* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The skeletal system - Mrs. Pronger`s Science Class
Survey
Document related concepts
Transcript
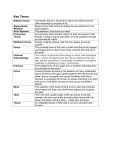
THE SKELETAL SYSTEM
Chapter 5
I. Bones: An Overview
A. Functions of the Bones
1.
2.
3.
4.
5.
Support – holds the body up, anchors soft organs
Protection – protects soft organs
Movement – helps body move, like levers
Storage – fat, calcium salts, phosphorus; works like a bank
Blood cell formation (hematopoiesis) – helps to form all blood cells
B. Classification of Bones
1.
Two types of bone
a.
Compact bone – dense and smooth or homogenous
b.
Spongy bone – small, needle-like pieces of bone and lots of open space
I. Bones: An Overview
2.
Four groups of bones
a.
Long bones – longer than wide, shaft with head on both ends, mostly compact
bone, all limb bones except wrist and ankles
b.
Short bones – cube-shaped, mostly spongy bone, wrist and ankles
i.
Sesamoid – special short bone in tendons, patella
c.
Flat bones – thin, flat, usually curved; 2 thin layers of compact sandwiching
spongy; skull, ribs, sternum
d.
Irregular bones – does not fit in other categories; spine, hips
I. Bones: An Overview
C. Structure of a long bone
1.
Gross anatomy
a.
Diaphysis – shaft, most of long bone’s length, compact bone
b.
Periosteum – connective tissue covering diaphysis
c.
Epiphyses – ends of long bones, thin layer of compact over spongy
i.
d.
i.
Articular cartilage – made of hyaline cartilage to decrease friction
Epiphyseal plate – line of hyaline cartilage that causes lengthwise growth of
long bones; found in young, growing bones
Epiphyseal line –cartilage turned to bone and left after growth is finished
e.
Yellow marrow (medullary) cavity – in shaft of bones in adults, is for fat
storage
f.
Red marrow – in shaft of bones in young children to form blood cells; confined
to cavity of spongy bone and epiphyses of long bones in adults
I. Bones: An Overview
2.
Microscopic anatomy
a.
Osteon or Haversian system – consists of central (Haversian) canals and matrix
rings (lamellae) that run lengthwise through the bone
b.
Lamellae – concentric circles of lacunae
c.
Lacunae – tiny cavities in the matrix filled with osteocytes
d.
Osteocyte – mature bone cell
e.
Canaliculi – tiny canals radiating out from central canals to all lacunae
f.
Perforating (Volkmann’s) canals – communication pathway from outside of
bone to interior; run into compact bone at right angles to shaft
g.
Calcium salts give bone hardness
h.
Organic matrix (collagen fibers) give bones flexibility and tensile strength
I. Bones: An Overview
D. Bone Formation, Growth, and Remodeling
1.
Formation
a.
Embryos are mostly hyaline cartilage, usually completely replaced by bone as a
young child
b.
Bones develop using hyaline cartilage as their “model” in a process called
ossification, which occurs in 2 phases
i.
Hyaline cartilage is completely covered by osteoblasts (bone forming cells)
ii.
Hyaline cartilage model is digested away opening medullary cavity
I. Bones: An Overview
2.
Growth
a.
Articular cartilage persists through life
b.
Hyaline cartilage grows on outside away from medullary cavity, it is replaced
on the inside by bony matrix (osteoblasts) for lengthwise growth
c.
Appositional growth is widening of the bones by removing bone from the inner
face (endosteum) of the diaphysis and adding it to the external face as
osteoblasts
d.
Longitudinal and appositional growth happen at the same rate
e.
End of growth phase is marked by epiphyseal plates turning to bone
I. Bones: An Overview
3.
Remodeling
a.
Calcium levels in the blood
i.
If drops below homeostatic levels then the parathyroid hormone (PTH) is released,
PTH activates osteoclasts to destroy bone cells releasing calcium into blood
ii.
When too high (hypercalcemia), calcium is deposited as hard calcium salts
b.
Pull of gravity and muscles on skeleton
i.
