* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pneumonia
Cryptosporidiosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Gastroenteritis wikipedia , lookup
Typhoid fever wikipedia , lookup
Orthohantavirus wikipedia , lookup
Henipavirus wikipedia , lookup
West Nile fever wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Hepatitis C wikipedia , lookup
Schistosomiasis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Neonatal infection wikipedia , lookup
Tuberculosis wikipedia , lookup
Leptospirosis wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Swine influenza wikipedia , lookup
Hepatitis B wikipedia , lookup
Antiviral drug wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Whooping cough wikipedia , lookup
Influenza A virus wikipedia , lookup
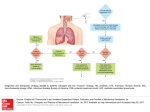
Pulmonary Infectious Disease Tory Davis, PA-C Pneumonia What is it? – Acute infection of the lung parenchyma, including alveolar spaces and interstitial tissue – Alveoli fill with exudate (pus), fibrin, cells – Usually bacterial or viral infection – May be fungi, rickettsial, yeasts, parasites Classification of Pneumonia “Typical” vs. “Atypical” By site of acquisition (ie where the pt picked up the bug) By location in lung Other pt factors (such as imunocompromised, HIV-associated, aspiration) General Info Community acquired pneumonia (CAP)- 2-3 million cases per year Most deadly infectious disease in US 6th leading cause of death in US 60,000 deaths annually Worldwide: leading cause of death in children Community Acquired Pneumonia (CAP) Definition – Onset outside hospital or diagnosed within 48 hours of admission in a patient who has NOT been in long-term care facility for 14d prior to symptom onset AND who does not meet the criteria for health-care associated pneumonia (HCAP) HAP & VAP Hospital Acquired pneumonia – New infection occurring 48 hours or longer after hospital admission Ventilator Associated Pneumonia – 48-72 hours after endotracheal intubation HealthCare Associated Pneumonia (HCAP) Infection occurring within 90 days of a 2-day or longer hospitalization In nursing home or long-term care residence Within 30 days of IV abx therapy, chemotherapy, wound care or hemodialysis in a hospital or hemodialysis clinic Pneumonia in any pt in contact with a multidrug-resistant pathogen HCAP Includes many pts who used to be considered CAP Newer evidence suggest that pts with HCAP are more like pts with HAP (than CAP) and may need HAP-like treatments Other things to consider Aspiration pneumonia- who would get this? Opportunistic organisms- such as Pneumocystis jerovecii pneumonia (seen only in immunocompromised patients.) Classify by Location Primarily from x-ray observation Lobar pneumonia- Entire lobe Segmental or lobular pneumonia (segment of lobe) Bronchopneumonia- (alveoli contiguous with bronchi) Interstitial pneumonia- (Involvement of tissue between the alveoli) Common Signs and Symptoms Fever Cough sputum Dyspnea Chills/Rigors Diaphoresis Chest pain Abd pain Pleurisy Hemoptysis Fatigue Myalgias Arthralgias Anorexia Headache Typical Presentation Sudden onset fevers, cough with purulent sputum, dyspnea, occasional pleuritic chest pain Signs of consolidation, x-ray abnormalities Usually caused by more common bacteria: – Pneumoccocus, H. influenza, etc. Remember Clinical Assessment? Consolidation: – tactile fremitus (“Ninety-nine”) – Bronchophony (Auscultate “Ninety nine”) – sounds like listening without stethoscope – Egophony (EA changes) – Rales (crackles) Associated pleural effusion: – tactile fremitus – Distant breath sounds – Pleural friction rub (creaking leather) Atypical Presentation Gradual onset, dry cough, myalgias, fatigue, sore throat, N/V, diarrhea, dyspnea Less remarkable pulmonary exam despite abnormal x-ray findings Organisms: