* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Print - Circulation
Coronary artery disease wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Marfan syndrome wikipedia , lookup
Turner syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Artificial heart valve wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
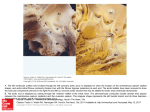
in Subendocardial Blood Flow Children with Congenital Aortic Stenosis L. JEROME KROVETZ, M.D., PH.D., AND J. PARKER KURLINSKI, M.D. Downloaded from http://circ.ahajournals.org/ by guest on June 15, 2017 SUMMARY Subendocardial blood flow may be estimated from the ratio of flow to the subendocardium to myocardla oxygen consumption. The first may be estimated from the diastolic pressure time index (area between aortic and left ventricular (LV) preure during diastole) and the latter by the tension time index (integral of LV pressure during systolic ejection). Subendocardial flow index (SEFI) averaged 1.27 (0.96-1.78) in 13 children with normal aortic valves. SEFI averaged 0.88 (0.43-1.65) in asymptomatic children with congenital aortic stenosis and was never greater than 0.9 in symptomatic children. Aortic valve area and sYstolic pressure difference did not correlate well with symptoms SEFI and aortic valve area increased in 26 of 28 patients after surgery. However, 23 of 28 had varying degrees of aortic regurgitatin following valvotomy. Since calculation of SEFI is not affected by aortic regurgitation, it would appear to be a more useful measure of surgical success than aortic valve area. POOR CORRELATION between symptoms and pressure difference across the left ventricular outflow tract obstruction in congenital aortic stenosis has been noted previously.'-' We had a vivid example of this in a six-year-old boy with congenital aortic stenosis who had episodes of apparent syncopal attacks. At cardiac catheterization, peak systolic pressure difference averaged only 54 mm Hg and the calculated aortic valve area was 0.8 cm2. Both suggested only moderate obstruction in a child of his size. Following another and better documented syncopal episode a few weeks after the catheterization, valvotomy was carried out with subsequent relief of symptoms. The presence of dizziness, syncope, or congestive heart failure correlates poorly with peak systolic pressure difference.2 In one study of 32 patients with syncope,5 18 had peak systolic pressure differences greater than 100 mm Hg, but five had less than 50 mm Hg across the outflow tract. Little relationship between symptoms and aortic valve area or aortic valve index was noted in another study.' Poor correlation has been noted between presence of symptoms, electrocardiographic and roentgenologic findings and the systolic pressure difference6 or aortic valve index.1 4 In a study of supravalvar aortic stenosis in adults,7 angina, the most common symptom, was often disproportionately severe to the degree of obstruction as measured by the pressure difference. Since the subendocardial flow index was shown to have a good correlation with the severity of obstruction,8' we decided to compare this index with peak systolic pressure difference and calculated valve area in children with congenital aortic stenosis. The clinical histories were examined by each author without knowledge of catheterization findings or subsequent clinical course. Patients were considered to be asymptomatic if they had been free of symptoms for at least one year prior to catheterization. Patients were classified as mildly symptomatic if they had a history of exercise intolerance, fatigue, excessive sweating, feeding difficulties, or dizziness without true syncope. Patients who had syncopal attacks, dyspnea at rest, angina or congestive heart failure were considered to be severely symptomatic. No patient in this study had a history of infective endocarditis or one suggesting coronary artery disease. A total of 45 children (36 male, nine female) with adequate clinical, catheterization and angiographic data were located. The average age at catheterization was 9.5 years, with a range of one month to 16 years. Thirty-three of these children had valvar, seven discrete subvalvar, four supravalvar aortic and one combined valvar and subvalvar stenosis. Thirty-five patients underwent two or more catheterizations, including 28 who were catheterized before and after open-heart repair of their lesions. The other seven children were recatheterized either because of a change in their clinical status or as part of a study of the natural