Bones become thicker and form large projections to increase strength in areas where
bulky muscles attach, osteoblasts lay down new matrix and become trapped inside,
thus becoming maturing bone cells (osteocytes)
ii.
Bones and muscles of bedridden or physically inactive people become atrophied
because they are not subjected to stress
I. Bones: An Overview
E. Bone Fractures
1.
2.
3.
4.
Most fractures in youth result from trauma; those in old age from
thinning, weakened bones
Closed (simple) fractures – bone is broken cleanly and does not
penetrate the skin
Open (compound) fractures – broken bone end penetrates the skin
Common types of fractures
a.
Comminuted – bone breaks into many fragments
b.
Compression – bone is crushed
c.
Depressed – broken bone portion is pressed inward
d.
Impacted – broken bone ends are forced into each other
e.
Spiral – ragged break occurs when excessive twisting forces are applied
f.
Greenstick – bone breaks incompletely, much in the way a green twig breaks
I. Bones: An Overview
5.
Fracture treatment
a.
Reduction – realignment of the broken bones
i.
Closed reduction – bone ends are coaxed back into normal positions without surgery
ii.
Open reduction – surgery is performed and the bone ends are secured together with
pins or wires
b.
Immobilized to heal for 6-8 weeks for a simple fracture and longer for large
bones and those of elderly
6. Repair of bone fractures
a.
Hematoma (blood-filled swelling) forms from ruptured blood vessels and those
deprived of nutrition die
b.
Fibrocartilage callus splints break, growth of capillaries (granulation tissue),
disposal of dead tissue
c.
Fibrocartilage is gradually replaced with spongy bone called bony callus
d.
Bony callus is remodeled to form a strong permanent patch at fracture site
II. Axial Skeleton
A. Skull
1.
2.
All bones of the skull except the mandible are held together by sutures,
or interlocking, immovable joints
Cranium
a.
Encloses and protects fragile brain tissue
b.
8 flat bones, all single bones except parietal and temporal (paired bones)
c.
Frontal bone – forehead, bony projections under eyebrows, superior part of
eye’s orbit
d.
Parietal bones – superior and lateral walls of cranium, meet at midline of skull
to form sagittal suture and coronal suture where they meet frontal bone
II. Axial Skeleton
e. Temporal bones – inferior to the parietal bones and join them at squamous
sutures, have several important bone markings
i.
ii.
iii.
iv.
v.
f.
External auditory meatus – canal leading to eardrum and middle ear
Styloid process – sharp, needlelike projections inferior to the external auditory meatus;
serves as an attachment point for many neck muscles
Zygomatic process – thin bridge of bone joining cheekbone (zygomatic bone)
anteriorly
Mastoid process – rough projection posterior and inferior to external auditory meatus, full of air
cavities (mastoid sinuses), and provides an attachment point for some muscles of the neck
Jugular foramen – junction of occipital and temporal bones, allowing passage of large jugular vein
to drain the brain; anterior to carotid canal which internal carotid artery runs through supplying
blood to the brain
Occipital bone – most posterior bone in cranium forming floor and back wall of skeleton,
joins parietal bones at lambdoid suture
i.
ii.
Foramen magnum – large opening in the base of the occipital bone, allowing brain to connect with
the brain
Occipital condyles – rocker-like, lateral to foramen magnum, rest on first vertebra of spinal column
II. Axial Skeleton
g. Sphenoid bone – butterfly-shaped bone forming floor of cranial cavity, can be
seen from the eye orbits, central part is riddled with air cavities (sphenoid
sinuses)
i.
Sella turcica (Turk’s saddle) – depression in midline of sphenoid bone, forms a place for
pituitary gland
ii.
Foramen ovale – large oval opening in line with posterior end of sella turcica which
allows nerves to pass to the chewing muscles of mandible
II. Axial Skeleton
h.
Ethmoid bone – irregularly shaped,
anterior to sphenoid, forms roof of
nasal cavity and part of the medial
walls of the orbits
i.
Crista galli project from superior
surface (cock’s comb), outermost
covering of the brain attaches to
this projection
ii.
