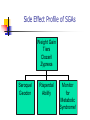
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Psychopharmacology Training
Survey
Document related concepts
Serotonin syndrome wikipedia , lookup
Pharmacognosy wikipedia , lookup
Lithium (medication) wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Atypical antipsychotic wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Prescription costs wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Drug discovery wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Neuropharmacology wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
Drug design wikipedia , lookup
List of off-label promotion pharmaceutical settlements wikipedia , lookup
Drug interaction wikipedia , lookup
Theralizumab wikipedia , lookup
Transcript
Mid-Ohio Psychological Services, Inc. Staff Training: Psychopharmacology Daniel DiSalvo, CNP February 8, 2008 Outline Welcome, Introduction & Lunch Content Pharmacodynamics/kinetics & Basic Principles Antidepressants MAOIs, TCAs SSRIs SNRIs Other Mood Stabilizers Antipsychotics Discussion Question & Answer Conclusion Psychopharmacology The study of the effects of drugs on affect, mood, cognition and behavior and the use of drugs to treat disorders of the central nervous system where it is the expressed intent to alter mood, thought or behavior. The Concept of Chemical Imbalance NT in deficit in excess acetylcholine dopamine memory impairment/delirium aggression/depression dementia/depression psychosis/anxiety/ confusion/aggression serotonin depression/impulsivity/anxiety anxiety norepinephrine depression/anxiety/dementia anxiety/aggression GABA anxiety/impulsivity cognitive/motor slowing glutamate cognitive slowing/dementia seizures/neuronal degeneration The Basis of Psychopharmacology Correcting the chemical imbalance – either increasing or decreasing activity of that NT. 1. 2. 3. 4. 1. 2. For disorders associated with hypofunctioning: Stimulate NT release Use chemical (drug) that mimics NT Block metabolic inactivation of NT Block reuptake For disorders associated with hyperfunctioning: Inhibit or reduce NT release Block target receptors Antidepressants >8 different pharmacological MOAs >2 dozen ADs Most block monoamine reuptake Some block alpha-2 receptors Others might work on the enzyme MAO Some have direct actions on only one monoamine NT system, while others work on multiple monoamine NT systems The immediate pharmacological actions of all ADs eventually have the effect of boosting the levels of monoamine NTs Why Does It Take So Long? Down Regulation: no matter what their initial actions on receptors and enzymes, ADs eventually cause a desensitization of key NT receptors in a time course consistent with the delayed onset of AD action of these drugs. Delayed actions of ADs may not only explain the delay in onset of therapeutic action of ADs; they may also explain why some patients fail to respond to ADs, as… It is possible that in such patients the initial pharmacological actions are not translated into the required delayed pharmacologic and genetic actions. Function Pharmacokinetics: How the body acts on the drug. Pharmacodynamics: How the drug acts on the body, especially the brain. Drug is absorbed and delivered through the gut wall to the liver to be biotransformed so that it can be excreted. CYP450: enzyme in the gut wall or liver converts the drug substrate into a biotransformed product in the bloodstream. After the passing through the gut wall and liver, the drug will exist partly as unchanged drug and partly as biotransformed drug. CYP450 Systems 1A2 2D6 2C9 2C19 3A4 Substrates of this enzyme: clomipramine imipramine 5-10% of Caucasians are poor metabolizers 20% of Japanese and Chinese persons Inhibitors: bupropion, fluphenazine, sertraline Some BDZs are substrates Biggie for ADs Several SSRIs are inhibitors (paroxetine, fluoxetine – most) fluvoxamine inhibits 3-5% of Caucasians Inducers: carbamazepine, ethanol, phenytoin, St. Johns’ wort Some ADs are inhibitors (nefazodone) Mood stabilizers Classical ADs: MAOIs & TCAs MAOIs – the very first! 