* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download neuropathy classification
Biochemistry of Alzheimer's disease wikipedia , lookup
Embodied language processing wikipedia , lookup
Central pattern generator wikipedia , lookup
Evoked potential wikipedia , lookup
Nutrition and cognition wikipedia , lookup
Microneurography wikipedia , lookup
Neuroregeneration wikipedia , lookup
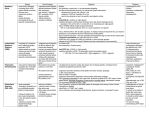
NEUROPATHY CLASSIFICATION Does the patient actually have a neuropathy? Causes of generalized weakness: 1) Motor Neuron Disease (MND) 2) Disorders of the NMJ: Myasthenia 3) Myopathy MND: Unknown aetiology Affects anterior horn cells, motor nuclei of medulla & descending tracts So: MIXTURE OF UMN & LMN signs FASCICULATIONS – almost always present Reflexes often present/ 15-20% Get sensory Syx, rarely any objective sensory signs Peripheral neuropathy can also be mimicked by: 1) Myelopathy 2) Syringomyelia 3) Dorsal column disorders (eg tabes dorsalis) NB: It is important to distinguish whether the neuropathy is axonal, demyelinating, or both. This differentiation is best achieved using nerve conduction studies (NCS) and electromyography (EMG). ARE SIGNS FOCAL? Entrapment Common sites of compression: carpal tunnel syndrome ulnar neuropathy at the elbow peroneal neuropathy at fibular head Myxedema Rheumatoid arthritis Amyloidosis Acromegaly Compressive neuropathies Trauma Ischemic lesions Diabetes mellitus Vasculitis Leprosy Sarcoidosis Neoplastic infiltration or compression ARE SIGNS MULTI-FOCAL? (suggests a mononeuritis multiplex) Diabetes mellitus Vasculitis Polyarteritis nodosa Systemic lupus erythematosus Sjögren's syndrome Sarcoidosis Leprosy HIV/AIDS Multifocal variant of CIDP Hereditary predisposition to pressure palsies NB: Mononeuritis multiplex may result in sensory abnormalities in specific nerve or nerve root distributions Affects two or more non-contiguous peripheral nerves in separate parts of the body Pattern of involvement is random, multifocal, and typically evolves quickly Distal Symmetric Sensorimotor (Axonal) Polyneuropathies NB: Most toxic and metabolic neuropathies are initially sensory and later may involve the motor fibers (ALSO REMEMBERED BY THE DAMMIT BICH MNEMONIC) Endocrine diseases Diabetes mellitus Hypothyroidism Acromegaly Nutritional diseases Alcoholism Vitamin B12 deficiency Folate deficiency Whipple's disease Postgastrectomy syndrome Gastric restriction surgery for obesity Thiamine deficiency Hypophosphatemia Critical illness polyneuropathy Connective tissue diseases Rheumatoid arthritis Polyarteritis nodosa Systemic lupus erythematosus Churg-Strauss vasculitis Cryoglobulinemia Amyloidosis Gouty neuropathy Carcinomatous axonal sensorimotor polyneuropathy Lymphomatous axonal sensorimotor polyneuropathy Infectious diseases Acquired immunodeficiency syndrome Lyme disease Sarcoidosis Toxic neuropathy Acrylamide Carbon disulfide Dichlorophenoxyacetic acid Ethylene oxide Hexacarbons Carbon monoxide Organophosphorus esters Glue sniffing Metal neuropathy Chronic arsenic intoxication Mercury Gold Thallium Medications (see Table 8) NB: Motor symptoms such as weakness and wasting also commence distally Common complaints are tripping on the toes and loss of grip strength may have cramps or fasciculations Polyneuropathies involve more than one type of nerve but there is usually one (e.g. sensory or motor, large fiber or small fiber) that is predominant. Proximal Symmetric Motor Polyneuropathies Guillain-Barré syndrome Chronic inflammatory demyelinating polyradiculoneuropathy Diabetes mellitus Porphyria Osteosclerotic myeloma Waldenstrom's macroglobulinemia Monoclonal gammopathy of undetermined significance Acute arsenic polyneuropathy Lymphoma Diphtheria HIV/AIDS Lyme disease Hypothyroidism Vincristine (Oncovin, Vincosar PFS) toxicity Proximal involvement may result in difficulty climbing stairs, getting out of a chair, lifting and swallowing, and in dysarthria Neuropathies with cranial nerve involvement A limited number of neuropathies involve the cranial nerves (Table 4) Diabetes mellitus Guillain-Barré syndrome HIV/AIDS Lyme disease Sarcoidosis Neoplastic invasion of skull base or meninges Diphtheria Neuropathies predominant in upper limbs Another uncommon pattern is greater involvement of the arms than the legs Guillain-Barré syndrome Diabetes mellitus Porphyria Hereditary motor sensory neuropathy Vitamin B12 deficiency Hereditary amyloid