history of aortic stenosis. Two patients were catheterized three times each, twice prior to and once after successful surgical treatment of subvalvar aortic stenosis. All of the patients with more than one catheterization demonstrated a significant change in at least one of the indicators of severity considered in this investigation; hence, for the purpose of this study, each of the 82 catheterizations was considered as a separate data point. In addition, data from three patients apparently recovered from endocardial fibroelastosis, one patient with a ligated anomalous left coronary artery, four patients with small ventricular septal defects (pulmonary-to-systemic flow ratio of less than 2:1), one patient with mild aortic insufficiency, and four normal patients were analyzed. These 13 children are referred to as the control group. Aortic valve area was calculated from a modified Gorlin formula'0 as follows: Materials and Methods Data were examined for all patients under 16 years of age with congenital aortic stenosis catheterized at the Johns Hopkins Hospital between 1963 and 1973. Patients with cardiac lesions other than aortic insufficiency were excluded. From the Departments of Pediatrics and Biomedical Engineering, The Johns Hopkins University School of Medicine, The Johns Hopkins Hospital, Baltimore, Maryland. Supported in part by research grants from NHLI (HL-14207-03 and HL17996) and the General Clinical Research Centers Program of the Division of Research Sources (RR-52), NIH. Address for reprints: L. Jerome Krovetz, M.D., Division of Pediatric Cardiology, Department of Pediatrics, University of Virginia Hospital, Charlottesville, Virginia 22901. Received February 12, 1975; revision accepted July 9, 1976. Valve area = CO X 1000 co_______________ SEP X HR X 29.5 x v'- where CO = cardiac output in ml/min, SEP = systolic ejection period in seconds/beat, HR = heart rate in 961 962 CIRCULATION beats/min, and AP = the mean pressure difference between left ventricle and aorta during the systolic ejection period. Puyau et al.1' demonstrated that the valve area calculated using 29.5 as the constant in Gorlin's hydrodynamic formula was closer to the surgically measured orifice in children than the 44.5 usually used. Cardiac output was calculated by indicator dilution technique in 61 instances, by Fick method in five, average of Fick and dye in five, and was not available for 11 patients. Surface area was estimated from the nomogram of Sendroy and Cecchini'2 and aortic valve index calculated. Calculation of the Subendocardial Flow Index Downloaded from http://circ.ahajournals.org/ by guest on June 15, 2017 In 35 catheterizations, pressure recordings of catheter pull-backs from the left ventricle across the site of the obstruction to the root of aorta were recorded on analog magnetic tape. The simultaneously recorded ECG signal was sent to an R wave detector whose output was connected to the priority interrupt module of a Varian Model 620/L minicomputer to separate each pulse beat for subsequent analysis. Analog-to-digital conversion was performed at a rate of 200 samples per minute and approximately 15 waves digitized and recorded on LINC tape. Consecutive left ventricular waveforms were then displayed on a Tektronix 4010 display unit. Pressure waveforms during which PVCs occurred and the next two successive waves were omitted. The average R to R interval was computed for at least 5 pressure waveforms, each wave linearly interpolated or extrapolated to this wave length, and the waveforms averaged. This approach reduces the nonperiodic artifact by the square root of the number of waves averaged. The diastolic pressure time index (DPTI) was measured as the area between aortic pressure and left ventricular pressure during diastole (fig. 1). Tension time index (TTI) was computed as the integral of the left ventricular pressure during the systolic ejection period. Subendocardial flow index was FIGURE 1. Redrawn graphic display used for calculation of the subendocardialflow index. The tension time index (TTI) is the area under the left ventricular curve during the time when left ventricular pressure is greater than aortic pressure. Diastolic pressure time index (DPTI) is the area under the aortic curve during the period when aortic pressure is greater than left ventricular pressure. The subendocardialflow index is the ratio of the DPTI (the pressure and time when subendocardialflow occurs) to TTI which is proportional to myocardial oxygen consumption. VOL 54, No 6, DECEMBER 1976 