1950s, 1960s Anti-TB drug Great for panic and social phobia Used to stop ‘em…dead! Subtypes: A (depression – 5-HT, NE), B (anti-neurodegenerative Parkinson’s) Hypertensive crisis MAOI Diet Cheese pizza, sour cream, yogurt, and all cheeses except cream and cottage Beef and chicken livers, unrefrigerated fermented sausage, summer sausage, bologna, salami, pepperoni, tofu, pickled fish/herring, lox caviar, dried salted herring/other smoked fish Broad bean pods, fava beans, Italian green beans, snow pea pods, sauerkraut, avocados Chocolate cake, cookies, ice cream, pudding, chocolate candy Chianti, sherry, red, burgundy, ale, beer, vermouth, Reisling, liqueurs Salad dressings with cheese or MSG Brewer’s yeast/yeast extract (e.g., some soups, sauces, gravies), MSG, meat tenderizers , soy sauce. MAOI Medication Interactions Sympathomimetics General anesthetics Local or spinal anesthetics w/ epi (e.g., Novocaine) OTC cough, cold and sinus w/ sympathos (e.g., Actifed, Sudafed, Contact, Dristan, Afrin, NyQuil, Dimetapp, Triaminic, etc.) Demerol and other narcotics containing codeine, morphine, hydrocodone (e.g., Percocet, Percodan) Cocaine Macrolantin Other ADs Drug Form MAOIs-A Generic Daily Dose Max Price (qd dose) Marplan 10mg tab No 30mg 60mg $2.45 Nardil 15mg tab No 60mg 90mg $2.64 Parnate 10mg tab No 40mg 60mg $3.94 MAOIs-B & RIMAs Selegiline – parkinsonism… Emsam (selegiline): greater affinity for B, but works on both at AD doses 6/9/12mg transdermal/qd – no restrictions at 6 RIMAs not available in US Manerix – few dietary restrictions Pharmacological Actions MAOIs Readily absorbed through GI Peak plasma in 2hr. T ½ is 2-3hr. Irreversibly inactivate MAOs – i dose can last for 2w. Therapeutic Indications – MAOIs Depression, esp. that associated with mood reactivity, extreme sensitivity to interpersonal loss or rejection, prominent anergia, hyperphagia, hypersomnia (atypical features) Also great for panic, PTSD, AN, BN, SP and pain syndromes. Refractory Panic (high) OCD (none) GAD (moderate) BDD (moderate) Precautions & Adverse Reactions – MAOIs Orthostasis, insomnia, weight gain, edema, sexual dysfunction (divide dose, increase fluids/salt, support stockings, take in a.m., add sleep agent, or…switch) HTN crisis w/o tyramine (Parnate) – avoid Taper and wait for >2w w/ a switch Paresthesias, myoclonus, muscle pains Pyridoxine 50-150mg/d Less cardiotoxic, epileptogenic compared to TCAs Caution, though, w/ renal, CV and hyperthyroidism May alter dosage of a hypoglycemic agent Associated w/ induction of mania in pts. in depressed phase of BPAD I and triggering psychotic decompensation in scz Contraindicated in pregnancy/nursing Precautions & Adverse Reactions – MAOIs OD: agitation coma w/ hyperthermia, HTN, tachypnea, tachycardia, dilated pupils and hyperreflexia, involuntary movements (face, jaw) Asymptomatic 1-6hrs. acidify urine, dialyze Multi-drug (esp. 5-HT) – increase effects Precautions & Adverse Reactions – MAOIs Labs: DM meds (hypoglycemia) minimal, false elevation of TFTs Periodic LFTs TCAs Wide range: MDD, Panic, GAD, PTSD, OCD, EDs, Pain Syndrome Yet, very