Cribriform plates – holey areas on
each side of the crista galli, allow
nerve fibers to pass from olfactory
receptors (in the nose) to reach in
the brain
II. Axial Skeleton
3.
Facial Bones
a.
Fourteen bones, all paired bones except mandible and vomer (single bones)
b.
Maxillae – fuse to form upper jaw, all bones but mandible join maxillae making
it “keystone”
i.
Contain sinuses that drain into nasal passages, infections in nasal/throat areas can
migrate to sinuses causing sinusitis
ii.
Upper teeth in alveolar margins
iii.
Palatine processes form anterior part of hard palate of mouth
c.
Palatine bones – posterior to palatine processes, posterior part of hard palate,
failure to fuse medially causes cleft palate
d.
Zygomatic bones – cheekbones, good-sized portion of lateral walls of orbits
e.
Lacrimal bones – fingernail-size bones forming part of the medial walls of each
orbit, has a groove that serves as passageway for tears
f.
Nasal bones – small rectangular bone forming the bridge of the nose
II. Axial Skeleton
II. Axial Skeleton
g. Vomer bone – single bone in median line of nasal cavity (vomer means plow,
references shape of bone), forms most of nasal septum
h. Inferior conchae – thin, curved bones projecting from lateral walls of nasal
cavity
i.
4.
a.
5.
Mandible – lower jaw, strongest bone in the face, joins to temporal bones
forming only free moving join in the skull
Hyoid Bone – not really part of skull, but closely related to mandible and
temporal bones
Only bone that does not articulate directly with any other bone, suspended in
midneck region by ligaments to the styloid processes
Fetal skull
a.
Face very small compared to cranium, but large compared to whole body
b.
Some areas still hyaline cartilage, and some not bony called fontanels which
allow for brains to grow late in fetal development and skull to be compressed
slightly during birth
c.
Gradually converted, usually complete at 22-24 months of age
II. Axial Skeleton
B. Vertebral Column (spine)
1.
2.
3.
4.
5.
Axial support of the body from skull to pelvis
26 irregular bones connected and reinforced with ligaments to make a
flexible curved structure
Surrounds and protects spinal cord
7 cervical, 12 thoracic, 5 lumbar, sacrum (5 fused), coccyx (4 fused)
Vertebrae separated by pads of flexible fibrocartilage called
intervertebral discs, to cushion and absorb shock
a.
Discs in young person about 90% water, but decreases as a person ages
becoming less compressible
b.
Drying of the discs and weakening of ligaments predisposes people to
herniated discs leading to pressure on spinal cord or nerves
II. Axial Skeleton
6. Common features of vertebrae
a.
Body or centrum – disc-like, weight-bearing part of vertebra, faces anteriorly in
column
b.
Vertebral arch – arch formed from joining of all posterior extensions from the
vertebral body
c.
Vertebral foramen – canal through which the spinal cord passes
d.
Transverse processes – two lateral projections from the vertebral arch
e.
Spinous processes – single projection arising from the posterior aspect of the
vertebral arch
f.
Superior and inferior articular processes – paired projections lateral to the
vertebral foramen, allowing a vertebra to form joints with adjacent vertebrae
II. Axial Skeleton
7.
Cervical vertebrae - C1 – C7, in neck region
a.
C1 – atlas vertebra, no body, superior surface of transverse process has large
depressions for occipital condyles, allows for flexion and extension
b.
C2 – axis vertebra, large upright process (odontoid process or dens) acts as
left/right pivot point of head
c.
C3 – C7 – are typical, smallest, lightest vertebrae, spinous processes short and
divided into two branches, contain openings (foramina) that allow vertebral
arteries to pass through on way to brain
8. Thoracic vertebrae - T1 – T12
a.
All typical, larger than cervical, two articulating surfaces on each side for heads
of ribs, spinous processes are long and hook downward sharply
9. Lumbar vertebrae - L1 – L5
a.
Massive block-like bodies since they receive most of the stress, short, hatchetshaped spinous processes
II. Axial Skeleton
10. Sacrum
a.
Fusion of 5 vertebrae gives its shape, forming posterior wall of pelvis
b.