obtained by dividing DPTI by TTI. The averaged waveforms were then displayed on a graphics display terminal along with the pertinent calculations and printed out on a Tektronix 4610 hardcopy unit for the permanent record (fig. 1). The remaining 47 catheterizations were calculated in a similar manner utilizing the original oscillographic tracings recorded at 200 mm/sec. Nine simultaneous left ventricular and root of aorta pressure tracings were available, while 38 catheterizations involved sequential left ventricular and root of aorta pressure tracings. For the latter cases, aortic and left ventricular pressure tracings with identical R to R intervals during the same stage of respiration were selected. The tracings were superimposed and DPTI and TTI calculated by planimetry of the areas described above. The values for SEFI were obtained by dividing DPTI by TTI. In addition, a coronary artery oxygen supply/demand ratio was calculated for 94 of the 95 catheterizations by multiplying SEFI by the arterial oxygen content."3 Aortic root angiograms were performed during each catheterization; 70 of these were available for review to assess the presence and severity of aortic insufficiency (Al). Where the cineangiograms were not available, the original observer's description was relied upon to assess the severity of AI. Al was graded as 1 + (trivial) if present on only one cardiac cycle, 2+ (mild) if present on two or more cardiac cycles, 3+ (moderate) with opacification of entire LV cavity, and 4+ (4evere) with opacification of entire LV cavity and elevation of LV end-diastolic pressure. For analyses involving pressure difference, aortic valve area, or aortic valve index, the five patients with 3+ or 4+ AI were eliminated. Subendocardial flow was compared for varying degrees of aortic regurgitation and no significant differences were found by Student's t-tests. Therefore, subendocardial flow index values were included in later analyses without respect to the presence of aortic insufficiency. No significant difference was found between the mean aortic valve area and mean aortic valve index, probably due to the fact that the mean surface area for this group of patients was close to 1 M2. Correlation coefficients for AP versus valve area and AP versus aortic valve index were -.51 and -.54, respectively. Correlation coefficients for subendocardial flow index versus valve area and versus aortic valve index were 0.70 and 0.65, respectively. Results Subendocardial flow index (SEFI) for the 13 patients in the control group averaged 1.27, with a range of 0.96 to 1.78. All of the children with congenital aortic stenosis (AS) having either mild or severe symptoms had SEFI below this range (fig. 2). SEFI was reduced even for asymptomatic AS patients, averaging 0.88 with a range of 0.43 to 1.65. Slightly less significant differences between asymptomatic and symptomatic patient groups were found for aortic valve area (fig. 3). Eleven of the 29 asymptomatic patients had valve areas less than 0.75 cm2, a value usually considered to indicate surgically important narrowing (fig. 3). A similar lack of differentiation between asymptomatic and symptomatic groups was found for the systolic pressure difference across the aortic valve (fig. 4). Six of the 29 symptomatic patients had pressure differences across their valves less than or equal to 50 mm Hg. BLOOD FLOW IN AS/Krovetz, Kurlinski Downloaded from http://circ.ahajournals.org/ by guest on June 15, 2017 Subendocardial flow index correlated better with aortic valve area (r = 0.70) than did the pressure difference across the left ventricular outflow tract obstruction (r = - 0.51). The values obtained for SEFI were compared to those modified by using the arterial oxygen content. The coefficient correlation was 0.968. In no instance was there a change in the estimation of the degree of severity when arterial oxygen content was taken into account. This would imply that variation of arterial oxygen content was not as important as the ratio of DPTI/TTI in these children even though the oxygen content ranged from 12.2 to 21.1 ml/dl. Table 1 shows that of 24 patients who had either mild or severe symptoms, seven had only an abnormal SEFI. In six other patients, both a low SEFI and a small aortic valve area were found. In 11 symptomatic patients, all the hemodynamic measurements were in agreement in indicating a high degree of stenosis. In no symptomatic patient was the pressure difference across the LV outflow tract the only positive finding. None of the symptomatic