* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Increased Levels of Endothelin-1 in Plasma of Sickle Cell Anemia
Survey
Document related concepts
Transcript
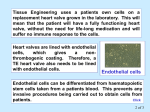
From www.bloodjournal.org by guest on June 17, 2017. For personal use only. 2594 CORRESPONDENCE cell disorder (ie, b-talassemia). The presented clinical cases are severe forms. In one case b-thalassemia could account for the increased clinical feature; in the other case no other red blood cell abnormality was demonstrated, but the coinheritance of thrombocytopenia in a consanguineous tree suggested the presence of two hematopoietic defects. CDA-II diagnosis was confirmed by bone marrow observation, electron microscopy, and laboratory data. From the biochemical point of view the disease appears very homogeneous. All the subjects showed the characteristic pattern of SDS-PAGE and the presence of reticulum endotelial proteins exposed on the surface. These two new families demonstrated for the first time that in these severe cases, although in the presence of an identical biochemical pattern, the disease is caused by a different gene and, thus, that genetic heterogeneity is present. Moreover, the biochemical defect most likely could present into a different step of the same pathway. A complementation assay could confirm this data. ACKNOWLEDGMENT We thank the families who collaborated in this work. This work is supported in part by Ministero Italiano della Sanita’ (to P.G.) and by Telethon (to A.I.) project E-645. Achille Iolascon Domenico De Mattia Dipartimento di Biomedicina dell’Età Evolutiva Università di Bari Bari, Italy Silverio Perrotta Dipartimento di Pediatria II Università Napoli Napoli, Italy Massimo Carella Paolo Gasparini Servizio di Genetica Medica IRCCS-CSS San Giovanni Rotondo (Fg), Italy Giorgio Lambertenghi Deliliers Istituto di Scienze Mediche Università di Milano Milano, Italy REFERENCES 1. Iolascon A, D’Agostaro G, Perrotta S, Izzo P, Tavano R, Miraglia del Giudice E: Congenital dyserythropoietic anemia type II: Molecular basis and clinical aspects. Haematologica 81:543, 1996 2. Wong KY, Hug G, Lampkin BC: Congenital dyserythropoietic anemia type II. Ultrastructural and radioautographic studies of blood and bone marrow. Blood 39:23, 1972 3. Alloisio N, Texier P, Denoroy L, Berger C, Miraglia del Giudice E, Perrotta S, Iolascon A, Gilsanz F, Berger G, Guichard J, Massé JM, Debili N, Breton-Gorlus J, Delaunay J: The cisternae decorating the red blood cell membrane in congenital dyserythropoietic anemia (type II) originate from the endoplasmic reticulum. Blood 87:4433, 1996 4. Iolascon A, Miraglia del Giudice E, Perrotta S, Granatiero M, Zelante L, Gasparini P: Exclusion of three candidate genes as determinants of congenital dyserithropoietic anemia type II (CDA II). Blood 90:4197, 1997 5. Gasparini P, Miraglia del Giudice E, Delaunay J, Totaro A, Granatiero M, Melchionda S, Zelante L, Iolascon A: Localization of the congenital dyserythropoietic anemia II locus to chromosome 20q11.2 by genomewide search. Am J Hum Genet 61:1112, 1997 6. Fukuda MN, Dell A, Scartezzini P: Primary defect congenital dyserythropoietic anemia type II: Failure in glycosylation of erythrocyte lactosaminoglycan proteins caused by lowered N acetylglucosaminyltransferase II. J Biol Chem 262:7195, 1987 7. Fukuda MN, Masri KA, Dell A, Luzzatto L, Moremen KW: Incomplete synthesis of N-glycans in congenital dyserythropoietic anemia type II (HEMPAS) caused by a gene defect encoding a mannosidase II. Proc Natl Acad Sci USA 87:7443, 1990 Increased Levels of Endothelin-1 in Plasma of Sickle Cell Anemia Patients To the Editor: Interactions between circulating blood cells and the vascular endothelium are tightly regulated to maintain the integrity of a functional