Mycoplasma pneumoniae, Legionella pneumophila, Chlamydia pneumoniae, Chlamydia psittaci, Francisella tularensis, viruses Pathogenesis Some combination of: – Defect in normal host defenses, which include: Cough reflex Mucociliary clearance system Immune response – Very large infectious inoculation – Highly virulent pathogen Mechanism of spread Most common – Inhalation of droplets small enough to get to alveoli – Aspiration of secretions from upper airways Other – Hematogenous or lymphatic dissemination – Direct spread from nearby infection Predisposing factors URI Smoking Alcoholism – dec immune fxn and inc aspiration Institutionalization Heart failure COPD Age extremes Debility or consciousness Immunocompromise (including CRF, DM) Dysphagia What’s Buggin’ Ya? Community Acquired (CAP)- bacterial – Streptococcus pneumoniae (pneumococcus) 20-60% of CAP – Haemophilus influenzae (H. flu) – Mycoplasma pneumoniae – And a bunch of others What’s Buggin’ Ya 2 Viral – Infants and children: major pulmonary pathogens are VIRAL: RSV, parainfluenza, influenza A and B – Adults: influenza A (B less often), rare varicellazoster Fungal: Histoplasma capsulatum, coccidiodies immitis, blastomyces dermatitidis, cryptococcus neoformans, aspergillus fumigatus, pneumocystis carinii/jerovecii Rickettsial: primarily Coxiella burnetii What’s Buggin’ You Worse? HAP/HCAP – – – – Enteric aerobic gram-negative bacilli Pseudomonas aeruginosa S. aureus (includng MRSA) Oral anaerobes HIV Infection-Associated – – – – Pneumocystis jerovecii M. tuberculosis S. pneumoniae H. influenzae Demographics Aids Diagnosis Influenza assoc with community outbreaks – Typical pneumonia outbreak after flu outbreak Legionella: exposure to aerosolized water vapor (cooling systems) → outbreak Mycoplasma in younger pts in conjugate settings (college, military), with slow transmission Chlamydia psittaci in bird handlers, Tularemia from cute bunnies, Anthrax from pigs… Pneumococcal pneumonia Caused by Streptococcus pneumoniae (>80 serotypes) Most common cause of bac-t pnu Most frequent in winter Most common in age extremes Inhaled/aspirated pneumococci lodge in alveoli. Inflammatory process in alveolar spaces, causes accumulation of protein-rich fluid which is great growth medium for bac-t, helps them spread to nearby alveoli Pneumococcal S & S Often preceded by URI Sudden onset with SINGLE shaking chill, followed by fever up to 40.5º, pleurisy, cough, dyspnea Tachypnea with RR rising to 20-45 Tachycardia P 100-140 Can have: n/v, malaise, myalgias Cough initially dry, progresses to producing purulent, rusty or blood streaked sputum Exam may show signs of lobar consolidation or pleural effusion (know exam signs) Complications Progressive pneumonia Respiratory distress Septic shock Contiguous infections Bacteremia extrapulmonary infections PrognosisPneumococcus Pneumococcus accounts for 85% of lethal CAP cases Overall, 10% mortality Poor prognostic markers: – – – – – – – – – age <1 or >60 positive blood cx involvement of >1 lobe low WBC count extrapulm complication immunosupression CHF Cirrhosis asplenia Staphylococcal Pneumonia 2% of CAP, 10-15% of HAP/HCAP are caused by Staph aureus Risks: age extremes, hospitalized pts, intubated, tracheostomy, immunosuppressed, recent surgery, pts with cystic fibrosis, IVDU (who are prone to tricuspid valve endocarditis with resultant embolic pneumonia) CXR- multiple bilateral nodular infiltrates with central cavitation Staph Aureus S & S Similar to pneumococcus, except: – Recurrent rigors (vs single chill) – Tissue necrosis and abscess formation – Empyema common- suspect S. aureus in post thoracotomy empyema or an empyema complicating chest tube drainage s/p chest wall trauma – Fulminant course with prostration Staph Aureus prognosis Mortality 30-40%, often (but not always) due to