Wing-like alae articulate laterally with hip bones forming sacroiliac joints
11. Coccyx
a.
From 3-5 fused vertebrae, is the “tailbone”, remnant of tail that other
vertebrate animals have
C. Bony Thorax
1.
2.
Made up of sternum, ribs, and thoracic vertebrae
Forms a protective, cone-shaped cage around organs of thoracic cavity
(heart, lungs, major blood vessels)
II. Axial Skeleton
3.
Sternum
a.
Breastbone is a flat bone resulting from fusion of three bones and attached to
first 7 pairs of ribs
b.
Three important landmarks
i.
Jugular notch – can be palpated easily, at level of T3
ii.
Sternal angle – transverse ridge where second rib is
iii.
Xiphisternal joint – sternal body and xiphoid process fuse, bottom of sternum
c.
4.
Because it lies so close to body surface, can be aspirated for bone marrow with
a sternal puncture
Ribs – 12 pairs, all articulate with vertebral column posteriorly
a.
True ribs are first 7 pairs attached directly to sternum with costal cartilage
b.
False ribs are next 5 pairs either attached indirectly or not at all (last 2 pairs –
called floating ribs) to sternum
c.
Intercostal space filled with intercostal muscle to aid in breathing
III. Appendicular Skeleton
• Composed of 126 bones of the limbs (appendages) and pelvic and
shoulder/pectoral girdles
A. Bones of the Shoulder Girdle
1.
2.
2 bones – clavicle and scapula
Clavicle – known as collarbone, slender, double-curved; attaches
medially to sternum and laterally to scapula; acts as brace to hold arm
away from thorax
III. Appendicular Skeleton
3.
Scapula – called shoulder blade, looks like a triangle
a.
Acromion process – enlarged end of the scapula, joins laterally with the clavicle
b.
Coracoid process – anchors muscles of the arm
c.
Suprascapular notch – nerve passageway
d.
The scapula does not attach directly to the axial skeleton, but is held on with
muscles, this allows for freer movement
e.
Glenoid cavity – shallow socket that takes the head of the arm
f.
Because of flexibility it can be dislocated easily
III. Appendicular Skeleton
B. Bones of the Upper Limbs
1.
30 bones form each upper limb
2.
Arm – formed by a single bone –
the humerus, a typical long bone
a.
Proximal head of humerus fits into
glenoid cavity of scapula
b.
Greater and lesser tubercles are sites
of muscle attachment
c.
Deltoid tuberosity is in middle of shaft
and where deltoid muscle attaches
d.
Radial groove for radial nerve
III. Appendicular Skeleton
3.
Forearm – two bones – radius and
ulna
a.
Radius is on thumb side and ulna on
little finger side
b.
Connected along length by flexible
interosseous membrane
c.
Head of radial tuberosity where
biceps muscle attaches
d.
Ulna grips humerus in pliers-like joint
III. Appendicular Skeleton
4.
Hand – 3 major parts
a.
Carpals – two rows of four irregular
bones that make up the wrist, held
together with ligaments that restrict
movement
b.
Metacarpals – numbered 1 – 5 from
thumb to little finger, make up palm
of hand
c.
Phalanges – 14 total, each finger has
three (distal, middle, and proximal)
and thumb has 2 (distal and proximal)
III. Appendicular Skeleton
D. Bones of the Pelvic Girdle
1.
2.
3.
Pelvic girdle is formed by two coxal bones (hip bones)
Bony pelvis is formed from coxal bones, sacrum and coccyx
Pelvic girdle is large, heavy bones attached securely to axial skeleton
since the total weight of the upper body rests on the pelvis
4. Deep sockets heavily reinforced by ligaments receive thigh bone
5. Also functions to protect
reproductive organs, urinary
bladder, and part of large
intestine
III. Appendicular Skeleton
6. Coxal bone (hip bone) – fusion of three bones, all meet at deep socket
called the acetabulum that receives head of thigh bone
a.
Ilium – connects posteriorly with sacrum, large flaring bone, where you put
your hands
b.
