* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The Digestive System
Survey
Document related concepts
Transcript
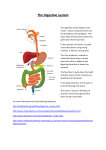
The Digestive System Chapter 16 Introduction to the Digestive System: Also known as the gastrointestinal tract (GIT) or gut. Consists of a long tubular system (alimentary canal). The size and shape changes along the way. Lined by a thin epithelium Tubular structures include: the oral cavity, pharynx, esophagus, stomach, S.intestine and L. intestine Histology of the tubular digestive system: 4 major layers or tunics (from the inside out): Mucosa: (innermost) mucous membrane attached to thin visceral muscle Submucosa: loose connective tissue binds the mucosa to muscularis Muscularis: skeletal and smooth muscle Serosa (outermost): connective & epithelial tissue. Also known as visceral peritoneum (covers & binds organs to one another) extends to mesentery. Introduction to the Digestive System: Accessory structures are also included in this system: Teeth Tongue Salivary glands Liver Gallbladder Pancreas Terms used to refer to different organs: Oral: mouth Gastric: stomach Enteric: small intestine Colonic: large intestine Hepatic: liver Used to describe diseases ( e.g. gastroenteritis = vomiting & diarrhea involving stomach & intestines) Function of the Digestive System: Ingestion and peristalsis: Take in food & water and move it along Digestion: breakdown the food into smaller pieces Absorption: uptake of the small molecules resulting from digestion from the epithelial cells to blood or lymph Function of the Digestive System: Provide nutrients: process of digestion & absorption provides water , electrolytes, vitamins, minerals ( esp. Ca, Fe, Ph) Defecation: eliminate wastes, indigestible (fiber) that cannot be absorbed are excreted in the feces. Oral cavity (buccal): Involved in mastication (chewing process) Lips and cheeks : keep food between upper and lower teeth, assist in speech Hard palate: anterior part of roof of the mouth Soft palate: posterior part Lips: orbicularis oris, covered internally by mucosa & externally by stratified, squamous epithelium (thin, red peeks through) Oral cavity (buccal): Cheeks: form lateral walls, buccinator muscle Tongue: covered in bumps or papillae (friction & taste buds) -attachment to floor of mouth by the frenulum: Attached & supported by hyoid bone Moves food in mouth-collects into BOLUS Holds food in place Aids in swallowing Sensory (taste) speech Oral cavity (buccal): Uvula: Made of muscle & connective tissue covered in mucus membrane Latin word for “grape” Last step in fusion of soft palate Can be divided like an upside down “Y” Aids in swallowing & speech (gutteral sounds) Prevents food from backing up into nasal area Teeth: Dentes collectively called “dentition” 20 deciduous teeth in childhood (start at 6 mo. – 30 mo.) 32 “permanent” in the mandible & maxilla (6 – 25 years) Divided into quadrants: R upper L upper R lower L lower Each quadrant: One central incisor One lateral incisor One canine 1st premolar 2nd premolar 2 molars 3rd molar is “wisdom” tooth Teeth: 4 types Incisors (front): biting Cuspids or Canines (behind incisors): tearing Bicuspids or premolars ( behind cuspids): crushing Molars: (behind bicuspids): crushing Deciduous >>> Permanent <<<< Tooth anatomy: Crown: above gumline Neck: constriction between crown & root Root: below gumline (anchor) 1-3 projections into alveolar bone Enamel: hard, protective outer covering of the crown (protects from acids & wear) Dentin: firm, main structure of the tooth Pulp: arteries, veins and nerves of tooth Tooth anatomy: Apical foramen: where the blood vessels & nerves enter the tooth to become part of the pulp Cementum: covers the dentin which attaches the root to the periodontal ligament. Joint between tooth & bone = gomphosis Gingiva (gum) covers bone Gingiva sulcus : space between gum & tooth (flossing!) Salivary glands: Located outside the oral cavity but have ducts (tubes) leading into cavity. 