serious associated conditions – Can be lethal in previously healthy adult who develops Staph superinfection after influenza Slow response to abx, prolonged convalescence Gram Negative Bacilli Account for <2% CAP, but the majority of HAP/HCAP pneumonias Klebsiella, Pseudomonas aeruginosa, Escherichia coli, Enterobacter sp, Proteus sp, Acinetobacter sp Rare in healthy adults Seen in infants, elderly, alcoholics, debilitated/immunocompromised hosts, esp those with neutropenia Bronchopneumonia similar to other infections, except: very high mortality 2550% despite abx Klebsiella pneumoniae CAP in alcoholics, common HAP Frequent abscess formation causes Friedlander’s pneumonia- affects upper lobes, produces current jelly sputum, tissue necrosis, early abscess, and fulminant course CXR- “bulging fissure” sign. Upper lobar consolidation with bowing fissure, also abscess and lung necrosis Pseudomonas aeruginosa Common VAP pathogen Seen in neutropenic, intubated, ICU or burn unit pts, CF, AIDS High mortality CXR- microabscesses coalescing into large abscesses Haemophilus influenza 2nd most common cause of CAP (when bug is ID’d) Strains containing type B polysaccharide capsule most virulent; cause meningitis, epiglottitis, bacteremic pneumonia. Nearly gone in US due to HiB vaccine. Non-type B strains colonize lower resp tract of pts with chronic bronchitis, implicated in exacerbations (thus abx in bronchitis in pts w/ COPD) H. influenza Hib pneumonia usually in kidsmedian age 1 year – esp if not immunized Usually proceeded by coryza Early pleural effusion in 50% In adults, presentation similar to other bac-t pneumonias Bacteremia and empyema uncommon Legionnaire’s Disease Pneumonia caused by Legionella pneumophilia. Discovered in members of American Legion during 1976 convention in Philadelphia. 1-8% of CAP and 4% of lethal nosocomial cases. Occurs in late summer, early fall. Caused by aerosolization of contaminated water source, spread by AC systems or shower heads. Risk factors: smoking, etoh abuse, immunosuppression Legionella Incubation 2-10 days Prodrome resembles influenza: malaise, fever, myalgia, headache, cough- initially non-productive, then productive of mucoid sputum Characteristic high fever, relative bradycardia, commonly diarrhea Less common: altered mental status Legionella CXR shows patchy segmental or lobar infiltrate, unilateral progressing to bilateral, often with pleural effusion. Abnormalities persist Labs: leukocytosis, hyponatremia, hypophosphatemia, abnl LFTs Mortality >15% in CAP, higher in hospitalized or immunosuppressed pts Slow convalescence Mycoplasma pneumoniae Most common pathogen in ages 5-35 “Walking pneumonia” Slow spreading epidemics due to incubation time of 10-14 days. Spread common thru close contacts, closed populations such as military, families, PA students Attaches to and destroys ciliated epithelial cells of respiratory tract mucosa M. pneumoniae Initial sx are flu-like: malaise, sore throat, dry cough with progressive severity Gradual progression (vs fast onset of “typicals”) Coughing may be paroxysmal, produces mucoid, mucopurulent, or blood-streaked sputum Acute sx 1-2 weeks, then slow recovery. Often mild sx, spontaneous recovery usually- pts will recover with or without treatment M. pnemoniae Prolonged cough due to inhibition of ciliary action Exam: unimpressive, esp compared to pt complaint and xray findings Prognosis good. Abx tx will fever and pulm infiltrates and recovery speed- BUT pts will continue to carry mycoplasma for weeksNB! Mycoplasma doesn’t have cell wall, and therefore won’t respond to abx that interfere with cell wall-go with macrolides Chlamydia pneumoniae 5-10% of CAP and nosocomial pnu in adults. May be provocative for asthma Resembles Mycoplasma pneumoniae symptoms Cough, sputum, fever- most not seriously