* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Pulmonary and Systemic Circuits Path of Blood Flow Heart Anatomy
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Artificial heart valve wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Myocardial infarction wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
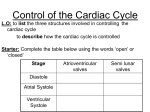
3/22/2013 Pulmonary and Systemic Circuits • Heart: double pumps – pulmonary circuit • short, low-pressure circulation – systemic circuit • long, high-friction circulation • Trace the flow of blood to & away from the heart Path of Blood Flow P:4–6X Heart Anatomy • Atria: Receiving Chambers – R. atrium • Vena cava & Coronary sinus – L atrium • Pulmonary veins • Ventricles: Discharging Chambers – Papillary muscles – Chordae tendinae – R. ventricle • Pulmonary trunk – L. ventricle • aorta Heart valves • Open and close in response to pressure changes • atrioventricular (AV) valves: Tricuspid & mitral – Open: P.atrium > P.ventricle – Close: ___________ • semilunar (SL) valves: aortic & pulmonary – Open: P.ventricle > P.great vessels – Close: ___________ 1 3/22/2013 Cardiac Muscle Fibers Anatomy of Cardiac Muscle • striated, short, branched, 1 central nucleus • T tubules: wide, less numerous • large mitochondria – 25–35% of cell volume – Aerobic respiration Anatomy of Cardiac Muscle • Intercalated discs – Desmosomes: anchoring cells – Gap junctions: electrically couple adjacent cells • Allows heart to be functional syncytium (single coordinated unit) © 2013 Pearson Education, Inc. Similarities between skeletal and cardiac muscles Skeletal muscle Cardiac muscle 1) Depolarization (-90mV => +30mV) •Opening VG fast Na+ channels 2) Depolarization waves travel down T-tubules •Ca2+ release 3) Excitation contraction coupling Differences between skeletal and cardiac muscles Source of stimulation Contraction Contraction duration absolute refractory period Skeletal muscle Cardiac muscle Somatic nervous system Motor unit contraction 15-100ms Auto-rhythmic Brief: 1-2ms All cardiomyocytes contract as unit, or none do 200ms •blood ejection from heart Long: 250ms •Prevents tetanic contractions 2 3/22/2013 Differences between skeletal and cardiac muscles Skeletal muscle Cardiac muscle Ca2+ source Sarcoplasmic reticulum Extracellular Ca2+ - 20% •Depolarization: slow Ca2+ channels in sarcolemma SR – 80% Action potential Depolarization Brief: 1-2ms Long: 200ms •Due to plateau phase •Fast VG Na+ channels •Slow Ca2+ channels •Inactivation Ca2+ channels •Opening VG K+ channels Repolarization Fast VG Na+ channels Opening VG K+ channels Cardiac Contractile Cells: Excitation-Contraction Coupling • Excitation – Contraction – T-tubules • ↑Ca2+ : PLATEAU PHASE • Ca2+-induced Ca2+ release • Relaxation Action Potential of contractile muscle cells Setting the Basic Rhythm • Intrinsic cardiac conduction system • Network of autorhythmic cells • gap junctions – Allow coordinated heartbeat -- synchrony – SR: Ca2+ – Plasma membrane • 3Na+/1Ca2+-antiport • 3Na+/2K+-ATPase – Digitalis (Digoxin) © 2013 Pearson Education, Inc. APs Initiation by Pacemaker Cells APs Initiation by Pacemaker Cells • unstable RMPs (pacemaker potentials or prepotentials) – gradual depolarization • Open slow Na+ channels • Close K+ channels • At threshold: Depolarization – Open Ca2+ channels • Repolarization – Close Ca2+ channels – Open K+ channels © 2013 Pearson Education, Inc. 3 3/22/2013 Conduction System Extrinsic Innervation of the Heart • cardiac centers in medulla oblongata – Cardioacceleratory center • Sympathetic – Cardioinhibitory center • Parasympathetic © 2013 Pearson Education, Inc. Heart Sounds • lub-dup – LUB: louder, longer • P.ventricle > P.atria • Ventricular systole begins – DUP: Short, sharp • Ventricular diastole begins © 2013 Pearson Education, Inc. Cardiac Cycle • Mechanical Events occurring during one complete heartbeat – 2 phases • Systole = contractile phase of cardiac cycle • Diastole = relaxation phase of cardiac cycle – Series of pressure and blood volume changes during 1 heartbeat • Heart murmurs – incompetent or stenotic valves © 2013 Pearson Education, Inc. Ventricular filling Phase of Cardiac Cycle • AV valves – open; semilunar valves - closed – passively flows into ventricles -- 80% of blood • pressure low – Atrial systole -- 20% • End diastolic volume (EDV): volume of blood in ventricle at end of ventricular diastole © 2013 Pearson Education, Inc. Ventricular systole Phase of Cardiac Cycle • Ventricles contract (while Atria relax) – ventricular pressure: AV valves – closed; semilunar valves - open – Isovolumetric contraction phase: Volume – ejection phase: volume • End systolic volume (ESV): volume of blood remaining in each ventricle after systole © 2013 Pearson Education, Inc. 4 3/22/2013 Isovolumetric relaxation Phase of Cardiac Cycle Wigger’s Diagram: Summary of events during cardiac cycle Left heart QRS P EKG • Ventricles relax T 1st Heart sounds – Isovolumetric: volume – AV valves: closed – Semilunar valves: closed P 2nd Dicrotic notch 120 80 Aorta Pressure (mm Hg) Left ventricle 40 • atria relaxed Atrial systole Left atrium 0 120 EDV Ventricular volume (ml) – Atrial filling SV 50 ESV Atrioventricular valves Aortic and pulmonary valves Phase Closed Open 2b 2a 1 Open Closed 3 1 Ventricular Isovolumetric contraction phase ejection phase 2a 2b Ventricular filling (mid-to-late diastole) Ventricular systole (atria in diastole) Atrial contraction Ventricular filling © 2013 Pearson Education, Inc. Open Closed 1 Isovolumetric relaxation 3 Ventricular filling Early diastole Pressure EKG vs. Heart Sounds Ventricular ejection Isovolumetric contraction Ventricular volume Isovolumetric relaxation Cardiac Output (CO) • Cardiac output varies to meet metabolic demands – CO = HR × SV – At rest • CO = HR (75 beats/min) SV (70 mL/beat) – CO = 5.25 L/min • HR – (+) - chronotropic factors: HR – (-) - chronotropic factors: HR © 2013 Pearson Education, Inc. 5 3/22/2013 Stroke Volume • SV = EDV – ESV = • factors affect SV Frank Starling’s Law of the Heart •The heart pumps all the blood that returns to it •MAP = CO x TPR Residual – Preload = degree of stretch (tension) of cardiac muscle cells before they contract (Frank-Starling law of heart) Stroke volume •End-diastolic volume (EDV) contraction EDV SV • Venous return => EDV (preload) • Slow HR => ventricular filling (filling time) => EDV – Afterload = pressure ventricles must overcome to eject blood (resistance) • Loss of arterial elasticity => Afterload • Afterload => SV & ESV Larger EDV Stronger contraction Larger SV – Contractility Contractility Atrial (Bainbridge) reflex • Contractility: the amount of force produced at a given preload • sympathetic reflex initiated – by venous return => atrial filling • Stretch of atrial walls stimulates SA node HR – ONLY sympathetic – NO parasympathetic influence • Increased by Positive inotropic agents – stimulates atrial stretch receptors, activating sympathetic reflexes – Thyroxine, glucagon, epinephrine, digitalis, high extracellular Ca2+ • Decreased by negative inotropic agents – Acidosis, increased extracellular K+, calcium channel blockers © 2013 Pearson Education, Inc. Figure 18.22 Factors involved in determining cardiac output. Exercise (by sympathetic activity, skeletal muscle and respiratory pumps; see Chapter 19) Heart rate (allows more time for ventricular filling) Exercise, fright, anxiety epinephrine, thyroxine, excess Ca2+ Principles of Blood Pressure and Flow • Blood Flow= pressure/ resistance – pressure gradient: driving force for blood flow Venous return Sympathetic activity Contractility EDV (preload) Parasympathetic activity • Large gradient: from aorta to capillaries – At aorta: 2.5 cm diameter and 100 mm Hg pressure – At capillaries: 8 µm diameter and 25 mm Hg pressure ESV – Resistance opposes flow Initial stimulus Physiological response Result Stroke volume Heart rate Cardiac output © 2013 Pearson Education, Inc. 6 3/22/2013 Blood pressure and flow Changes in • vessel diameter • blood pressure • velocity of blood flow • Arterial pressure is variable – Example: 120/90 • systolic pressure • diastolic pressure – Pulse pressure (difference between systolic and diastolic) • Example: 120 – 90 = 30 mm Hg • Mean arterial pressure (MAP) Mean arterial pressure • the average arterial pressure during a single cardiac cycle – perfusion pressure = driving force that pushes blood through the systemic circuit • MAP = 1/3(PSyst) + 2/3(PDiast) • MAP = CO x TPR – Total peripheral resistance: the force that opposes the flow of blood Peripheral resistance • Resistance opposes flow (R=8nl/πr4) • Vasomotor – vessel radius: principal method of blood flow control – blood in direct contact w/ vessel wall Congestive heart failure (CHF) – Progressive condition; CO is so low that blood circulation inadequate to meet tissue needs – Pulmonary congestion • LH failure blood backs up in lungs – Peripheral congestion • RH failure blood pools in body organs edema – Failure of either side ultimately weakens other – Treat by removing fluid, reducing afterload, increasing contractility 7