toxic and we have alternatives Significant FPE Peak plasma 2-8hrs T ½ 10-70hrs 2D6: (Is) quinidine, cimetidine, fluoxetine, sertraline, paroxetine, phenothiazines, carbamazepine, some antiarrhymics (propafenone, flecainide) Block reuptake of NE, 5-HT Competitive antagonists of muscarinic acetylcholine, H1, alpha-1, -2 Use if cannot tolerate anxiety/GI upset (SSRIs) TCAs – Approved / Off-Label Uses MDD: induce mania in susceptible pts. (compared to bupropion, SSRIs) Panic: imipramine, yet anxiogenic, so start low, go slow GAD: doxepin, imipramine OCD: clomipramine (2-4w…4-5m) and depressed pts. w/ marked obsessive features EDs: imipramine, desipramine, clomipramine Pain: any Enuresis: imipramine Peptic ulcer: doxepin Others: narcolepsy, nightmare d/o, PTSD, sometimes for ADHD, sleepwalking, separation anxiety, sleep terrors, premature ejaculation, movement d/os Precautions & Adverse Reactions – TCAs Anticholinergic, sedation, orthostasis, seizure, conduction abnormalities, weight gain Can induce mania (over SSRIs, bupropion) May exacerbate psychotic d/os Confusion, delirium Tachycardia, flattened T waves, prolonged QTc intervals, depressed ST segments Don’t use w/ cardiac pts., unless other agents have failed (monitor) Sore throat in initial stages – monitor Transient increase in LFTs vs. hepatitis Drug Interactions – TCAs MAOIs Antihypertensives Esimil, Ismelin (block reuptake) propranolol, clonidine (also block) Aldomet + TCA = agitation DA blockers perphenazine = doubling of plasma [ ] of both products (add to anticholinergic SE profile, too) Sympathomimetics Serious CV effects CNS depressants Opioids, EtOH, anxiolytics, hypnotics, OTC cold remedies Oral contraceptives BCPs may decrease TCA plasma [ ] through the induction of hepatic enzymes Diamox, ASA, cimetidine, thiazide diuretics, fluoxetine, sodium bicarbonate = increase, while ascorbic acid, ammonium chloride, barbiturates, cigarette smoking, carbamazepine, chloral hydrate, lithium decrease levels TCA Labs Can get levels, though Should be clinically driven TCA Dosages / Clinical Guidelines DRUG TABLET (mg) CAPSULES PARENTERAL (mg/mL) imipramine 10, 25, 50 75, 100, 125, 150 12.5 desipramine 10, 25, 50, 75, 100, 150 25, 50 trimipramine amitriptyline 25, 50, 100 10, 25, 50, 75, 100, 150 nortriptyline protriptyline 5, 10 amoxapine 25, 50, 100, 150 doxepin maprotiline clomipramine SOLUTION (mg/mL) 10 10, 25, 50, 75 10/5 10, 25, 50, 75, 100, 150 10 25, 50, 75 25, 50, 75 Clinical Guidelines of TCAs Prior to tx: PE, CBC w/ diff, lytes, LFTs, EKG (esp. women >40, men >30) Contraindicated in pts. w/ a QTc >450msc Consider using newer agents 1st, esp. if pt. has an interfering medical dx In kids, elderly – avoid, but if need to use, EKG should be monitored frequently Those w/ chronic pain might be sensitive to initial dosing, but may benefit later Taper to avoid cholinergic rebound syndrome Dosing & Levels – TCAs Drug Usual Adult Dosage Range (mg/d) Therapeutic Plasma [ ] (mcg/mL) Tofranil 150-300 150-300 Norpramin 150-300 150-300 Surmontil 150-300 ? Elavil 150-300 100-250 Pamelor 50-150 50-150 Vivactil 15-60 75-250 Asendin 150-400 ? Sinequan 150-300 100-250 Ludiomil 150-230 150-300 Anafranil 130-250 ? TCAs & OD Serious, can easily be fatal NRF, <1w quantity for those at risk amoxapine – most fatal OD Sx: agitation, delirium, convulsions, hyperreflexia, bowel/bladder paralysis, dysregulation of BP, T and mydriasis…coma, respiratory depression cardiac arrhythmias may not be correctable, and are at risk for up to 4d s/p OD d/t long T ½ SSRIS (the ones we know and love) fluoxetine – 1987 