patients had SEFI > .90. However, there were nine asymptomatic patients who had a low SEFI and aortic valve area as well as a pressure difference of more than 75 mm Hg, so that the discrimination was not complete. Subendocardial flow index and aortic valve area increased in all except two of the patients following surgical repair (fig. 5). However, over 80% of these children had some degree of aortic regurgitation following valvotomy. Because estimation of aortic valve area depends upon forward flow through the valve, AI may invalidate this measurement. Calculation of SEFI is not affected by aortic regurgitation. Furthermore, because AI decreases DPTI in proportion to the decrease in diastolic pressure, it would appear to be a more useful measure of surgical success than aortic valve area. Left maximum spatial vector (LMSV) was calculated from the vectorcardiograms in 44 patients. A correlation 963 0 2.5- S S 2.0S IS.D. E -1.5' 4 0* 4 w . -i MEAN 4c a - > 1.0- .5. S IS.D. - 0 S.~~~~~ *- P<.OI- oF-PC.50-* - PC.005- m MILD NONE SEVERE FIGURE 3. Aortic valve areas grouped by symptoms for patients with left ventricular outflow obstruction, excluding those with moderate or severe A!. Eleven of the 29 symptomatic patients had aortic valve areas, > .75 cm2 and three were above 1.2 cm2. coefficient of 0.35 was found between LMSV and systolic pressure difference across the valve and only 0.10 between LMSV and SEFI. LMSV averaged 1.88 mv for the asymptomatic patients with aortic stenosis, 1.81 mv for patients with mild symptoms and 2.6 mv for those with severe symptoms. This latter value was elevated almost entirely by one 200- 1.8I.6- 150- 1.41.2- IS.D. E 2 I 1.0. MEAN n. o 4 I- .8 .6- I 0 D IS.0. 0 510 IS.D. MEAN I 501 .400 .2- -PCOO P0 M PC005 NONE MILD IS.D. -N.S. I d m SEVERE FIGURE 2. Subendocardial flow index grouped by symptoms for patients with left ventricular outflow obstruction. There was no difference between those with mild or severe symptoms. All of the symptomatic patients had DPTI/TTI < 0.9. NONE - 0 1 - N.S.P PCw05 I MILD 34 F SEVERE FIGURE 4. Peak systolic left ventricular to root of aorta pressure differences grouped by symptoms, excluding those with moderate or severe AL Six of the 29 symptomatic patients had a AP < 50 mm Hg, while six of the asymptomatic patients had AP > 100 mm Hg. 964 CIRCULATION VOL 54, No 6, DECEMBER 1976 TABLE 1. Correlation of Symptoms and Preoperative Catheterization Findings Severe stenosis indicated by: Low SEFI (<.90) Low SEFI & low AV area (<.75sqcm) Low SEFI & high LV-aortic pressure (>75 mm Hg) Low SEFI <.90 + low AV area + high LV-Ao pressure .8- Asymptomatic Symptomatic 1.6- 10 7 1.4- 2 6 .2- 1 0 1.0- , 9 11 a- a subject with a LMSV of 4.85 mv; there was no statistically significant difference among these three groups. There was a small but statistically insignificant decrease in LMSV in nine patients following surgery. . .6- MEAN IS. D. .4- .2- Downloaded from http://circ.ahajournals.org/ by guest on June 15, 2017 Discussion Despite the simplicity of its calculation, the area beneath the LV pressure curve during systole, termed the tension time index (TTI) by Sarnoff et al.,1 gives a reasonable approximation of myocardial oxygen consumption. Left ventricular subendocardial muscle (in contrast to subepicardial muscle) must receive most, if not all, of its flow during diastole due to the high intramyocardial compressive forces in the subendocardium that reduce systolic perfusion. Buckberg et al.,8 by constricting the supravalvar aorta in dogs, demonstrated a lowering of the subendocardial flow index. Homogeneous myocardial flow distribution was maintained over a wide range of subendocardial flow index values in the dogs, until values of .7 or below were achieved, and then relative underperfusion of the subendocardium was seen. During control periods, 80% of left coronary artery flow in dogs occurred in diastole and though the total flow rose as the supravalvar aorta was constricted, the increase in flow occurred predominantly during systole. The proportion of flow during diastole fell progressively with increasing aortic constriction and averaged 34% of total flow with severe constriction and the proportion of total flow perfusing the subendocardial muscle fell significantly. In their calculations of the subendocardial flow index9 in 18 control patients and in one patient each with valvar aortic stenosis and supravalvar aortic stenosis, they demonstrated that the relationship between oxygen needs (TTI) and the available subendocardial