40 3 0 2006 20 2007 2008 Numbers are cumulative 2009 2010 2011 11 0 2006 2007 2008 2009 2010 2011 Global Disease Detection Regional Centers Field Epidemiology Training Programs • 2-year, full-time postgraduate program • Modeled after CDC’s Epidemic Intelligence Service • Since 1980, 41 FETPs trained >2,600 epidemiologists • Residents assigned to positions that provide epidemiologic service to MOH • >80% stay in-country after graduating • Effective, low-cost, practical – but has trained only small proportion of numbers needed Current CDC-supported FETPs Strengthening global lab capacity • Concrete aspect of strengthening health systems at national, referral, and clinical levels • Sustainable, accredited labs • Coordinated epidemiology and lab development • Point of care tests expanding, potentially low cost • Multi-pathogen assays for rapid detection and response, as well as surveillance Vaccination saves >3 million lives worldwide each year Categories Vaccines Lives saved/globally/year Existing, widely used vaccines • Measles • Pertussis • Polio Lives saved, compared to pre-vaccine era • Measles: 2.5M • Pertussis: 687,000 • Polio (paralytic cases prevented): 350,000 Vaccines being scaled up • Human papillomavirus (HPV) • Pneumococcus • Rotavirus Potential additional lives saved: • HPV: 275,000 women • Pneumococcus: 1.6M • Rotavirus: 450,000 Potential new vaccines • HIV • Malaria • TB Potential lives saved: • HIV: 1.7M • Malaria: 780,000 • TB: 1.4M Sources: All sources from WHO HPV and rotavirus source: GAVI Alliance, 2012 The world is closer than ever to polio eradication Data as of 20 Nov 2011 and 2012; source: www.polioeradication.org A Safer U.S. and a Safer World A safer U.S. and a safer world Detect threats early • Surveillance systems • Lab systems to characterize pathogens • Trained disease detectives • Facilities to investigate outbreaks Respond effectively • Interconnected emergency operations centers and response capacity • Improved border safety, quarantine measures, and rapid response Prevent avoidable catastrophes • Safer food and drug supply • Reduced pace of drug resistance • Safer, more secure labs working with dangerous pathogens Centers for Disease Control and Prevention 1600 Clifton Road NE, Atlanta, GA 30333 Phone: 1-800-CDC-INFO (232-4636)/TTY: 1-888-232-6348 E-mail: [email protected] Web: www.cdc.gov