Rapidly eclipsed the MAOIs/TCAs Don’t necessarily work better, but are safer and have a less (different) SE profile Subtle differences between compounds: T 1/2 , potency for reuptake inhibition and affinity for some other receptors Overall, less effects on adrenergic, histaminergic and cholinergic Pharmacologic Actions – SSRIs Selectively block the reuptake of 5-HT presynaptically Slightly different pharmacokinetic profiles, as each drug is structurally different from the others Many are highly protein bound Varying T ½ - 24hr to several days fluoxetine (active metabolite) = 7-15d citalopram = 1.5d sertraline / paroxetine = 1d All are well absorbed and not generally affected by food administration except for sertraline (level may be increased w/ food) No correlation between T ½ and time to onset All eliminated in urine as active metabolites citalopram / escitalopram – more selective for 5-HT receptor blockade Indications For / Off-Label Use of SSRIs MDD – acute, single, recurrent, prevention, etc. DD, PD OCD (may need more, take longer) GAD, SP, PTSD AN, BN (APA recommends use for persistent depression after pt.’s gained wt.) BDD PMDD Children Repetitive-type abnormalities, e.g., autism, ADHD (as adjunct), MR/DD, chronic enuresis Other complex behavioral d/os Obesity (high dose fluoxetine) Binge eating (sertraline) Substance abuse Decrease aggressive behaviors – impulsivity / uncontrolled anger in all ages Migraine / cluster HAs Diabetic neuropathy, facial pain, fibrositis, arthritis, RLS Pharmacokinetic Profiles – SSRIs Drug Time to T½ Peak Plasma [] T½ metabolite Time to PlasmaSteady State Protein (days) Binding (%) fluoxetine 6-8h 4-6d 4-16d 28-35 95 fluvoxamine 3-8h 15h -- 5-7 80 paroxetine 5-6h 21h -- 5-10 95 sertraline 4.5-8.5h 26h 62-104h 5-7 95 escitalopram 3-5h 30h 50-60h 10 90 citalopram 4h 35h 3h 7 80 Basics – SSRIs Drug Generic/Supply Dose/Day Price Index ($ cost of dose/d) Prozac Y/Soln, Tabs, Delayed Cap 60mg 1.10 Zoloft Y/Soln, Tabs 100mg 3.02 (brand) Paxil Y/Soln, Tabs 40mg 2.97 Luvox Y/Tabs 200mg 5.25 Lexapro N/Soln, Tabs 20 2.65 Celexa Y/Soln, Tabs 40 2.65 Precautions & Adverse Reactions – SSRIs ¾ of pts. experience no SEs ¼ have SEs in first 2w, usually subside 10-15% are unable to tolerate Sexual dysfunction: 50-80%, might not go away… GI: sertraline, fluvoxamine, citalopram Decrease dose; switch (bupropion, nefazodone); add (bupropion) N, V, D, anorexia, dyspepsia – transient? Weight gain: initially lose, but 1/3 will gain (>20lbs.); paroxetine (d/t anticholinergic SE) HAs: 18-20% (fluoxetine – most); alternately, SSRIs are wonderful for tension HAs/migraines Precautions & Adverse Reactions – SSRIs CNS Anxiety: fluoxetine (most), but then tx it Insomnia/sedation: ¼ have insomnia (fluoxetine – take in a.m.); sertraline = fluvoxamine; citalopram/paroxetine – sedation Tx w/ trazodone, BDZ, other off-labels Nightmares: small amount of pts. (resolves) Seizures: 0.1 - 0.2% of all pts. txd w/ SSRIs (comparable to other ADs/placebo) EPS: Tremor 5-10% TD (exceptionally rare) Pts. w/ well-controlled Parkinson’s – acute worsening of their motor symptoms Bruxism (buspirone) Most common w/ fluoxetine Precautions & Adverse Reactions – SSRIs Anticholinergic: paroxetine (mild) Can decrease plt. function = bruisability paroxetine, fluoxetine (reversible neutropenia – rare, usually if concurrent w/ clozapine) Electrolyte / Glucose: Dry mouth (up to 20%) Dose-dependent Hematologic: opposite of S.L.U.D. Hypoglycemia (rare – DM pts. need to be careful) Hyponatremia/ADH release (also rare) – if diuresing/H2O deprived Endocrine / Allergic: Decrease prolactin/galactorrhea (breast changes may take several months to correct) Various rash types – 4% (d/c) Precautions & Adverse Reactions – SSRIs 5-HT Syndrome: SSRI + MAOI or SSRI + L-tryptophan or SSRI + lithium = can raise 5-HT concentrations to toxic levels, causing cascade of: D Restlessness Extreme agitation Hyperreflexia Autonomic instability Myoclonus Seizures Hyperthermia Uncontrollable shivering, rigidity Delirium Coma Status epilepticus CV collapse Death Precautions & Adverse Reactions – SSRIs 5-HT Syndrome Tx: D/C offender Supportive care Nitro Cyproheptadine Methysergide Cooling blankets Chlorpromazine Dantrolene Benzodiazpines Anticonvulsants Mechanical vents Paralyzing agents Precautions & Adverse Reactions – SSRIs SSRI W/D: Abrupt discontinuation, esp. w/ a shorter T ½ (paroxetine, fluvoxamine) After 6w; ends by 3w dizziness, weakness, N, HA, rebound depression, anxiety, insomnia, poor concentration, UR Sx, paresthesias, migrainelike Sx Tx: don’t abruptly stop; use fluoxetine SSRIs & Labs None SNRIs “3rd Generation” ADs 5-HT, NE – equal affinity duloxetine, venlafaxine, mirtazapine Differences among the three: mirtazapine – antagonist of central presynaptic alpha2adrenergic receptors; potent antagonist of H1 venlafaxine – a little faster onset w/ rapid dose increase; great for severe MDD w/ melancholy; 1st non-bdz drug (other than buspirone) to be approved for GAD duloxetine – compared w/ venlafaxine, it has a greater effect on 5-HT reuptake in vitro; approved for diabetic neuropathic pain Other ADs bupropion (DA, NE) – late 80’s trazodone structurally related to nefazodone, structurally unrelated to SSRIs, TCAs, MAOIs active metabolite is mCPP (5-HT2c agonist), is especially sedating (off-label use), blocking H1 priapism (1:6000; surgical intervention in 33%) nefazodone augmentation, SEs, off-label, etc. be careful w/ OD and EDs – sz d/o mixed 5-HT antagonist/reuptake inhibitor great for anxiety less sedation, hypotension than TCAs, trazodone atomoxetine (NOT approved for depression) – NRI; could use off-label Special Considerations in the Selection of an AD Gender: women have less gastric acid / slower emptying = slower GI absorption volume distribution = more adiposity than lean muscle H2O retention associated w/ menses = affects volume distribution, too PO contraceptives can alter hepatic metabolism (TCAs) Special Considerations in the Selection of an AD Ethnicity: AAs slow metabolizers compared to Europeans d/t metabolic enzyme expression AAs have higher plasma levels per dose of AD (demonstrated most w/ TCAs) Asians are slower to metabolize nortriptyline than other groups Minorities were less likely than nonminorities to be offered AD treatment, independent of dx (study of CMHCs’ prescribing practices in Westchester County, NY) Special Considerations in the Selection of an AD Age: Remember: start low, go slow Comorbidities: Elderly? Steady-state [ ] are minimally affected by age (except paroxetine) Renal – dose adjustment (except fluoxetine, sertraline) Liver – can increase levels of TCAs (monitor); give lower doses of SSRIs; don’t use nefazodone Pregnant Women and Nursing Mothers: Risks vs. benefits Generally safe, but be careful of w/d for neonate Mood Stabilizers Agents that are geared at affecting one phase of illness w/o worsening any other phase(s) 3 families: lithium anticonvulsants atypicals Lithium 1970 Used the longest, quite frequently and is excellent for mania, maintenance – all phases Yet non-response rate can be as high as 40% Narrow TI Structurally simple = Li+ MOA: unclear if NTs are involved, like