blood supply (DPTI) seem to be distributed in a similar manner. Both of their patients with left ventricular outflow tract obstruction had SEFI values significantly below .7. Increased coronary artery perfusion pressure may occur in SVAS'8 18 but does not increase subendocardial flow.9 Values for SEFI in our investigation are slightly higher than those calculated by Vincent et al.9 because our calculation of TTI excludes the periods of isometric ventricular contraction and relaxation. In our series, all 29 studies in symptomatic patients had SEFI values below .9 (fig. 2). Four patients with pressure differences across their valves greater than 50 mm Hg had SEFI values greater than .9 (.92, .96, .98, 1.06). Also, there were only two patients with valve areas less than .75 cm2 and subendocardial flow index values greater than .9 (.96, 1.03). Lewis et al."7 also analyzed the relationship between the T wave configuration of the - P<.001 - I~~~~~~~~~~~~~~~~~~~~ I PRE-OP POST-OP FIGURE 5. Effect of aortic valvotomy on subendocardial flow indexfor 23 patients with aortic stenosis. SEFI increased in all except two cases. electrocardiogram and demonstrated with supply/demand ratio. a strong correlation A modified index has been proposed which multiplies DPTI by oxygen content."' Comparison of this modified coronary artery oxygen delivery ratio to SEFI was done for 94 catheterizations in our present study. The correlation coefficient obtained was 0.968, suggesting that arterial oxygen content was not a major determinant in the degree of variation of myocardial oxygen supply/demand ratios. Data from two other studies in the literature were also compared for SEFI alone and SEFI multiplied by arterial oxygen content. For the 80 children of the study by Lewis et al.,'7 the correlation coefficient was 0.96, and for the 10 neonates described by Lakier et al.'8 it was 0.93. SEFI showed an excellent correlation with the presence of symptoms (fig. 2). No patient with either mild or severe symptoms had an SEFI > 0.90. Of particular interest in this regard are the findings in six patients who exhibited changes in symptomatology prior to recatheterization (table 2). In four instances SEFI worsened with the development of symptoms and in two instances spontaneous relief of symptoms was accompanied by an increase in SEFI. An unexpected finding was that mildly symptomatic patients did not differ significantly from severely symptomatic patients for any of the measures studied. This would imply that at least in the pediatric age range, our so-called mild symptoms are as meaningful as severe symptoms in the assessment of the disease. Poorer correlation of systolic pressure across the obstruction and symptoms was found in our study (fig. 4). The presence of severe symptoms showed a statistically significant difference (P < 0.05) while the mildly symptomatic patients did not differ from the asymptomatic group. Furthermore, six of the asymptomatic patients had pressure differences of over 100 mm Hg while six of the symptomatic patients had pressure differences of less than 50 mm Hg. In spite of a number of theoretical objections about the 965 BLOOD FLOW IN AS/Krovetz, Kurlinski TABLE 2. Selected Data of Six Patients with Congenital Aortic Stenosis and a Spontaneous Change in Symptoms Pt Age Sex Site of stenosis JD 5 F Valvar M Valvar M Valvar F Valvar M Valvar M Subvalvar JK MS LP RM MG 13 6 10 11 14 10 13 7 12 9 DPTI TTI NA - 0.78 70 16 24 -55 57 45 36 65 46 78 0.91 1.74 2.38 1.08 0.97 0.96 1.34 1.22 2.55 0.73 0.66 1.93 2.16 1.03 0.73 0.95 0.96 1.18 1.82 0.73 0.70 0.75 1.65 0.75 0.58 1.07 0.74 0.86 1.54 0.67 192 0.70 0.46 0.45 1+ 0 Exer. intol. 26 Angina 1+ 0 0 2+ 2+ 0 0 0 1+ 1+ Exer. intol. 0 0 Angina 0 Exer. intol. Angina 0 0 Exer. intol. Exces. sweating Downloaded from http://circ.ahajournals.org/ by guest on June 15, 2017 use of aortic valve area, statistically significant differences were seen between the asymptomatic and both the mildly and severely symptomatic groups (fig. 3). However, the presence of aortic regurgitation invalidates this measurement since the forward aortic valve flow is required for its estimation while the usual dye dilution or Fick method measures net flow. Subendocardial blood flow can be estimated easily from cardiac catheterization data and appears to be a sensitive index of ischemia that should be considered when surgical intervention is being entertained. It should be noted, however, that we are not certain of the exact numerical value below which surgical intervention is