ill, but can require admit Older kids, young adults usually Chlamydia psittaci Bird handler’s pneumonia Clinically and antigenically distinct from C. pneumo Atypical pneumonia transmitted to humans by psitticine birds via inhalation of dust from feathers, excreta or by bite Clinically similar to other “atypicals”, plus epistaxis, splenomegaly CXR- Pneumonitis radiating from hilum Pneumocystis jerovecii Fungal agent (previously thought to be parasite) and previously called P. carinii causes pnu only in immunocompromised pts S&S: fever, dyspnea, nonproductive cough. Evolves over days to weeks CXR- diffuse bilateral perihilar infiltrates, but 20-30% of CXR are normal PCP/PJP and HIV/AIDS 30% of HIV+ pts get PCP/PJP as initial AIDS defining illness Become vulnerable when CD4 count <200 80% of AIDS pts will get PCP if not prophylaxed, usually with TMP/SMX (Bactrim) 80/400 mg daily starting when CD4 count hits 200 Post-Op/ Post-traumatic Hypoventilation Poor diaphragmatic excursion Impaired cough reflex Bronchospasm Dehydration Combine to cause retention of bronchial secretions, segmental atelectasis, and ultimately pnu Aspiration 3 syndromes from aspiration – Chemical pneumonitis (when aspirated material is directly toxic, i.e. gastric acid) – Mechanical obstruction (“So you inhale a meatball…”) – Bacterial pneumonia caused by anaerobic bacteria colonizing oropharynx. CXR will show infiltrate in whatever lung segment was dependant at time of aspiration. Workup Hx and PE – good psx hx CXR- PA and Lateral CBC with diff BMP (glucose and lytes) Liver function tests (LFTs) – Remember CMP=BMP+LFTs Renal function Pulse ox &/or ABG What else? Consider EKG, HIV test If immunocompromised pt, consider other causes: fungal, viral, TB, PCP Flu season: rapid flu test with back-up culture PORT severity index Prediction model for prognosis of CAP Scoring system based on 19 variables – Demographics – Comorbid disease – PE Findings – Lab findings PSI Risk stratification for death from all causes in next 30 days – Class I (by algorithm) LOW (outpt tx) – Class II 70 points LOW (outpt tx) – Class III 71-90 points LOW (consider admit) – Class IV 91-130 MODERATE (admit, maybe intermediate care) – Class V >130 HIGH (likely ICU) Other Admission Considerations Virulence of organism if known (S. aureus) Support at home and functional status Ability to comply with medications Ability to afford treatment Immune status Multilobar involvement Follow-up Clinical judgment paramount Drugs Tx with abx usually initiated before ID of causative agent, then modified Outpatient tx usually empiric (= guided by practical experience) Often institutions have rotating schedule of 1st choice abx Treat pneumococcus PLUS other likely bugs Antibiotics for Pneumonia Choose least-toxic, most cost-effective, narrowest spectrum possible Penicillin was mainstay anti-pneumococcal – BUT 40% resistance in many locales – If you know resistance rates in your community, can consider its use IDSA Guidelines for outpts: – Macrolide (e.g. azithromycin, clarithromycin) – Doxycycline – Fluoroquinolone: (levofloxacin, moxifloxacin, gatifloxacin) IDSA Antibiotics for Pneumonia Hospitalized pts: – Fluoroquinolone, or – Ceftriaxone (or cefotaxime) plus macrolide ICU pts: – Fluoroquinolone or macrolide plus ceftriaxone or cefotaxime or ampicillinsulbactam or piperacillin-tazobactam Antibiotics Switch to oral Abx when clinically stable Afebrile 8 hrs, nl resp rate, reduced oxygen requirement, wbc Fluoroquinolones same bioavailability (IV and oral) Treat for 7 to 14 days total Other Therapies IV fluids Oxygen Incentive spirometry Anti-pyretics like acetaminophen Cough suppressants and mucolytics Chest physical therapy PT/OT and consider rehab hospital Preventing Pneumonia Infection control: handwashing, cleaning, gloves, isolate