* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download File
Heart failure wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Electrocardiography wikipedia , lookup
Atrial septal defect wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
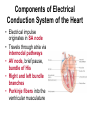
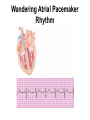
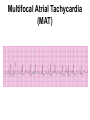
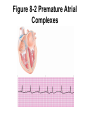
8 Introducing the Atrial Rhythms Introducing the Sinus Rhythms • Objectives – Discuss the origin of the atrial rhythms – Recall the components of the electrical conduction system of the heart – Identify a wandering atrial pacemaker rhythm, including EKG characteristics – Describe a premature atrial contraction, including EKG characteristics – Identify atrial flutter rhythm, including EKG characteristics Introducing the Sinus Rhythms • Objectives (continued) – Describe atrial fibrillation rhythm, including EKG characteristics – Describe supraventricular tachycardia, including EKG characteristics – Discuss clinical significance of atrial rhythms – Describe EKG characteristics of WolffParkinson-White syndrome Origin of the Atrial Rhythms • The rhythms are classified according to the heart structure in which they begin, or their site of origin • Sinoatrial (SA) node fails to generate an impulse, atrial tissues, or internodal pathways may initiate an impulse Origin of the Atrial Rhythms • These are Atrial Dysrhythmias • Rhythms not considered life-threatening or lethal; They must however, provide continuous assessment Components of Electrical Conduction System of the Heart • Electrical impulse originates in SA node • Travels through atria via internodal pathways • AV node, brief pause, bundle of His • Right and left bundle branches • Purkinje fibers into the ventricular musculature Electrical Conduction System of the Heart Pacemaker Sites Wandering Atrial Pacemaker Rhythm • They occur when pacemaker sites wander, or travel, from SA node to other pacemaker sites in atria, internodal pathways, or AV Node • SA node remains basic pacemaker Wandering Atrial Pacemaker Rhythm • Observation of at least three different P waves required • Size and shape of P waves vary according to site of origin • The P waves may appear upright, inverted, or absent waveforms Wandering Atrial Pacemaker Rhythm • The absence of P wave may indicate P wave buried in QRS complex • PR interval may be regular, vary based on point of origin • Produces no symptoms and only recognized by EKG observation Wandering Atrial Pacemaker Wandering Atrial Pacemaker Rhythm Multifocal Atrial Tachycardia (MAT) • A variant of wandering atrial pacemaker • Occurs when the rate reaches 100 bpm or greater • May be confused with atrial fibrillation • Observed in patients with advanced chronic obstructive pulmonary disease, digoxin toxicity, and electrolyte imbalances. Multifocal Atrial Tachycardia (MAT) Premature Atrial Contractions (Complexes) or PACs • A single electrical impulse that originates outside the SA node in the atria • Can occur in the atria, AV junction, or in the ventricles • The premature beat is a complex that arises earlier than next expected beat Premature Atrial Contractions (Complexes) or PACs • The word contraction commonly used to describe premature beats • All complexes represent only electrical activity of the heart • Complexes do not show mechanical activity. • Should use complexes rather then contraction Premature Atrial Complexes • An incomplete, or noncompensatory, pause often follows a PAC – Looks like normal complexes of underlying rhythm – Underlying rhythm is interrupted due to PAC – After noncompensatory pause, underlying rhythm of heart returns, and continues until next PAC occurs Premature Atrial Complexes Figure 8-2 Premature Atrial Complexes Premature Atrial Complexes • Two sequential PACs – Occur in pairs • Atrial bigeminy – Every other beat PAC • Atrial trigeminy – Every third beat PAC Premature Atrial Complexes • Remember – Premature atrial complexes look very much like the normal complexes of the underlying rhythm Premature Atrial Complexes • Causes include – Use of stimulants (caffeine, alcohol) hypoxia, increased sympathetic tone, imbalances of electrolytes, digitalis toxicity • When any premature beat occurs more than six times per minute it is termed “frequent” Reentry Dysrhythmias • The reactivation of myocardial tissue for a second or subsequent time by the same impulse • Short circuit of electrical conduction system • Develops when course of electrical impulse is delayed or blocked Reentry Dysrhythmias • Due to this delay, electrical impulse allowed to travel in only one direction • The impulse moves in cycle throughout heart tissue • A series of fast depolarizations ensues Reentry Dysrhythmias Reentry Dysrhythmias • Causes of reentry – Due to conduction delays or blocks include hyperkalemia, myocardial ischemia, and certain antidysrhythmic medications • Specific rhythms include – Atrial flutter, atrial fibrillation, premature atrial complexes, and paroxysmal supraventricular tachycardia Atrial Flutter Rhythm • Presence of regular atrial activity with a picket fence, or sawtooth pattern • Single irritable site in atria initiates many electrical impulses at a rapid rate • Normal P wave not produced • Electrical impulses conducted throughout atria at fast rate Atrial Flutter Rhythm • Rather than the presence of normally appearing P waves, flutter (or sawtooth) waves, also known as F waves, are patterned • AV node becomes “gate keeper” to ventricles – Based on number of impulses AV node accepts, ventricular response is established Atrial Flutter Rhythm • Conduction ratio 2:1 – Two atrial contractions for each ventricular contraction • Conduction ratio 4:1 – Four atrial contractions for each ventricular contraction – An atrial rate of 300 bpm will parallel a ventricular rate of 75 bpm Atrial Flutter Rhythm • Atrial flutter with a slow ventricular response – Ventricular rate of less than 60 bpm • Atrial flutter with a rapid ventricular response – Ventricular rate of 100-150 bpm Atrial Flutter Atrial Flutter