* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiovasculat presentation from Kay Elliot
Saturated fat and cardiovascular disease wikipedia , lookup
Baker Heart and Diabetes Institute wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Rheumatic fever wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Electrocardiography wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Jatene procedure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Infective endocarditis wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Coronary artery disease wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
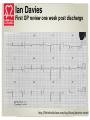
Ian Davies Ian Davies Mr Davies is a 57 year old –self-employed IT consultant Discharge summary: • STEMI – PPCI- 2 x DES • Past medical history: nil of note • Medication: aspirin 75mg, clopidogrel 75mg, bisoprolol 2.5mg, ramipril 2.5mg, atorvastatin 80mg & GTN spray Ian Davies First GP review one week post discharge • He continues to smoke (although he’s cut down a bit) and he has a strong family history of coronary heart disease ; offered smoking cessation support • Reports occasional left chest discomfort always at rest eases if he changes position • Blood Pressure: 145/90mmhg & Heart Rate: 50 bpm, regular • Diet high in sat fats – BMI 34; – hasn’t engaged with cardiac rehab Ian Davies First GP review one week post discharge http://lifeinthefastlane.com/ecg-library/anterior-stemi/ What event and interventions has Mr Davies experienced? STEMI – PPCI- 2 x DES • ST elevation myocardial infarction treated with • Primary percutaneous coronary intervention and • 2 x Drug eluting stents What’s missing? Discharge summary: • STEMI – PPCI- 2 x DES • Past medical history: nil of note • Medication: aspirin 75mg, clopidogrel 75mg, bisoprolol 2.5mg, ramipril 2.5mg, atorvastatin 80mg & GTN spray Medication changes needed? Discharge medication GP Review aspirin 75mg clopidogrel 75mg bisoprolol 2.5mg ramipril 2.5mg atorvastatin 80mg GTN spray • • • • • • • Is Mr Davies taking them? How/when is he taking them? Side-effects/problems Uptitrate/monitor (ramipril/bisoprolol) How to use GTN When to stop clopidogrel Eplerenone? “For patients who have had an acute MI and who have symptoms and/or signs of heart failure and left ventricular systolic dysfunction, initiate treatment with an aldosterone antagonist licensed for post-MI treatment within 3–14 days of the MI, preferably after ACE inhibitor therapy” (NICE, CG172) Secondary Prevention & Statins Atorvastatin 80mg – do not delay • This should be continued unless the patient cannot tolerate, has abnormal LFT’s, or patient preference (AST, ALT, GGT: do not exclude if transaminases less than 3 times the upper limit) • Target <40 % reduction in Non HDL • Check LFT at 3 months, then at 12 months (annual review?) • If unexplained muscle symptoms consider stopping statin immediately – (Check CK: x 5 upper limit of normal or more - stop statin) Follow-up Check patients’ understanding of their: • • • • • Diagnosis and risk of re-stenosis secondary prevention measures required medication regime cardiac rehabilitation what do they think are the key problems; work, travel, finance, getting back to hobbies/driving…..? Plan for: • • • • drug titration length of dual anti-platelet therapy follow-up blood tests/physical examination Check follow-up with cardiologist is in place John Bryant John Bryant Mr Bryant is 64 years old and had a primary prevention CRT-D fitted in 2010 for severe LV systolic dysfunction and he also is known to have ischaemic heart disease. He felt much better in terms of his heart failure symptoms after implant initially Over the last three weeks his heart failure symptoms have returned; He has gained 5 lbs in weight, he is breathless on minimal exertion and his ankles are swollen. John Bryant What action might you take? John Bryant • ask about other symptoms; angina, palpitations, syncope/pre-syncope, orthopnoea, paroxysmal nocturnal dyspnoea • physical examination • blood Tests: U&E, ?FBC, • consider ECG depending on examination and symptoms • treat heart failure symptoms • Is medication optimised? Check medication concordance and for any significant lifestyle change Evidence Based Medicine for LVSD Optimal titration of appropriate • ACE Inhibitors (CONSENSUS, SOLVD, SAVE, AIRE,TRACE) • βblockers (CIBIS II, COPERNICUS, MERIT-HF, SENIORS) • MRAs (RALES, EMPHASIS-HF) reduces mortality at 12 months from 44% to 17% National Heart Failure Audit, 2015 John Bryant • Contact ICD centre for sooner ICD check: – is LV lead working? – Does he need biventricular optimisation? • Is referral to or advice from cardiologist indicated? John Bryant Calculate stroke risk score with: • Symptomatic, asymptomatic, paroxysmal, persistent or permanent atrial fibrillation • Atrial Flutter • a continuing risk of arrhythmia recurrence after cardioversion back to sinus rhythm Do not offer Aspirin monotherapy solely for stroke prevention to people with atrial fibrillation *National Clinical Guideline Centre (NCGC) 2014 **The Task Force for the Management of Atrial Fibrillation of the European Society of Cardiology (ESC - 2012) Stroke risk CHA2DS2-VASc Score C H A D S V A Sc Congestive heart failure? Hypertension Age >75 yrs Diabetes Stroke ,TIA or thromboembolism Vascular disease Age 65-74 Sex category (female) 1 1 2 1 2 1 1 1 Points (max 9) Ensure that anticoagulation is discussed and offered to individuals with a score of ≥2, and considered for all those with a score of 1, except if they are aged <65 yrs and the point is due to female gender alone (NICE, CG180) Bleeding Risk: HAS-BLED H A S B L E D Hypertension Abnormal renal and liver function* Stroke Bleeding Labile INRs Elderly >65years Drugs eg aspirin, NSAID, alcohol* 1 1 or 2 1 1 1 1 1 or 2 *1 point each. A Score >=3 indicates high risk Therefore, caution required with either anti-platelet or oral anticoagulant therapy Atrial Fibrillation ESC Guidelines 2012 • • • • • • • • • Most common arrhythmia in HF Increases stroke risk May lead to worsening of symptoms Identify correctable causes Identify potential precipitating factors Determine rhythm or rate control strategy Assess for thromboembolism prophylaxis In LVSD BB preferred to digoxin for rate control IN HF-PEF rate limiting CCBs are an alternative Typical course of heart failure http://www.nhsiq.nhs.uk/media/2574509/end-of-life-care-in-heart-failure-framework-for-implementation.pdf Mike Baker Mike Baker Mr Baker is 46 years old, married with two daughters (five and three years old) PMH: Born with a malformed aortic valve Developed flu like symptoms, which would not resolve Mike Baker • Reviewed by GP’s (x3) over five months • Diagnosed with flu • Treated with steroids, NSAID’s and sent for chest x-ray Mike Baker He continued to worsen over five months: • One stone weight loss • Severe cough • Breathless on stairs Mike Baker His wife finally took him to hospital: • Diagnosed with endocarditis (aortic valve) • IV antibiotics (via PICC Line) • Developed atrial fibrillation • Cardiac arrest and failed resuscitation Mrs Claire Baker Following the death of her husband Mrs Baker would like to know that: • Those at risk know what to look out for • Healthcare practitioners remember to consider/investigate possible endocarditis At risk of infective endocarditis: • acquired valvular heart disease with stenosis or regurgitation • hypertrophic cardiomyopathy • previous infective endocarditis • structural congenital heart disease, including surgically corrected or palliated structural conditions (but excluding isolated atrial septal defect, fully repaired ventricular septal defect or fully repaired patent ductus arteriosus, and closure devices that are judged to be endothelialised) • valve replacement NICE, CG64 Advise ‘at risk’ patients • • • • • Good oral hygiene & regular dental review Avoid body piercing and tattooing Don’t inject non-prescription drugs Any infection; report it to your GP immediately carry an Endocarditis warning card; show to any other health professionals who may need to give you treatment CVD Clinical Development Coordinator Can provide in-house education for your team: [email protected] • Often interactive with questions and case studies throughout Presentations • Facilitated discussions & reflection • Case studies Group Work • Individual practice (ECG reading) – worksheets, practice ECG’s • Quizzes Individual work or in pairs How to order BHF Resources All our resources are free to order, although we do ask for a donation if you can afford one. Web: bhf.org.uk/publications Call: 0870 600 6566 Email: [email protected] References • • European society of cardiology ( 2012) Guidelines for the diagnosis & treatment of acute and chronic heart failure. The task force for the diagnosis and treatment of chronic heart failure of the European society of cardiology, European Heart Journal National Institute for Clinical Excellence Acute Heart Failure (CG187) October, 2014 Atrial Fibrillation (CG180) June 2014 Chest pain of recent onset (CG 95) March 2010 Chronic Heart Failure (CG 108) August 2010 Management of stable angina (CG 126) July 2011 Unstable angina and NSTEMI (CG 94) March 2010 MI with ST segment elevation (CG 167) July 2013 MI – secondary prevention (CG172) November 2013 NICE quality standard (QS99) September 2015 Prophylaxis against infective endocarditis overview (CG64) Sept, 2015 • http://www.nhsiq.nhs.uk/media/2574509/end-of-life-care-in-heart-failureframework-for-implementation.pdf • National Heart Failure Audit (2015) https://www.ucl.ac.uk/nicor/audits/heartfailure • British heart Foundation (www.bhf.org.uk)