they are in depression tx; occurs intracellularly w/ secondmessenger systems A monocovalent cation – a direct competitior of Mg+ @ regulatory enzyme, IMPase = reduces intracellular Ca+/protein kinase C activation Lithium lithium carbonate, Lithobid, Eskalith CR = immediate and extended (better tolerated, convenience) Peak plasma 1-4h T ½ 18-36h Rapid, complete absorption Low protein binding No first-pass effect 95% drug excretion by kidneys Can remit mania in many cases, but clinically an antiepileptic or atypical is also used Lithium – Labs / PreTreatment Testing CBC Lytes KFTs TFTs EKG Pregnancy Check level q3-6mos, as well as associated labs/EKG Normal range: 0.5-1.5mEq/L Lithium 150mg, 300mg, 600mg cap $15.54, $17.77, $42.30 (#100) Eskalith CR 450mg cap $81.97 (#180) Adverse Effects – Lithium Narrow TI Prolonged exposure to >2.0mEq/L: CNS impairment, renal collapse, coma, permanent brain injury, death Tox s/s: tremor, confusion, ataxia, N, V, D, tinnitus, blurred vision, HA, dizziness. Common SEs: N, V, D, tremor, polydipsia, polyuria, weight gain, hypothyroidism (reversible), fatigue Drug Interactions – Lithium Increase levels ACE Is Alprazolam Antipsychotics Fluoxetine Ibuprofen Indomethacin Naprosyn NSAIDs Some antibiotics Aldactone Thiazide diuretics Decrease levels Caffeine Carbonic anhydrase Is Dilor Laxatives Osmotic diuretics Atenolol Theophylline Lithium & Pregnancy No!…? 1st trimester = Ebstein’s anomaly (1:2000) However, discuss the risk and benefit Be very clear in initial interview about risks, as a female pt. might be well into her 1st trimester… Retrospective studies have shown to use aggressive pharmacotherapy in the immediate PPP (90% of bipolar I females are at risk for relapse in first 2mos of PP) Depakote / Depakene Acts at Na channels, at steps in GABA metabolism, and on the activity of histone deacetylase -Kote “coats” Available in IR, ER Rapid absorption, reaching peak plasma in 2-4h Bioavailability unaffected by food, though absorption may be delayed Rapid distribution and high (90%) plasma protein binding T ½ 9-16h Depakote / Depakene Uses / Indications Bipolar I d/o Acute, maintenance, prophylaxis SCZ (off-label) IED, kleptomania, other behavioral dyscontrol syndromes Physical aggression, restlessness, agitation Also off-label for anxiety d/os such as panic, PTSD, OCD, BN MDD EtOH, sedative/hypnotic w/d; cocaine detox Borderline PD Depakote / Depakene – PreTreatment / Labs CBC w/ diff., LFTs, check levels and associated labs q3-6mos Level: 50-100mcg/mL, but be clinicallydriven Check for bleeding and bruisability Depakote / Depakene Preparations Depakene: 250mg caps, #100, $207.01 Depakote: 125mg tab, #180, $110.29; also available in 250mg and 500mg tabs, and in ER (which does not affect timing of lab, but affects timing of dose) Depakote / Depakene Common SEs: Alopecia GI upset Sedation Tremor Weight gain Rare SEs: Acute pancreatitis Anemia Ataxia Bone marrow suppression Breast enlargement Dermatitis Diplopia, dizziness Edema Hepatotoxicity Irregular menses Leukopenia Nystagmus Parotid gland swelling Stevens-Johnson syndrome Thrombocytopenia Depakote / Depakene Drug Interactions 2D6 metabolism Can increase phenobarb, phenytoin, TCAs, Retrovir, diazepam Can decrease lamotrigine, carbamazepine DVP levels can be increased by ASA, highly protein-bound drugs DVP levels can be decreased by carbamazepine, Rifampin, mefloquine Depakote / Depakene & Pregnancy / Nursing Do not give to pregnant or nursing pts. Associated w/ neural tube defects (e.g., spina bifida) in 1-2% of all women during 1st trimester This risk