Ischium – “sit down bone” since it forms most inferior part of coxal
c.
i.
Ischial spine – narrows the outlet of the pelvis through which a baby must pass during
birth
ii.
Greater sciatic notch – allows blood vessels and sciatic nerve to pass from pelvis to
thigh
Pubis – most anterior, pubic bone of each hip fuse anteriorly to form a
cartilaginous joint –
the pubic symphisis
III. Appendicular Skeleton
7.
Dimensions of pelvis for a woman are
very important to allow enough room
for head of infant to pass during birth,
checked by obstetrician
8.
Comparing male and female pelvis
a.
Female inlet larger and more circular
b.
Female pelvis as a whole is shallower, and
bones are lighter and thinner
c.
Female ilia flare more laterally
d.
Female sacrum is shorter and less curved
e.
Female ischial spines are shorter and
farther apart; thus the outlet is larger
f.
Female pubic arch is more rounded
because the angle of the pubic arch is
greater
III. Appendicular Skeleton
D. Bones of the Lower Limbs
1.
Must be thick and strong to carry
our total body weight when
standing erect
2.
Thigh – one bone – femur, heaviest
and strongest bone in body
a.
Ball-like head, neck , and greater and
lesser trochanters
b.
Trochanters and gluteal tuberosity –
sites of muscle attachment
c.
Head articulates with acetabulum in
hip
d.
Neck of femur usually common
fracture site, especially in old age
e.
Slants medially as runs downward to
bring knees in line with center of
gravity
f.
Distally attaches to tibia and patella
III. Appendicular Skeleton
3.
Leg – two bones – tibia and fibula,
connected along length with
interosseous membrane
a.
Tibia (shinbone) more medial,
articulates with femur at proximal
end to form knee joint, distally the
medial malleolus forms inner bulge of
ankle
b.
Fibular – lies laterally to tibia, forms
joints with it proximally and distally,
no part of knee, on distal end the
lateral malleolus forms outer part of
ankle
III. Appendicular Skeleton
4.
Foot – 26 bones, supports weight
and serves as lever for forward
propulsion
a.
Tarsus – forms posterior half of foot,
7 tarsal bones, weight of body carried
mostly by calcaneus (heel) and talus
(ankle)
b.
Metatarsals – 5 form sole of foot
c.
Phalanges – 14, like fingers of hand, all
have 3 (distal, middle, proximal)
except great toe (distal, proximal)
d.
Bones are arranged to form 3 strong
arches, 2 longitudinally and 1
transversely; ligaments and tendons
hold position of bones and muscles
firmly, but allow for springiness, but
weak arches are called fallen arches
or flat feet
IV. Joints
• All bones form a joint with at least one other bone in the body
except the hyoid bone
• Joints (articulations) hold bones together but also give mobility
A. Functional classifications of joints – based on amount of
movement
1.
2.
3.
Synarthroses – immovable joints, mainly axial skeleton
Amphiarthroses – slightly movable joints, mainly axial skeleton
Diarthroses – freely movable joints, mostly in the limbs
IV. Joints
B. Structural classifications of
joints
1.
Fibrous joints
a.
Joined with fibrous tissue
b.
Sutures of the skull are most common
c.
Syndesmoses – the connecting fibers
are longer than those of sutures; thus
the joint has more “give”; distal ends
of tibia/fibula
2.
Cartilaginous joints
a.
Bone ends connected by cartilage
b.
Pubic symphisis, intervertebral joints,
and hyaline cartilage (growth plates,
ribs/sternum)
IV. Joints
3.
Synovial joints
a.
Articulating bone ends are separated
by a joint cavity containing synovial
fluid
b.
Four distinguishing features
i.
Articular cartilage – hyaline
cartilage covers ends of bones
forming joint
ii.
Joint cavity – cavity of joint filled
with lubricating synovial fluid
iii.
Fibrous articular capsule – encloses
joint surfaces by a sleeve or capsule
of fibrous connective tissue and
lined with smooth synovial
membrane
iv.
Reinforcing ligaments – ligaments
reinforcing fibrous capsule
IV. Joints
c.
