* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Normal Sinus Rhythm
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Jatene procedure wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Electrocardiography wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
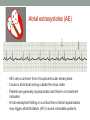
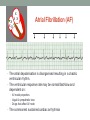
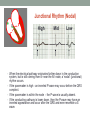
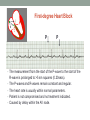
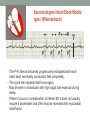
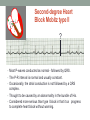
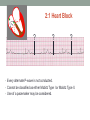
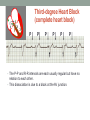
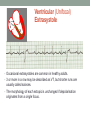
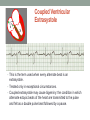
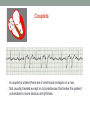
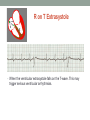
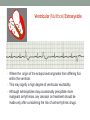
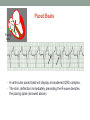
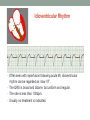
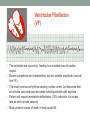
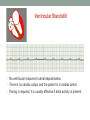
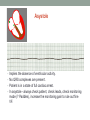
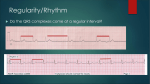
© Hayley Coxon 2014 ECG Rhythm Recognition What to Look for on a rhythm strip • • • • • Is there electrical activity? Is it regular or irregular? What is the QRS rate? Is the QRS narrow or wide (>0.12 s)? Is atrial activity present: – If P waves, are they consistent? – If other activity, what? • How is P wave related to QRS? – Is there a P wave in front of every QRS complex? – What Is the PR interval too short (<0.12 s) or too long (>0.2 s)? – Is the PR interval constant or does it vary? © Hayley Coxon 2014 Muscle Tremor P P P P • All waveforms are present, but are difficult to define due to the wavering appearance on the isoelectric line. • Common causes of muscle tremor are patient shivering or anxiety. • It may be difficult to accurately assess an ECG where muscle tremor is present. © Hayley Coxon 2014 Electrical Interference • It may be difficult to make any assessment of an ECG where there is electrical interference; none of the waveforms are clearly defined. • Common causes of this phenomenon are any electrical appliances in close proximity to the ECG machine: i.e TV, electrical beds, infusion pumps etc. • Usually once all appliances are unplugged, a satisfactory quality ECG can be carried out. © Hayley Coxon 2014 x Atrial extrasystoles (AE) • AE’s are a common form of supraventricular extrasystole. • Cause is atrial beat arising outside the sinus node. • Patients are generally asymptomatic and there is no treatment indicated. • A trial extrasystole falling on a critical time of atrial repolarisation may trigger atrial fibrillation (AF) in some vulnerable patients. © Hayley Coxon 2014 x x x x xx Atrial Fibrillation (AF) • The atrial depolarisation is disorganised resulting in a chaotic ventricular rhythm. • The ventricular response rate may be normal/fast/slow and dependent on: • AV nodal properties • Vagal & sympathetic tone • Drugs that affect AV node • The commonest sustained cardiac arrhythmia © Hayley Coxon 2014 © Hayley Coxon 2014 Atrial Fibrillation • It’s prevalence doubles with each advancing decade of life • Risk factors for developing AF • Increasing age, diabetes, HTN, valve disease • Often caused by coexisting medical conditions • cardiac and non cardiac • Adverse effects results from • haemodynamic changes – 20% reduction in CO • thromboembolic complications – prothrombotic state • Major cause of morbidity and mortality, increasing risk of death, heart failure and embolic phenomena including stroke • Treatment is usually with oral drug therapy, although may be successfully electrically cardioverted in patients with persisting AF of recent onset. x xx Atrial Flutter • A malfunction in the pattern of atrial depolarisation. A flutter usually gives atrial waves in the range of 280-320bpm. • The AV node usually blocks 1/2 of these impulses and gives a ventricular response rate of 150bpm. • Atrial flutter is usually regular in rhythm and displays a ‘sawtoothed’ appearance (especially V1) as above. • Very responsive to DC electrical cardioversion. © Hayley Coxon 2014 x Supraventricular Tachycardia (SVT) • SVT is a general term for tachycardias that originate above the ventricles. • Rate may be in the range of - 150-250bpm • Commonly starts in early adult life and is normally inconvenient but benign. • Adenosine to block AV response may slow the rate to determine underlying atrial rhythm or may facilitate chemical cardioversion. © Hayley Coxon 2014 Junctional Rhythm (Nodal) x High Mid Low • When the electrical pathway originates further down in the conduction system, but is still coming from or near the AV node, a ‘nodal’ (junctional) rhythm occurs. • If the pacemaker is high - an inverted P-wave may occur before the QRS complext. • If the pacemaker is within the node - the P-wave is usually absent. • If the conducting pathway is lower down, then the P-wave may have an inverted appearance and occur after the QRS and even resemble a S wave. © Hayley Coxon 2014 Supraventricular Tachycardias • Atrial Fibrillation • Atrial flutter • Atrial tachycardia, • Automatic junctional tachycardia, • Atrioventricular re-entry tachycardia (AVRT) • WPW • AV nodal re-entry tachycardia • Can be intermittent and self-terminating © Hayley Coxon 2014 © Hayley Coxon 2014 Wolff-Parkinson-White Syndrome (WPW) Normal pathway Accessory pathway Paroxysmal tachycardia Delta wave anterograde / retrograde conduction PR • WPW is a syndrome (AVRT) with a characteristic electrocardiogram shortened PR interval (<0.12secs) and a slurred upstroke on the QRS complex (delta wave) together with a tendency to supraventricular arrhythmias. • It