circulatory system. Endothelial cells, which are bipolar, provide the vascular system with a nonthrombogenic surface on the lumenal side and perform a number of specialized metabolic and transport functions while in contact with the subendothelial matrix on the basal side.1 Injury to the vascular endothelium can expose the thrombogenic subendothelium and upset the delicate balance between blood flow and hemostasis. In sickle cell (SS) disease, injury to the vascular endothelium has been shown to result from increased adherence of SS red blood cells (RBCs) to endothelial cells and by vaso-occlusion of abnormally shaped SS RBCs.2,3 Vaso-occlusion by SS RBCs can produce prolonged hypoxia to local areas of the microvasculature resulting in endothelial cell damage.4 In addition, vaso-occlusion can contribute to the adherence of activated polymorphonuclear neutrophils, which can further damage endothelial cells by release of reactive oxygen metabolites.5 One endothelial-cell–derived component extremely sensitive to cell injury is the vasoconstrictor peptide, endothelin-1 (ET-1), which has been found to be increased in the plasma of patients with diabetes,6 uremia,7 myocardial infarction,8 cardiogenic shock,9 and in patients after hemodialysis.10 Damage to endothelial cells in SS disease may be another system in which plasma ET-1 is increased. If this were the case, the local vasoconstriction produced by ET-1 could decrease the diameter of some blood vessels and cause slower microvasculature transit times hypothesized to be necessary for cell sickling in vivo.11 If ET-1 were elevated in SS disease, it would not only be a marker for endothelial cell damage but could also be a factor in exacerbating a vaso-occlusive event. We measured the plasma levels of immunoreactive ET-1 in patients with SS disease in both steady state and crisis, and in normal age- and race-matched controls (AA) using an enzyme-linked immunosorbent assay (ELISA) method (Amersham Pharmacia Biotech, Arlington Heights, IL). Thirty-seven homozygous SS patients, (13 in crisis and 24 in steady state) from the Bronx Comprehensive Sickle Cell Center and 10 hematologically normal (AA) controls participated in the study. Individuals with hypertension or renal disease were excluded from the study. Plasma from 1 mL of heparinized blood was acidified with 0.25 mL 1 N HCl and loaded onto Sep-Pak C18 columns (Waters Associates, Milford, MA). ET-1 was eluted from the columns with 2 mL 80% methanol, 0.1% trifluoroacetic acid; the eluant lyophilized; and the pellet reconstituted in 0.25 mL assay buffer. The median ET-1 plasma level for SS patients in steady state was 18.79 pg/mL (n 5 24), which From www.bloodjournal.org by guest on June 17, 2017. For personal use only. CORRESPONDENCE was significantly higher than the median ET-1 plasma level of 0.58 pg/mL (n 5 10) for AA control subjects (P , .0001). Because the distribution of data points was not symmetrical, we used a nonparametric analysis, the Kruskal-Wallis One-Way Analysis of Variance on Ranks. There was no significant difference in median plasma ET-1 levels in SS patients in steady state (18.79 pg/mL) and those in crisis (26.16 pg/mL, n 5 13) (Fig 1). Asterisks indicate that the median plasma ET-1 levels for SS steady state and crisis were significantly different than the AA control median plasma ET-1 level at P , .0001. Our data indicate that ET-1 is elevated in SS disease; however, the mechanism by which this occurs has not been determined. Direct evidence for damage to the endothelium in SS disease comes from studies by Sowemino-Coker et al,12 who measured circulating endothelial cells in plasma from SS patients and found increased circulating endothelial cells during crisis. An alternative mechanism to account for increased