desirable. Further, DPTI tends to be decreased with increasing heart rates in the presence of severe stenosis'7 so that exact numerical values may be exceedingly hard to evaluate. As patients with AS age and begin to have associated coronary artery obstruction disease, attempts to estimate the supply/demand ratio of the LV myocardium may seriously overestimate potential supply. DPTI is a useful indicator of subendocardial blood flow only in the presence of maximally dilated and unobstructed coronary arteries. References 1. Cohen LS, Friedman WF, Braunwald E: Natural history of mild congenital aortic stenosis elucidated by serial hemodynamic studies. Am J Cardiol 30: 1, 1972 2. Eddleman EE Jr, Frommeyer WB Jr, Lyle DP, Bancroft WH Jr, Turner ME Jr: Critical analysis of clinical factors in estimating severity of aortic valve disease. Am J Cardiol 31: 687, 1973 Ao valve index (Cm2/m2) Symptoms 1+ 13 Peak LV to root of Ao Valve area (mm Hg) (cm2) Ao insuff 3. El-Said G, Galioto FM Jr, Mullins CE, McNamara DG: Natural hemodynamic history of congenital aortic stenosis in childhood. Am J Cardiol 30: 6, 1972 4. Friedman WF, Modlinger J, Morgan JR: Serial hemodynamic observations in asymptomatic children with valvar aortic stenosis. Circulation 43: 91, 1971 5. Hohn AR, VanPraagh S, Moore AAD, Vlad P, Lambert EC: Aortic stenosis. Circulation 31 and 32 (suppl III): 111-4, 1965 6. Braunwald E, Goldblatt S, Aygen MM, Rockoff SD, Morrow AG: Congenital aortic stenosis. Circulation 27: 426, 1963 7. Pansegrau DG, Kioshos JM, Durnin RE, Kroetz, FW: Supravalvar aortic stenosis in adults. Am J Cardiol 31: 635, 1973 8. Buckberg DG, Fixler DE, Archie JP, Hoffman JIE: Experimental subendocardial ischemia in dogs with normal coronary arteries. Circ Res 30: 67, 1972 9. Vincent WR, Buckberg GD, Hoffman JIE: Left ventricular subendocardial ischemia in severe valvar and supravalvar aortic stenosis: A common mechanism. Circulation 49: 326, 1974 10. Gorlin R, Gorlin SG: Hydraulic formula for calculation of the area of the mitral valve, other cardiac valves, and central circulatory shunts. Am Heart J 41: 1, 1951 11. Puyau FA, Hastings CP, Collins HA: Pulmonary stenosis: Comparison of measurements by three methods. Circulation 33 and 34 (suppl III): III193, 1966 12. Sendroy J Jr, Cecchini LP: Determination of human body surface area from height and weight. J Appl Physiol 7: 1, 1954 13. Brazier J, Cooper N, Buckberg G: The adequacy of subendocardial oxygen delivery. Circulation 49: 968, 1974 14. Sarnoff SJ, Braunwald E, Welch GH, Case RB, Stainsby WN, Marcruz R: Hemodynamic determinants of oxygen consumption of the heart with special reference to the tension time index. Am J Physiol 192: 148, 1958 15. Underhill WL, Tredway JB, D'Angelo GJ, Baay JEW: Familial supravalvar aortic stenosis: Comments on the mechanisms of angina pectoris. Am J Cardiol 27: 560, 1971 16. Maron BJ, Sissman NJ: The electrocardiogram in supravalvar aortic stenosis. Am Heart J 82: 300, 1971 17. Lewis AB, Heymann MA, Stanger P, Hoffman JIE, Rudolph AM: Evaluation of subendocardial ischemia in valvar aortic stenosis in children. Circulation 49: 987, 1974 18. Lakier JB, Lewis AB, Heymann MA, Stanger P, Hoffman JIE, Rudolph AM: Isolated aortic stenosis in the neonate. Circulation 50: 801, 1974 Subendocardial blood flow in children with congenital aortic stenosis. L J Krovetz and J P Kurlinski Downloaded from http://circ.ahajournals.org/ by guest on June 15, 2017 Circulation. 1976;54:961-965 doi: 10.1161/01.CIR.54.6.961 Circulation is published by the American Heart Association, 7272 Greenville Avenue, Dallas, TX 75231 Copyright © 1976 American Heart Association, Inc. All rights reserved. Print ISSN: 0009-7322. Online ISSN: 1524-4539 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://circ.ahajournals.org/content/54/6/961 Permissions: Requests for permissions to reproduce figures, tables, or portions of articles originally published in Circulation can be obtained via RightsLink, a service of the Copyright Clearance Center, not the Editorial Office. Once the online version of the published article for which permission is being requested is located, click Request Permissions in the middle column of the Web page under Services. Further information about this process is available in the Permissions and Rights Question and Answer document. Reprints: Information about reprints can be found online at: http://www.lww.com/reprints Subscriptions: Information about subscribing to Circulation is online at: http://circ.ahajournals.org//subscriptions/