if indicated, treat promptly Chemoprophylaxis: antivirals during flu outbreaks, TMP-SMZ for PCP prevention Vaccinations Aspiration precautions Incentive spirometry post-op Follow up Consider repeat CXR in 4-6 weeks to demonstrate resolution of imaging findings. Opportunity to address risk factors, possibly modify them Great time for intervention with smokers Acute Bronchitis What is it? Inflammation of tracheobronchial tree Usually infectious, but can also be irritant Often occurs in relation to other respiratory illness (ie common cold) 5% of US population dx with bronchitis yearly Tends to be self-limited Bronchitis is not pneumonia – Infection of bronchial tree by similar organisms but no parenchymal infection Cough, sputum, upper respiratory symptoms No lung findings except wheeze, nl xray – Usually viral infection, rarely bacterial (* see Pertussis) Pathogenesis Infectious – Viral: adenovirus, influenza, parainfluenza, rhinovirus – Bacterial: chlamydia, pertussis Noninfectious – GERD – Irritant – Asthmatic Risk Factors for Infectious Bronchitis Recent URI Recent LRI Smoker Lung compromise, ie: COPD Symptoms Cough (+/- purulent) Fever Malaise Nasal congestion +/- rhinorrhea Sore throat Looks a lot like a cold so far… More sx Wheeze Dyspnea Chest pain-costochondritis inflammation from coughing so much (press on it by sternum to elicit pain) Myalgia/arthralgia Physical exam No uniform description Can be normal exam +/- wheeze/rhonchi No signs of consolidation – Because if there IS consolidation, it’s NOT bronchitis DDX Asthma COPD Bronchiolitis Croup Pneumonia Bronchiectasis Influenza TB Cancer Foreign body URI Sinusitis Work up Thorough history PE CXR? – can r/o pneumonia if you can’t do it with hx and PE Treatment Generally aimed at symptoms: Analgesics Antipyretic Anti-inflammatory Antitussives Expectorants Bronchodilators “but my doc always gives me….” In immunocompetent individuals, no abx needed. BUT 80% get them. Who should get abx? Moderate-severe COPD Asthma…maybe Immunocompromised pts Suspected pertussis NB! <5% of bronchitis pts will develop pneumonia. “Prophylactic” antibiotics will NOT decrease incidence of pneumonia ABX Macrolides effective against mycoplasma chlamydial organisms and B. pertussis – Erythromycin, Clarithromycin, Azithromycin Also tetracyclines, tmp/smx (Bactrim), and cefditoren (Spectracef) Prevention Stop smoking Influenza vaccines Stop smoking Tdap vaccine Stop smoking Cover that cough Stop smoking Pneumococcal vaccine And WASH YOUR HANDS Pertussis Pertussis aka whooping cough Classic: at least 21 days of cough illness with paroxysms, associated whoops or posttussis vomiting Bordatella Pertussis: highly contagious gram neg bac-t in respiratory tract, spread by direct contact with secretions Incubation 7-10 days Pertussis Phases Catarrhal (1-2 weeks) Looks like URI, rhinorrhea, sneezing, fever, occasional cough Paroxysmal-severe spasms of quick, short, coughs like a machine gun without breathing in between coughs. Gagging and gasping. After cough spasm, pts strain to inhale, making high-pitched whooping sound. May be followed by vomiting and exhaustion Convalescent- Gradual recovery Pertussis Nearly eradicated in 70s (1,000 cases in 1976), now increased incidence (11,000 in 2007) Waning immunity, under-vaccination Infants at greatest risk for complications: apnea, pneumonia, seizures, brain damage, cerebral hemorrhage Milder disease in older children can contribute to spread Diagnosis Hx PE Culture respiratory secretions Elevated white count with lymphocytosis Treatment Macrolides for 5 days: erythromycin, clarithromycin, azithromycin. (2nd line: TMP/SMX) Treat EARLY, treat often, treat contacts to reduce spread If no abx (ie pt refuses), then no contact with other humans for 21 days. No work, school, daycare, etc. Fluids (IV prn) O2 Sedatives Prevention Vaccination with DTaP (kiddos) and Tdap (adolescents and adults) Handwashing Prophylactic abx to close contacts to prevent spread Tuberculosis Infection with Mycobacterium tuberculosis Most commonly attacks the lungs (as pulmonary TB) but can also affect the CNS, the lymphatics, the circulatory system, the genitourinary system, bones, joints and skin. Background Among communicable diseases, 2nd leading cause of death worldwide. Prevalence: 2 billion Incidence: 8 million Mortality: 2 million people yearly 20-40% of world population is infected 15 million people infected in US Mycobacterium tuberculosis Non-motile pleomorphic rod Highly resistant to desiccation Very slow growing- generation time 12-18 hours (vs 20 min for E. coli) Pathophysiology Aerosol transmission: cough, sneeze, speak or sing One cough→ 3000 infective droplets 10 bacilli can initiate pulmonary infection In alveoli, taken up by alveolar macrophage, then on to the nodes, and to organs- 80% of disease is in lung, but can affect ANY organ Risk Minority: 2/3 of cases Indigent: 300x risk of national average HIV+ : 200-400% increase risk Other high risk groups: hospital employee, inner city resident, nursing home resident, alcoholic, incarcerated, illicit drug users, travel to endemic area LTBI vs Active Disease Two forms- distinct Latent TB Infection- pt is infected with M. tuberculosis, but is NOT sick, NOT infectious Active Disease- Pt is infected, sick, and contagious 2-8 weeks after inoculation, +PPD caused by cell-mediated immunity and hypersensitivity reaction 90-95% primary infections are unrecognized 10-30% of healthy pts will proceed directly to active disease (up to 50 % if MDR- TB) The rest will have latent infection. No symptoms, non-infectious. Can convert to active ANY time. Stages Primary or initial infection- often leaves nodular scars called Simon foci in one/both lungs. – Simon foci provide “seeds” for reactivation Latent or dormant infection Can convert to active later Can be treated to decrease risk/likelihood of conversion Active TB Either direct from initial infection, or reactivated latent infection Symptomatic Infectious Must be treated to decrease mortality and spread Increasingly RESISTANT to treatment – MDR-TB – XDR-TB Classic Symptoms of Active TB Productive cough Hemoptysis Fever Weakness Anorexia Weight loss Night sweats Malaise Physical Findings Fever Cachexia Hypoxia Tachycardia Lymphadenopathy Abnormal lung sounds- post-tussive rales Extrapulmonary Symptoms Skin Kidney Bone Brain More common with decreased immune function Lab Presence of acid-fast bacteria in sputum is a rapid presumptive positive Definitive dx from sputum cx or DNA/RNA amplification demonstrating M tuberculosis Culture takes weeks PPD/Mantoux Test 0.1ml intradermal purified protein derivative Area of INDURATION (NOT erythema) seen 48-72h after placement I said INDURATION, not erythema Measure transverse to long axis of arm Expressed in mm- and a lack of induration is written as 0 mm, not “neg” False Neg PPD 20% of active cases Cancer/recent chemo Anergy Drugs (steroids) AIDS Recent live attenuated virus vaccines (so place PPD same day or 6 weeks after vax) Concurrent infection Metabolic derangement (CRF) Lymphoid disease Stress (surgery, burn, graft-vs-host) Distant primary infection- role for 2step testing, “booster reaction” Population Based PPD Criteria >5 mm: HIV +, abnl CXR, recent TB contact >10 mm: IVDU, nursing home, jail, minority groups, age < 4, DM, CRF >15 mm: no risk factors Positives are reportable to state False positives may occur in persons with previous BCG vaccine This will be on boards! QuantiFERON®-TB Gold Test Whole blood test to detect both latent and active TB One visit/one sample testing Results in 24 hrs No reader bias Not affected by BCG