plasma levels of ET-1 in SS disease is the upregulation of specific endothelial cell genes by circulating plasma factors and/or hypoxic conditions.13,14 In a recent report, Phelan et al15 found that SS RBCs that have previously undergone sickling induce a fourfold to eightfold increase in the transcription of the ET-1 gene as well as a fourfold to sixfold increase in ET-1 peptide production. The induction by sickled SS RBCs is specific for ET-1 and unsickled SS RBCs had no effect. Now that animal models for SS disease have been developed,16,17 it should be possible to determine which mechanism is responsible for increased plasma ET-1. Specific inhibitors of endothelin converting enzyme (ECE) that prevent the conversion of proET-1 to ET-1 are available18; increased synthesis of ET-1 would be blocked by these ECE inhibitors. The physiological significance of increased ET-1 in SS disease is also an open question. So many factors contribute to the pathophysiology of SS disease (eg, tissue hypoxia, vaso-occlusion, increased blood flow) that it is difficult to assess the contribution of one specific factor. A mouse model for SS disease where one of the autocrine functions of ET-1, such as endothelial cell proliferation, can be assessed will be an invaluable system in which to study the role of ET-1 in SS disease. Fig 1. Plasma ET-1 levels in SS patients in steady state and crisis (asterisks) were significantly increased compared to control AA subjects. There was no significant difference in plasma ET-1 levels between SS patients in steady state and crisis. 2595 ACKNOWLEDGMENT This research was supported by National Institutes of Health Sickle Cell Center Grant No. HL-38655. We thank Sylvia Musto for excellent technical assistance, Gwendolyn Swinson, RN, for procurement of patient blood samples, Dr Robert Schwartz for statistical analysis of the data, and Dr Ronald Nagel for helpful discussions. A preliminary report of this work was published in Blood 78:202a, 1991 (abstr, suppl 1). Anne C. Rybicki Lennette J. Benjamin Division of Hematology Department of Medicine Montefiore Medical Center Bronx, NY REFERENCES 1. Fajardo LF: The complexity of endothelial cells. Am J Clin Pathol 92:241, 1989 2. Hebbel RP, Yamada O, Moldow CF, Jacob HS, White JG, Eaton JW: Abnormal adherence of sickle erythrocytes to cultured vascular endothelium. J Clin Invest 65:154, 1980 3. Kaul DK, Fabry ME, Nagel RL: Vaso-occlusion by sickle cells: Evidence for selective trapping of dense red cells. Blood 68:1162, 1986 4. Hebbel RP, Boogaerts MAB, Eaton JW, Steinberg MH: Erythrocyte adherence to endothelium in sickle cell anemia: Possible determinant of disease severity. N Engl J Med 302:992, 1980 5. Warren JS, Ward PA: Oxidant injury to the vascular endothelium. Am J Med Sci 292:97, 1986 6. Takahashi K, Ghatei MA, Lam HC, O’Halloran DJ, Bloom SR: Elevated plasma endothelin in patients with diabetes mellitus. Diabetologia 33:306, 1990 7. Koyama H, Tabata T, Nishzawa Y, Inoue T, Morii H, Yamaji T: Plasma endothelin levels in patients with uraemia. Lancet 1:991, 1989 8. Salminen K, Tikkanen I, Saijonmaa O, Nieminen M, Fyhrquist F, Frick MH: Modulation of coronary tone in acute myocardial infarction by endothelin. Lancet 2:747, 1989 9. Cernacek P, Stewart DJ: Immunoreactive endothelin in human plasma: Marked elevation in patients in cardiogenic shock. Biochem Biophys Res Commun 161:562, 1989 10. Yoshizumi M, Kurihara H, Sugiyama T, Takaku F, Yanagisawa M, Masaki T, Yazaki Y: Hemodynamic shear stress stimulates endothelin production by cultured endothelial cells. Biochem Biophys Res Commun 161:859, 1989 11. Hofrichter J, Ross PD, Eaton WD: Kinetics and mechanism of deoxyhemoglobin S gelation: A new approach to understanding sickle cell disease. Proc Natl Acad Sci USA 71:4864, 