neuropathy type II* Lead neuropathy Pure sensory neuropathies and neuronopathies Paraneoplastic Medications (see Table 8) Carcinomatous sensory neuronopathy Lymphomatous sensory neuronopathy Sjögren's syndrome Paraproteinemias Nonsystemic vasculitic neuropathy Idiopathic sensory neuronopathy Styrene-induced peripheral neuropathy Primary biliary cirrhosis Crohn's disease Chronic gluten enteropathy Vitamin E deficiency Hereditary sensory neuropathy types I and IV Friedreich's ataxia Small-fiber neuropathies (often painful) Diabetes mellitus Alcoholic neuropathy Amyloidosis AIDS Leprosy Hereditary Small-fiber neuropathies often present with burning pain, lightning-like or lancinating pain, aching, or uncomfortable paresthesias (dysesthesias). Patients may complain of pain with innocuous stimuli such as sheets rubbing over their feet (allodynia). They may also describe a tight, band-like sensation around the ankles or wrists. Sensory symptoms include tingling or paresthesias, increased sensation in affected areas (hypesthesia), and numbness or reduced sensation Neuropathies with autonomic involvement Diabetic neuropathy Alcoholic neuropathy Guillain-Barré syndrome Paraneoplastic neuropathy HIV/AIDS Lymphoma Amyloidosis Porphyria Thallium, arsenic, mercury toxicity Thiamine deficiency Vincristine (Oncovin, Vincosar PFS) toxicity Acute pandysautonomia Neuropathies with Abrupt/Rapid Onset Diabetes mellitus Cranial neuropathies Diabetic amyotrophy Ischemic neuropathies Polyarteritis nodosa Rheumatoid arthritis Nerve compression Hemorrhage Swelling within a restricted anatomic compartment (e.g., anterior tibial syndrome) Direct external compression Penetrating wounds Thermal injury Iatrogenic (e.g., injection into nerves) Drugs Causing Neuropathies Axonal Vincristine (Oncovin, Vincosar PFS) Paclitaxel (Taxol) Nitrous oxide Colchicine (Probenecid, Col-Probenecid) Isoniazid (Laniazid) Hydralazine (Apresoline) Metronidazole (Flagyl) Pyridoxine (Nestrex, Beesix) Didanosine (Videx) Lithium Alfa interferon (Roferon-A, Intron A, Alferon N) Dapsone Phenytoin (Dilantin) Cimetidine (Tagamet) Disulfiram (Antabuse) Chloroquine (Aralen) Ethambutol (Myambutol) Amitriptyline (Elavil, Endep) Demyelinating Amiodarone (Cordarone) Chloroquine Suramin (Fourneau 309, Bayer 205, Germanin) Gold Neuronopathy Thalidomide (Synovir) Cisplatin (Platinol) Pyridoxine EXAMINATION: Peripheral neuropathies are by definition LOWER MOTOR NEURONE lesions Cranial Nerves: Can provide evidence of: Mononeuropathies OR Proximal involvement NB: Motor nerves: V, VII, IX/X, XI, XII Motor Examination General Inspection Fasciculations Cramps Trophic changes: in Severe, longstanding neuropathy pes cavus kyphoscoliosis loss of hair in affected areas ulcers Trophic changes are most prominent in: Diabetes Amyloid neuropathy Leprosy Hereditary motor sensory neuropathy (HMSN) with prominent sensory involvement Hereditary sensory neuropathy Tone: Normal or Power: Pattern of weakness: Symmetric/Assymetric Distal/Proximal Confined to Particular nerve Plexus Nerve root level Proximal weakness results in an inability to squat or to rise unassisted from a chair. A bilateral foot drop may result in a steppage gait in which the patient must lift the knees very high in order to clear the toes Reflexes: or absent Sensation: Eg: Distal symmetric sensorimotor neuropathy light touch, pinprick and temperature in a stocking-and-glove distribution Vibration and position sense are reduced in the distal legs prior to involvement of the arms In severe loss of position sense, there may be athetoid movement of the fingers or arms when the eyes are closed (pseudoathetosis) or a Romberg sign Mononeuritis Multiplex may have sensory loss in specific nerve distributions EXTRAS Postural Hypotension: Autonomic neuropathy Respiratory rate &Vital Capacity GBS Lymphadneopathy/Hepato/splenomegaly Ie Evidence of systemic disease INITIAL Ix: Blood glucose HbA1C FBE U&E LFT (alcoholic) ESR Urinalysis B12/Folate TFT ECG: To look for sinus arrhythmia (lost in autonomic neuropathy) Postural BP’s CSF: In myelinopathies & polyradiculopathies High protein & < 5 WBC GBS CIDP Cytology: Lymphoma CMV DNA (AIDS) NERVE BIOPSY: Only helpful in very specific cases to diagnose vasculitis, leprosy, amyloid neuropathy, leukodystrophies, sarcoidosis and, occasionally, CIDP Sural nerve is the one most commonly selected for biopsy Cx: infection, poor wound healing and painful dysesthesias