is caused by an accessory conduction pathway which bypasses the AV node, Bundle of Kent • Type A and B depending on the side of the accessary pathway First-degree Heart Block P P • The measurement from the start of the P-wave to the start of the • • • • R-wave is prolonged to >5 sm squares (0.20secs). The P-waves and R-waves remain constant and regular. The heart rate is usually within normal parameters. Patient is not compromised and no treatment indicated. Caused by delay within the AV node. © Hayley Coxon 2014 Second-degree Heart Block Mobitz type I (Wenckebach) P P P R P P ? • The P-R interval becomes progressively elongated with each heart beat; eventually conduction fails completely. • The cycle then repeats itself once again. • May be seen in individuals with high vagal tone especial during sleep. • Where it occurs in complication of inferior MI, it does not usually require a pacemaker and often may be reversed with myocardial reperfusion. © Hayley Coxon 2014 Second-degree Heart Block Mobitz type II ? • Most P-waves conducted as normal - followed by QRS. • The P-R interval is normal and usually constant. • Occasionally, the atrial conduction is not followed by a QRS complex. • Thought to be caused by an abnormality in the bundle of His. • Considered more serious than type I block in that it can progress to complete heart block without warning. © Hayley Coxon 2014 2:1 Heart Block ? ? ? • Every alternate P-wave is not conducted. • Cannot be classified as either Mobitz Type I or Mobitz Type II. • Use of a pacemaker may be considered. © Hayley Coxon 2014 Third-degree Heart Block (complete heart block) x x P P P P P P • The P-P and R-R intervals are each usually regular but have no relation to each other. • This dissociation is due to a block at the AV junction. © Hayley Coxon 2014 Ventricular (Unifocal) Extrasystole x • Occasional extrasystoles are common in healthy adults. • 3 or more in a row may be described as VT, but shorter runs are usually called salvoes. • The morphology of each ectopic is unchanged if depolarisation originates from a single focus. © Hayley Coxon 2014 Coupled Ventricular Extrasystole x • This is the term used when every alternate beat is an extrasystole. • Treated only in exceptional circumstances. • Coupled extrasystole may cause bigeminy: the condition in which alternate ectopic beats of the heart are transmitted to the pulse and felt as a double pulse beat followed by a pause. © Hayley Coxon 2014 Couplets x • A couplet is where there are 2 ventricular ectopics in a row. • Not usually treated except in circumstances that make the patient vulnerable to more serious arrhythmias © Hayley Coxon 2014 R on T Extrasystole x • When the ventricular extrasystole falls on the T-wave. This may trigger serious ventricular arrhythmias. © Hayley Coxon 2014 Ventricular (Multifocal) Extrasystole x x x • Where the origin of the ectopic beat originates from differing foci within the ventricle. • This may signify a high degree of ventricular excitability. • Although extrasystoles may occasionally precipitate more malignant arrhythmias, any decision on treatment should be made only after considering the risk of anti-arrhythmic drugs. © Hayley Coxon 2014 Paced Beats Pacing wire x • A ventricular paced beat will display a broadened QRS complex. • The slim, deflection immediately preceding the R-wave denotes the pacing spike (arrowed above). © Hayley Coxon 2014 Idioventricular Rhythm x • Often seen with reperfusion following acute MI, idioventricular rhythm can be regarded as ‘slow VT’. • The QRS is broad and bizarre, but uniform and regular. • The rate is less than 100bpm. • Usually no treatment is indicated. © Hayley Coxon 2014 Torsades de Pointes • From the French ‘twisting of points’. This describes a form of VT where the cardiac axis twists round the isoelectric line. • The rhythm may be intermittent and self-terminating. If it lasts more than a few seconds the patient will become symptomatic. • Common causes are electrical imbalance - i.e K+ and/or Mg++ depletion or prolonged Q-T interval frequently caused by drugs such as Sotalol/Amiodarone or tricyclic antidepressants. © Hayley Coxon 2014 x Ventricular Tachycardia (VT) • The origin of the heartbeat is in the ventricles, producing a QRS complex >0.12secs. • 3 ventricular beats in succession may be called VT (or salvoes). • VT can range in rate from 100-300bpm and the patient may be conscious and asymptomatic, symptomatic, or unconscious. Treatment will depend principally on the patients’ clinical status. © Hayley Coxon 2014 x x xx Ventricular Fibrillation (VF) x • The ventricles are ‘quivering’, leading to a complete loss of cardiac • • • • output. Bizarre complexes are characteristic, but are variable amplitude (course / fine VF). The most common arrhythmia causing cardiac arrest, but becomes finer as minutes pass and soon becomes indistinguishable with asystole. Patient will require immediate defibrillation (10% reduction in success rate as each minute passes). Most common cause of death in early acute MI. © Hayley Coxon 2014 Ventricular Standstill • No ventricular response to atrial depolarisation. • There is no cardiac output and the patient is in cardiac arrest. • Pacing is required. It is usually effective if atrial activity is present. © Hayley Coxon 2014 Asystole • Implies the absence of ventricular activity. • No QRS complexes are present. • Patient is in a state of full cardiac arrest. • In asystole - always check patient, check leads, check monitoring mode (? Paddles), increase the monitoring gain to rule out fine VF. © Hayley Coxon 2014 © Hayley Coxon 2014