* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 5-Cardiomyopathy and Myocarditis
Management of acute coronary syndrome wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Echocardiography wikipedia , lookup
Cardiac surgery wikipedia , lookup
Heart failure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Myocardial infarction wikipedia , lookup
Electrocardiography wikipedia , lookup
Mitral insufficiency wikipedia , lookup
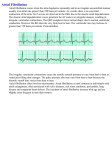
Heart arrhythmia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dr. Talaat Ali Sabeeh Al-Jarrah Pediatric Cardiologist Cardiomyopathy Classification (2 systems): Based on Suspected Etiology: 1-Primary. 2-Secondary Based on echocardiography: 1-Dilated – usually mostly Systolic dysfunction 2-Restrictive – usually mostly Diastolic dysfunction 3-Hypertrophic – usually mostly Diastolic dysfunction I-Dilated Cardiomyopathy Dilation of all four chambers (ventricles > atria); increased muscle mass; systolic failure Usually presents as unexplained heart failure (prior to echo) Signs & symptoms: Dyspnea on exertion, fatigue, PND, dependent edema, orthopnea, palpitations Manifestations of embolizaiton: neurologic deficits, flank pain, hematuria, pulseless cyanotic extremity Rales, S3 & S4 gallops, narrow pulse pressure, mitral or tricuspid regurgitation. Causes: 80% are usually classified as idiopathic Ischemic is the most common identified cause. Toxins: Alcohol, cocaine, amphetamines, lead, lithium Infectious: CMV, HIV, Varicella, Hepatitis Endocrine: Thyroid/Growth hormone excess or deficiency Peripartum Diagnosis ECG: LVH, Lt. or biatrial hypertrophy, poor R wave progression, new BBB, atrial fibrillation. Chest Xray: nonspecific; cardiomegaly & pulmonary vascular congestion (globular appearance) Echocardiograpy: ventricles & atria enlargement, increased systolic/diastolic volumes, EF <45%, abnormal ventricle contraction, valvular regurgitation: MR,AR. Treatment Treat CHF: diuretics, digitalis, vasodilators, ACE inhibitors Anticoagulants: all with mural thrombi; evidence of pulmonary or systemic emboli; atrial fibrillation II-Restrictive Cardiomyopathy Characterized by diastolic restriction of ventricular filling Low end diastolic volume Decreased cardiac output Causes 1-Infiltrative: Amyloidosis (most common), Sarcoidosis, Scleroderma 2-Storage diseases: Hemochromotosis 3-Endomyocardial diseases: radiation, hypereosinophlic syndrome, carcinoid Presentation:Similar to dilated cardiomyopathy, but more pronounced right sided heart failure & dyspnea on exertion. Physical Exam: Rales, peripheral edema, JVD, gallops, tachycardia, regurgitation murmurs, KUSSMAUL’s Sign? Diagnostic Studies: ECG: chamber enlargement (atria > ventricles); low voltage, atrial fibrillation. Chest X ray: normal to enlarged heart with pulmonary vascular congestion. Echocardiogram: Thickened walls, markedly dilated atria, normal systolic function, mitral/tricuspid regurgitation Catheterization Treatment Usually diuretics and digitalis Vasodilators can cause pronounced hypotension and may need to be avoided. III-Hypertrophic Cardiomyopathy Hypertrophy of the left ventricle, and occasionally of the right ventricle Interventricular septum is typically more prominently involved than the left ventricular free wall Left ventricular volume is normal or reduced; Diastolic dysfunction usually present 50% inherited - autosomal dominant Presentation Dyspnea on exertion, ischemic chest pain Palpitations, arrhythmias, syncope, pre-syncope Sudden Death Physical Exam S4 gallop Prominent systolic ejection murmur at left sternal border that increases with valsalva maneuver, sudden standing, or exercise. Diagnosis Chest Xray: usually normal Echocardiogram: LVH with disproportionate septal hypertrophy; small ventricular volume ECG: LVH & LAH, atrial fibrillation. NB. think hypertrophic cardiomyopathy in any young person whose ECG shows large septal Q waves Treatment Can become unstable in atrial fibrillation. 1-Long term care with Beta blockers 2-Amiodarone is treatment of choice for ventricular dysrhhythmias 3-Diuretics in the face of pulmonary congestion 4-Avoid agents that reduce ventricular volume (nitrates) or increase myocardial contractility (digoxin) 5-Antibiotic prophylaxis for dental procedures 6-Avoidance of competitive athletics 7-Anticoagulation if in atrial fibrillation Myocarditis Definition: inflammation of the heart muscle Causes 1- Infection: Viruses are the most frequent pathogens, but , bacteria, fungi, protozoa, and helminths have been implicated ,most frequently identified viruses were enteroviruses (including coxsackievirus) until the 1990s, but now parvovirus B19 and Human Herpes Virus 6 are more common. Parasites: Chagas’s, Toxoplasmosis, Trichinosis 2-Autoimmune disorders: such as SLE, Wegener's granulomatosis, giant cell arteritis, Kawasaki’s, and Takayasu arteritis 3-Drugs: Penicillin, sulfonamides 4-Toxins: Cocaine, toluene Presentation Think myocarditis in a young male with recent viral prodrome & now presents with unexplained CHF, new dysarrythmias/conduction defect, or symptoms of pericarditis with heart failure! Spectrum of presentation of myocarditis: Excessive fatigue Chest pain Unexplained sinus tachycardia Acute pericarditis S3, S4, or summation gallop Abnormal electrocardiogram Abnormal echocardiogram New cardiomegaly on chest x-ray Atrial or ventricular arrhythmia Partial or complete heart block New onset congestive heart failure Atypical myocardial infarction Cardiogenic shock Diagnosis Combination of clinical presentation and laboratory/imaging studies ESR: elevated. Cardiac Enzymes: rise over several days as opposed to hours in AMI. Endomyocardial Biopsy: definitive diagnosis. CBC: Mild leukocytosis Echocardiography: Dilated chambers with focal wall motion defects. ECG: Low Voltage, non specific ST/T wave changes, any dysrhhythmia, sinus tachycadia most common. Treatment Admit to ICU Administer Antibiotics if suspected bacterial infection Aspirin & IVIG if suspected Kawasaki’s Bed Rest CHF treated , but caution with digoxin Dysarrythmias managed per normal protocol. PERICARDITIS Follows a viral URI Sharp chest pain, retrosternal, difficulty in deep inspiration Patient resists lying down Pain worsened by pressure over the sternum Friction rub, pulsus paradoxus ECG is diagnostic: diffuse ST elevation. TREATMENT: Reassurance NSAIDS Occasional pericardial tap Post-pericardiotomy Syndrome: 2 weeks after surgery.