vaccine Imaging Pos CXR trumps neg PPD, but neg CXR doesn’t r/o active TB Classic xray of active TB shows lesions in: – Post RUL – Apicoposterior LUL – Apical segments of LLL Differential Asthma Pneumonia Influenza CA HIV/AIDS ARDS Pneumothorax Pleural effusion MAC (mycobacterium avian complex) Treatment Therapeutic principles: 1. Must use multiple drugs to which M. tuberculosis is susceptible 2. Must be taken regularly 3. Must have sufficient duration to resolve the illness Treatment: Active TB Isolation Negative pressure rooms Mask- N95 Abx - First dose decreases bacillary load 10 fold 2 weeks decreases load 100-fold 4 wk tx plus 3 neg sputum smears means pt is no longer infectious Tx: Daily Regimen Initial 4 drug regimen – INH (isoniazid) 300 mg po q day Hepatitis, rash, GI upset, neuropathy Co-administer pyridoxine (vitamin B6) – RIF (rifampin) 600 mg po q day GI upset, rash, orange body fluids, hepatitis – PZA (pyrazinamide) 2 g po q day Hepatotoxicity, rash, GI upset – ETB (ethambutol) 2 g po q day Optic neuritis Daily Regimen Drop ETB if cx favorable Drop ETB and PZA after 2 mo if decreased symptoms and nl smear 6 month total Compliance ~ 60%. Denver Protocol DOT 91% compliance First 2 weeks: DAILY INH 300mg, RIF 600 mg, PZA 2g, streptomycin 1g Next 6 weeks, Same doses, 2 x/week Next 18 weeks: INH & RIF 2x/wk Relapse comparable to daily protocol (1.6%) Exceptions HIV+ tx to 9 months min Pregnant- tx 9 months, daily INH, RIF, ETB. OK to breastfeed Meningitis- add dexamethasone MDR TB- 7 (yup, seven) drug daily protocol, DOT essential. There are organisms resistant to SEVEN drugs. What then? XDR-TB Latent infection +PPD or QFT-G Neg CXR No signs/symptoms of active disease In healthy adult, 1% per year conversion to active HIV+ person has 10% per year conversion Latent Infection Tx INH 300 qd x 12 m has 75% risk reduction for converting to active disease INH 300 qd x 6 m (65% RR) INH 900 2x/wk for 12 m Seasonal Influenza Respiratory illness usually occurring in epidemic form in Oct- April, epidemics in US q 2-3 years Caused by strains of influenza virus (an orthomyxovirus) Annually in US: – Affects 5-20% of population – Results in 200k hospitalizations for complications – Causes 36,000 deaths Tell me you already know this... Influenza has 2 surface glycoproteins to allow virus to attach to and infect hosts HA- hemagglutinin-to fuse to host membrane NA- neuraminidase- enzyme to allow dispersion of new budding viruses Mutations of HA or NA drift Exchange of entire gene segments (usually between human flu and animal flu) shift Influenza: Acute S&S Chills, fever to 39.5C Sudden onset myalgias- worse in back and legs Prominent HA with photophobia and retrobulbar aching Sore throat, retrosternal burning +/- coryza Nonproductive cough Later on… Lower respiratory symptoms become dominant with persistent productive cough Acute symptoms and fever resolve in about 3 days Weakness, diaphoresis and fatigue can persist for weeks Secondary bacterial pneumonia suggested by recurrence of symptoms in 2nd week Transmission Droplet nuclei (not large particle aerosol like the common cold.) Rare fomite transmission. Cough or sneeze Incubation average 48 hours (range 1-4 days) Infectious for – – – – 1 d before sx onset to 5 d after (Adults) 1 d before to 10d after (Kiddos) Several days before sx +10d after (Wee kiddos) Immunocompromised folks can shed virus for weeks to months Complications Bacterial pneumonia Purulent bronchitis Otitis media Sinusitis Dehydration Worsening of chronic medical illnesses, ie: CHF, DM, asthma Rarer complications Encephalopathy Myocarditis Pericarditis Rhabdomyolysis Reye’s Syndrome- (fatty liver with encephalopathy) no ASA for children under 18 Diagnosis Good history, incl knowledge of current local trends. – As of October 3, 2009, 99% of