1974 12. Sowemino-Coker SO, Meiselman HJ, Francis RB: Increased circulating endothelial cells in sickle cell crisis. Am J Hematol 31:263, 1989 13. Moon DG, Horgan MA, Anderson TT, Krystek SR, Fenton JW, Malik AB: Endothelin-like pulmonary vasoconstrictor peptide release by alpha-thrombin. Proc Natl Acad Sci USA 86:9529, 1989 14. Kourembanas S, Marsden LP, McQuillan LP, Faller DV: Hypoxia induces endothelin gene expression and secretion in cultured human endothelium. J Clin Invest 88:1054, 1991 15. Phelan M, Perrine SP, Brauer M, Faller DV: Sickle erythrocytes, after sickling, regulate the expression of the endothelin-1 gene and protein in human endothelial cells in culture. J Clin Invest 96:1145, 1995 16. Rubin EM, Witkowska HE, Spangler E, Curtin P, Mohandas N, Lubin BH: Hypoxia-induced in vivo sickling of transgenic mouse red cells. J Clin Invest 87:639, 1991 From www.bloodjournal.org by guest on June 17, 2017. For personal use only. 2596 17. Fabry ME, Sengupta A, Suzuka SM, Costantini F, Rubin EM, Hofrichter J, Christoph G, Mancie E, Culberson D, Factor SM, Nagel RL: A second generation of transgenic mouse model expressing HbS and HbS-Antilles results in increased phenotypic severity. Blood 86:2419, 1995 CORRESPONDENCE 18. Ikegawa R, Matsumura Y, Tsukahara Y, Takaoka M, Morimoto S: Phosphoramidon, a metalloproteinase inhibitor, suppresses the secretion of endothelin-1 from cultured endothelial cells by inhibiting a big endothelin-1 converting enzyme. Biochem Biophys Res Commun 171:669, 1990 Activating Mutations of the Transmembrane Domain of MPL In Vitro and In Vivo: Incorrect Sequence of MPL-K, an Alternative Spliced Form of MPL To the Editor: Recently, many gene alterations have been identified as causes of leukemia, most of which are gross rearrangements of transcription factors, receptors, and kinases derived from chromosomal translocations. In addition, mutations of tyrosine kinase receptors such as c-kit1 and FLT-32 have been reported in mastocytosis and myeloid leukemia, respectively. In particular, it is noticeable that duplication of the juxtamembrane region of FLT-3 is observed in 20% of patient leukemic cells. However, no cytokine receptors (type I cytokine receptor family) have been reported to be involved in human leukemia except that truncation of the C-terminal domain of the granulocyte colony-stimulating factor (G-CSF) receptor caused by various point mutations is implicated in a fraction of leukemic patients. Most of these leukemias are secondary acute myeloid leukemias (AMLs) developed from Kostmann syndrome, and the significance of the mutations in leukemogenesis is still controversial.3,4 MPL, thrombopoietin (TPO) receptor, is the only hemopoietin receptor (type I cytokine receptor family) identified as an oncogene.5,6 Thus, MPL was originally identified as a truncated form v-mpl that is an oncogene of a murine retrovirus MPLV, which causes myeloproliferative disorders in mice, and was later recognized as a receptor for TPO. Using a combined strategy including polymerase chain reaction (PCR)driven random mutagenesis and retrovirus-mediated high-efficiency gene transfer, we have recently identified a constitutive active form of MPL.7 This point mutation causes a single amino acid substitution from Ser498 to Asn498 in its transmembrane domain. Expression of the mutant MPL in a mouse interleukin-3 (IL-3)–dependent pro-B cell line Ba/F3 resulted in constitutive activation of both the Ras-Raf-MAPK and the Jak-STAT pathways and IL-3–independent growth. Moreover, when the Ba/F3 transfectants expressing the mutant MPL were injected into syngeneic mice after sublethal irradiation, they developed severe infiltration of the Ba/F3 transfectants in liver and spleen, suggesting that the mutant form of MPL is highly oncogenic in