2 pairs under jaw- submandibular and sublingual (below tongue) 1 pair on side of face near ears- Parotid (serous gland) Mumps: viral inflammation of Parotid, if testicles become inflamed, sterility could occur. MMR vaccine protects. Saliva: 1 ½ Qts of saliva/day >99% water Moistens food –makes it easier to break up and swallow Serous secretion is watery (parotid) increases with parasympathetic stimulation Sympathetic stimulation results in decrease of volume and increased mucus ( thick & sticky) Swallowing: Considered a REFLEX – automatic, preprogrammed response to a stimulus Assists in the movement of the food materials into the stomach Peristaltic contractions move the material down the esophagus to the stomach. Esophagus: A tube which leads from the pharynx to the stomach Contains glands which produce mucus for lubrication of the passage Passes through a small hole in the diaphragm – usually fits tightly (if too large, a hiatal hernia may result Peristalsis – movement of materials into the esophagus from the stomach “heartburn” (section posterior to heart) The Stomach: A bag-like structure which attaches to the esophagus at one end and the small intestine at the other. To be sure food moves in the right direction, numerous sphinters are present: gastroesophogeal/cardiac sphincter: junction between stomach and esophagus Pyloric sphincter: junction between the stomach and the small intestine The Stomach: Inside, large folds (rugae) are present – allow stretching without damaging the wall of the organ. Fundus : expanding storage area Body : storage /digestion area Pylorus : digestion/dispensing area Muscularis – longitudinal, circular & oblique (churning) Glands & cells of the Stomach: Gastric submucosal glands and the lining epithelium produce large amounts of mucus which creates protection on inner surface (prevents damage from HCl/enz) Chief (peptic) cells: pepsinogen converted to pepsin when activated HCl is there (pH must be right) – breaks down protein. Pariietal cells: produces intrinsic factor which is necessary for the absorption of Vit. B12 ( RBC production) and DNA (low pH for pepsin and breakdown of food within the chyme) Lack of B12 can result in Pernicious anemia – note size compared to the lymphocyte Absorption and ulcers: Very little absorption in the stomach (mucus layer interferes) Materials must be both fat & water soluble to be absorbed: Aspirin & ethyl alcohol Ulcers: erosions of the mucosal lining exposing the underlying layers to HCl and enzymes – duodenum common MANY DUE TO Helicobactor pylori Small Intestine: 21’ long! Composed of 3 sections: Duodenum : attached to stomach (10”) Jejunum : middle Ileum :attached to colon Microscopic anatomy: increases digestive and absorptive surface area Plica circularis – small ridges/folds of the inner lining Villi – finger-like projections which extend out of the mucosal surface (blood capillaries and lacteals) looks like shag carpet. Small Intestine: Microvilli –folds of the mucosal epithelial • Contains some membrane-bound enzymes and are the sites of nutrient absorption Enteric lining is replaced every 5 days – this keeps microbes from clinging Intestinal motility: 3-5 hours Segmentation – contraction of circular layer of muscles – mixing motion (contact with enzymes & mucosa) Peristalsis – moves chyme longitudinally down to next segment or into colon Note mesentary (cat) See the lymphatic system? Large Intestine: Consists of Transverse colon-across abdomen Ascending colon-right side of abdomen Descending colon- left side of abdomen Cecum -pouch Ileocecal valve- between ileum & cecum Appendix - closed end of cecum Sigmoid colon- last part of colon, joins Rectum Anal spincter 5 feet in length & ave. 2 ½ in. in diameter Microscopic anatomy of the Large Intestine: Taenia coli: 3 bands of smooth muscle derived from the longitudinal layer of the muscularis Leaves colonic wall thin “gathers” up the colon Haustra: wrinkles/pouches which form as a result of the contraction of the taenia coli Increases surface area for absorption, primarily WATER Functions of the colon: Reabsorption of water from the chyme Some vitamin(Vit B & K) and mineral ( esp. NaCl) absorption Bacterial synthesis of B and K vitamins Storage and elimination of feces: mostly rectum Colonic motility: Normally 18-24 hours are required for material to pass through Peristalsis (wavelike) contractions occur slowly Mass peristalsis or movement – strong, rapid contractions of the colon which moves feces (undigestible materials)into the rectum – occurs several times a day(esp. after a meal – gastro-colonic reflex) Defecation: Spinal reflex which empties the rectum: Pressure increases in the rectum, initiates the defecation reflex which will cause contraction of the rectum to push feces out of the body. Voluntary control can occur because the external sphincter is composed of skeletal muscle which can be voluntarily tightened Liver and Gallbladder: An organ that fill most of the upper abdomen – 2 lobes, right is larger Hepatic, cystic and bile ducts transport bile to intestine or gallbladder Capable of regeneration Each tiny section is capable of doing all of the functions of the liver on a smaller scale. Functions of the liver: Stores glucose, lipids and vitamins (esp. A,D, E, K and B12) and some minerals such as iron & copper Regulates blood composition -keeps levels of nutrients at an adequate level for body cells Removes cell debris, pathogens, hormones, antibodies, toxins, and drugs and converts them into less toxic materials for excretion by the kidneys or in the bile. Functions of the liver: Manufactures the anticoagulant heparin and most of the blood proteins (clotting factors) Can convert some amino acids into other varieties needed by the body. Converts ammonia (a harmful waste product of protein digestion) to urea (less harmful) & is excreted by the kidneys. Produces bile which breaks down fats Kupffer’s cells eat bacteria & old WBC & RBC’s (if not, bilirubin accumulates) Gallbladder: Stores and concentrates the bile while it is not needed in the intestine. Choleliths: gallstones – caused by precipitation of cholesterol when the concentration of some bile components is abnormal. Blood flow: Normally blood goes from heart to a body organ and back to the heart. In the digestive system, blood flows through the PORTAL VEIN to the liver BEFORE going back to the heart – the liver has a chance to stabilize levels of nutrients (some stored) Pancreas: A soft, oblong gland about 6 inches long and 1 inch thick Found beneath the great curvature of the stomach Connected by the common bile duct to the duodenum of the S.I. Composed of 2 lobes – the one inferior to the stomach is larger Microscopic anatomy of the Pancreas: Endocrine portion: Islets of Langerhans – rely on blood to transport their secretions (hormones) Alpha cells make glucagon Beta cells make insulin Exocrine portion: Acini cells release a mixture of secretions: Microscopic anatomy of the Pancreas: Pancreatic juices/enzymes: Protease – completes protein breakdown left undone by pepsin lipase – breaks down lipids Carbohydrase – completes breakdown of carbohydrates (pancreatic amylase) Ribonuclease/deoxyribonuclease – breaks RNA and DNA into their component nucleotides for absorption. Microscopic anatomy of the Pancreas: Other important secretions: Bicarbonate HCO3 • Neutralizes gastric acid • Creates pH 7.0 enteric environment allowing enzymes to work best Control of the digestive system: Primarily controlled by the parasympathetic nervous system (vagus nerve). Hormones can keep an ideal balance for digestion: Stomach: • Gastrin: increases motility and secretions – speeds up movements to help mix food with increased secretions. Control of the digestive system: Duodenum: • Secretin: helps keep proper pH in the small intestine. ( e.g. pH too low, secretin will be released, pancreas makes more bicarbonate, less acidic). • Cholecystokinin: causes contraction of the gallbladder& stimulates bile production. Stimulates enzymes of pancreas. Histamines – sometimes released into the tissues of the digestive system when there is an infection, inflammation or allergic reaction. • This results in increased acid production by the