circulating influenza viruses in the United States were 2009 H1N1 influenza PE: febrile, tachycardic, flushed face, pharyngeal, tonsillar and soft and hard palates injected without exudate. Conjunctival injection. Usually normal lung exam. No signs of consolidation. Clinical alone low sensitivity and specificity Check some labs? Better living thru nasopharyngeal swabs Rapid testing (30 min)-often performed in office. Vary in types of flu detected, ability to distinguish types, also in specimen type needed. Know your lab! Viral culture, esp to f/u negative rapid test when clinical suspicion is high. Results in 3 to 10 days Also available: immunofluorescence, EIA, PCR. Use of serology reserved for public health/research. Treat ‘em Conservative tx: rest, fluids, acetominophen for fever, headache, myalgia, cough suppressant prn. NB- NO ASA for children!! (Why?) Monitor for complications Antivirals: effective in sx duration, severity, also to contagion. Ideally initiate tx within 2 d of sx onset, duration of tx 5 days – Currently reserving antivirals for ill, high-risk folks with H1N1 Antivirals Oseltamavir (Tamiflu)- seasonal and H1N1 Zanamavir (Relenza)- seasonal and H1N1 Amantidine and rimantidine- Only effective against influenza A. Rapidly developing resistance to these drugs, so use of these agents is currently NOT advised. Awaiting reestablishment of susceptibility. PREVENTION Vaccinations Chemoprophylaxis with antivirals (7090% effective) Handwashing- soap and water or waterless alcohol based Education Fingers out of nose, eyes, mouth Good respiratory hygiene Avoid sick people if you’re well, and well people if you’re sick The Flu Shot Trivalent inactivated vaccine- –Killed viruses- 2 A strains, and a B – Representative of the influenza strains predicted to circulate New vaccine yearly. Usually one strain changes. Available thimerosal-free This year’s model A/Brisbane/59/2007(H1N1)-like virus A/Brisbane/10/2007 (H3N2)-like virus B/Brisbane/60/2008-like virus Too early to tell if we got it right! Also, attention and data is all about H1N1 Vaccine If well matched to circulating strains, vaccine can decrease risk of flu 70-90% in healthy adults and 66-90% in children Can be 30-70% effective in preventing hospitalization for pneumonia in elderly Decrease risk of death from influenza by 80% in elderly people in nursing homes Even poorly matched vax can provide crossprotection Other option: LAIV Live attentuated influenza vaccine Nasal spray LIVE virus, weakened Only for healthy, non-preg people ages 5-49 Who gets flu shot? People at risk for complications: kids 6 months to 19 years, pregnant women, age over 50, residents of LTC facilities or nursing homes, those with chronic medical conditions (see next slide), healthcare workers Folks who live with/care for the above Anyone who wants to risk of flu Chronic Medical Conditions Pulmonary ds (incl asthma and any other disease that can compromise respiratory function) Cardiovascular ds (except HTN) Renal ds Hepatic ds Hematologic ds Metabolic ds (including diabetes!) Immunosuppressed folks NO SHOT for you Severe egg allergy Hx of severe reaction to a flu vax Hx Guillain Barre Syndrome Age <6 months Currently moderately ill with fever – Fine to give to pt w/ low-grade fever Influenza vaccine factoids Production starts in January Usually available in October and after Works by provoking immune response and antibody development Effective in about 2 weeks. Immunity lasts months to a year Pandemics 1918- Spanish influenza. Killed 40-50 million people worldwide. 1957- Asian Influenza (2 million dead) 1968- Hong Kong Influenza (1 million) 2009- H1N1 Swine Flu ????- Avian Influenza. WHO conservative estimate of about 7.4 million deaths. Pandemic within 3 months of evolution of virus to easily transmissible state. Are we ready?