vivo. We were interested in whether similar mutations can be found in patients’ leukemic cells, and examined the sequence of the transmembrane portion of MPL in 43 patients, including 2 patients with essential thrombocytosis (ET), 6 with AML-M1, 6 with AML-M2, 1 with AML-M3, 3 with AML-M4, 2 with AML-M5, 9 with AML-M6, 12 with AML-M7 (megakaryoblastic leukemia), and 2 with myelodysplastic syndromes (MDS). To sequence the corresponding part in the patients’ sample and to avoid the contamination of the plasmid harboring the mutant MPL, a DNA fragment spanning the transmembrane portion of MPL (exon 9) and a part of intron 10 of the human MPL gene8 was amplified from high-molecular-weight DNA by PCR using a 58 transmembrane primer (ATCTCCTTGGTGACC) and a primer in the 10th intron (AGATCTGGGGTCACACAGAG) (Fig 1). To avoid mutations during the recovery procedure as much as possible, we used Pfu polymerase for the reaction. PCR fragments were subcloned into the TA vector, and at least six subclones were sequenced for each patient. However, no mutations were found in the transmembrane portion of MPL. Our results indicate that the mutation in the transmembrane region of MPL is not a frequent cause of leukemogenesis. There are two major transcripts for MPL, a full-length MPL-P and an alternative splicing form MPL-K.6 MPL-K is supposed to be translated from an alternative spliced mRNA harboring intron 10 after exon 9 encoding the transmembrane region (Fig 1). The function of MPL-K product was not known.6 During the course of our screening for MPL mutations in leukemic patients, we happened to find a sequence error in the sequence of intron 10 that had been published as a part of the MPL-K transcript (Fig 1). Thus, the sequence CG (1616-1617) was GGCC (1616-1619) in all patients tested as well as in a normal control, which will result in frame-shift and earlier termination in the MPL-K product (Fig 2). The predicted length of the intracellular domain of MPL-K should be 36 instead of 66 amino acids. To confirm this, it is required to molecularly clone cDNA for MPL-K and confirm the sequence of the corresponding part. Toshio Kitamura Department of Hemopoietic Factors Institute of Medical Science University of Tokyo Tokyo, Japan Mayumi Onishi Third Department of Internal Medicine University of Tokyo Tokyo, Japan Takashi Yahata Department of Immunology Tokai University School of Medicine Isehara, Japan Yuzuru Kanakura Department of Hematology and Oncology Osaka University Suita, Japan Shigetaka Asano Department of Internal Medicine Institute of Medical Science University of Tokyo Tokyo, Japan Fig 1. PCR primers to amplify the transmembrane region of MPL from genomic DNA. TM (shadowed box), transmembrane region; arrows, PCR primers. From www.bloodjournal.org by guest on June 17, 2017. For personal use only. 1998 92: 2594-2596 Increased Levels of Endothelin-1 in Plasma of Sickle Cell Anemia Patients Anne C. Rybicki and Lennette J. Benjamin Updated information and services can be found at: http://www.bloodjournal.org/content/92/7/2594.full.html Articles on similar topics can be found in the following Blood collections Information about reproducing this article in parts or in its entirety may be found online at: http://www.bloodjournal.org/site/misc/rights.xhtml#repub_requests Information about ordering reprints may be found online at: http://www.bloodjournal.org/site/misc/rights.xhtml#reprints Information about subscriptions and ASH membership may be found online at: http://www.bloodjournal.org/site/subscriptions/index.xhtml Blood (print ISSN 0006-4971, online ISSN 1528-0020), is published weekly by the American Society of Hematology, 2021 L St, NW, Suite 900, Washington DC 20036. Copyright 2011 by The American Society of Hematology; all rights reserved.