stomach. • Pepsid-AC and Tagamet are actually antihistamines Disorders: Vomiting (emesis): forceful expulsion of the gastric contents – occurs because of a reverse peristalsis that starts at the pylorus. Gastric reflux (GERD): “heartburn” usually result of excessive gastric motility, hiatal hernia, weak sphincter, or excessive acid production of the stomach Disorders: Pyloric stenosis: defect in pyloric valve – will not allow food to pass into duodenum (often requires surgery) Diarrhea: excess water in the feces Intestinal irritant ( microbe or toxin) or injury to lining (cancer or infiltrate) Unabsorbed molecules (lactose or laxatives) Disorders: S. Intestine has too much chyme passed on to the colon and it is unable to deal with it. If caused by L. Intestine, there is a proper amount of chyme, but unable to deal with it, partially formed Constipation: excessive distension of the rectum & colon due to buildup Caused by decreased motility from nerve/muscle damage, stress, pregnancy, diet Inflammatory disorders: Gastritis Enteritis Hepatitis Pancreatitis Colitis Appendicitis Peritonitis Print materials: Mini Poster My Plate Contributing Factors to Overweight/Obesity computers Junk food Behavioral Factors Portion sizes Video games t.v. child Fast food genetics Pop machines Family influence Lack of P.A. Meals Away from home Our kids are being bombarded with all of these factors that promote a sedentary, calorie laden lifestyle. Look at what’s happened over the last 50 years… Obesity Trends in Children and Adolescents Ogden, et al. JAMA 2002;288;1728-1732 1960’s 2-5 year olds 6-11 year olds 12-19 year 19881994 19992000 7.2% 10.4% 4% 11.3% 15.3% 5% 10.5% 15.5% Unfortunately, our kids are just following our lead. Have you noticed your pants getting You’re not alone. tighter? Obesity Trends* Among U.S. Adults BRFSS, 1991-2002 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) 1991 1995 2002 No Data <10% 10%–14% 15%–19% 20%–24% ≥25% Obesity Trends* Among U.S. Adults BRFSS, 1985 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% Obesity Trends* Among U.S. Adults BRFSS, 1988 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% Obesity Trends* Among U.S. Adults BRFSS, 1989 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% Obesity Trends* Among U.S. Adults BRFSS, 1992 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% 15%–19% Obesity Trends* Among U.S. Adults BRFSS, 1993 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% 15%–19% Obesity Trends* Among U.S. Adults BRFSS, 1995 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% 15%–19% Obesity Trends* Among U.S. Adults BRFSS, 1998 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% 15%–19% ≥20 Obesity Trends* Among U.S. Adults BRFSS, 1999 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% 15%–19% ≥20 Obesity Trends* Among U.S. Adults BRFSS, 2001 (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% 15%–19% 20%–24% ≥25% Obesity Trends* Among U.S. Adults BRFSS, 2002 (*BMI 30, or ~ 30 lbs overweight for 5’4” person) (*BMI ≥30, or ~ 30 lbs overweight for 5’ 4” woman) No Data <10% 10%–14% 15%–19% 20%–24% Source: Behavioral Risk Factor Surveillance System, CDC ≥25% Obesity Trends* Among U.S. Adults BRFSS, 2005 (*BMI ≥30, or ~ 30 lbs. overweight for 5’ 4” person) No Data <10% 10%–14% 15%–19% 20%–24% 25%–29% ≥30% Obesity Trends* Among U.S. Adults BRFSS, 2010 (*BMI ≥30, or ~ 30 lbs. overweight for 5’ 4” person) No Data <10% 10%–14% 15%–19% 20%–24% 25%–29% ≥30% Health Implications Short Term Hypertension Abnormal glucose metabolism Accelerated growth Orthopedic problems Sleep apnea Psychosocial problems Asthma Long Term Increased risk for CVD Increased risk for some cancers Increased health care costs Psychosocial issues Lead to being an obese adult Do Overweight kids make obese adults? If a child is overweight at 6 years of life, the likelihood that he or she will be obese as an adult is greater than 50% NEJM Source: Whitaker RC et at. (1997) If an adolescent is obese, then he or she has a 70% chance of remaining obese Source; Epstein LH et al. (1985) AJCN