Associates of joints
i.
Not actually part of joint, but
closely associated, reduce
friction between adjacent
structures during joint activity
ii.
Bursae – flattened sacs lined with
synovial membrane; where
ligaments, muscles, skin,
tendons, or bones rub together
iii.
Tendon sheath – elongated bursa
that wraps completely around a
tendon subjected to friction, like
a hot dog bun
IV. Joints
C. Types of Synovial Joints Based
on Shape
1.
Shape of bone determines
movements allowed at joint
2.
Plane joint – essentially flat, only
short slipping or gliding
movements allowed; nonaxial (no
axis for rotation); intercarpal joints
of wrists
3.
Hinge joint – cylindrical end of one
bone fits into trough-shaped
surface on another bone; uniaxial
(one axis for movement); angular
movement allowed in one plane,
elbows, ankles, phalanges
IV. Joints
4.
5.
6.
7.
Pivot joint – rounded end of bone fits
into a sleeve or ring of bone (and
possibly ligaments); uniaxial;
proximal radioulnar joint and joint
between atlas and dens of axis in
spine
Condyloid joint – “knuckle-like”,
surface of one bone fits into
concavity of another, both surfaces
oval; allows side to side and back and
forth, but no rotation making it
biaxial
Saddle joint – each surface has
convex and concave area like a
saddle, biaxial movement
Ball-and-socket joint – spherical head
fits into round socket of another
bone; multiaxial – allows movement
in all axes including rotation
IV. Joints
8. Dislocations happen when a bone is
forced from normal position,
returning it to its proper position is
reduction
IV. Joints
D. Inflammatory Disorders of Joints
1.
2.
3.
Bursitis – inflammation of the bursae or synovial membrane
Sprains – ligaments and/or tendons reinforcing a joint are excessively
stretched or torn away from bone; painful and heal slowly
Arthritis – actually describes over 100 different joint diseases, all have
same initial symptoms of pain, stiffness, and swelling of the joint
a.
Most widespread, crippling disease in US, 1 out of 7 Americans suffer from it
b.
Acute forms result from bacteria causing increase in and thickening of synovial
fluids leading to increased friction and pain, treated with antibiotics
c.
Chronic forms are conditions that last longer than 3 months and are persistent
IV. Joints
i.
Osteoarthritis (OA) – most common form, degenerative, course is slow and irreversible, but rarely
crippling
–
from wear and tear of weight bearing joints
–
articular cartilage softens, frays, and breaks down exposing the bone which thickens and makes
bone spurs which restrict joint movement
–
pain controlled with analgesics, joint creams, or glucosamine-chondroitin sulfate (nutritional
supplement)
IV. Joints
ii.
Rheumatoid arthritis (RA) {rheumat = susceptible to change or flux} – onset is usually
between 40 – 50 yoa, usually symmetrically
– autoimmune disease where body is trying to destroy its own tissues, triggered by a
bacterial or viral infection
IV. Joints
ii.
Gouty arthritis (gout) – caused from a build up of uric acid
V. Developmental Aspects of the Skeleton
A. Long bone growth
1.
2.
Starts as hyaline cartilage, gradually ossifies, usually complete by 2 yoa
Long bone continues to grow at epiphyseal plate until end of
adolescence
B. Bones of skull
1.
At birth cranium is huge compared to face, grows to ¾ of full size by 2
yoa due to brain growth, usually almost full size by 8-9 yoa, then face
grows to size of skull and differentiates by sex
C. Spinal Curvatures
1.
2.
3.
Born with thoracic and sacral curvatures (primary)
Cervical and lumbar curvatures develop (secondary)
Most spinal problems are congenital, but can be treated
V. Developmental Aspects of the Skeleton
D. Osteoporosis
1.
2.
3.
4.
5.
Bone thinning disease
About 20% of men over age 70 afflicted
About ½ of women over 65 afflicted, though to be caused from a
decrease in estrogen production after menopause
Effect are kyphosis, pathologic fractures, and osteoarthritis
Staying active and getting exercise (including weight-bearing) are the
best prevention