can be reduced if FA (1-4mg/d) is taken 90d prior to and throughout gestation Antipsychotics Rapidly expanding! Atypicals over conventionals, w/ birth of clozapine Newer agents have less EPS, TD, cognitive impairment, and improvement in negative Sx Nonconventionals are used for other d/os, not just psychosis Atypicals: Clozaril, Zyprexa, Seroquel, Risperdal, Geodon, Abilify Pharmacology – Atypicals All have affinity for DA, but vary in potency 5-HT2a > D2 (different SE profile compared to conventionals) Attracted to alpha1/2-adrenergic, muscarinic acetylcholine, H1 as well Antagonize DA, 5-HT2a Rapidly absorbed from GI tract w/ extensive FPM Highly lipophilic – cross BBB Primarily metabolized by 2D6, 1A2, 3A4 & 2C19 Average T ½ is 20-24h, except for aripiprazole: 95h Parenteral form: olanzapine, aripiprazole, ziprasidone as IR and risperidone as decanoate Indications for Use – Antipsychotics SCZ, Schizoaffective d/o Acute manic/mixed episodes – bipolar MDD w/ psychosis Delusional d/o Delirium Dementia MR Developmental d/o (e.g., autism) Huntington’s Tourette’s Substance-induced psychotic d/o (stimulants, PCP, levodopa, steroids) Preparations / Dosage – Antipsychotic Risperdal (mg tabs 0.25, 0.5, 1, 2, 3, 4; soln; M-tabs; RisConsta): 2-8mg/d Geodon (mg caps 20, 40, 60, 80; soln): 80-200mg/d Clozaril (mg tabs 25, 100): 25-600mg/d Zyprexa (mg tabs 2.5, 5, 7.5, 10, 15, 20; Zydis; soln): 530mg/d Seroquel (mg tabs 25, 50, 100, 200, 300, 400): 150800mg/d Abilify (mg tabs 5, 10, 15, 20, 30; soln): 10-30mg/d Drug Selection & Initiation of Treatment – Antipsychotics Tests: height, weight, waist circum., BMI; interview about personal and family h/o diabetes or lipid dysregulation Obtain FBS, lipid panel Is this psychotic episode consistent w/ SCZ? Have affective syndromes such as mania and depression with psychotic features been ruled out? Is this the patient’s first episode? Previous AP exposure – efficacy and tolerability profiles? H/O EPS or TD? H/O NMS? What Sx are current predominant: + or -? H/O noncompliance/depot exposure? If AP trials have failed, were the doses/duration of tx adequate? Etc. Side Effect Profile of SGAs aripiprazole clozapine risperidone olanzapine quetiapine ziprasidone EPS + 0 ++ + 0 + TD + 0 ++ + 0 + NMS ? + + + ? + Prolactin 0-+ 0 +++ 0-+ 0 0-+ QTc 0 0 + 0 + ++ Hypotension + +++ + ++ ++ + Anticholinergic 0 +++ 0 ++ + 0 Hepatic + +++ + ++ + + Agranulocytosis 0 ++ 0 0 0 0 Sedation + +++ + ++ +++ + Seizure 0-+ +++ 0 0-+ 0-+ 0-+ Side Effect Profile of SGAs Weight Gain Tiers Clozaril Zyprexa Seroquel Geodon Risperdal Abilify Monitor for Metabolic Syndrome! Case Study 32yo MWF who’s escorted to the clinic by her BF. Pt.’s been c/o, and partner corroborates, that she’s been feeling quite sad lately, cannot get out of bed, has been w/ regular crying spells, is sleepless, has felt hopeless and believes she’d be better off dead. She adds that she has no health insurance and is 13w pregnant. You observe that she is nearly morbidly obese. She is not sure, but she’s been so sad that she thinks she’s been hearing her name being called and hears occasional, indecipherable whispers. She’s w/ severe GI discomfort, associated w/ her pregnancy, as well as sedation, probably within the context of both pregnancy and mood. The BF’s asking for a medication to help the pt., and the pt. is very willing to try a product. What thoughts come to mind as far as a product for this pt.? Discussion Divide into small groups to process this case. Questions, Comments, Concerns? Thank you for your time, interest and participation. Daniel DiSalvo 614-519-4880